Sore throat is the second most common illness for which Australians seek medical attention. Recent data from the BEACH (Bettering the Evaluation and Care of Health) project show that 4% of all symptomatic presentations to general practitioners were for throat complaints, second only to cough at 7%.1 Sore throat is also one of the most common reasons for prescribing antibiotics, with prescriptions resulting from 88.7% of consultations for sore throat in Australia in 2001.2 Yet, there is a growing argument that antibiotic treatment of sore throat caused by group A streptococci (GAS) — the predominant cause for which antibiotics may be indicated — has limited value in relieving symptoms and preventing complications in settings where acute rheumatic fever is rare.3 Published guidelines from the United Kingdom, Scotland and Australia reflect this approach.4-6 However, guidelines from the United States and Canada continue to stress the importance of diagnosis and treatment of streptococcal pharyngitis.7,8
This article details the main arguments for and against the investigation and antibiotic treatment of GAS pharyngitis and gives recommendations for Australian clinicians. It also highlights deficiencies in the available literature and the need for accurate epidemiological and cost-effectiveness studies.
Bacterial causes for sore throat other than GAS are rare, while antibiotics are not indicated for viral causes. Therefore, the aim of diagnosis is to identify the approximately one-third of cases in children and the 5%–10% of cases in adults that are caused by GAS.9,10 This is often difficult in primary care. Available options include clinical diagnosis, throat swab and culture, serological tests, and rapid antigen testing.
The clinical features of GAS pharyngitis may be quite distinctive, but are rarely sufficient to allow a confident diagnosis without confirmatory laboratory tests. For example, pharyngeal exudate may be present in more than a third of patients with non-GAS pharyngitis.11 Patient age may help: GAS pharyngitis occurs predominantly in school-aged children.12 However, it can occur in younger children and adults. Moreover, the characteristic symptoms and signs are less specific in children aged under three years.13 Even in older children and adults, clinical scoring systems predict positive results of throat cultures or rapid antigen detection tests 80% or less of the time (Box 1).14-20
A correctly cultured throat swab has a sensitivity of 90%–95%.21 However, the limitations of routine throat swabbing include the 24–48-hour delay while awaiting the result, the cost of the test compared with empirical treatment (or of initiating and then ceasing treatment if the swab is negative), the discomfort of the test, false negative results from poorly performed or processed swabs, and the difficulty in differentiating between infection and carriage of GAS. A recent Australian study found that only 13% of 284 Australian general practitioners would have taken a throat swab from a child with classical clinical signs of bacterial pharyngitis (fever, tender cervical lymph nodes and pharyngeal exudate).22 Streptococcal serological testing can distinguish carriage from infection, but is of little value in diagnosing acute pharyngitis, as the peak antistreptolysin O titre occurs three to six weeks after symptom onset.23
Rapid antigen tests may be used for same-day diagnosis in primary care. These tests are highly specific (over 95%), and the newer optical immunoassay may be as sensitive as a throat swab.24 A recent US study found the cost of a throat swab to be $2.40, compared with $6.50 for an optical immunoassay (in 1995 US dollars). It also found that throat swab with culture was the most cost-effective diagnostic strategy.25 Although rapid antigen tests are widely used in the United States, they have not been embraced in Australia, perhaps because they are expensive and attract no Medicare rebate.
The potential benefits of antibiotic treatment are:
decrease in symptom severity and duration;
prevention of suppurative complications, such as otitis media and retropharyngeal abscess;
decrease in infectivity and hence reduced numbers of secondary cases; and
prevention of acute rheumatic fever.26
There is no definitive evidence that antibiotic treatment of GAS pharyngitis prevents acute post-streptococcal glomerulonephritis.27 An important consideration is the need to minimise potential adverse effects from in-appropriate antibiotic therapy.
If antibiotics are used, a 10-day course of oral penicillin (or a single dose of intramuscular benzathine penicillin G) is still the treatment of choice for GAS pharyngitis, because of its proven efficacy in eradicating the organism and preventing subsequent rheumatic fever, its safety, narrow spectrum and low cost.28 Twice-daily dosing (250 mg of phenoxymethyl penicillin in children, 500 mg in adults) is as effective as three- or four-times-daily dosing and is now the preferred regimen.29 Regimens using broader-spectrum antibiotics have comparable bacteriological and clinical cure rates with shorter courses, but are not recommended, as they promote resistance, are more expensive and have more side effects, particularly gastrointestinal.30 The documented treatment failure rate with penicillin is 10%–15%.31 This failure is not caused by antibiotic resistance (no clinical isolates resistant to penicillin have been reported). Possible explanations include antibiotic tolerance (a decrease in bactericidal effect of penicillin with maintenance of inhibition of further growth has been observed in vitro), modification of the response to penicillin by other organisms in the upper respiratory tract, or sequestration of GAS organisms within epithelial cells, out of reach of β-lactam antibiotics.32 Penicillin-allergic patients should be treated with macrolides.28 As about 8% of GAS isolates in Australia are resistant to erythromycin,6 and macrolide resistance continues to increase around the world, these recommendations may change.
A recent Cochrane meta-analysis assessed the benefits of antibiotics in management of sore throat, and included 25 studies with a total of 11 452 cases.33 Antibiotics were found to reduce the risk of acute rheumatic fever by 70%, with a minimum reduction of 55% (odds ratio [OR], 0.30; 95% CI, 0.20–0.45). They also led to a 78% reduction in subsequent cases of acute otitis media (OR, 0.22; 95% CI, 0.11–0.43), and an 84% reduction in cases of quinsy (OR, 0.16; 95% CI, 0.07–0.35). The observed 54% reduction in cases of sinusitis had a wide 95% CI that included 1 (OR, 0.46; 95% CI, 0.10–2.05). Antibiotics also shortened the duration of pharyngitis symptoms, including headache, throat soreness and fever, by a mean of one day when assessed three days into the illness. The reviewers concluded that the effect of antibiotics on suppurative complications and symptom reduction was too small to justify antibiotic treatment of sore throat. However, they emphasised that the option of not treating GAS pharyngitis with antibiotics should be considered only in areas with low rates of acute rheumatic fever.
The limited Australian data suggest that Australians with sore throat rarely have throat swabs taken, but that most receive antibiotics. This is clearly at odds with the strategies of either treating based on a confirmed diagnosis of GAS pharyngitis, or of not treating GAS pharyngitis with antibiotics at all.
There are no good-quality Australian data on the incidence and costs of GAS pharyngitis and current approaches to management, which makes it difficult to recommend management strategies that take into account clinical and public health needs and cost-effectiveness. Comprehensive studies in Australia are limited to the Indigenous population of the Northern Territory, where the incidence of acute rheumatic fever is the highest reported in the world, and it is clear that prevention and treatment of GAS skin and throat infections should remain a priority.34 Studies of superficial GAS infections in urban Australian populations are uncommon and do not attempt to quantify the incidence or costs.13,35 More data are needed on the effectiveness (including cost-effectiveness) of antibiotic treatment of proven GAS pharyngitis in children, and on the effectiveness of antibiotics in limiting spread of virulent organisms and secondary cases.
Recommendations for antibiotic treatment of sore throat in Australia are summarised in Box 2. In settings where antibiotics are not to be recommended, surveillance systems should be established to monitor the emergence of virulent GAS strains and cases of acute rheumatic fever. In the United States, during the 1980s, the incidence of acute rheumatic fever and invasive GAS disease increased after a steady decline in antibiotic prescriptions for GAS pharyngitis over the previous decade. It is now thought that the major contributing factor to these outbreaks was the emergence of new, virulent GAS strains,36 but there is clearly a need for caution when adopting new treatment strategies. Monitoring systems will also allow sensible decisions about the use and effectiveness of GAS vaccines when they become available.
1: Clinical algorithms for diagnosing group A streptococcal (GAS) pharyngitis in patients with sore throat
Study author (year) |
Features included in final algorithm |
Age group (years) |
Sample size |
Sensitivity (%) |
Specificity (%) |
Positive predictive value (%) |
|||||
Walsh† (1975)14 |
Recent exposure to GAS infection
|
< 15 to |
418 |
55 |
74 |
28 |
|||||
Breese‡ (1977)15 |
Season (late winter or early spring)
|
Children |
670 |
68 |
85 |
84 |
|||||
Centor† (1981)16 |
History of fever
|
> 15 |
234 |
NS |
NS |
56 |
|||||
Steinhoff† (1997)17 |
Pharyngeal/tonsillar exudate or enlarged anterior cervical lymph nodes |
2–13 |
451 |
84 |
40 |
30 |
|||||
McIsaac† (1998)18 |
Tender and enlarged anterior cervical lymph nodes
|
3–14
|
90
|
63
|
67
|
51
|
|||||
Wald† (1998)19 |
Age (5–15 years)
|
2–16 |
365 |
22 |
93 |
75 |
|||||
Attia† (2001)20 |
Tonsillar swelling
|
1–18 |
545 |
18 |
97 |
79 |
|||||
NS = not stated (and not able to be calculated from the data provided). † Calculations are based on the presence of all listed features. ‡ Calculations are for a score of 32 out of a possible score of 38, based on a complex weighted score using the nine features listed. |
|||||||||||
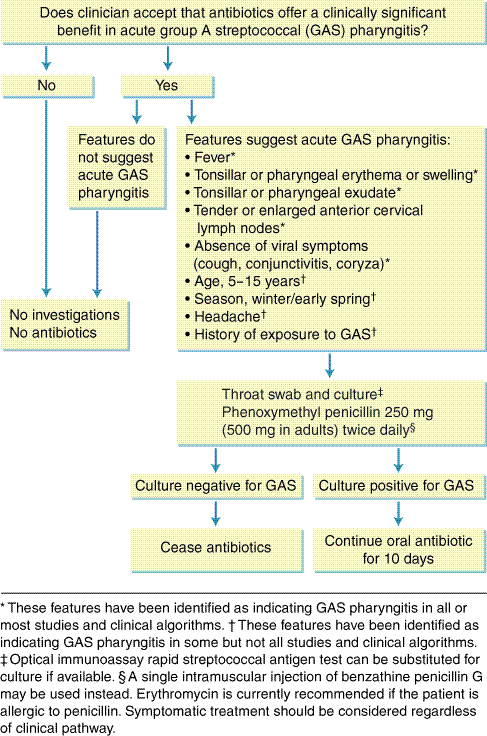
2: Recommendations for antibiotic treatment of sore throat in Australia
Antibiotic treatment is not indicated for sore throat without a high suspicion of GAS pharyngitis, except in populations with a high incidence of acute rheumatic fever.
In non-Indigenous Australians, the decision to treat GAS pharyngitis with antibiotics should not at present be based on prevention of acute rheumatic fever.
On the available evidence, it is reasonable for clinicians to choose not to treat GAS pharyngitis (see algorithm, Box 3); in that case there is no point undertaking diagnostic tests.
However, as antibiotic treatment of GAS pharyngitis may substantially reduce symptom duration, and as the effect on indirect costs and prevention of secondary cases has yet to be quantified, clinicians may also reasonably choose to treat cases of sore throat with features suggesting GAS pharyngitis (Box 1), particularly if signs of viral upper respiratory infection are absent (cough, conjunctivitis and rhinorrhoea).
In such cases, we recommend confirming the diagnosis using a throat swab and culture, as clinical diagnosis of GAS pharyngitis is inaccurate (see algorithm, Box 3).
Which of these two options is optimal cannot be decided until further population-based studies are undertaken.
- Margaret H Danchin1
- Nigel Curtis2
- Jonathan R Carapetis3
- Terence M Nolan4
- 1 Department of Paediatrics, University of Melbourne and Murdoch Children's Research Institute, Royal Children's Hospital, Parkville, VIC.
- 2 School of Population Health, University of Melbourne, Melbourne, VIC.
None identified.
- 1. Britt H, Miller GC, Knox S. General practice activity in Australia 2000-01. Canberra: Australian Institute of Health and Welfare, 2001. (AIHW Catalogue No. GEP 8.)
- 2. Prescribing practice review (PPR 18): Antibiotics in primary care. Surrey Hills: National Prescribing Service, 2002.
- 3. Del Mar C, Glasziou PP. Antibiotics for sore throats? J Paediatr Child Health 1998; 34: 498-499.
- 4. Royal College of Paediatrics and Child Health. Management of acute and recurring sore throat and indications for tonsillectomy. RCPCH guidelines for good practice, London: RCPCH, 2000.
- 5. Management of sore throat and indications for tonsillectomy. A national clinical guideline. Edinburgh: Scottish Intercollegiate Guidelines Network, Scottish Cancer Therapy Network, 1999.
- 6. Charlesworth K, Warrick T, Braddon J. National Prescribing Service Antibiotics Program. Antibiotics for sore throat, sinusitis, otitis media and acute bronchitis. Daw Park, SA: Drug and Therapeutics Information Service, 1999.
- 7. Bisno AL, Gerber MA, Gwaltney JM, et al. Diagnosis and management of group a streptococcal pharyngitis — a practice guideline. Clin Infect Dis 1997; 25: 574-583.
- 8. British Columbia Medical Association. Diagnosis and management of sore throat. BCMA Guidelines and Protocols Advisory Committee, 2000.
- 9. Poses RM, Cebul RD, Collins M, Frager SS. The accuracy of experienced physicians' probability estimates for patients with sore throats: implications for decision making. JAMA 1985; 254: 925-929.
- 10. Komaroff A, Pass TM, Aronson MD. The prediction of streptococcal pharyngitis in adults. J Gen Intern Med 1986; 1: 1-7.
- 11. Schwartz RH, Gerber MA, McKay K. Pharyngeal findings of group A streptococcal pharyngitis. Archiv Pediatr Adolesc Med 1998; 152: 927-928.
- 12. Bisno AL. Acute pharyngitis. N Engl J Med 2001; 344: 205-211.
- 13. Edmond K, Grimwood K, Carlin J, et al. Streptococcal pharyngitis in a paediatric emergency department. Med J Aust 1996; 165: 420-423.
- 14. Walsh BT, Bookheim WW, Johnson RC, Tomkins RK. Recogniton of streptococcal pharyngitis in adults. Arch Intern Med 1975; 135: 1493-1497.
- 15. Breese B. A simple scorecard for the tentative diagnosis of streptococcal pharyngitis. Am J Dis Child 1977; 131: 514-517.
- 16. Centor RM, Witherspoon JM, Dalton HP, et al. The diagnosis of strep throat in adults in the emergency room. Med Decis Making 1981; 1: 239-246.
- 17. Steinhoff M, El Khalek M, Khallaf N, et al. Effectiveness of clinical guidelines for the presumptive treatment of streptococcal pharyngitis in Egyptian children. Lancet 1997; 350: 918-921.
- 18. McIsaac WJ, White D, Tannenbaum D, Low DE. A clinical score to reduce unnecessary antibiotic use in patients with sore throat. Can Med Assoc J 1998; 158: 75-83.
- 19. Wald ER, Green MD, Schwartz B, Barbadora K. A streptococcal score card revisited. Pediatr Emerg Care 1998; 14: 109-111.
- 20. Attia MW, Zaoutis T, Klein JD, Meier FA. Performance of a predictive model for streptococcal pharyngitis in children. Arch Pediatr Adolesc Med 2001; 155: 687-691.
- 21. Gerber M. Comparison of throat cultures and rapid strep test for diagnosis of streptococcal pharyngitis. Pediatr Infect Dis J 1989; 8: 820-824.
- 22. Carr FC, Wales SG, Young D. Reported management of patients with sore throat in Australian general practice. Br J Gen Pract 1994; 44: 515-518.
- 23. Kaplan E, Ferrieri P, Wannamaker L. Comparison of the antibody response to streptococcal cellular and extracellular antigens in acute pharyngitis. J Pediatr 1974; 84: 21-28.
- 24. Gerber M, Tanz, RR, Kabat W, et al. Optical immunoassay test for group A beta-hemolytic streptococcal pharyngitis: an office-based, multi-center investigation. JAMA 1997; 277: 899-903.
- 25. Tsevat J, Kotagal U. Management of sore throats in children: a cost-effectiveness analysis. Arch Pediatr Adolesc Med 1999; 153: 681-688.
- 26. Krober MS, Bass JW, Michels GN. Streptococcal pharyngitis: placebo-controlled double-blind evaluation of clinical response to penicillin therapy. JAMA 1985; 253: 1271-1274.
- 27. Taylor JL, Howie JG. Antibiotics, sore throats and acute nephritis. J R Coll Gen Pract 1983; 33: 151-153.
- 28. Dajani A, Taubert K, Ferrieri P, et al. Treatment of acute streptococcal pharyngitis and prevention of rheumatic fever: a statement for health professionals. Committee on Rheumatic fever, Endocarditis, and Kawasaki disease of the Council on Cardiovascular Disease in the Young, the American Heart Association. Pediatrics 1995; 96: 758-764.
- 29. Gerber M, Spadaccini L, Wright L, et al. Twice-daily penicillin in the treatment of streptococcal pharyngitis. Am J Dis Child 1985; 139: 1145-1148.
- 30. Boccazzi A, Tonelli P, De'Angelis M, et al. Short course therapy with cefitbuten versus azithromycin in pediatric streptococcal pharyngitis. Pediatr Infect Dis J 2000; 19: 963-967.
- 31. Markowitz M, Gerber M, Kaplan E. Treatment of streptococcal pharyngotonsillitis: reports of penicillin's demise are premature. J Pediatr 1993; 123: 679-685.
- 32. Pichichero ME, Margolis PA. A comparison of cephalosporins and penicillins in the treatment of group A beta-hemolytic streptococcal pharyngitis: a meta-analysis supporting the concept of microbial copathogenicity. Pediatr Infect Dis J 1991; 10: 275-281.
- 33. Del Mar CB, Glasziou PP, Spinks AB. Antibiotics for sore throat. Cochrane Database of Systematic Reviews 2001: 2.
- 34. Carapetis JR. Cumulative incidence of rheumatic fever in an endemic region: a guide to the susceptibility of the population? Epidemiol Infect 2000; 124: 239-244.
- 35. Rogers M, Dorman D, Gapes M, Ly J. A three-year study of impetigo in Sydney. Med J Aust 1987; 147: 63-65.
- 36. Johnson D, Stevens D, Kaplan E. Epidemiologic analysis of group A streptococcal serotypes associated with severe systemic infections, rheumatic fever, or uncomplicated pharyngitis. J Infect Dis 1992; 166: 374-382.





Abstract
There are few good-quality studies of the effectiveness of antibiotic treatment of proven group A streptococcal (GAS) pharyngitis in children; available data suggest that antibiotics may reduce symptom duration.
While there is limited justification for antibiotic treatment of GAS pharyngitis to prevent acute rheumatic fever in non-Indigenous Australians, there is no justification for routine antibiotic treatment of all patients with sore throat.
Two strategies are open to clinicians: not to treat GAS pharyngitis with antibiotics, in which case no investigations should be done; or to treat cases of sore throat with clinical features that suggest GAS, in which case diagnosis should be confirmed with a throat swab, and penicillin started while awaiting the result. Penicillin should be discontinued if the swab is negative, or continued for 10 days if it is positive for GAS.
Surveillance of GAS infections and acute rheumatic fever is needed in Australia, as are further studies of effectiveness (including cost-effectiveness) of antibiotic treatment of proven GAS pharyngitis.