Jellyfish stings in northern Australia cause significant morbidity and mortality. Since early descriptions of Irukandji syndrome,1,2 relatively little further knowledge has been gained about it. Although Carukia barnesi has been shown to cause the syndrome,3 other species of jellyfish are also suspected to be responsible.3-7
We hypothesise, firstly, that many different cubozoans may produce Irukandji syndrome in Cairns, and secondly, that these different species of jellyfish may be responsible for different severities of this syndrome.
All patients with a discharge diagnosis of "marine stings" (ICD-10 code T63.6)8 after presenting to Cairns Base Hospital, Queensland, between 1 July 2001 and 30 June 2002 were retrospectively identified from the emergency department computer database, and epidemiological and clinical data were extracted and entered on a standardised form. Details collected included geographic location of sting, physiological parameters, analgesia required, biochemical abnormalities, electrocardiographic and echocardiographic findings.
We assessed the clinical severity of each patient's condition at presentation according to peak systolic blood pressure, total opioid dose administered, peak troponin I level, and length of hospital stay. As individual patients received either morphine, pethidine or fentanyl according to clinician preference, we arbitrarily converted their opioid dose to "morphine equivalents" (where 1 mg morphine = 10 mg pethidine = 10 μg fentanyl) to give a rough comparison of analgesic requirements between patients.
From 1 July 2001 to 30 June 2002, 128 patients at the Cairns Base Hospital emergency department had a discharge diagnosis of marine stings. Of these, 116 had symptoms consistent with Irukandji syndrome. Sixty-seven of the 116 patients (58%) were male and their average age was 26.5 years (range, 3–63 years).
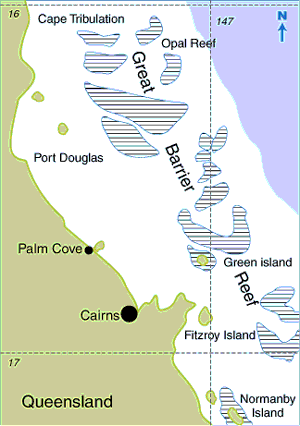
Of the 116 patients with Irukandji syndrome, 89 (7%) were stung along the shore, 26 (22%) were stung offshore (Great Barrier Reef and islands; see Box 1), and one patient did not have the location recorded.
Skin scrapings were taken from 50 patients. Of these, four patients had local symptoms only, and the remainder had symptoms consistent with Irukandji syndrome. Forty patients (80%) had positive scrapings, while, in the remainder, either no nematocysts were found or the nematocysts were too damaged to be confidently identified (positive predictive value of 80%). Thirty-nine patients had a nematocyst cnidome identifiable as Carukia barnesi; two of these experienced only a mild sting at the site, and 37 had Irukandji syndrome. Of these 39 patients, 13 had a raised cTnI level; five of these had abnormal echocardiograms and seven had abnormal ECGs. Thirty-one patients with Carukia barnesi identified on skin scrapings (79%) were stung at local mainland beaches. The rest were stung at Fitzroy Island (4), Green Island (1), and Normanby Island (1) (see Box 1).
The patient with the most severe symptoms who had Carukia barnesi identified from skin scrapings was a 44-year-old man with a peak blood pressure of 160/100 mmHg and peak cTnI level of 30.8 μg/L, who required a total morphine equivalent dose of 255 mg over five days. He had widespread T-wave inversion and ST-segment depression on his ECG. His echocardiogram showed severe left ventricular dysfunction and anteroseptal hypokinesis, with an ejection fraction of 30%–35%. Six months later his echocardiogram was completely normal.
One 44-year-old man had an unidentified cnidome on skin scraping, which is of concern, as he was one of two patients reported to have died from Irukandji syndrome (the other having occurred in the Whitsundays).9 Although some of the nematocysts identified were similar to those from Carukia barnesi, a morphologically different additional nematocyst was also present (Box 2). It is possible that this nematocyst was a "rogue" mastigmophore, and hence may be an incidental finding from another source. Alternatively, the cnidome may represent an unidentified jellyfish. The patient was stung at Opal Reef (see Box 1), had a peak blood pressure of 230/90 mmHg, peak cTnI level of 34 μg/L, and required 30 mg of morphine equivalents before being intubated for a depressed level of consciousness from an intracerebral haemorrhage.
In recent years a number of serious envenomations causing Irukandji syndrome have been described,6,10-13 all associated with cardiac failure and pulmonary oedema. However, it has been observed that most stings in the Cairns region are, in fact, mild, without serious complications, and do not require admission to hospital.4 Our study confirms this, as most patients were discharged within 24 hours of presentation.
Surprisingly, myocardial damage, as measured by an elevated cTnI level, was seen in 25 patients (22%) experiencing Irukandji syndrome. Six of these patients had echocardiographic evidence of myocardial dysfunction. It is evident that those with continuing pain and analgesic requirements are at risk of cardiac complications. Clinicians should therefore consider closely monitoring these patients with serial cTnI level measurements, and, if these are abnormal, consider echocardiographic evaluation.
Skin-scraping methods have been described for a number of jellyfish species,14-17 but, to date, there are no published data on successful identification of Carukia barnesi nematocysts in patients with Irukandji syndrome. While acknowledging some limitations, it is reasonable in this setting to equate the species identified through cnidome assessment with causation. Therefore, we can, with reasonable confidence, assert that Carukia barnesi was causative in 39 patients. We can also deduce that envenomation by this species produces a wide range in severity of illness, and that it was the only identifiable causative cuboidal jellyfish in patients stung on the Cairns beaches. We can less confidently claim that a single victim may have been stung by an unknown species of box jellyfish, ultimately leading to his death. The cnidome in this case was similar to, but with distinct differences from that of, Carukia barnesi (Box 2). We acknowledge that Carukia barnesi may have been causative in this instance, as the mastigophore isolated from this patient may have been an incidental finding. A further possibility is that the Carukia barnesi cnidome may change to include mastigophores as the animal ages or grows (as is seen with Chironex fleckeri). We are ignorant of the life cycle of Carukia barnesi, and therefore can only speculate.
There are obvious serious implications if the cnidome is that of an unidentified cuboidal jellyfish. It has long been suspected that jellyfish species other than Carukia barnesi can cause Irukandji syndrome.3-7 Case reports include a patient with severe Irukandji syndrome in whom a 2 mm length of tentacle not from Carukia barnesi was found in a skin scraping of the sting site,6 and where tentacles isolated resembled, but were distinctly different from, those of Carukia barnesi.7 Our results provide further supportive evidence that species other than Carukia barnesi may be linked to Irukandji syndrome.
Interestingly, two patients with cnidomes consistent with Carukia barnesi did not develop Irukandji syndrome. These patients had mild local symptoms only. Thus, a sting by Carukia barnesi does not necessarily result in Irukandji syndrome. Factors affecting venom load, such as thickness of the keratinised skin, presence of hair, length of tentacle involved, duration and pressure of the contact between tentacle and skin have been proposed by other authors.3,17
As only a single cnidome suggestive of a different jellyfish species was found, we can make no statistical inferences about the severity of Irukandji syndrome and the jellyfish species identified from skin scrapings. Additionally, patients were not randomly selected in terms of whether or not they would have skin scrapings performed. Thus, it is possible that more seriously affected patients would have attracted more interest and were more likely to have skin scrapings performed.
Our interpretation of these findings is based on a number of assumptions. Our conversion of "equivalent doses" of narcotics has not taken into account the differences in their duration of action. Finally, we have assumed that jellyfish (indicated by their cnidome) caused the patients' symptoms.
In conclusion, we can infer that, in patients with Irukandji syndrome, the causative jellyfish can usually be successfully identified from skin scrapings on the basis of known cnidomes. Most patients with Irukandji syndrome in the Cairns region were stung by Carukia barnesi, which has now been shown to cause illness ranging from local symptoms to severe Irukandji syndrome with cardiac dysfunction. Our finding of a cnidome that was not that of Carukia barnesi suggests that other species of jellyfish may cause Irukandji syndrome.
2: Nematocysts from Carukia barnesi compared with unidentified nematocysts from a fatal envenomation
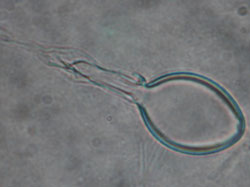 A: Discharged nematocyst from the tentacle of Carukia barnesi. |
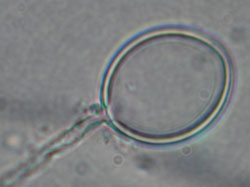 B: Discharged nematocyst from the bell of Carukia barnesi. |
||||||||||
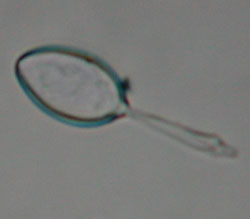 C: Discharged nematocyst from unidentified species of jellyfish (similar morphology to [A]). |
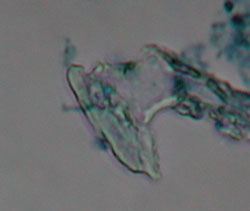 D: Cigar-shaped nematocyst from unidentified species of jellyfish. |
||||||||||
- Truc T Huynh1
- Peter Pereira2
- Richard Mulcahy3
- Paul Cullen4
- Jamie Seymour5
- Teresa Carrette6
- Mark Little7
- 1 Emergency Department, Cairns Base Hospital, Cairns, QLD.
- 2 School of Tropical Biology, James Cook University, Smithfield, QLD.
- 3 Emergency Department, Sir Charles Gairdner Hospital, Perth, WA.
None identified
- 1. Southcott RV. Fatal stings in North Queensland bathers. Med J Aust 1952; 1: 272-273.
- 2. Flecker H. Irukandji sting to North Queensland bathers without production of wheals but severe general symptoms. Med J Aust 1952; 2: 89-91.
- 3. Barnes JH. Cause and effect in Irukandji stingings. Med J Aust 1964; 1: 897-904.
- 4. Little M, Mulcahy RF. A year's experience of Irukandji envenomation in far north Queensland. Med J Aust 1998; 169: 638-641. <eMJA full text>
- 5. Fenner P, Carney I. The Irukandji syndrome. A devastating syndrome caused by a north Australian jellyfish. Aust Fam Physician 1999; 28: 1131-1137.
- 6. Little M, Mulcahy RF, Wenck DJ. Life-threatening cardiac failure in a healthy young female with Irukandji syndrome. Anaesth Intensive Care 2001; 29: 178-180.
- 7. Taylor D, Pereira P, Seymour J, Winkel K. A sting from an unknown jellyfish species associated with persistent symptoms and raised troponin I levels. Emerg. Med 2002; 14: 175-180.
- 8. National Centre for Classification in Health – ICD-10 –Australian Modification. Sydney, NCCH Publishers, Shannon Books, 2002.
- 9. Fenner PJ, Hadok JC. Fatal envenomation by jellyfish causing Irukandji syndrome. Med J Aust 2002; 177: 362-363. <eMJA full text>
- 10. Fenner PJ, Burnett JW, Colquhoun DM, et al. The "Irukandji Syndrome" and acute pulmonary oedema. Med J Aust 1988; 149: 150-156.
- 11. Herceg I. Pulmonary oedema following an Irukandji sting. SPUMS J (South Pacific Underwater Medicine Society Journal) 1987; 17: 95-97.
- 12. Martin JC, Audley I. Cardiac failure following Irukandji envenomation. Med J Aust 1990; 153: 164-166.
- 13. Fenner PJ, Williamson J, Callanan VI, Audley I. Further understandings of and a new treatment for "Irukandji" (Carukia barnesi) stings. Med J Aust 1986; 145: 569-574.
- 14. Barnes JH. Observations on jellyfish stingings in North Queensland. Med J Aust 1960; 2: 993-999.
- 15. Currie BJ, Wood YK. Identification of Chironex fleckeri envenomation by nematocyst recovery from skin. Med J Aust 1995; 162: 478-480.
- 16. Fenner PJ, Fitzpatrick PF, Hartwick RJ, Skinner R. "Morbakka", another cubomedusan. Med J Aust 1985; 143: 550-555.
- 17. Lumley J, Williamson A, Fenner PJ, et al. Fatal envenomation by Chironex fleckeri, the north Australian jellyfish: the continuing search for lethal mechanisms. Med J Aust 1988; 148: 527-534.





Abstract
Objectives: (1) To identify the causative jellyfish species by examining skin scrapings in patients presenting to Cairns Base Hospital with marine stings, and (2) to describe clinical outcomes of those with Irukandji syndrome and those in whom nematocysts were identified from skin scrapings.
Design and setting: (1) A retrospective case series of 128 patients, identified from Cairns Base Hospital emergency department records with discharge diagnoses of marine stings between 1 July 2001 and 30 June 2002. (2) A prospective study of skin scrapings from 50 patients presenting with marine stings from the same period.
Main outcome measures: Number of patients with Irukandji syndrome, their opioid requirements and cardiac findings (where available); identification of causative species from nematocysts isolated from skin scrapings.
Results: 116 patients retrospectively identified with marine stings had Irukandji syndrome. Of 50 patients who had skin scrapings, 39 had nematocysts consistent with Carukia barnesi. Symptoms experienced ranged from local pain alone to severe Irukandji syndrome with elevated troponin I levels, changes on electrocardiogram, cardiac dysfunction on echocardiography, and high opioid dose requirements. One patient had an unidentified cnidome on his skin scraping. He developed severe Irukandji syndrome and subsequently died from its complications.
Conclusion: This is the first published report of Carukia barnesi being successfully identified from skin scrapings. Most patients with identifiable cnidomes experiencing Irukandji syndrome were stung by Carukia barnesi, which we show causes a wide range of illness, including cardiac dysfunction. Our finding of a cnidome not consistent with Carukia barnesi in the setting of Irukandji syndrome makes it possible that other species of jellyfish may also cause this syndrome.