The application of embryo freezing to human in-vitro fertilisation (IVF)1 has revolutionised its clinical practice and helped to convert IVF from an experimental procedure to widespread practice. In Australia, more than 7000 babies have now been born following the transfer of frozen–thawed embryos.2
A recent analysis of data from our clinic (the Monash University IVF clinic, Melbourne) showed the significant contribution made to overall pregnancy rates by the use of frozen–thawed embryos.3 The advantages of using frozen embryos rather than initiating another stimulated egg pickup cycle include greatly reduced risk, cost and effort involved.
One of the potential problems of embryo freezing is the creation of a growing bank of frozen embryos.4 In Australia and New Zealand, in 2000, there were 71 176 frozen embryos in storage.2 Many couples complete their families or cease to have treatment while they still have embryos in frozen storage.
One of the options for couples who no longer need their cryostored embryos is embryo donation. The first description of embryo donation came from our clinic in 1983,5 and reports from several other countries have followed.6,7
The use of frozen–thawed donated embryos is ideal for couples in which both partners are infertile. Embarking on embryo donation is a way of using a readily available resource — already created embryos — to help infertile couples achieve parenthood.
Our aims in conducting this study were to determine what proportion of couples donate embryos and to review the outcomes of embryo donation. We also wished to assess whether changes to Victorian legislation in 1998 (which introduced a storage time limit of five years for frozen embryos) have affected the decisions of couples relinquishing frozen embryos.
Over the 11.5 years audited, 1246 couples had completed consent forms to either donate or dispose of their frozen embryos. The total number of embryos in storage, by calendar year, is shown in Box 1. Out of an average of 93 couples (range, 16–153) discarding embryos in any one year, an average of 11 (range, 4–18) donated embryos. Of 1246 couples relinquishing embryos during the study period, 1116 (89.5%) opted to discard their embryos and 130 couples agreed to donate 425 embryos. The median storage time for donated embryos was 2.8 years (range, 0.6–12.2 years) (Box 2).
The outcomes of embryo donation are shown in Box 2. During the study period, 300 embryos were thawed for donation, with 197 (66%) embryos surviving thawing and undergoing transfer in 92 cycles for 50 recipient couples. (A transfer cycle is one in which the recipient has one or more embryos introduced at the appropriate time of her cycle.)
Sixteen pregnancies resulted from the 92 transfer cycles in 50 women (a pregnancy rate of 17.4% per transfer cycle and 32% per couple). From these pregnancies, 10 women delivered live babies at term (including one set of twins). No abnormalities were reported in the babies born.
Between January 1999 (one year after Victoria introduced legislation to limit embryo storage to a maximum of five years) and July 2002, 693 couples requested consent forms to determine the fate of their embryos. So far, 596 couples (86%) have returned their forms, of whom 525 (88%) requested disposal of all their embryos and seven (1%) stated they were still undecided. Although 64 couples (11%) indicated they would donate, only 48 (8%) have formally completed the process. Currently, 98 couples are on our waiting list to adopt embryos, the average waiting time being 3.0 years (range, 2.5–3.8 years).
The percentage of relinquishing couples who donated rather than disposed of their embryos in each biennium is shown in Box 1. This peaked at 14.0% in 1993–1994, fell to a low of 7.4% in 1999–2000, and rose slightly to 9.3% in 2001–2002.
Our pregnancy rate of 17% per transfer cycle for donated embryos is in keeping with a national pregnancy rate for frozen embryo transfers of 14.2%.2 At present there are nearly 100 couples on our waiting list to adopt embryos. However, with an average of only 10% of couples donating surplus frozen embryos (a figure that is not increasing), demand for donated embryos exceeds supply. It is too early to tell whether the 1998 legislative changes in Victoria have had any effect on couples' choices.
Published reports on the outcomes of embryo donation are limited, and most series have been small (eg, two US reports involved eight couples8 and eight donated embryos9). In one Finnish study involving 24 couples undertaking 54 treatment cycles,10 pregnancy rates ranged from 23% to 57% per cycle. Our study represents the largest series of frozen-embryo donation cycles ever reported.
Frozen embryos are obtained at great financial and emotional cost. It is well documented10-13 that the majority of couples have great difficulty coming to terms with the need to dispose of their excess frozen embryos. They often delay the decision; indeed, they may find it the most difficult decision they have ever had to make.12 Other studies have confirmed our finding that most couples dispose of their embryos rather than donate them to another couple.13,14 A Canadian survey of 51 couples found that, although a majority (73%) supported embryo donation in principle, only 12% indicated a "definite interest in donating".14
In Australia, although there are no specific laws about embryo donation, there is legislation relating to storage of embryos and identification of donors.
The National Health and Medical Research Council (NHMRC)15 and the Reproductive Technology Accreditation Committee of the Fertility Society of Australia16 both recommend a 10-year limit on embryo storage. Individual States vary in their requirements (Box 3). A confusing paradox in the Victorian legislation is that freshly created embryos are not allowed to be discarded after syngamy (which occurs about 21 hours after insemination), yet five years later they are compulsorily discarded if the couple does not wish to use or donate them.
Regarding the identification of donors, the NHMRC's Ethical guidelines on assisted reproductive technology state that children born as a result of assisted reproductive technology procedures are entitled to know the identity of their biological parents.15 In Victoria, when such children reach 18 years of age, they can access identifying information on the donors. However, in other States, children have no access to identifying information without the donors' permission.
The Code of Practice of the Fertility Society of Australia requires appropriate educative and psychological counselling for all donors and recipients of embryos, with ongoing counselling for recipient families.16 However, there seems to be no consensus on the degree of screening a couple should undergo before being provided with donated embryos.4 For some clinicians, counselling for couples requesting embryo donation is sufficient, while others would prefer to follow the adoption model, which involves extensive screening of couples wishing to adopt. This would reassure the relinquishing couple that their embryos would be given to an appropriate couple.4
Some studies have considered the emotional barriers to embryo donation.9,10,12,17 Having a child through IVF appears to influence parents' subsequent attitudes to their remaining embryos, so that they become less willing to donate them. They do not want to consider full siblings of their existing children living with other families, or the risk of unwitting sibling intermarriage. The uncertainty of not knowing whether they have other genetic offspring, and how this might affect their own future and that of their children, is unacceptable to them.
Clinicians need to raise embryo donation as a possible option, perhaps using educational programs, while media coverage of the issues can educate the general public. The timing of this "education" may also be important. In a study of couples' attitudes to embryo disposition after IVF,18 52 couples with frozen embryos stored for an average of 4.5 years were interviewed. The most interesting finding was that, for couples who had made a choice both before and after treatment about disposition, only 29% kept the same choice.
Although not everyone in the community approves of embryo donation and adoption, if both the relinquishing and adoptive couples are comfortable with the arrangement it is a cost-effective use of a valuable resource.
1: Frozen embryos at Monash University in-vitro fertilisation clinic, 1991–2002
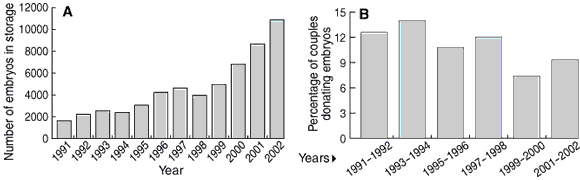
A: Number of frozen embryos in storage. B: Percentage of couples relinquishing frozen embryos who agree to donate them.
2: The destiny of frozen embryos stored at Monash University in-vitro fertilisation clinic, 1991–2002
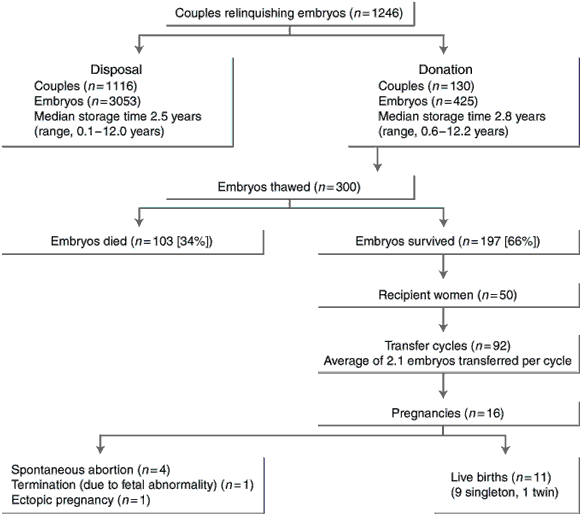
3: Storage of embryos: legislation in different States
Victoria (Infertility Treatment Act 1995) |
Five-year limit for storage, with some provision for extension |
South Australia (Reproductive Technology Act 1988) |
Ten-year limit for storage, with no provision for extension |
Western Australia (Human Reproductive Technology Act 1991) |
Consent for storage to be renewed every three years, with maximum of 15 years' storage |
Northern Territory |
Guided by South Australian legislation |
Other states |
National Health and Medical Research Council15 and Reproductive Technology Accreditation Committee16 guidelines; maximum of 10 years' storage |
- 1. Trounson A, Mohr L. Human pregnancy following cryopreservation, thawing and transfer of an eight cell embryo. Nature 1983; 305: 707-709.
- 2. Hurst T, Lancaster P. Assisted conception Australia and New Zealand 1999 and 2000. Sydney: Australian Institute of Health and Welfare National Perinatal Statistics Unit and Fertility Society of Australia, 2001. Available at: http://www.npsu.unsw.edu.au/Publications.htm (accessed Nov 2002).
- 3. Kovacs GT, MacLachlan V, Breheny S. What is the probability of conception for couples entering an IVF program? Aust N Z J Obstet Gynaecol 2001; 41: 207-209.
- 4. Saunders DM, Bowman MC, Grierson A, Garner F. Frozen embryos: too cold to touch? The dilemma ten years on. Hum Reprod 1995; 10: 3081-3085.
- 5. Trounson A, Leeton J, Besanko M. Pregnancy established in an infertile patient after transfer of a donated embryo fertilised in vitro. BMJ 1983; 286: 835-838.
- 6. Devroey P, Camus M, van den Abbeel E, et al. Establishment of 22 pregnancies after oocyte and embryo donation. Br J Obstet Gynaecol 1989; 96: 900-906.
- 7. Chan CL, Kumar J, Ong ML, et al. The first frozen embryo pregnancy for hypergonadotrophic hypogonadism in Singapore — hormonal profile and obstetric outcome. Med J Malaysia 1996; 51: 482-484.
- 8. Van Voorhis BJ, Grinstead DM, Sparks AET, et al. Establishment of a successful donor embryo program: medical, ethical, and policy issues. Fertil Steril 1999; 71: 604-608.
- 9. Lindheim SR, Sauer MV. Embryo donation: a programmed approach. Fertil Steril 1999; 72: 940-941.
- 10. Söderström-Antilla V, Foudila T, Ripatti UR, et al. Embryo donation: outcome and attitudes among embryo donors and recipients. Hum Reprod 2001; 16: 1120-1128.
- 11. McMahon CA, Gibson FL, Leslie GI, et al. Emerging IVF families: siblings, setbacks and embryo dilemmas. Planning and proceedings of the 11th World Congress on In Vitro Fertilization and Human Reproductive Genetics, 9–14 May 1999, Sydney. Sydney: Parthenon, 1999.
- 12. McMahon CA, Gibson F, Cohen J, et al. Mothers conceiving through invitro fertilization: siblings, setbacks, and embryo dilemmas after five years. Reprod Technol 2000; 10: 131-135.
- 13. Hounshell CV, Chetkowski RJ. Donation of frozen embryos after in vitro fertilization is uncommon. Fertil Steril 1996; 66: 837-838.
- 14. Newton CR, McDermid F, Tekpetey F, et al. Embryo donation: attitudes to donation procedures and factors predicting willingness to donate. Fertil Steril 2001; 76: S27.
- 15. Ethical guidelines on assisted reproductive technology. Canberra: National Health and Medical Research Council, Commonwealth of Australia, 1996: section 3.1.5.
- 16. Reproductive Technology Accreditation Committee. Code of practice for centres using assisted reproductive technology. Sydney: Fertility Society of Australia, 2002: 34.
- 17. Hammarberg K, Oke EK. The impact of changing legislation on couples with embryos frozen in excess of five years. 16th Annual Meeting of the European Society for Human Reproduction and Embryology, 25–28 June 2000, Bologna, Italy. (Abstract P-251)
- 18. Klock SC, Sheinin S, Kazer R. Couples' attitudes regarding embryo disposition after in vitro fertilization (IVF). Fertil Steril 2001; 76: S25.





Abstract
Objectives: To review the choices of couples relinquishing frozen embryos and the outcomes of embryo donation at a major in-vitro fertilisation (IVF) clinic.
Design and setting: Retrospective audit of 11.5 years of data (1991–2002) from the Monash University IVF clinic, Melbourne.
Participants: Couples who make decisions regarding the fate of their frozen embryos, and recipient couples taking part in embryo adoption.
Main outcome measures: Couples' choices with regard to the fate of their frozen embryos, and the outcome of donated embryo treatment cycles.
Results: Of 1246 couples relinquishing frozen embryos, 1116 (89.5%) opted to discard rather than donate their embryos. Sixty-six per cent of donated embryos survived thawing. From donated-embryo transfer to 50 women in 92 cycles, a 17.4% pregnancy rate per transfer cycle was achieved, and 10 women delivered 11 healthy babies at term. At the time of our audit there were 98 couples on the waiting list to adopt embryos.
Conclusions: It is worth considering how couples can be encouraged to donate rather than discard their surplus frozen embryos. An educational program on relevant legal, social and clinical issues may facilitate this.