Psychological morbidity, especially depression, is common in women in the year after childbirth.1 Many mothers perceive their experience of childbirth as traumatic,2 and this appears to increase their risk of psychological disorders, including stress disorders.2,3 This occurs whether or not labour was complicated or prolonged, or delivery was operative.4,5 Psychological outcome appears to depend on women's subjective, as well as objective, experiences.6 This has led to the introduction of debriefing after childbirth in Australian and overseas hospitals to reduce psychological morbidity.
However, two recent trials of unstructured debriefing by midwives after childbirth had conflicting results, one finding positive effects on psychological outcome7 and the other negative effects.8 Critical incident stress debriefing is a structured form of debriefing, generally comprising a single, brief, standardised intervention to facilitate the ventilation and normalisation of reactions to traumatic stimuli. It is designed to reduce the incidence of long-term adverse psychological outcomes, especially stress disorders but including anxiety and depression, in victims of traumatic events.9
We undertook a randomised single-blind controlled trial to assess whether a short session of critical incident stress debriefing led by a midwife reduces the incidence of postnatal psychological disorders in women who have recently given birth. To our knowledge, this is the first trial to investigate the effect of critical incident stress debriefing on postnatal psychological disorders.
Women in the intervention group received a single, standardised debriefing session in their hospital rooms immediately after randomisation or the next day. Debriefing used the seven key stages from the critical incident stress debriefing model of Mitchell,9 adapted for use in individual sessions with women in the postpartum period (Box 1). Duration ranged from 15 minutes to 1 hour. All research midwives received training in critical incident stress debriefing. The control group received standard postnatal care.
Psychological outcomes were determined in two stages. Firstly, women were mailed self-report questionnaires containing the Impact of Event Scale — Revised10 and the Edinburgh Postnatal Depression Scale (EPDS)11 at 2, 6 and 12 months postpartum.
In the two weeks after each questionnaire, selected women were interviewed by research clinical psychologists using a standardised psychological interview, the Schedule for Affective Disorders and Schizophrenia (SADS).12 Interviews also included open-ended questions about depressive symptoms and a clinician-administered scale for acute and chronic post-traumatic stress disorders.13 Research psychologists were trained in the structured interview techniques during a pilot study.
Women selected for interview at each follow-up comprised:
Women selected for interview at any follow-up were also interviewed at subsequent follow-ups, using a structured interview schedule (Streamlined Longitudinal Interval Continuation Evaluation14) designed to detect psychological symptoms that emerged between assessments.
Women who failed to return a questionnaire were contacted by telephone up to three times, while those who failed to return any questionnaires were, if possible, interviewed by telephone at about 12 months postpartum.
All researchers except the research midwife were blinded to the women's group allocation. Clinical psychologist interviewers were blinded to questionnaire scores and group allocation.
The primary outcome was a diagnosis of major depression, minor depression with significantly depressed mood and functional impairment, or post-traumatic stress disorder, with onset in the 12 months after delivery, using criteria of the Diagnostic and statistical manual of mental disorders, 4th edition (DSM IV).15 All women meeting criteria for any disorder were directed to professional help.
Data were analysed on an intention-to-treat basis using SAS statistical package version 6.12.16 Baseline comparisons were made using Fisher's exact test for categorical variables, t test for normally distributed variables, and the Wilcoxon rank sum test for those with non-parametric distributions. Psychological outcomes were compared using Fisher's exact test, and onset and duration of depression using Kaplan–Meier survival analysis. Mixed model repeated measures analysis of variance was used to analyse EPDS scores over time. It was decided a priori that a subset analysis for those who had an unplanned operative delivery would also be conducted. The null hypothesis was that there was no difference in the incidence of depression between the two groups.
There were no significant differences between the groups for any demographic or obstetric factor (age, educational, socioeconomic, marital and health insurance status, planned pregnancy, assisted pregnancy, parity, induced labour, duration of first and second stages of labour, mode of delivery, analgesia during labour or birth, gestational week, birth weight and twins). There were also no differences in history of psychological treatment or feelings about the labour and birth (Box 2). Neutral or negative feelings were reported by 26.5%, with 31.5% stating the birth experience did not meet their expectations, and 13.5% reporting poor pain control.
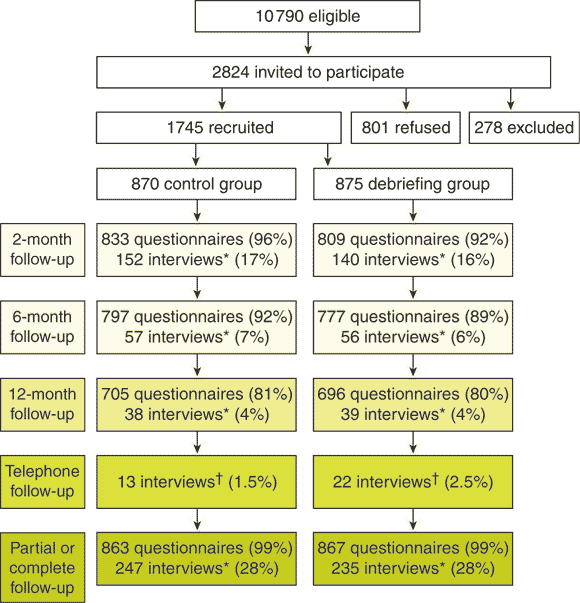
Partial or complete follow-up information was available for 1730 women (99.1%), with 482 of these undergoing a SADS interview (Box 3).
There were no significant differences between the groups in any outcome measure at any follow-up, including scores on the EPDS and Impact of Event Scale.
There were also no significant differences in the proportions of women who met diagnostic criteria for a stress disorder or for major or minor depression in the year after giving birth, in either the whole group or any of the subgroups (Box 4). Kaplan–Meier survival analysis showed no difference between the groups for time to onset of depression (not shown). Median time to onset was 6 weeks in the debriefing group (interquartile range [IQR], 4–9 weeks) versus 4 weeks in the control group (IQR, 3–8 weeks) (P = 0.84). Duration of depressive episodes was also similar in the groups — 24 weeks in the debriefing group (IQR, 12–46 weeks) versus 22 weeks in the control group (IQR, 10–52 weeks) (P = 0.98).
Two-thirds of women rated the debriefing session as moderately or greatly helpful, 23% as minimally helpful, and 10% as not at all helpful.
In contrast, two previous trials of debriefing after childbirth found positive and negative effects, respectively.7,8 Both used unstructured debriefing by midwives. A trial in primiparous women with normal births reported a reduction in anxiety and depression at three weeks postpartum,7 but did not assess longer-term outcomes. Another trial in women with operative births found a higher prevalence of depressive symptoms six months postpartum in those who were debriefed (measured by self-report questionnaires).8
In those trials, midwives listened to women talk about their experiences in unstructured sessions. In contrast, we used a clearly defined, standardised intervention based on the principles of critical incident stress debriefing. While the previous trials used screening self-report questionnaires on one postpartum occasion for diagnosis, which may have missed disorders, we used a rigorous, standardised clinical assessment performed three times over a year. For over a quarter of women, this included a structured diagnostic psychological interview, which is far more robust in assessing psychological morbidity. These measures have been extensively validated and can provide an accurate time of onset and duration.
Our finding that critical incident stress debriefing does not prevent or reduce postnatal psychological morbidity is compatible with the results of most randomised controlled trials of its effects in non-obstetric trauma.17-19 Indeed, some trials have reported adverse effects,17,20 as did one of the trials of unstructured debriefing after childbirth.8 However, in our study, repeated follow-up over a year found no evidence of such adverse outcomes. Despite the lack of effect of debriefing, most women in our study rated it as helpful or very helpful. It may thus play a role in the natural psychological processing of events around the birth.
Why did our intervention have no effect? We used an accepted debriefing format.9,21 While some may argue that psychiatric nurses could have provided more effective and skilled intervention than midwives, our research midwives were experienced practitioners and had extensive training in structured debriefing. Only one session was offered, and it is possible that extra sessions targeted to those with more negative experiences might have had positive results, even though we showed no effect in subgroup analyses.2
Was our follow-up appropriate? We believe that it was sufficiently long to identify any effects of the intervention.22 It was not feasible to interview the entire study cohort. Although our method of selecting women for interview may have missed some women with psychological morbidity, this is unlikely to have biased our findings as it should have occurred randomly in both arms of the trial.
Is giving birth a traumatic event? A recent study of 500 Queensland women who had just given birth found that a third reported a traumatic birthing event and had acute trauma symptoms.2 Clinicians may not appreciate that a woman's subjective perception matters as much as the clinician's objective assessment.2,6 This has led to the interest in debriefing after delivery in non-selected populations.
Our study confirms a high prevalence of depression in Australian women in the year after childbirth. When women are included who are not eligible for our intervention because of current psychological treatment, then more than one in five children have a principal caregiver who may be depressed for significant periods of their first year of life. Given the critical nature of the early attachment period, this has major public health implications.23 We must continue to develop and test interventions that reduce, or identify early, psychological morbidity in women after giving birth, and encourage and facilitate early and effective treatment.
1: Phases of the critical incident stress debriefing procedure
Midwife described the debriefing process.
Relating the birth experience (eg, What happened when your labour started?).
Describing thoughts at the time (eg, What were your main thoughts during ... ?).
Midwife emphasised the normality of the woman's response to a stressful situation.
Coping with early parenting; identifying sources of assistance if emotional problems continue.
3: Participation rates at each stage of the trial
* Number of women who underwent a SADS (Schedule for Affective Disorders and Schizophrenia)12 interview; numbers of follow-up interviews are not shown. † Modified interviews were conducted by telephone at about 12 months postpartum for women who did not respond to any questionnaires.
Received 29 August 2002, accepted 6 February 2003
- Susan R Priest1
- Jenni Henderson2
- Sharon F Evans3
- Ronald Hagan4
- Women and Infants Research Foundation, King Edward Memorial Hospital, Perth, WA.
- 1 Department of Neonatal Paediatrics, King Edward Memorial Hospital, Perth, WA.
We thank research midwives Jennie Sharpe and Leonie Batson, research psychologists Anne St Jack and Senia Malmgren, Colleen Ryan, who entered the data, and the trial participants. This study was supported by a grant from the National Health and Medical Research Council.
None identified.
- 1. Cooper PJ, Campbell EA, Day A, et al. Non-psychotic psychiatric disorder after childbirth — a prospective study of prevalence, incidence, course and nature. Br J Psychiatry 1988; 152: 799-806.
- 2. Creedy DK, Shochet IM, Horsfall J. Childbirth and the development of acute trauma symptoms: incidence and contributing factors. Birth 2000; 27: 104-111.
- 3. Ballard CG, Stanley AK, Brockington IF. Post-traumatic stress disorder (PTSD) after childbirth. Br J Psychiatry 1995; 166: 525-528.
- 4. Astbury J, Brown S, Lumley J, Small R. Birth events, birth experiences and social differences in postnatal depression. Aust J Public Health 1994; 18: 176-184.
- 5. Fisher J, Astbury J, Smith A. Adverse psychological impact of operative obstetric interventions: a prospective longitudinal study. Aust N Z J Psychiatry 1997; 31: 728-738.
- 6. Green JM, Coupland VA, Kitzinger JV. Expectations, experiences, and psychological outcomes of childbirth: a prospective study of 825 women. Birth 1990; 17: 15-24.
- 7. Lavender T, Walkinshaw SA. Can midwives reduce postpartum psychological morbidity? A randomized trial. Birth 1998; 25: 215-219.
- 8. Small R, Lumley J, Donohue L, et al. Randomised controlled trial of midwife led debriefing to reduce maternal depression after operative childbirth. BMJ 2000; 321: 1043-1047.
- 9. Mitchell J. When disaster strikes. The Critical Incident Stress Debriefing Process. J Emerg Med Services 1983; 8: 36-39.
- 10. Weiss DS, Marmar CR. The Impact Of Event Scale–Revised. In: Wilson JP, Keane TM, editors. Assessing psychological trauma and PTSD. New York: USA Guildford Press 1997: 399-411.
- 11. Cox JL, Holden JM, Sagovsky R. Detection of postnatal depression. Development of the 10-item Edinburgh Postnatal Depression Scale. Br J Psychiatry 1987; 150: 782-786.
- 12. Endicott J, Spitzer R. A diagnostic interview — The Schedule For Affective Disorders And Schizophrenia. Arch Gen Psychiatry 1978; 35: 837-844.
- 13. Blake DD, Weathers FW, Nagy LM, et al. The development of a clinician-administered PTSD scale. J Traumatic Stress 1995; 8: 75-90.
- 14. Keller MB, Lavori PW, Friedman B, et al. The longitudinal interval follow-up evaluation. Arch Gen Psychiatry 1987; 44: 540-548.
- 15. American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4th ed. Washington: American Psychiatric Association, 1994.
- 16. SAS statistical package, version 6.12. Cary, NC: SAS Institute, 1998.
- 17. Wessely S, Bisson J. Brief psychological interventions ("debriefing") for trauma-related symptoms and prevention of post traumatic stress disorder. Cochrane Review. The Cochrane Library, Issue 1, 2001. Oxford: Update Software, 2001.
- 18. van Emmerik AAP, Kamphuis JH, Hulsbosch AM, Emmelkamp PMG. Single session debriefing after psychological trauma: a meta-analysis. Lancet 2002; 360: 766-771.
- 19. Rose S, Bisson J. Brief early psychological interventions following trauma: a systematic review of the literature. J Traumatic Stress 1998; 11: 697-710.
- 20. Carlier IVE, Voerman AE, Gersons BPR. The influence of occupational debriefing on post-traumatic stress symptomatology in traumatized police officers. Br J Med Psychol 2000; 73: 87-98.
- 21. Dyregrov A. The process in psychological debriefings. J Trauma Stress 1997; 10: 589-605.
- 22. O'Hara MW, Swain AM. Rates and risks of postpartum depression — a meta-analysis. Int Rev Psychiatry 1996; 8: 37-54.
- 23. Laucht M, Esser G, Schmidt MH. Differential development of infants at risk of psychopathology: the moderating role of maternal responsivity. Dev Med Child Neurol 2001; 43: 292-300.





Abstract
Objective: To test whether critical incident stress debriefing after childbirth reduces the incidence of postnatal psychological disorders.
Design: Randomised single-blind controlled trial stratified for parity and delivery mode.
Setting: Two large maternity hospitals in Perth.
Participants: 1745 women who delivered healthy term infants between April 1996 and December 1997 (875 allocated to intervention and 870 to control group).
Intervention: An individual, standardised debriefing session based on the principles of critical incident stress debriefing carried out within 72 hours of delivery.
Main outcome measures: Diagnosis of stress disorders or depression in the 12 months postpartum, using structured psychological interview and criteria of the Diagnostic and statistical manual of mental disorders, 4th edition.
Results: Follow-up information was available for 1730 women (99.1%), 482 of whom underwent psychological interview. There were no significant differences between control and intervention groups in scores on Impact of Events or Edinburgh Postnatal Depression Scales at 2, 6 or 12 months postpartum, or in proportions of women who met diagnostic criteria for a stress disorder (intervention, 0.6% v control, 0.8%; P = 0.58) or major or minor depression (intervention, 17.8% v control, 18.2%; relative risk [95% CI], 0.99 [0.87–1.11]) during the postpartum year. Nor were there differences in median time to onset of depression (intervention, 6 [interquartile range, 4–9] weeks v control, 4 [3–8] weeks; P = 0.84), or duration of depression (intervention, 24 [12–46] weeks v control, 22 [10–52] weeks; P = 0.98).
Conclusions: There is a high prevalence of depression in women during the first year after childbirth. A session of midwife-led, critical incident stress debriefing was not effective in preventing postnatal psychological disorders, but had no adverse effects.