A 55-year-old taxi driver presented with a three-week history of intermittent sore throat associated with fever and rigors, which responded to paracetamol. On the morning of admission, he woke with severe aching pain in the left groin radiating to the scrotum, with associated vomiting, fever and rigors. There were no urinary symptoms and he had not had any recent new sexual contacts. His medical history included uncomplicated haemochromatosis only.
Examination revealed a temperature of 39.6°C and sinus tachycardia. Otorhinopharyngeal, parotid and abdominal examinations were normal. Scrotal examination revealed a 4 cm, hot, swollen, erythematous area, with tenderness in the left epididymis and left testis.
The results of investigations, including streptococcal serology (confirming recent infection) and ultrasound imaging, are shown in Box 1 and Box 2. Urine microscopy and culture were negative. Streptococcus pyogenes susceptible to penicillin was isolated from both aerobic and anaerobic blood culture bottles at 24 hours. Polymerase chain reaction tests of urine were negative for Neisseria gonorrhoeae and Chlamydia trachomatis.
Despite commencement of intravenous penicillin, the patient required incision and drainage of the scrotum on Day 4. He was discharged from hospital nine days after presentation on a two-week course of oral amoxycillin and made a full recovery.
Epididymo-orchitis can result from bacterial or viral infections. Predisposing trauma may be identified, but the majority of cases appear to be idiopathic.
Different types of causative bacteria occur more frequently in certain age groups: 1,2 for example, urinary tract pathogens (eg, Escherichia coli, Proteus mirabilis, Enterobacter spp.) in men over 35 years; sexually acquired pathogens (eg, N. gonorrhoeae, C. trachomatis) in sexually active men under 35 years; and pathogens acquired as part of a systemic infection (eg, Haemophilus influenzae, N. meningitidis, Mycobacterium tuberculosis) in preadolescent boys.
In a few rare cases,1-3 streptococcal infections have been found to cause epididymo-orchitis as part of a local infection. However, all these cases occurred in preadolescent boys. There has been one report of a 17-year-old man with invasive group A streptococcal infection of the scrotum in the context of streptococcal toxic shock syndrome.4 Our case is unusual in that it occurred as a systemic illness in a 55-year-old man with haemochromatosis. This infection has not, to our knowledge, been previously described in association with haemochromatosis.5
1: Investigations
Value |
Reference range |
||||||||||
Neutrophils |
11.4 x 109/L |
1.0–7.0 x 109/L |
|||||||||
C-reactive protein |
98 mg/L |
< 3 mg/L |
|||||||||
Ferritin |
205 μg/L |
20-300 μg/L |
|||||||||
% Transferrin saturation |
45% |
20%–52% |
|||||||||
Streptococcal exotoxin |
|||||||||||
AntiDNase B |
> 2560 |
< 320 |
|||||||||
Antistreptokinase |
> 20480 |
< 2560 |
|||||||||
Antistreptolysin O |
> 1200 |
< 300 |
|||||||||
2: Scrotal ultrasound images
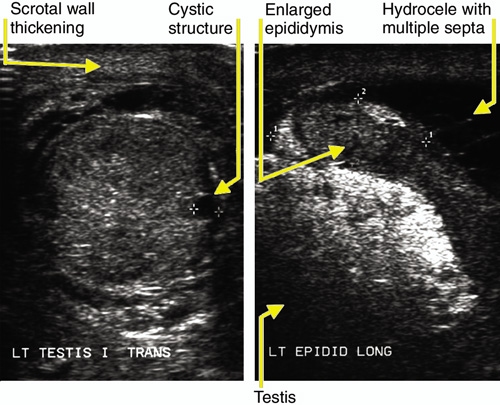
Left: Transverse image of the enlarged left testis (4.5 x 3 x 2 cm), with non-homogeneous echotexture and several small, rounded, echolucent cystic structures within the testis measuring 3 mm in diameter. The right testis showed similar, but less severe, features.
Right: Longitudinal image of the enlarged left epididymis.
- Sebastiaan J van Hal1
- Robyn P Hardiman2
- Department of Infectious Diseases, Prince of Wales Hospital, Randwick, NSW.
- 1. Ireton RC, Berger RE. Prostatitis and epididymitis. Urol Clin North Am 1984; 11: 83-94.
- 2. Kaver I, Matzkin H, Braf ZF. Epididymo-orchitis: A retrospective study of 121 patients. J Fam Pract 1990; 30: 548-552.
- 3. Teel LD, Shemonsky NK, Aronson N. Group G streptococcal bacteremia in a healthy young man. South Med J 1989; 82: 633-634.
- 4. Walker BR, Pribble CG, Cartwright PC. Invasive group A Streptococcus infection of the scrotum and streptococcal toxic shock syndrome. J Urol 2000; 56: 669-670.
- 5. Jurado RL. Iron, infections and anemia of inflammation. Clin Infect Dis 1997; 25: 888-895.




