The Thoracic Society of Australia and New Zealand developed the Asthma Management Plan to assist health professionals and patients with the management of asthma.1 This was followed by the introduction of the National Asthma Campaign (NAC) in 1990, which promoted asthma education and the use of the Asthma Management Plan to health professionals and people with asthma.1 A key aspect of this management plan was the development of an action plan to enable patients with asthma to recognise deterioration in their condition and worsening of symptoms, especially wakening at night, and to control worsening symptoms. The NAC also developed policy on asthma-related issues, conducted epidemiological surveys on asthma and identified issues for future action.2
Given that it is now over a decade since this initiative was introduced, it is appropriate to evaluate its impact on patients with asthma. We aimed to examine trends in asthma since 1990 and the uptake of the asthma action plans in South Australia since 1992.
The data for this survey were collected in the South Australian Health Omnibus Survey (SAHOS) between 1990 and 2001. The SAHOS methods are documented in detail elsewhere.3
Briefly, the sample for the survey was obtained by multistage, systematic clustered area sampling of people aged 15 years or older who live in South Australia. People in a random sample of Australian Bureau of Statistics collector districts were surveyed. Within each collector district, a random starting point was selected, and from this point 10 households were selected using a fixed skip interval. Hotels, motels, hospitals, nursing homes and other institutions were excluded. The person whose birthday was next in each selected household was interviewed by trained health interviewers. Up to five call-backs were made in an attempt to interview the selected person. There were no replacements for non-respondents.
The smallest sample used over the years of collecting asthma data was 2559 in 1990 (the first year of the SAHOS). Since then, the minimum sample size was 3010 in 1998 and the maximum was 3379 in 1991. The response rate for each survey has been in excess of 70%. For reliability purposes, 5% of each interviewer's work was selected for re-interview on selected questions. Data obtained in each year were weighted to correspond with the age, sex and geographical profile from the nearest Census data collection, to provide estimates that were representative of the South Australian population for each year.
Participants were asked if they had ever had asthma, whether a doctor had confirmed their asthma and if they still had asthma. Those who answered yes to all three questions were considered to have doctor-diagnosed current asthma, and were asked if they had an asthma action plan, defined as written instructions about what to do if their asthma is out of control (requiring a yes or no response). To estimate morbidity, from 1994 to 2001, people were also asked: "In the last twelve months have you lost any days from work, school or home duties or usual activities from asthma?", and "How often do you waken during the night with asthma?"
Following weighting as described, data were analysed using SPSS Version 10.4 Prevalence estimates (and confidence intervals) were calculated for each year. Differences between proportions were calculated by means of the χ2 test.
The Box (Figure a) shows that the prevalence of self-reported diagnosed asthma increased from 8% (95% CI, 6.4%–9.6%) in 1990 to a high of 12.8% (95% CI, 11.4%–14.2%) in 2001. This increasing trend is statistically significant (χ2 trend, 63.8; df, 9; P < 0.001). Figure b shows that 21.9% (95% CI, 19.8%–24.6%) of those with asthma reported having an asthma action plan in 1992, when asthma action plans were promoted. This rose to a peak of 42.3% (95% CI, 40.3%–44.3%) in 1995, but declined to 22.2% (95% CI, 20.7%–23.7%) in 2001.
Further analyses of the data showed that the prevalence of asthma in males had risen from 7.8% in 1992 to 9.8% in 2001 (P < 0.05), and from 10.7% to 15.3% for females (P = 0.06) over the same period. The proportion of patients who had action plans increased over the period for males (from 17.9% to 21.9%; P < 0.0001) and declined for females (from 24.7% to 22.3%), although this difference was not significant (P = 0.09). In terms of wakening at night weekly or more frequently, male prevalence declined from 21.9% in 1995 to 16.7% in 2001 (P = 0.004). Over the same period, the prevalence of wakening among females increased from 11.5% to 15.4% (P = 0.0007).
It can be seen from Figure c that morbidity, as measured by wakening nightly or weekly, and by days lost from work or normal activity, remained fairly constant.
Our study is limited by the fact that it was a self-report study of asthma prevalence and related information. However, a major advantage is the representative population sample which increases confidence in the external validity of our results.
Our finding of increasing prevalence of asthma in the first half of the 1990s is contemporaneous with the introduction of the National Asthma Campaign. As this was the major asthma initiative of the decade, the apparent increase in asthma prevalence may be the result of heightened awareness and vigilance on the part of patients and physicians. Our findings may simply reflect an increased number of patients with possible asthma presenting to doctors, thus increasing the detection rate.
We found that morbidity associated with asthma, indicated by night-time wakening either nightly or weekly, and days lost from usual activities, remained fairly constant. In two previous studies, nocturnal symptoms were described, respectively, as the dominant symptom in asthma severity,5 and an important marker of asthma severity.6 Days lost from work and usual activities because of asthma have also been identified as an important indicator of morbidity.7 It is important to note that the rate of ownership of asthma action plans during the decade appears to have had little effect on morbidity.
Over the entire study period, asthma prevalence increased by 38%, while morbidity (especially wakening at night) remained fairly constant. This means that the community burden of asthma has increased, and implies that this is not simply the result of more mild cases being diagnosed.
The fact that the percentage of patients with asthma who had asthma action plans was the same in 2001 as in 1992, when they were introduced, is a disappointing statistic. The results of this survey are supported by those of the Asthma in America study,8 which identified that while 70% of doctors say they prepare an action plan for all, most, or some of their patients with asthma, only 27% of patients say their doctor has developed an action plan. In an Australian pilot survey of 17 general practices, Collins et al showed that 48% of patients with asthma had a record on their charts that they had been given a written action plan.9 However, in a national survey, Bauman et al found that only 9% of patients had a written plan of action for asthma, but concluded that data from patient surveys may underestimate clinical practice.10
The fact that the written asthma action plan is an important and effective educational tool has been strongly demonstrated by Gibson et al.11 In a Cochrane review of asthma education programs, they showed that training in asthma self-management, which includes a written asthma action plan, improved health outcomes for adults with asthma. They also concluded that asthma plans enabling people to adjust their medication dosages by following a written action plan appeared to be more effective than other forms of self-management.
The National Asthma Council must persist with developing and promoting guidelines and action plans if improved asthma health outcomes are to be achieved. It must also investigate the reasons why we have such a low current prevalence of written action plans among patients with asthma, and introduce any necessary additional measures to redress this deficit.
Prevalence of doctor-diagnosed asthma, asthma management plans and asthma symptoms in South Australia during the study period
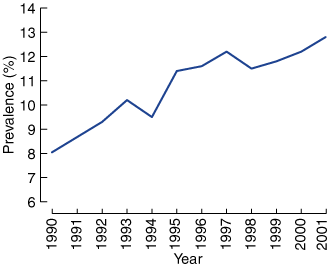
(a) Prevalence of asthma in South Australia, 1990–2001.
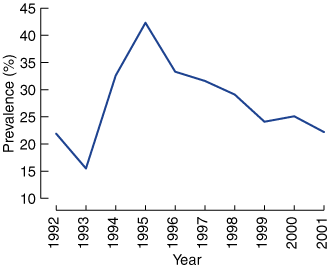
(b) Prevalence of asthma management plans in South Australia, 1992–2001.
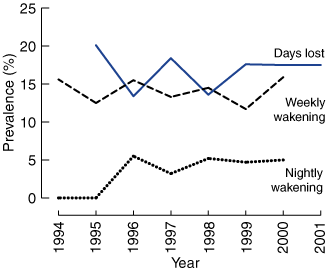
(c) Prevalence of days lost from usual activities and daily or weekly night time wakening with asthma symptoms for those with asthma, 1994–2001.
Received 6 November 2002, accepted 24 February 2003
- David H Wilson1
- Robert J Adams2
- Sarah L Appleton3
- Graeme Hugo4
- Janet Hiller5
- Philip Ryan6
- Richard E Ruffin7
- David Wilkinson8
- Julianne Cheek9
- 1 University of Adelaide, Adelaide, SA.
- 2 University of South Australia, Adelaide, SA.
R Ruffin has received, on behalf of the Adelaide University, honoraria from AstraZeneca, GlaxoSmithKline, Merck Sharp & Dohme and 3M Pharmaceuticals for participation on advisory boards and educational programs.
- 1. Woolcock A, Rubinfeld AR, Seale JP, et al. Thoracic Society of Australia and New Zealand. Asthma management plan, 1989. Med J Aust 1989; 151: 650-653.
- 2. National Asthma Campaign. National asthma strategy implementation plan. Melbourne: National Asthma Campaign Ltd, 1999.
- 3. Wilson DH, Wakefield M, Taylor AW. The South Australian Health omnibus survey. Health Promotion J Aust 1992; 2: 47-49.
- 4. Statistical package for the social sciences [computer program]. Version 10. Chicago: SPSS Inc., 2002.
- 5. Fix A, Sexton M, Langenberg P, et al. The association with nocturnal asthma with asthma severity. J Asthma 1997; 34: 329-336.
- 6. Colice GL, Vanden Burgt J, Song J, Thompson PJ. Categorising asthma severity. Am J Respir Crit Care Med 1999; 160: 1962-1967.
- 7. Campbell DA, Yellowlees PM, McLennan G, et al. Psychiatric and medical features of near fatal asthma. Thorax 1995; 50: 254-259.
- 8. GlaxoSmithKline. Asthma in America — executive summary. Washington DC: Glaxo Welcome Inc., 1998.
- 9. Collins S, Beilby J, Fardy J, et al. The national asthma audit. Bridging the gap between guidelines and practice. Aust Fam Physician 1998; 10: 907-913.
- 10. Bauman A, Cooper C, Bridges-Webb C, et al. Asthma management and morbidity in Australian general practice: the relationship between patient and doctor estimates. Respir Med 1995; 89: 665-672.
- 11. Gibson PG, Coughlan J, Wilson AJ, et al. Self-management education and regular practitioner review for adults with asthma. Cochrane Database Systematic Reviews 2000; (2): CD001117.





Abstract
Objectives: To assess trends in the prevalence of self-reported doctor-diagnosed asthma, associated asthma related morbidity, and the uptake of written asthma action plans in South Australia, 1990–2001.
Design, setting and participants: Surveys by telephone interview of the South Australian population between 1990 and 2001, and interview of participants in their own homes by trained health interviewers.
Main outcome measures: Asthma prevalence, percentage of patients with written action plans, and asthma associated morbidity.
Results: The reported prevalence of doctor-diagnosed asthma has increased from 8% (95% CI, 6.4%–9.6%) in 1990 to 12.8% (95% CI, 11.4%–14.2%) in 2001. Morbidity, as measured by wakening at night (daily or weekly) and days lost from normal activities because of asthma, has remained constant over the decade. The percentage of patients with written asthma action plans increased to a peak of 42.3% (95% CI, 40.3%–44.3%) in 1995, but then declined to 22.2% (95% CI, 20.7%–23.7%) in 2001.
Conclusions: The prevalence of asthma has increased while morbidity has remained constant, indicating that the burden of asthma has increased. The associated decline in the percentage of patients with asthma action plans in recent years is cause for concern.