Phimosis is the narrowing of the preputial orifice, leading to an inability to retract the foreskin, or prepuce, over the glans penis. Severe phimosis may cause pain on voiding, urinary retention, urinary tract infections, localised skin infections, and calculi, and later in life may be associated with sexual dysfunction and squamous-cell carcinoma.1,2 Phimosis is often secondary to recurrent infections or inflammatory scleroses, such as balanitis xerotica obliterans (see Box 1), where it may be accompanied by white scarring and induration.2 Circumcision is a standard treatment option for phimosis, although there is increasing evidence that topical steroids are also effective.3,4 One study estimated that 0.6% of boys were affected by phimosis before reaching 15 years of age,5 while, in Denmark, about 1.5% of boys were affected by age 17 years.6 The condition rarely occurs before five years of age, and reaches its peak incidence before puberty.2
Non-retractable foreskins, or preputial adhesions, occur in young boys as a normal part of penile development, and these adhesions separate over time, requiring no surgical intervention. A United Kingdom report showed that only four percent of newborns had a completely retractable prepuce, but that by two years of age this had increased to 80%.7
After concerns were raised in the UK that normal preputial adhesions were being misdiagnosed as phimosis, particularly in children, and were leading to unnecessary circumcisions,8 the rate of circumcisions performed for medically indicated reasons declined, most notably in boys less than five years of age.9
We aimed to determine the rates of circumcision to treat phimosis in Western Australian boys over a 19-year period and to compare these with circumcision rates for other medical conditions.
Our study was conducted as part of the Western Australian Safety and Quality of Surgical Care Project,10 using the Western Australian Health Services Research Data Linkage System (WA Data Linkage System) to access hospital separation data based on a population of over 1.9 million people, spanning a 19-year period.11
Anonymous hospital morbidity data on all males circumcised in all Western Australian hospitals between 1 January 1981 and 31 December 1999 were extracted using the WA Data Linkage System.
The morbidity dataset included standard demographic and hospital details, but did not include physician identifiers. The quality of the hospital administrative data used to compile the Hospital Morbidity Data System is regularly validated by 21 different quality checks and periodic audits.11 Morbidity records were selected using the International classification of diseases (ICD) procedure codes for circumcision (ICPM,12 5-640; ICD-9-CM,13 64.0; or ICD-10-CM,14 30653-00). The ICD diagnosis codes used to identify circumcisions performed for medically indicated reasons are listed in Box 2. We did not include diagnosis codes relating to urinary tract infections, as it is not possible to distinguish between preoperative and postoperative infections, and as there were only 63 circumcisions associated with this code over the 19 years.
Circumcisions performed for routine (non-medical) reasons were distinguished from medically indicated circumcisions by ICD codes V50.0, V50.2 and Z41.2. Most circumcisions performed during the birth admission were for non-medical reasons and were excluded from analysis. A case was designated a birth admission if the date of birth subtracted from the hospital separation date was less than five days.
Circumcisions not performed in a hospital were not included in this study. Postcode of place of residence, and not hospital location, was used to assign a metropolitan or country status to account for non-metropolitan boys seeking treatment in Perth.
Poisson regression was performed in SAS15 to investigate the association between circumcision rates and calendar year, age group, place of residence (metropolitan or country) and race. Western Australian population data, used as denominators in rate calculations and stratified by calendar year, location, race and age group, were obtained from the Western Australian Department of Health. Calendar year was treated as a continuous variable and age group and place of residence as categorical variables. Interaction terms were entered into the regression model to test whether the association between the rate of circumcision and both calendar period and place of residence varied by age group.
Age-specific circumcision rates are reported in the age groups 0–4 years, 5–9 years, 10–14 years and 15 years and older. The percentage changes in rates and 95% confidence intervals over the 19-year study period were estimated from the rate ratio generated by multiplying the yearly beta coefficients, standard errors and, where applicable, covariances by 19 before taking the exponential. The calculation of change in circumcision rates associated with balanitis xerotica obliterans over time was restricted from 1987 onwards, as ICD-9 codes before this time also included other disorders of the penis. All analysis was performed on anonymous data current to 31 December 1999.
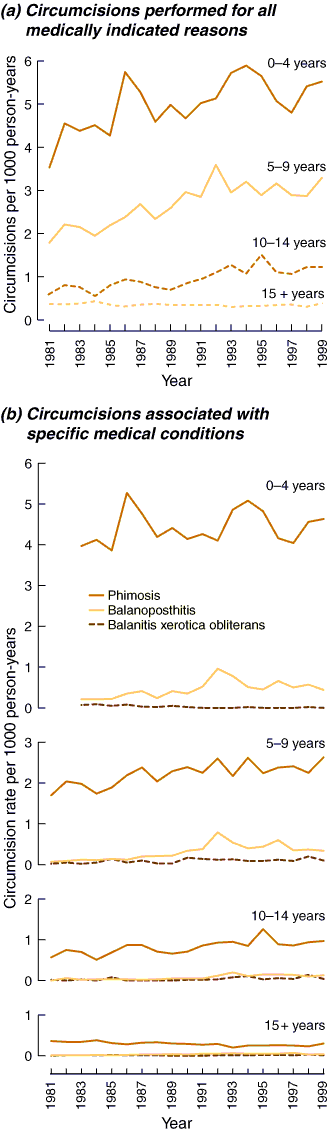
There were 25 718 index admission records for circumcision in Western Australian hospitals from 1 January 1981 to 31 December 1999, of which 56% (14 416) were performed for medically indicated reasons. Age-specific rates of circumcision for medically indicated reasons are shown in Box 3. Boys aged 0–4 years had consistently higher rates of circumcision than any other age group. The largest increase in rates over the study period was in boys aged 10–14 years. In contrast, there was a decline in the rate of circumcision in males aged 15 or more years during the same period (Box 4). No significant difference was detected between the rates of circumcision for medical indications in Aboriginals and/or Torres Strait Islanders compared with the non-Indigenous Western Australian population (P = 0.08).
The most common medical indication for circumcision at all ages was phimosis, followed by balanoposthitis and balanitis xerotica obliterans. After controlling for age group and calendar year, the rate of circumcision associated with phimosis was 20 times that for balanitis xerotica obliterans (95% CI, 14.0–31.1 times) and 8.3 (95% CI, 6.9–10.1) times that for balanoposthitis. Boys aged 0–4 years consistently had the highest rate of circumcision to treat phimosis compared with the other age groups (Box 4). The three youngest age groups showed an increase in the rate of circumcision associated with phimosis over the study period. Boys aged 10–14 years showed the greatest change, with the rate increasing by 70% from 1981 to 1999. In contrast, there was a 33% decrease in the rate of circumcision to treat phimosis in males aged 15 or more years from 1981 to 1999.
The rate of circumcision to treat balanoposthitis was also highest in boys aged 0–4 years, with a rate 12.6 (95% CI, 10.5–15.1) times that of males aged 15 years and over. After adjusting for calendar year, boys aged 5–9 years and 10–14 years had rates 9.3 (95% CI, 7.7–11.3) and 2.5 (95% CI, 1.9–3.4) times higher than males aged 15 or more years, respectively. From 1981 to 1999, the overall rate of circumcision to treat balanoposthitis increased 232% (95% CI, 154%–336%). There was no significant difference in the rate of increase between age groups (P = 0.61). After adjusting for calendar year, the rate of circumcision to treat balanitis xerotica obliterans in boys aged 5–9 years was 10.5 times higher (95% CI, 7.8–14.1) than in males 15 years and older. Boys aged 0–4 years were circumcised to treat balanitis xerotica obliterans 3.1 (95% CI, 1.5–6.1) times and boys aged 10–14 years were circumcised 5.4 (95% CI, 3.7–7.9) times more often than males aged 15 years and older.
Place of residence had a significant effect on the rate of circumcision to treat phimosis (Box 4). Boys aged 0–4 years living in country areas were 1.5 times more likely to be circumcised than those living in metropolitan Perth, and those aged 10–14 years living in the country were 1.4 times more likely to be circumcised than boys of the same age living in Perth. For males aged 15 or more years the inverse was found.
The past 19 years have seen a steady rise in the rate of medically indicated circumcision in boys aged less than 15 years. Most of the increase is the result of an increase in the rates of phimosis, the most common medical condition associated with circumcision. If the 1999 rate remains stable, it is estimated that four percent of all boys will be circumcised for phimosis by the time they reach age 15 years. This is seven times higher than the estimated occurrence rate of pathological phimosis.5 Over half of these boys (around 300 a year) will be circumcised for phimosis before they reach five years of age, despite the condition being rare in early childhood, when preputial adhesions are the norm. Our findings indicate that a review of current practice guidelines for the paediatric management of phimosis in Australia may be warranted.
The high incidence rate of phimosis and subsequent circumcision in young Western Australian boys could have several reasons. Firstly, physicians may be mistaking normal penile development for pathological phimosis. This hypothesis is supported by two studies that concluded physicians (including general practitioners) who made inappropriate referrals to paediatric surgeons had difficulty discriminating between the two conditions.8,16 A prospective study of the histopathology of removed foreskins would be necessary to confirm this hypothesis. Secondly, the Australasian Association of Paediatric Surgeons does not support routine (elective) circumcision,17 and the rate of routine circumcision in boys aged less than six months in Western Australia had fallen to 7.9% by 1999 (personal unpublished data) from the 20.5% reported for 1982 and 1983.18 The rate of decline was greater for routine circumcisions performed in hospitals than for those performed elsewhere. It may be that hospital physicians may feel more pressure to conform to medical opinion and to ascribe a medical reason and code to a routine circumcision. However, there was no evidence to suggest this was case, as the rate of routine circumcision in boys older than six months actually increased over the study period.
Boys aged less than five years living in country areas were more likely to be circumcised for a medical reason compared with boys living in metropolitan areas, and this disparity was the result of the difference in circumcision rates to treat phimosis. In contrast, the rates of circumcision to treat balanoposthitis or balanitis xerotica obliterans did not significantly differ between country and metropolitan areas. It is unclear why the diagnosis of phimosis is made more frequently in young boys living in country areas. Substantial variations in medical practice between country and metropolitan areas of Western Australia have also been observed in appendicectomy19 and elective circumcisions (personal unpublished data).
In the interests of best medical practice, the factors resulting in high circumcision rates to treat phimosis in young boys need to be examined. The cost of a circumcision ranges from $100 to $1600, depending on whether an overnight hospital admission and general anaesthetic are involved. In addition, as with any medical procedure, circumcision has a complication risk and raises ethical issues if an unnecessary procedure is being performed on a non-consenting minor. Physicians and parents concerned about preputial adhesions should be encouraged to consider alternatives and to delay circumcision. Young boys with a confirmed diagnosis of phimosis do not necessarily need to be circumcised. Topical steroids have been shown to be a cost-effective approach in reversing phimosis.4,20 Our findings suggest that improved education for physicians, and perhaps parents, with regard to foreskin development and management is required.
1: Definition of terms
Non-retractile foreskin (preputial adhesions)
A normal developmental process involving the gradual separation of the prepuce from the glans as epithelial cell layers become keratinised and smegma is produced.
Phimosis
Narrowing of the preputial orifice leading to non-retractability of the prepuce that in rare instances may be a congenital condition, but which is more commonly associated with balanitis xerotica obliterans or balanoposthitis.
Balanitis xerotica obliterans
A chronic sclerosis and atrophic process of the glans penis and prepuce of unknown aetiology. Genetic factors have been implicated. Associated phimosis, if present, is characterised by white scarring and induration.
Balanoposthitis
Acute or chronic inflammation of the mucous surface of the prepuce that results from a wide variety of causes, including fungal, bacterial and protozoal infections and risk factors such as poor penile hygiene.
2: International classification of diseases diagnosis codes used to identify circumcision performed for medically indicated reasons
Medical indication |
ICD-9* |
ICD-9-CM† |
ICD-10-AM‡ |
||||||||
Phimosis |
605 |
605 |
N47 |
||||||||
Balanoposthitis |
607.1 |
607.1 |
N48.1 |
||||||||
Balanitis xerotica obliterans |
607.8 |
607.81 |
N48.0 |
||||||||
Hypospadias |
752.6 |
752.6 |
Q54, Q64.0 |
||||||||
Congenital abnormalities of penis |
752.8-9 |
752.8-9 |
Q55.0-9 |
||||||||
Other penile disorders |
607.2-9 |
607.0-8, 607.82-9 |
N48.2-9 |
||||||||
Penis cancer |
187.1-4 |
187 |
C60.1-2, 9 |
||||||||
* International classification of diseases, 9th revision. † International classification of diseases, 9th revision, clinical modification. ‡ International classification of diseases, 10th revision, Australian modification. |
|||||||||||
4: Trends in the rates of circumcision for medically indicated conditions in males living in metropolitan and country areas of Western Australia, 1981–1999, stratified by age group
|
Cases* |
Rate† |
Rate ratio (95% CI) for country v metropolitan‡ |
Total % rate change (95% CI) from 1981 to 1999§ |
|||||||
All medical indications |
|||||||||||
0–4 years |
361 |
5.51 |
1.40 |
(1.30–1.50) |
35 |
(20–53) |
|||||
5–9 years |
225 |
3.29 |
0.98 |
(0.88–1.09) |
66 |
(40–98) |
|||||
10–14 years |
86 |
1.23 |
1.28 |
(1.07–1.52) |
105 |
(55–270) |
|||||
15 + years |
281 |
0.39 |
0.77 |
(0.69–0.86) |
–10 |
(–22 to –5) |
|||||
Phimosis |
|||||||||||
0–4 years |
303 |
4.63 |
1.50 |
(1.39–1.62) |
23 |
(8–39) |
|||||
5–9 years |
180 |
2.63 |
1.07 |
(0.95–1.19) |
41 |
(18–68) |
|||||
10–14 years |
68 |
0.97 |
1.39 |
(1.17–1.67) |
70 |
(27–126) |
|||||
15 + years |
217 |
0.30 |
0.75 |
(0.67–0.84) |
–33 |
(–43 to –22) |
|||||
Balanoposthitis |
|||||||||||
0–4 years |
29 |
0.44 |
0.94 |
(0.79–1.11) |
232 |
(154–336) |
|||||
5–9 years |
23 |
0.34 |
|||||||||
10–14 years |
9 |
0.13 |
|||||||||
15 + years |
32 |
0.04 |
|||||||||
Balanitis xerotica obliterans |
|||||||||||
0–4 years |
0 |
— |
0.91 |
(0.63–1.31)¶ |
141 |
(48–292)¶ |
|||||
5–9 years |
7 |
0.10 |
|||||||||
10–14 years |
3 |
0.04 |
|||||||||
15 + years |
8 |
0.01 |
|||||||||
Poisson regression modelling was used with continuous variable calendar period and categorical variables age group and place of residence all entered simultaneously. Interaction terms age group x calendar period and age group x place of residence were included in the final regression model for "all medically indicated" and "phimosis". * Number of circumcisions performed in 1999. † Actual rate of circumcision per 1000 person-years for 1999. ‡ Rate ratio depicting the difference in circumcision rate between country and metropolitan Perth residence after adjusting for calendar year (metropolitan Perth was used as the reference group). § Calculated by multiplying the average yearly change by length of study period. ¶ Calculations restricted from 1987 onwards because of non-specific International classification of diseases coding before this year. |
|||||||||||
Received 22 April 2002, accepted 26 August 2002
- Katrina Spilsbury1
- James B Semmens2
- C D'Arcy J Holman3
- Z Stan Wisniewski4
- 1 Centre for Health Services Research, School of Population Health, University of Western Australia, Crawley, WA.
- 2 Western Australian Safety and Quality of Surgical Care Committee, Royal Australasian College of Surgeons, Western Australian Branch, Nedlands, WA.
We thank the Data Linkage Unit, Western Australian Department of Health, for the linked hospital morbidity data files. This project was funded through the Western Australian Safety and Quality of Surgical Care Project by a National Health and Medical Research Council research grant.
None identified
- 1. Maiche AG. Epidemiological aspects of cancer of the penis in Finland. Eur J Cancer Prev 1992; 1: 153-158.
- 2. Rickwood AM. Medical indications for circumcision. BJU Int 1999; 83 Suppl 1: 45-51.
- 3. Chu CC, Chen KC, Diau GY. Topical steroid treatment of phimosis in boys. J Urol 1999; 162: 861-863.
- 4. Berdeu D, Sauze L, Ha-Vinh P, Blum-Boisgard C. Cost-effectiveness analysis of treatments for phimosis: a comparison of surgical and medicinal approaches and their economic effect. BJU Int 2001; 87: 239-244.
- 5. Shankar KR, Rickwood AM. The incidence of phimosis in boys. BJU Int 1999; 84: 101-102.
- 6. Oster J. Further fate of the foreskin. Incidence of preputial adhesions, phimosis, and smegma among Danish schoolboys. Arch Dis Child 1968; 43: 200-203.
- 7. Gairdner D. The fate of the foreskin: a study of circumcision. Br Med J 1949; 2: 1433-1437.
- 8. Rickwood AM, Walker J. Is phimosis over diagnosed in boys and are too many circumcisions performed in consequence? Ann R Coll Surg Engl 1989; 71: 275-277.
- 9. Rickwood AM, Kenny SE, Donnell SC. Towards evidence based circumcision of English boys: survey of trends in practice. BMJ 2000; 321: 792-793.
- 10. Semmens JB, Lawrence-Brown MM, Fletcher DR, et al. The Quality of Surgical Care Project: a model to evaluate surgical outcomes in Western Australia using population-based record linkage. Aust N Z J Surg 1998; 68: 397-403.
- 11. Holman CD, Bass AJ, Rouse IL, Hobbs MS. Population-based linkage of health records in Western Australia: development of a health services research linked database. Aust N Z J Public Health 1999; 23: 453-459.
- 12. World Health Organization. International classification of procedures in medicine. Geneva: WHO, 1978.
- 13. Australian version of the international classification of diseases, 9th revision, clinical modification (ICD-9-CM). Sydney: National Coding Centre, 1995.
- 14. International statistical classification of diseases and related health problems, 10th revision, Australian modification (ICD-10-AM). Sydney: National Centre for Classification, 2000.
- 15. The SAS system for Windows [computer program]. Version 8.02. Cary, NC: SAS Institute, 2001.
- 16. Griffiths D, Frank JD. Inappropriate circumcision referrals by GPs. J R Soc Med 1992; 85: 324-325.
- 17. Leditschke JF. Guidelines for circumcision. Brisbane: The Australasian association of paediatric surgeons, 1996.
- 18. Wirth JL. Circumcision in Australia: an update. Aust Paediatr J 1986; 22: 225-226.
- 19. Donnelly N, Semmens J, Fletcher D, Homan C. Appendicectomy in Western Australia: profile and trends 1981–1997. Med J Aust 2001; 175: 15-18.
- 20. Dewan PA, Tieu HC, Chieng BS. Phimosis: is circumcision necessary? J Paediatr Child Health 1996; 32: 285-289.





Abstract
Objective: To investigate the incidence rate of circumcision for phimosis and other medically indicated reasons in Western Australian boys from 1 January 1981 to 31 December 1999.
Design and setting: A population-based incidence study using hospital discharge data of all circumcisions performed in all WA hospitals during the study period.
Main outcome measures: Changes in the incidence rate of circumcision for medically indicated reasons.
Results: The rate of medically indicated circumcisions increased in boys aged less than 15 years during the study period. Phimosis was the most common medical indication for circumcision in all age groups. The rate of circumcision associated with phimosis was eight times that associated with balanoposthitis and 21 times that of balanitis xerotica obliterans. Boys aged less than five years had the highest rate of circumcision to treat phimosis, at 4.6 per 1000 person-years, representing about 300 circumcisions per year. Boys aged less than five years living in country areas were 1.5 times more likely to be circumcised for phimosis than boys living in metropolitan Perth.
Conclusion: The rate of circumcision to treat phimosis in boys aged less than 15 years is seven times the expected incidence rate for phimosis. Many boys are circumcised before reaching five years of age, despite phimosis being rare in this age group.