Australian lipid management guidelines published in 2001 highlighted the need to assess absolute coronary risk before prescribing lipid-modifying drugs.1 Patients already manifesting coronary or other arterial disease, or those with diabetes or certain other conditions, were deemed to be at "higher absolute risk" and would merit intervention with lipid-lowering medication. Others at lesser risk would merit intervention if their absolute risk of cardiovascular disease (CVD) exceeded 10%–15% over the ensuing 5 years — as assessed by a CVD risk calculator2 derived from the Framingham Study.3 US and European guidelines advocate a generally similar approach, but target risk over 10 years rather than 5 years.4,5 A recent UK lipid intervention trial confirmed that lipid therapy reduces the incidence of stroke as well as coronary heart disease (CHD) in high risk patients.6 Hence, it is important that risk calculation relates to CVD risk, not just CHD risk.
The Framingham risk function has been validated in middle-aged men and women in Northern Europe7 and Busselton, WA,8 but has not been similarly validated in elderly populations outside Framingham. The Australian Dubbo Study of the elderly has previously reported on risk factors for myocardial infarction,9 CHD10 and stroke.11 In this report (i) we evaluate the Framingham risk function for CHD in this elderly Australian cohort and (ii) we derive an Australian CVD risk function for subjects 60 years and older.
The Dubbo Study is an ongoing prospective study in an elderly Australian cohort first examined in 1988.12 All non-institutionalised residents of the semi-urban town of Dubbo, NSW (population, 34 000), born before 1930 were eligible: the participation rate was 73%, with an ultimate cohort of 2805 men and women. Methods and measures have already been described in detail.12 Briefly, the baseline examinations comprised demographic, psychosocial and standard cardiovascular risk assessment. Venous blood was obtained after a 12-hour fast for assessment of total serum cholesterol and triglyceride levels by automated enzymatic methods,13,14 high-density lipoprotein (HDL) cholesterol level by a precipitation method,15 and plasma glucose level.
Outcomes at 5 and 10 years from the date of the baseline examination were included. Hospitalisation and death records were monitored continuously and postal surveys were conducted every 2 years to confirm vital status. The survey closest to 10 years successfully traced more than 95% of surviving participants. Outcomes assessed from records were coded according to the International classification of diseases, 9th edition (clinical modification) and 10th edition (Australian modification). Files indicating myocardial infarction were assessed individually.
From the original cohort of 2805 subjects, several smaller subcohorts were derived by removing subjects with prevalent CHD,16 stroke (including transient ischaemic attack) or diabetes, as described in the Results section. Diabetes was defined as a fasting plasma glucose level ≥ 7.0 mmol/L, self-reported history of diabetes, or taking diabetes therapy.17 The remainder were coded as non-diabetic; ex-smokers were coded as non-smokers, as in the Framingham risk function (Box 1).3
Age- and sex-specific incidence rates were calculated for the outcome CVD, comprising myocardial infarction, coronary death or stroke. This outcome (effectively "hard" CHD4) excluded other, non-fatal forms of CHD, but included transient ischaemic attack. Logistic regression analysis was used to calculate the 5- and 10-year probability of CVD. A large number of variables were entered in a single block and a final model was recalculated as the most parsimonious version, retaining only variables of statistical significance and potential confounders. Statistical analysis was conducted using SPSS.19
The Framingham risk function (Box 1) was applied to 1800 Dubbo men and women, aged 60–79 years, who were free of prevalent CVD or diabetes at study entry. Age- and sex-specific observed and predicted CHD incidence rates are presented in Box 2. Observed CHD incidence rates increased with age in an incremental fashion in both sexes. In general, there was good agreement between observed and predicted rates. This Framingham risk function offered no prediction in those older than 79 years and was not used further in this report.
Age- and sex-specific incidence rates over 5 and 10 years for CVD (acute myocardial infarction, coronary death or stroke) in 2102 Dubbo men and women free of prevalent CHD or stroke at study entry (but including those with diabetes) are presented in Box 3. The incidence rate increased with age and was greater in men than women, except for the 10-year rate in those 80 years and over. The proportion of CVD events attributable to stroke increased with age. The 5-year CHD incidence in women was very stable until 80 years and over, while 10-year CHD incidence increased with age.
This cohort of 2102 excluded more than 700 subjects with prevalent CVD who were at increased risk of a CVD event. For this subcohort of 2102 subjects, an age-adjusted CVD rate for 5 and 10 years was calculated based on the age distribution of the total cohort. The 5-year rate/100 subjects in men was 12.1 versus 16.7 in the total cohort of 1233, and the 10-year rate was 25.3 versus 31.2. The 5-year rate/100 subjects in women was 8.6 versus 12.3 in the total cohort of 1572, and the 10-year rate was 19.4 versus 23.2.
The following variables were selected for inclusion in the final logistic model for CVD risk at 5 and 10 years in the cohort of 2102 subjects free of prevalent CHD or stroke at study entry: age (years), sex, use of antihypertensive medication (yes/no), systolic blood pressure (mmHg), smoking (yes/no), total and HDL cholesterol levels (mmol/L), and diabetes (yes/no). The addition of the log of triglyceride level to the model produced a non-significant coefficient, did not influence other regression coefficients and was omitted. Family history of CHD was not significant. Quadratic terms for age or cholesterol level were non-significant, and there were no significant interactions between age or sex and other risk factors. This enabled the presentation of a single model, including a term for sex. The results with this model are presented in Box 4.
All risk factors achieved statistical significance except HDL cholesterol, but this still functioned as a protective factor. Goodness-of-fit for the logistic function was highly satisfactory (χ2 at 5 years, 107, P < 0.001, df = 8; χ2 at 10 years, 167, P < 0.001, df = 8).
Absolute CVD risk over the specified period may be calculated from the logistic function in Box 4 according to the formula given in the footnote to Box 4.
We have calculated 5-year CVD risk for a 75-year-old man and a 75-year-old woman for increasing cholesterol levels by the presence of additional risk factors (Box 5). Those with multiple risk factors have the highest CVD risk. At the age of 75 years the use of antihypertensive medication in a man indicated increased CVD risk/100 subjects from 9.5 to 18.2, the presence of diabetes indicated increased risk to 19.9, or smoking to 14.3. The use of antihypertensive medication in a woman indicated increased risk from 5.2 to 10.3, the presence of diabetes to 11.4, or smoking to 7.9.
This report extends previous work in the Dubbo Study on the epidemiology of CHD and stroke in the elderly9-11 by addressing two new objectives: to evaluate a Framingham risk function for "hard" CHD (myocardial infarction or coronary death) in an elderly Australian cohort; and to derive risk functions for CVD in elderly Australians using a short list of risk factors readily accessible to general practitioners.
Some limitations in a cross-study comparison between Framingham and Dubbo are discussed below. Nevertheless, we found excellent agreement between observed and predicted rates for hard CHD over 10 years in elderly men and women. A similar risk function developed from three European populations20 has some similarities with our findings, but true comparisons are difficult because that study did not exclude prevalent CHD and the outcome was CVD mortality, not incidence.
The Dubbo risk function was based on a single baseline assessment. Hence, the risk estimates may be slightly underestimated as a result of regression dilution bias.21 However, this would also apply to the Framingham estimates. The relative strengths of each predictor in the logistic model cannot be directly compared, as we have not shown standardised regression coefficients. However, they may be compared between time periods of 5 and 10 years. Taking antihypertensive medication and diabetes were substantially stronger predictors during the shorter term, which may justify further investigation of short- and long-term predictors, as they may differ in elderly people. This may also provide impetus for more aggressive treatment of hypertension and diabetes in the short term.
The five-year CHD incidence in women increased very little with age until 80 years and over (Box 3). However, the subcohort of 2102 subjects excluded those at high risk (prior CVD). The 10-year follow-up showed a clear rise in incidence with age.
It was surprising that HDL cholesterol level did not reach statistical significance as a predictor of CVD in the context of other variables. Our previous analyses, employing Cox proportional hazards regression, did not exclude prevalent CVD, and HDL cholesterol was a significant predictor of CHD9,10 and stroke.11 We have re-examined the 5- and 10-year CVD incidence data using proportional hazards regression and found regression coefficients very similar to those from the logistic regression (data not shown). Framingham models have employed a ratio of total to HDL cholesterol level.3 A previous Dubbo analysis in myocardial infarction showed similar prediction using total cholesterol or total/HDL cholesterol ratio,9 and we continue to model total and HDL cholesterol as separate variables.
For a given age and cholesterol level, CVD risk over 5 years is doubled in the presence of antihypertensive medication or diabetes, increased by 50% with cigarette smoking, and halved in women compared with men.
Australian lipid management guidelines recommend global risk assessment through use of a calculator,2 derived from an earlier Framingham equation (1991).3 We have computed 5-year CVD risk using both the current Dubbo model and the 1991 Framingham model for subjects 60 years and older and noted a large systematic difference between the rates. For example, in relatively low-risk subjects, the predicted CVD risk was 55%–70% lower using the Dubbo model. This might appear a surprising finding given the good agreement between observed CHD rates and those predicted by a different Framingham model (see Box 2). In reality, there are numerous Framingham algorithms available, and the one used in Box 2 (derived from ATP III) models only hard CHD (myocardial infarction and coronary death).4,18 Hard CHD excludes diagnoses such as angina pectoris or chronic CHD, which are often made in a clinic setting rather than during hospitalisation. The Framingham 1991 equation assessed total CHD, not just hard CHD.3 We subsequently computed CVD rates in the Dubbo cohort for an "extended" CVD outcome which included hospitalisation for angina or chronic CHD and this yielded CVD rates about 50% higher than those in Box 3, but still lower than those predicted by the 1991 Framingham equation. The Dubbo Study relies essentially on hospitalisation data, whereas this Framingham model relies on clinic assessment (ie, the two studies are not measuring the same outcomes). Hence, it is important to be very specific in nominating CVD outcomes — do they include hard CHD or total CHD? Where were they ascertained?
The Australian guidelines define "higher risk" as a calculated 5-year CVD risk threshold exceeding 10%–15% and recommend that such patients may require lipid intervention.1 With use of the Framingham 1991 model, this refers to the risk of total CHD plus stroke. A risk threshold exceeding 10%–15% would be highly inappropriate if considering only hard CHD, the outcome used in clinical trials.6
1: Framingham risk function
Lipid treatment guidelines in the United States (Adult Treatment Panel III [ATP III]) use a modified Framingham risk function to predict the 10-year risk of a major coronary heart disease (CHD) event (myocardial infarction or coronary death) in men and women 20–79 years who are free of prevalent cardiovascular disease (CVD) or diabetes.4,18 Calculating risk involves allocating a point system for the risk factors sex, age (5-year groupings), total and HDL cholesterol levels, smoking, systolic blood pressure and blood pressure treatment status (http://hin.nhlbi.nih.gov/atpiii/calculator.asp).
2: Observed 10-year coronary heart disease (CHD [myocardial infarction or coronary death]) incidence rates and Framingham-predicted CHD incidence rates in Dubbo men and women free of prevalent myocardial infarction, stroke or diabetes
CHD incidence rate/100 subjects |
|||||||||||
Age range (number of men/women) |
Men |
Women |
|||||||||
Observed |
Predicted |
Observed |
Predicted |
||||||||
60–64 years (310/386) |
10.3 |
11.9 |
4.9 |
4.6 |
|||||||
65–69 years (214/290) |
13.6 |
16.5 |
7.6 |
9.0 |
|||||||
70–74 years (149/225) |
16.8 |
16.5 |
11.1 |
10.7 |
|||||||
75–79 years (82/144) |
23.2 |
22.1 |
14.6 |
18.2 |
|||||||
χ2 tests showed no significant differences between observed and predicted rates for each age group. |
|||||||||||
3: Age-specific incidence rates of cardiovascular disease (with rates of coronary heart disease [CHD] and stroke in parentheses) over 5 and 10 years in Dubbo men and women free of prevalent CHD or stroke at study entry, but including those with diabetes
Age range (number of men/women) |
5-year incidence rate/100 subjects |
10-year incidence rate/100 subjects |
|||||||||
Men |
Women |
Men |
Women |
||||||||
60–64 years |
7.1 |
5.3 |
16.7 |
9.9 |
|||||||
(336/413) |
(5.4, 1.7) |
(4.1, 1.2) |
(11.9, 4.8) |
(6.1, 3.8) |
|||||||
65–69 years |
11.7 |
6.9 |
21.6 |
13.1 |
|||||||
(231/306) |
(7.8, 3.9) |
(4.6, 2.3) |
(14.3, 7.3) |
(7.8, 5.3) |
|||||||
70–74 years |
13.2 |
7.6 |
31.7 |
18.9 |
|||||||
(167/238) |
(6.6, 6.6) |
(3.8, 3.8) |
(18.0, 13.7) |
(11.8, 7.1) |
|||||||
75–79 years |
16.3 |
13.2 |
38.4 |
29.8 |
|||||||
(86/151) |
(10.5, 5.8) |
(3.3, 9.9) |
(23.3, 15.1) |
(15.2, 14.6) |
|||||||
80+ years |
25.9 |
17.2 |
37.9 |
45.7 |
|||||||
(58/116) |
(19.0, 6.9) |
(8.6, 8.6) |
(24.1, 13.8) |
(25.9, 19.8) |
|||||||
4: Prediction of 5- and 10-year incidence of cardiovascular disease in a multiple logistic model in Dubbo men and women 60 years and older
5-year incidence |
10-year incidence |
||||||||||
Regression coefficient |
P |
Odds ratio (95% CI) |
Regression coefficient |
P |
Odds ratio (95% CI) |
||||||
Age |
0.057 |
< 0.001 |
1.06 |
0.073 |
< 0.001 |
1.08 |
|||||
Sex |
– 0.610 |
< 0.001 |
0.54 |
– 0.590 |
< 0.001 |
0.55 |
|||||
Antihypertensive medication |
0.749 |
< 0.001 |
2.12 |
0.380 |
< 0.01 |
1.46 |
|||||
Systolic blood pressure |
0.008 |
< 0.01 |
1.01 |
0.008 |
< 0.001 |
1.01 |
|||||
Smoking |
0.458 |
< 0.03 |
1.58 |
0.340 |
< 0.03 |
1.41 |
|||||
Cholesterol level |
0.180 |
< 0.01 |
1.20 |
0.186 |
< 0.001 |
1.20 |
|||||
HDL cholesterol level |
– 0.234 |
< 0.30 |
0.79 |
– 0.255 |
< 0.13 |
0.77 |
|||||
Diabetes |
0.857 |
< 0.001 |
2.36 |
0.528 |
< 0.01 |
1.69 |
|||||
Intercept |
– 8.65 |
< 0.001 |
– 8.18 |
< 0.001 |
|||||||
Age, systolic blood pressure, total and HDL cholesterol levels were entered as continuous variables and the regression coefficient refers to a one-unit change. The remainder were entered as dichotomous variables and the coefficient refers to the presence or absence of the state (for sex, men were the reference category). Absolute CVD risk can be calculated from the formula: Probability of CVD = 1/(1 + e- k ), where k = – 8.65 + 0.057*age – 0.61*sex + 0.749*antihypertensive medication + 0.008*systolic blood pressure + 0.458*smoking + 0.18*cholesterol – 0.234*HDL cholesterol + 0.857*diabetes. |
|||||||||||
5: Calculated 5-year cardiovascular disease risk for a 75-year-old man (A) and woman (B) in the logistic model, according to cholesterol level and the presence of other risk factors
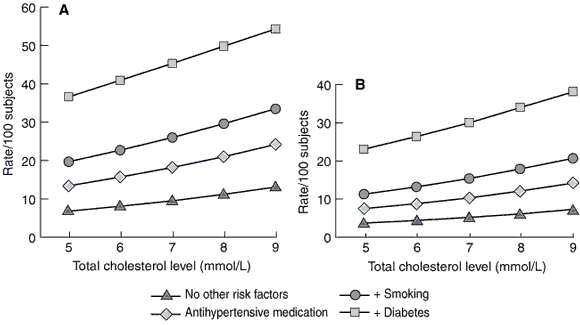
Reference group: not taking antihypertensive medication, systolic pressure 140 mmHg, non-smoking, HDL level 1.10 mmol/L, no diabetes.
Received 15 April 2002, accepted 16 August 2002
- Leon A Simons1
- Judith Simons2
- Latha Palaniappan3
- Yechiel Friedlander4
- John McCallum5
- 1 University of New South Wales Lipid Research Department, St Vincent's Hospital, Darlinghurst, NSW.
- 2 Department of Social Medicine, Hebrew University–Hadassah Hospital, Jerusalem, Israel.
- 3 University of Western Sydney, Campbelltown, NSW.
The Dubbo Study has been supported in part by grants from the National Health and Medical Research Council of Australia, AstraZeneca, Bayer Australia, Bristol-Myers Squibb Australia, Merck Sharp & Dohme Australia, Pfizer and Unilever Australasia. These organisations made no intellectual input to the design or conduct of the study.
None identified.
- 1. Lipid Management Guidelines – 2001. National Heart Foundation of Australia and Cardiac Society of Australia and New Zealand. Med J Aust 2001; 175 (Suppl 16 Oct): S57-S85.
- 2. New Zealand Guidelines Group. Cardiovascular disease: baseline risk and treatment benefit. Available at: http://www.nzgg.org.nz/working_groups/cardio_risk_chart.pdf (accessed Aug 2002).
- 3. Anderson KM, Odell PM, Wilson PWF, Kannel WB. Cardiovascular disease risk profiles. Am Heart J 1991; 121: 293-298.
- 4. Executive Summary of the Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). JAMA 2001; 285: 2486-2497.
- 5. Wood D, De Backer G, Faergerman O, et al. Prevention of coronary heart disease in clinical practice. Recommendations of the Second Joint Task Force of European and other Societies on coronary prevention. Eur Heart J 1998; 19: 1434-1503.
- 6. Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study of cholesterol lowering with simvastatin in 20536 high-risk individuals: a randomised placebo-controlled trial. Lancet 2002; 360: 7-22.
- 7. Haq IU, Ramsay LE, Yeo WW, et al. Is the Framingham risk function valid for northern European populations? A comparison of methods for estimating absolute coronary risk in high risk men. Heart 1999; 81: 40-46.
- 8. Knuiman MW, Vu HT. Prediction of coronary heart disease mortality in Busselton, Western Australia: an evaluation of the Framingham, national health epidemiologic follow up study, and WHO ERICA risk scores. J Epidemiol Community Health 1997; 51: 515-519.
- 9. Simons LA, Simons J, Friedlander Y, McCallum J. Risk factors for acute myocardial infarction in the elderly (The Dubbo Study). Am J Cardiol 2002; 89: 69-72.
- 10. Simons LA, Friedlander Y, McCallum J, Simons J. Risk factors for coronary heart disease in the prospective Dubbo Study of Australian elderly. Atherosclerosis 1995; 117: 107-118.
- 11. Simons LA, McCallum J, Friedlander Y, Simons J. Risk factors for ischemic stroke. Dubbo Study of the Elderly. Stroke 1998; 29: 1341-1346.
- 12. Simons LA, McCallum J, Friedlander Y, et al. Dubbo Study of the Elderly: sociological and cardiovascular risk factors at entry. Aust N Z J Med 1991; 21: 701-709.
- 13. Allain CC, Poon LC, Chan CSG, et al. Enzymatic determination of total serum cholesterol. Clin Chem 1974; 20: 470-475.
- 14. Bucolo G, David H. Quantitative determination of serum triglycerides by the use of enzymes. Clin Chem 1973; 19: 476-482.
- 15. Burstein N, Scholnick HR, Morphin R. Rapid methods for the isolation of lipoproteins from human serum by precipitation with polyanions. J Lipid Res 1970; 11: 583-595.
- 16. Simons LA, Friedlander Y, McCallum J, et al. The Dubbo Study of the Health of Elderly: correlates of coronary heart disease at study entry. J Am Geriatr Soc 1991; 39: 584-590.
- 17. Simons LA, McCallum J, Friedlander Y, Simons J. Fasting plasma glucose in non-diabetic elderly women predicts increased all-causes mortality and coronary heart disease risk. Aust N Z J Med 2000; 30: 41-47.
- 18. Wilson PWF, D'Agostino RB, Levy D, et al. Prediction of coronary heart disease using risk factor categories. Circulation 1998; 97: 1837-1847.
- 19. Statistical Package for the Social Sciences, release 9.0. Chicago: SPSS Inc, 1999.
- 20. Houterman S, Boshuizen HC, Verschuren WMM, et al. Predicting cardiovascular risk in the elderly in different European countries. Eur Heart J 2002; 23: 294-300.
- 21. Clarke R, Lewington S, Youngman L, et al. Underestimation of the importance of blood pressure and cholesterol for coronary heart disease mortality in old age. Eur Heart J 2002; 23: 286-293.





Abstract
Objectives: To evaluate a Framingham risk function for coronary heart disease in an elderly Australian cohort and to derive a risk function for cardiovascular disease (CVD) in elderly Australians.
Design and setting: Analysis of data from a prospective cohort study (the Dubbo Study) in a semi-urban town (population, 34 000).
Participants: 2805 men and women 60 years and older living in the community, first assessed in 1988, and a subcohort of 2102 free of CVD at study entry.
Main outcome measures: Incidence of CVD (myocardial infarction, coronary death or stroke) over 5 and 10 years.
Results: A Framingham risk function assessing "hard" coronary heart disease (ie, myocardial infarction or coronary death) accurately predicted 10-year incidence in men and women aged 60–79 years who were free of prevalent CVD or diabetes at study entry. In a multiple logistic model, CVD incidence was significantly predicted by age, sex, taking antihypertensive medication, blood pressure, smoking, total cholesterol level and diabetes. For a given age and cholesterol level, CVD risk over 5 years was doubled in the presence of antihypertensive medication or diabetes, increased by 50% with cigarette smoking, and halved in women compared with men.
Conclusions: We have derived a simple CVD risk function specifically for elderly Australians that employs risk factors readily accessible to all medical practitioners.