Before antibiotics were available, bacterial infections such as meningitis and endocarditis were almost uniformly fatal, and common infections such as Staphylococcus aureus bacteraemia had a mortality of 80%.1 One of the major medical advances of the last century was the development of effective antibiotics. However, with widespread use of antibiotics came antibiotic resistance.
By the late 1950s, many people with serious S. aureus infections had entered a "post-antibiotic" era, as most isolates were resistant to penicillin, the "last-line" antibiotic of the time. Fortunately, in the 1960s, new classes of drugs were developed, such as vancomycin and methicillin, which overcame the problem of resistance. These agents, or their subsequent derivatives (eg, dicloxacillin and flucloxacillin), remain the agents of choice for most S. aureus infections today.
Unfortunately, antibiotic resistance has moved on. Increasing numbers of S. aureus infections are caused by methicillin-resistant strains (MRSA), including many infections acquired in the community.2,3 None of the β-lactam antibiotics (including methicillin derivatives and cephalosporins) are effective in these infections. Until recently, this left vancomycin as the last-line antibiotic for hospital treatment of serious MRSA infections. However, although vancomycin was once reliable against all gram-positive organisms, including MRSA and enterococci, increasing numbers of S. aureus strains now also respond poorly to this antibiotic.4 These vancomycin-intermediate S. aureus strains (VISAs) have been found in many countries, including Australia.5 Vancomycin-resistant enterococci (VRE) have also been found in Australia, Europe and the United States.6,7 Patients with serious infections caused by VRE, such as bacteraemia, have high mortality.6
Because of concern about vancomycin resistance, two new agents — quinupristin–dalfopristin and linezolid — were developed and rapidly approved for clinical use. However, the former is not effective against Enterococcus faecalis, while resistance to the latter has been detected in bacteria isolated after therapy, including VRE and MRSA.8,9
The problem of antibiotic resistance also occurs in gram-negative bacteria. There are few or no antibiotics available now (or likely to be available soon) to treat life-threatening infections caused by some of these bacteria. For example, Acinetobacter baumanii has caused outbreaks of infections in intensive-care units in Australia, as well as overseas.10
Bacteria resistant to "last-line" antibiotics, such as carbapenems (eg, meropenem), glycopeptides (eg, vancomycin), fluoroquinolones (eg, ciprofloxacin) and third-generation cephalosporins (eg, cefotaxime), are often found in Australian hospitals. Some are also found in the community and even in food.7,11 Many taskforces and committees have reported on the growing problem of antibiotic resistance, including the Australian Joint Expert Technical Advisory Committee on Antibiotic Resistance (JETACAR).12 Both a United States interagency taskforce and the World Health Organization recently proposed plans to combat antibiotic resistance.13,14
Most antibiotics modify or interfere with essential functions or structures of bacteria, and many appear to be analogues of elements of bacterial metabolism or to mimic natural signals. This may explain why the genes encoding resistance may be widespread even before antibiotic use.15 For example, wild animals in Australia have little or no exposure to antibiotics, yet a study of Escherichia coli isolates from kangaroos and wombats found that 3% were resistant to amoxycillin, 2% to cephazolin, 0.2% to tetracycline, and 0.2% to trimethoprim.15 Antibiotic resistance was also present, albeit at low levels, in other Enterobacteriaceae isolates (eg, trimethoprim resistance in 3% of Enterobacter cloacae isolates).
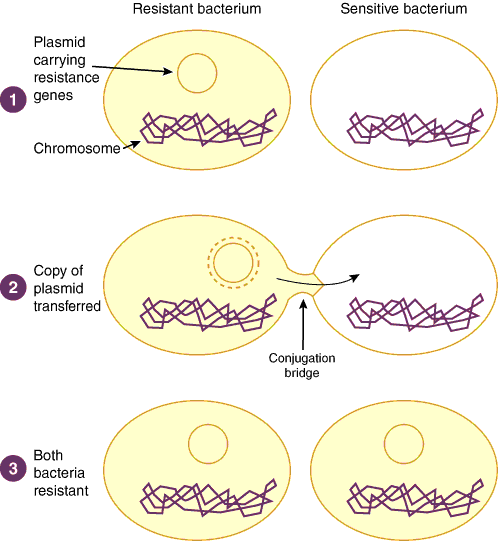
However, when antibiotics are used, bacteria with DNA encoding resistance have a selective advantage over sensitive bacteria and can more easily multiply (along with their genetic material). Their larger numbers facilitate their spread from bacterium to bacterium (Box 1), person to person, animal to animal, and within the environment.
For example, MRSA caused infections in hospital patients in India, Turkey and Poland before methicillin had been used in these countries.16 However, when methicillin and its derivatives became readily available, MRSA strains were encountered much more often.16 Individual strains spread efficiently not only within hospitals, but also between hospitals and internationally. Indeed, a major hospital epidemic strain of MRSA in the United Kingdom originated in Australia.17 In addition, strains of MRSA that originated in the community (eg, in Samoa and the Kimberley region of Australia) now cause infections in people who have had no hospital contact in Australia and many other countries.2,3
Most bacteria have mechanisms that allow them to share genetic material, such as conjugation (Box 1). These mechanisms allow the genes encoding antibiotic resistance to move between bacteria not only of the same species but also of different species and genera. Genetic material encoding resistance is often "clonal" (ie, identical across a wide range of bacteria) and can readily move between bacteria of the same species and different species and genera, especially when carried within a plasmid or transposon. For example, the vanA gene, which encodes vancomycin resistance, is carried within a transposon and moves easily between enterococcal species and potentially to other gram-positive cocci, such as staphylococci.18 Indeed, evidence of transfer of vanA from VRE to an MRSA strain was recently seen in a renal dialysis patient in the United States.19
To compound the problem of antibiotic resistance, exposure to one antibiotic may help select resistance to others. If an E. coli isolate is resistant to a first-generation cephalosporin (eg, cephalexin), then it will also be resistant to all other cephalosporins of the same generation (eg, cephazolin). Furthermore, if an isolate becomes resistant to a third-generation cephalosporin (eg, cefotaxime), then it will also be resistant to all first- and second-generation cephalosporins.
Cross-resistance also occurs across classes of antibiotics. For example, MRSA strains are resistant to methicillin and its derivatives because of changes to the bacterial receptors for these antibiotics (penicillin-binding proteins); these changed receptors have insufficient activity to result in bacterial death when exposed to the antibiotics. As similar receptors are required by all other β-lactams (including cephalosporins and carbapenems), they too are ineffective against MRSA.
The phenomenon of cross-resistance is one of the principal reasons for recommending narrow-spectrum antibiotics to treat infections whenever possible. If resistance develops, then it will usually be to fewer antibiotics than if a broad-spectrum agent had been used.
Bacteria can also be resistant to many different classes of antibiotics ("multiresistant"). An example is Streptococcus pneumoniae: some isolates are resistant to ampicillin, erythromycin, tetracycline and trimethoprim–sulfamethoxazole20 (case history, Box 2). This not only limits the choice of antibiotic therapy, possibly excluding all oral agents, but also means that the use of any of these antibiotics selects for the multiresistant strain ("coselection"), promoting its persistence.
The development and spread of antibiotic resistance are consequences of antibiotic use — in medicine, agriculture and other areas, such as aquaculture. To reduce antibiotic resistance, we need to use antibiotics less and to use them prudently. As bacteria do not respect artificial boundaries between environments, this is essential in all areas of use. Strategies to decrease the development and spread of antibiotic resistance are shown in Box 3.
In medicine, prudent antibiotic use dictates that we should not use antibiotics unless they improve patient outcome. Not all bacterial infections need antibiotic therapy. For example, in acute bacterial bronchitis and sore throat, any benefit to the patient from antibiotic therapy is small and counterbalanced by the risk of drug side effects, such as rash.22,23 Interventions other than antibiotics, such as regular analgesia, are more effective in decreasing symptoms.
In addition, when assessing whether antibiotics should be used for common bacterial infections, the population effect must be taken into account, especially in infections that usually resolve spontaneously with little extra benefit from antibiotic use. Antibiotic use exerts selective pressure not only on the pathogen being treated, but also on the patient's normal flora. Antibiotic resistance in S. pneumoniae is a rapidly growing problem in the community, both in Australia and abroad20 (case history, Box 2). An Australian study found that the presence of penicillin-resistant S. pneumoniae in the nasal flora of preschool children was significantly associated with their use of β-lactam antibiotics in the preceding two months.24 The risk that a child carried a resistant strain of S. pneumoniae increased by 4% for each day that the antibiotics were used.24
When antibiotic therapy is to be used, it should be targeted as far as possible to the pathogen, which may need to be cultured. Narrow-spectrum antibiotics should be chosen whenever possible. Antibiotics should be used in the optimal dosages and regimens, and should be stopped when the infection is treated.
In agriculture, large quantities of antibiotics are used for growth promotion.7,12 This has contributed to large numbers of antibiotic-resistant bacteria being ingested by humans via the food chain (eg, VRE in Europe7).
Use of antibiotics can also be reduced by preventing infections in the first place. For example, since the introduction of an effective vaccine for Haemophilus influenzae type B (Hib) in Australia, so few Hib infections have occurred25 that antibiotic resistance of this organism is no longer a major issue.
Antibiotic-resistant Salmonella species (eg, Salmonella typhi) are major causes of illness throughout the world. The problem of Salmonella infection is worst where the water supply is contaminated with faecal material from humans or animals. Providing a safe water supply will decrease antibiotic use and the consequent selective pressure on Salmonella species and other bacteria carried by patients.
In hospitals, improving infection control practices could prevent many infections and decrease the need for antibiotic therapy (eg, use of aseptic technique for inserting intravenous and urinary catheters, and compliance with handwashing protocols26). Specific modifications to medical procedures and protocols could also prevent infections. For example, the incidence of infections associated with intravenous catheters can be reduced by removing the devices when they are no longer essential.27 Research on the prophylactic use of antibiotics in surgery has shown that rates of postoperative infection are lower if a single dose of antibiotic is given at skin incision than if a longer course is given before and after the procedure — the previously established practice.28 Following the new guidelines can hugely decrease the amount of antibiotics used for surgical prophylaxis while improving outcomes. More research is needed into improving medical procedures and protocols to reduce infections.
Good hygiene in the home, especially during food preparation and storage, also has the potential to prevent infections, such as Salmonella and Campylobacter infections, and thereby minimise antibiotic use.
Resistance is a problem not only in bacteria. Whenever agents are used that interfere with the multiplication of organisms, resistance almost inevitably develops. Examples are viruses (eg, HIV), fungi (eg, Candida spp.) and herbicide resistance in plants. By using the optimal dosages and regimens, and most importantly by limiting their overuse, the lifetime of these important agents can be extended, and resistance minimised. Specific "action steps" that doctors can take to prevent antimicrobial resistance in the community are shown in Box 4.
Evidence-based recommendations
Antibiotics for sore throat: These confer some modest benefits. Symptom duration is shortened by 16 hours. In Western societies, protection against complications is achieved only by treating many with antibiotics who will derive no benefit (E1).23
Antibiotics for acute otitis media in children: These provide a small benefit, but with an absolute reduction in pain in only 5%. Most cases resolve spontaneously. Seventeen children must be treated to prevent one child having some pain after two days. Antibiotics have no effect on hearing problems or other complications (E1).29
Antibiotics for acute bronchitis: These have a modest beneficial effect, but magnitude of the benefit is similar to the detriment from potential adverse effects. Patients with other symptoms of the common cold who have been ill for less than a week are not likely to show any benefits (E1).22
Antibiotics for the common cold: Patients receiving antibiotics did no better in terms of cure or improvement than those taking placebo and had significantly more side effects (E1).30
Antibiotics for acute maxillary sinusitis: In sinusitis confirmed by aspiration or radiography, penicillin improved clinical cures compared with controls. Current evidence is limited but suggests penicillin or amoxycillin therapy for 7–14 days (E1).31
2: Case history — a consequence of long-term, broad-spectrum antibiotic therapy
Presentation: A 16-year-old boy was referred to a hospital emergency department by his general practitioner after presenting with fever (39ºC), rigors and left-sided pleuritic chest pain. Investigations and history: A chest x-ray showed left lower lobe pneumonia. The boy reported that he was allergic to amoxycillin and cephalosporins (as a child he had developed a rash to these agents). He had been taking daily doxycycline for the previous three months to treat mild acne, which had not responded to self-selected, over-the-counter preparations. Management and course: He was treated with intravenous erythromycin because of his reported β-lactam allergies, but continued to be unwell, with ongoing fevers and rigors. The day after admission, both sputum and blood cultures grew Streptococcus pneumoniae. After 48 hours, antibiotic sensitivity results showed that the isolate was intermediate-resistant to penicillin, and resistant to both erythromycin and tetracycline. The antibiotic treatment was changed to vancomcyin. His fever resolved over the next 12 hours, and he made a slow but full recovery over the next week. |
|
||||||||||
3: Strategies for decreasing antibiotic resistance
Prudent use of antibiotics
General
Use narrow-spectrum agents whenever possible.
Do not use antibiotics for non-infection-related purposes (eg, to improve gastric motility or as anti-inflammatory agents in humans and for growth promotion in animals).
Therapy
Treat infections only when this improves patient outcome overall (balance with adverse events; not all bacterial infections need antibiotics).
Restrict "last-line" antibiotics for serious infections and use only where simpler agents would be ineffective.
Prophylaxis
Use short courses (single dose is usually sufficient in surgery).
Give at the correct time (eg, at the time of surgical incision).
Prevention of infection
Improve infection control and hygiene.
Improve use of vaccines.
Improve infrastructure (eg, safe water supply, better hospital design).
Education
Educate about use of antibiotics, when not to use them, infection prevention strategies.
Target both healthcare professionals and the general public.
Surveillance
How much resistance is present, in which bacteria and where?
How, which, where and in what quantities are antibiotics used?
Use to devise targeted interventions to minimise antibiotic use.
Research
New agents and classes of antibiotics.
New and better vaccines.
Alternatives to antibiotics for prophylaxis.
Better use of current antibiotics (eg, shorter therapy).
Improved medical devices (eg, disinfectant-impregnated intravenous catheters).
Protocols for improved patient care (eg, urinary catheters in place for shorter periods; remove intravenous catheters when no longer necessary).
4: "Action steps" for doctors to prevent antimicrobial resistance in the community*
Vaccinate — have influenza vaccine yourself; make sure infants receive Hib (Haemophilus influenzae type b) vaccine; give influenza and Streptococcus pneumoniae vaccine to at-risk patients.
Target the pathogen — grow cultures from the patient; target empirical therapy to likely pathogens and definitive therapy to known pathogens.
Use local data — know your antibiogram (local antibiotic sensitivity profiles).
It's OK to say "no" to patients with viral infections.
Use narrow-spectrum antibiotics wherever possible.
Treat infection, not contamination or colonisation.
Stop antimicrobial treatment when the infection is unlikely (eg, cultures are negative) or has been treated (often short-course therapy is sufficient).
Remove the causes of persisting or recurrent infections — remove indwelling catheters; drain abscesses.
Practise antimicrobial control — engage in local antimicrobial control efforts; use antibiotic guidelines.
Break the chain of contagion — stay home when you are sick (and recommend that sick patients stay home from work); keep your hands clean; follow good infection control practices; set an example!
* Adapted from the website of the US Centers for Disease Control and Prevention, "Action steps" for preventing antimicrobial resistance in the hospital.13
- Peter J Collignon1
- Series Editors:
- Infectious Diseases Unit and Microbiology Department, Canberra Hospital, Woden, ACT.
- 1. Waldvogel F. Staphylococcus aureus (including toxic shock syndrome). In: Mandell G, Bennett J, Dolin R, editors. Principles and practice of infectious diseases. 5th ed. Philadelphia: Churchill Livingstone, 2000: 2065-2092.
- 2. Collignon P, Gosbell I, Vickery A, et al. Community-acquired methicillin-resistant Staphylococcus aureus in Australia. Australian Group on Antimicrobial Resistance. Lancet 1998; 352: 145-146.
- 3. Gosbell IB, Mercer JL, Neville SA, et al. Non-multiresistant and multiresistant methicillin-resistant Staphylococcus aureus in community-acquired infections. Med J Aust 2001; 174: 627-630.
- 4. Paterson D. Reduced susceptibility of Staphylococcus aureus to vancomycin — a review of current knowledge. Commun Dis Intell 1999; 24: 69-73.
- 5. Ward P, Johnson P, Grabsch E, et al. Treatment failure due to methicillin-resistant Staphylococcus aureus (MRSA) with reduced susceptibility to vancomycin. Med J Aust 2001; 175: 480-483. <eMJA full text>
- 6. Edmond MB, Ober JF, Dawson JD, et al. Vancomycin-resistant enterococcal bacteremia: natural history and attributable mortality. Clin Infect Dis 1996; 23: 1234-1239.
- 7. Collignon P. Vancomycin-resistant enterococci and use of avoparcin in animal feed: is there a link? Med J Aust 1999; 171: 144-146. <eMJA full text>
- 8. Gonzales RD, Schreckenberger PC, Graham MB, et al. Infections due to vancomycin-resistant Enterococcus faecium resistant to linezolid. Lancet 2001; 357: 1179.
- 9. Tsiodras S, Gold HS, Sakoulas G, et al. Linezolid resistance in a clinical isolate of Staphylococcus aureus. Lancet 2001; 358: 207-208.
- 10. Riley T, Webbs S, Cadwallader H, et al. Outbreak of gentamicin-resistant Acinetobacter baumanii in an intensive care unit: clinical, epidemiological and microbiological features. Pathology 1996; 28: 359-363.
- 11. McDonald LC, Rossiter S, Mackinson C, et al. Quinupristin-dalfopristin-resistant Enterococcus faecium on chicken and in human stool specimens. N Engl J Med 2001; 345: 1155-1160.
- 12. The use of antibiotics in food-producing animals: antibiotic-resistant bacteria in animals and humans. Report of the Joint Expert Technical Advisory Committee on Antibiotic Resistance (JETACAR). Canberra: Office of National Health and Medical Research, Oct 1999. Available at <http://www.health.gov.au/pubs/jetacar.htm>
- 13. Interagency Task Force on Antimicrobial Resistance, Co-chairs: Centers for Disease Control and Prevention, Food and Drug Administration, National Institutes of Health, Agency for Healthcare Research and Quality, Health Care Financing Administration, Health Resources and Services Administration, Department of Agriculture, Department of Defense, Department of Veterans Affairs, Environmental Protection Agency. A public health action plan to combat antimicrobial resistance, 2001. Available at <http://www.cdc.gov/drugresistance/actionplan/html/index.htm>
- 14. World Health Organization. WHO global strategy for containment of antimicrobial resistance. Geneva: WHO, 2001. Available at <http://www.who.int/emc/amrpdfs/WHO_Global_Strategy_English.pdf>
- 15. Sherley M, Gordon DM, Collignon PJ. Variations in antibiotic resistance profile in Enterobacteriaceae isolated from wild Australian mammals. Environ Microbiol 2000; 2: 620-631.
- 16. Rountree P, Beard M. Hospital strains of Staphylococcus aureus with particular reference to methicillin-resistant strains. Med J Aust 1968; 26: 1163-1168.
- 17. Townsend DE, Ashdown N, Bradley JM, et al. "Australian" methicillin-resistant Staphylococcus aureus in a London hospital? Med J Aust 1984; 141: 339-340.
- 18. Dutka-Malen S, Leclercq R, Coutant V, et al. Phenotypic and genotypic heterogeneity of glycopeptide resistance determinants in gram-positive bacteria. Antimicrob Agents Chemother 1990; 34: 1875-1879.
- 19. Sievert DM, Boulton ML, Stoltman G, et al. Staphylococcus aureus resistant to vancomycin — United States, 2002. MMWR Morb Mortal Wkly Rep 2002; 51: 565-567.
- 20. Collignon PJ, Turnidge JD. Antibiotic resistance in Streptococcus pneumoniae. Med J Aust 2000; 173 Suppl: S58-S64.
- 21. Therapeutic Guidelines Ltd. Therapeutic guidelines: antibiotic. Version 11. Melbourne: Therapeutic Guidelines Ltd, 2000: 169.
- 22. Smucny J, Fahey T, Becker L, Glazier R. Antibiotics for acute bronchitis (Cochrane Review). Cochrane Library 2001; 4. Oxford: Update Software.
- 23. Del Mar CB, Glasziou PP, Spinks AB. Antibiotics for sore throat (Cochrane Review). Cochrane Library 2001; 4. Oxford: Update Software.
- 24. Nasrin D, Collignon P, Roberts L, et al. Effect of β-lactam antibiotic use in children on pneumococcal resistance to penicillin: prospective cohort study. BMJ 2002; 324: 28-30.
- 25. McIntyre PB, Chey T, Smith WT. The impact of vaccination against invasive Haemophilus influenzae type b disease in the Sydney region. Med J Aust 1995; 162: 245-248.
- 26. Spelman DW. Hospital-acquired infections. Med J Aust 2002; 176: 286-291. <eMJA full text>
- 27. Collignon P. Hospital-acquired infections: a skeleton in the closet of medical progress. Med J Aust 1995; 163: 228.
- 28. Nichols R. Prophylaxis for surgical infections. In: Gorbach S, Bartlett J, Blacklow N, editors. Infectious diseases. Philadelphia: WB Saunders, 1992: 393-403. 1: Management plan for antibiotic resistance.
- 29. Glasziou PP, Del Mar CB, Sanders SL, Hayem M. Antibiotics for acute otitis media in children (Cochrane Review). Cochrane Library 2001; 4. Oxford: Update Software.
- 30. Arroll B, Kenealy T. Antibiotics for the common cold (Cochrane Review). Cochrane Library 2001; 4. Oxford: Update Software.
- 31. Williams JW, Aguilar C, Makela M, et al. Antibiotics for acute maxillary sinusitis (Cochrane Review). Cochrane Library 2001; 4. Oxford: Update Software.





Abstract
Antibiotic resistance is a consequence of antibiotic use — we need to use antibiotics less and to use them prudently.
Plans to combat antibiotic resistance were recently proposed by the World Health Organization, a United States interagency taskforce and the Australian Joint Expert Technical Advisory Committee on Antibiotic Resistance.
Prudent antibiotic use includes not using antibiotics when benefit is minimal (eg, in many respiratory tract infections), using narrow-spectrum antibiotics whenever possible and using optimal dosages and regimens.
The need for antibiotic therapy can be reduced by preventing infections through vaccination, infection control measures and improved sanitation.
Surveillance of antibiotic resistance is needed to target interventions for minimising antibiotic use.
More research is needed into new antibiotics and regimens and into improving medical devices and protocols to prevent infection.