The Australian population is ageing rapidly, with the number of people over 80 years projected to double between 1986 and 2006.1 As older people make up the largest segment of the population participating in rehabilitation programs, adequately meeting their needs is a challenge for rehabilitation services. In addition, the incidence of the common conditions causing major physical disability increases rapidly in old age. For example, the incidences of stroke and hip fracture are 300 per 100 000 and 75 per 100 000, respectively, at ages 65–74 years, and 2300 per 100 000 and 400 per 100 000 at age 85 and over.2,3
"Disability" is defined as any restriction of ability to perform an activity in a manner considered normal for a human being.4 There is a progressive increase in the prevalence of disability with age; at age 85 it is 84%.5
Rehabilitation can be defined in a number of ways. Pragmatically, it can be seen as a process that aims to restore the functional capacities of a disabled person.4 The major goal of rehabilitation programs for older people is to assist them to manage personal activities of daily living without the assistance of another person. If this is not possible, the goal is to minimise the need for external assistance through the use of adaptive techniques and equipment. It is important for medical practitioners who work with older people to be able to recognise both a person's need for rehabilitation and his or her potential to benefit from it.

The primary aim of rehabilitation is mobility and self-care without assistance.
Older people who may benefit from rehabilitation typically have a major disability of recent onset. They have had a stroke, hip fracture or other fracture, a fall-related injury, or a major illness (such as severe cardiac failure); or they have ongoing severe osteoarthritis or Parkinson's disease. The disability will have compromised their ability to live independently, or semi-independently.
Most older people with recent significant disability, or deterioration in a pattern of stable disability, have the potential to benefit from rehabilitation. Chronological age per se should not be a factor in determining participation in a rehabilitation program. The major consideration is the ability to benefit from rehabilitation. The prime determinants of this are the severity of the presenting disability and the extent of pre-existing disability.6 Severe cognitive impairment is a risk factor for a poor response to a rehabilitation program. Older people with more minor disability, as a result of wrist fracture or knee osteoarthritis, can also benefit from rehabilitation programs, often on an outpatient or domiciliary basis.
A broad, whole-person view is obviously important when assessing an older person for rehabilitation. After interviewing and examining the patient, it is necessary to speak with family members and the patient's general practitioner. A formal assessment of the person's premorbid functional status is essential, ideally using a standardised instrument such as the Barthel Index (Box 1).7 If the person was not independently mobile before the current illness, a rehabilitation program is unlikely to achieve this after the illness. The present level of disability, which is a strong predictor of outcome, should also be assessed, but should not totally determine the person's suitability for a rehabilitation program.
It is essential that underlying medical problems are identified and managed. Cardiac failure, anaemia and chronic urinary sepsis are examples of conditions that negatively impact on a person's ability to participate in and benefit from a rehabilitation program. Rehabilitation is a "highly energetic process,"8 and to gain the most benefit participants need to be as well and as medically stable as possible. Hearing and vision should also be assessed and corrected as far as possible to maximise the older person's ability to participate.
A cognitive assessment should also be performed on all patients being considered for a rehabilitation program. There are a variety of standardised assessment tools, but the Mini-Mental State Examination is the one most widely used in Australia (Box 2).9 This is a screening tool rather than a diagnostic test, and the results should be interpreted carefully. For example, major language impairments will be associated with a low score irrespective of underlying cognitive function. Although poor cognitive function is associated with limited rehabilitation benefits in older people, it should not rule out an older person from an inpatient rehabilitation program.
Depression is also common in older people presenting for rehabilitation. A standardised assessment questionnaire such as the Geriatric Depression Scale (short form) can be used to evaluate the level of mood disturbance and determine whether treatment or further psychiatric assessment is required (Box 3).10
Rehabilitation for older people should have specific goals. These are most commonly mobility and self-care without the assistance of another person. The goals can be achieved most effectively by a team of health professionals from a variety of professional backgrounds working collaboratively. Key health professionals are nurses, doctors, physiotherapists, occupational therapists, speech pathologists and social workers. Methods of coordination must be in place, and these generally include formal case discussion meetings, and involving the older person and his or her family in goal setting and program design. There is strong evidence that this approach is effective.11-13
The case reports in Box 5 illustrate the process of rehabilitation in older people with major disability. The essence of the process is to work towards defined rehabilitation goals, with specific and coordinated problem solving as difficulties are encountered. While there are common elements in rehabilitation programs for older people — specifically, retraining of mobility and self-care — each rehabilitation program is individualised to satisfy the person's unique needs and desires.
Comorbid medical conditions are almost universal in older people participating in rehabilitation programs, and these can unpredictably complicate and interrupt rehabilitation.14 For these reasons, time-specified clinical pathways do not work well with older people. Pain should be treated,15 and bed rest avoided.16 Careful attention to care of pressure areas is often required.17 Half a century ago, Asher eloquently summed up the problems of too much bed rest: "Look at a patient lying long in bed, the blood clotting in his veins, the lime draining from his bones, the scybala stacking up in his colon, the flesh rotting from his seat. . . .".18
In reviewing progress with rehabilitation, achievement of specific goals should be monitored. In general, the ability to achieve certain tasks tends to be regained in a defined order. For example, grooming and feeding are generally achieved early in a rehabilitation program after stroke, while stair climbing is a much later goal. The use of a functional assessment scale that is rescored regularly during the rehabilitation program assists this process. The Functional Independence Measure19 and the Barthel Index (Box 1) are those most widely used.
Rehabilitation programs for older people also have a major psychosocial component. A major advance in recent rehabilitation practice is recognition and resolution of psychosocial issues.20 Assisting an older person to adapt to the consequences of a disabling illness is an essential component of the rehabilitation program, and counselling, listening and quiet encouragement are important.
Complex intergenerational issues often arise in the family setting, which may relate to the family's concern about the impact of the disability on the wider family. This is a valid concern, as most assistance for people with disability is provided by family members, particularly spouses and daughters. Often family members have been assisting an older person before the current illness and crisis, and feel burdened and fatigued. It may be possible to resolve some of these issues through discussion and provision of appropriate support services, in addition to the rehabilitation program.
Communication with an older person's family, general practitioner and other health professionals outside the rehabilitation setting are fostered by formal meetings, which may be face to face or by telephone. The formal family interview is often the key setting to communicate progress with rehabilitation and to update and finalise goals. The general practitioner should be invited to participate in this dialogue, and the case-conferencing provisions of the revised Medicare Benefits Schedule (Primary Care Incentives) should assist this process.21
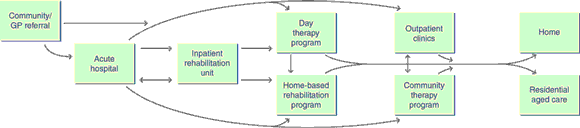
Contemporary rehabilitation practice occurs in the community and other settings outside hospital, as well as in traditional inpatient rehabilitation units. Home rehabilitation is increasingly an option for older people. Studies in patients with stroke or hip fracture, and in groups of patients with a mix of disabilities, suggest that outcomes of home rehabilitation are at least equivalent to those after traditional inpatient rehabilitation.12,22-24 In these programs, multidisciplinary rehabilitation is provided in the home, generally with the general practitioner supervising the patient's medical care.
In patients with less severe disability, rehabilitation may be conducted and supervised mainly by a single health professional, such as a physiotherapist or a speech pathologist, who consults with other health professionals about specific issues. An example may be a nurse assisting an older person to become more independent in self-care who consults a physiotherapist or rehabilitation physician for specific help with the patient's mobility retraining.
Rehabilitation for older people should be provided on an episodic rather than a continuing basis. When goals are achieved or when it is clear that only limited improvement is possible, they should be discharged from rehabilitation. Often older people will have multiple episodes of rehabilitation in association with specific disabling health conditions, as in the case reports in Box 5.
Among older people assessed for rehabilitation, a large group will require a long period of rehabilitation to recover from their disability, or will not recover sufficiently to return home. In general, these people have severe premorbid disability, or have developed very severe physical or cognitive disability as a result of their recent illness or injury. At least two important issues flow from this.
Firstly, a decision that a person is unsuitable for rehabilitation may not be accepted by the person or his or her family, or the referring health professionals. It is quite likely that the person has some potential to improve his or her level of functioning, even if remaining dependent. Studies after stroke confirm this,11 as people with all levels of disability appear to benefit from coordinated care after stroke. A more appropriate approach may be to view the person as being unsuitable for admission to an inpatient rehabilitation program, but to outline rehabilitation goals that can be achieved in other settings, such as a nursing home. These goals commonly relate to mobility, continence and self-care, and are achievable in a suitably supportive residential aged-care setting, with input from a physiotherapist or occupational therapist. Follow-up can be arranged to monitor progress with these limited goals, and to provide feedback and suggestions for further rehabilitation management to aged-care staff, the person's family and the general practitioner.
The second issue is the risk that patients with higher levels of disability will be excluded from rehabilitation services because of the perceived high cost of treatment. It is important that outcomes of rehabilitation programs for older people are monitored carefully. There will always be some patients who will not recover sufficiently to return home or to manage in a low-level residential aged-care facility (hostel), and therefore will require nursing home placement. In our opinion, an approximate benchmark for the proportion of older patients discharged from rehabilitation to high-level residential aged-care (nursing home) should be 10%–15%. Although these patients have not been able to gain sufficient independence to live in another setting, they may still have made useful gains in mobility, continence or self-care.
Evidence-based recommendations
Stroke – Inpatient stroke unit care improves outcomes for older people with stroke (E1).11
Hip and other fracture – Some types of geriatric rehabilitation after hip fracture improve the rate of return to community living (E2).12
Pain – Treatment of chronic pain in older people is efficacious (E1) and can be associated with other benefits (E2).15
Bed rest – There is no clear benefit of bed rest for older people (E1).16
Decubitus ulceration – Pressure-relieving mattresses are effective in reducing decubitus ulceration (E1).17
1: The Barthel Index7
The Barthel Index establishes a patient's degree of independence in activities of daily living (ADL). The patient's ability to perform the various activities is determined by direct observation or by asking the patient, the nurses, or the patient's relatives and friends. The assessment usually applies to the preceding 24–48 hours, and occasionally longer periods. The use of aids to complete a task independently is allowed. A score is assigned to each task — for example:
0 = dependent or unable to do the activity.
5 = needs some help to complete the activity.
10 = independent.
Scores for some activities that vary from this basic pattern are shown.
The activities are:
Feeding (normal food/soft food/able to eat and cut up food before eating or requires help)
Transfer (bed to chair and back) (5 or 10 points for transfer with assistance and 15 points if independent)
Grooming (face/hair/teeth/shaving)
Toilet transfer (getting on and off toilet)
Bathing (washing and getting in and out of bath/shower)
Mobility (wheelchair or walking) (5 points if able to use a wheelchair, 10 if able to walk 15 metres with assistance, and 15 if able to walk 15 metres without help)
Stairs (must be able to carry walking aids to be independent)
Dressing (including managing buttons/zips/shoelaces)
Bowels (5 points if accidents, 10 points if continent)
Bladder (5 points if accidents, 10 points if continent)
2: Mini-Mental State Examination9
Orientation 1. Ask the patient: "What is the year, season, date, day, month?" | /5 |
2. Ask: "Where are you?" — Country, State, city/town, suburb, address, number or floor (or ward) | /5 |
Memory registration 3. Tell the patient that you want him/her to remember something for you, then name three unrelated objects (speak clearly and slowly). Ask the patient to repeat the three objects (score 1 point for each object correctly named — may have up to 6 trials). Ask patient to keep the three things in mind. | /3 |
Attention and concentration 4. Ask the patient to take seven from 100, then seven from the result, and so on for five subtractions. Score 1 point for each correct answer. OR Ask the patient to spell "world" backwards, and score 1 point for each correct letter. | /5 |
Memory recall 5. Ask the patient to recall the three objects from test 3. | /3 |
Language 6. Show the patient two familiar objects (eg, a pen, a watch) and ask him/her to name them. | /2 |
7. Ask the patient to repeat a sentence after you: "No ifs, ands or buts". | /1 |
8. Ask the patient to follow a three-stage command: "Please take this paper in your left hand, fold it in half and put the paper on the floor". | /3 |
9. Ask the patient to read and follow a written instruction, eg, "Close your eyes". | /1 |
10. Ask the patient to write a simple sentence. The sentence should contain a subject and a verb and should make sense. | /1 |
11. Ask the patient to copy a picture
of intersecting pentagons. | /1 |
| /30 | |
A score below 24 indicates probable cognitive impairment. A score below 17 indicates definite cognitive impairment. |
3: Geriatric depression scale (short form)10
Choose the best answer for how you have felt over the past week:
1. Are you basically satisfied with your life? Yes / No
2. Have you dropped many of your activities and interests? Yes / No
3. Do you feel that your life is empty? Yes / No
4. Do you often get bored? Yes / No
5. Are you in good spirits most of the time? Yes / No
6. Are you afraid that something bad is going to happen to you? Yes / No
7. Do you feel happy most of the time? Yes / No
8. Do you often feel helpless? Yes / No
9. Do you prefer to stay at home, rather than going out and doing new things? Yes / No
10. Do you feel you have more problems with memory than most? Yes / No
11. Do you think it is wonderful to be alive now? Yes / No
12. Do you feel pretty worthless the way you are now? Yes / No
13. Do you feel full of energy? Yes / No
14. Do you feel that your situation is hopeless? Yes / No
15. Do you think that most people are better off than you are? Yes / No
"No" Answers indicate depression. Each answer counts 1 point; a score between 5 and 9 indicates the strong probability of depression, and a score of 10 or more is almost always indicative of depression.
- 1. Australian Bureau of Statistics. Projections of the population of Australia, States and Territories, 1993 to 2041. Canberra: ABS, 1994. (Catalogue No. 3222.0.)
- 2. Jamrozik K, Broadhurst RJ, Lai N, et al. Trends in the incidence, severity and short-term outcome of stroke in Perth, Western Australia. Stroke 1999; 30: 2105-2111.
- 3. Sanders KM. Seeman E, Ugoni AM, et al. Age- and gender-specific rate of fractures in Australia: a population-based study. Osteoporos Int 1999; 10: 240-247.
- 4. World Health Organization. ICF International Classification of Functioning, Disability and Health. Geneva: World Health Organisation, 2001. http://www3.who.int/icf/icftemplate.cfm (accessed August 2002).
- 5. Australian Bureau of Statistics. Disability, ageing and carers, Australia: Summary of findings. Canberra: ABS, 1998. (Catalogue No. 4330.0.)
- 6. Valderrama-Gama E, Damian J, Guallar E, Rodriguez-Manas L. Previous disability as a predictor of outcome in a geriatric rehabilitation unit. J Gerontol A Biol Sci Med Sci 1998; 53: M405-M409.
- 7. Mahoney FA, Barthel DW. Functional evaluation: the Barthel Index. Md State Med J 1965; 14: 61-65.
- 8. Young J, Robinson J, Dickinson E. Rehabilitation for older people [editorial]. BMJ 1998; 316: 1108-1109.
- 9. Folstein MF, Folstein SE, McHugh PR. "Mini-mental state". A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 1975; 12: 189-198.
- 10. Burke WJ, Roccaforte WH, Wengel SP. The short form of the Geriatric Depression Scale: a comparison with the 30-item form. J Geriatr Psychiatry Neurol 1991; 4: 173-178.
- 11. Stroke Trialists' Collaboration. Collaborative systematic review of the randomised trials of organised inpatient (stroke unit) care after stroke. BMJ 1997; 314: 1151-1159.
- 12. Cameron ID, Crotty M, Currie C, et al. Geriatric rehabilitation following fractures in older people: a systematic review. Health Technol Assess 2000; 4: 1-111.
- 13. Rubenstein LZ, Josephson KR, Wieland GD, et al. Effectiveness of a geriatric evaluation unit. A randomized clinical trial. N Engl J Med 1984; 311: 1664-1670.
- 14. Wilkinson TJ, Buhrkuhl DC, Sainsbury R. Assessing and restoring function in elderly people — more than rehabilitation. Clin Rehabil 1997; 11: 321-328.
- 15. Allen C, Glasziou P, Del Mar C. Bed rest: a potentially harmful treatment needing more careful evaluation. Lancet 1999; 354: 1229-1233.
- 16. The management of chronic pain in older persons: American Geriatrics Society Panel on Chronic Pain in Older Persons. J Am Geriatr Soc 1998; 46: 635-651.
- 17. Cullum N, Deeks J, Sheldon TA, et al. Beds, mattresses and cushions for pressure sore prevention and treatment (Cochrane Review). In: The Cochrane Library, Issue 3, 2002. Oxford: Update Software.
- 18. Asher RAJ. The dangers of going to bed. BMJ 1947; 2: 967-968.
- 19. Guide for the Uniform Data Set for Medical Rehabilitation (including the FIM? instrument, Version 5: Australia. Buffalo NY 14214: University at Buffalo; 1999.
- 20. Wade DT, de Jong BA. Recent advances in rehabilitation. BMJ 2000; 320: 1385-1388.
- 21. Commonwealth Department of Health and Aged Care. Primary Care Incentives: Enhanced Primary Care Package. Available from http://www.health.gov.au/hsdd/primcare/enhancpr/enhancpr.htm (accessed March 2002, no longer available).
- 22. Indredavik B, Fjaertoft H, Ekeberg G, et al. Benefit of an extended stroke unit service with early supported discharge: a randomized controlled trial. Stroke 2000; 31: 2989-2994.
- 23. Shepperd S, Harwood D, Jenkinson C, et al. A randomised controlled trial comparing hospital at home with inpatient hospital care (1): three month follow up of health outcomes. BMJ 1998; 316: 1786-1791.
- 24. Richards SH, Coast J, Gunnell DJ, et al. A randomised controlled trial comparing the effectiveness and acceptability of an early discharge hospital at home scheme with acute hospital care. BMJ 1998; 316: 1796-1801.





Abstract
Older people make up the majority of participants in general rehabilitation programs. Stroke and hip fracture are the major diagnostic groups.
Most older people with significant disability of recent onset have the potential to benefit from rehabilitation.
Assessing an older person's premorbid functional and cognitive status, which are strong determinants of rehabilitation outcome, is an important component of management.
The major goals of rehabilitation for older people are mobility and self-care without the assistance of another person.
Evidence suggests that rehabilitation for older people involving a coordinated multidisciplinary team of health professionals (including nurses and doctors) is effective.
Contemporary rehabilitation practice is not confined to traditional inpatient rehabilitation units; it also occurs in the community and other non-hospital settings, and involves general practitioners.