The national renal registries of Australia/New Zealand, the United States, Canada and Japan have reported an increasing incidence of end-stage renal disease (ESRD) of between 3% and 8% per year between 1993 and 1997.1 Despite improvements in treatment, the mortality of people on dialysis remains high.2 Annual mortality rates in the various renal registries range from 10% to 20%.3
The proportion of ESRD patients referred "late" to a nephrologist (ie, patients needing to commence dialysis within three to four months of referral) varies widely. In developing countries, the proportion is as high as 62%,4 while in developed countries it is normally 25%–40%.5-8 Previous US and UK reports have shown that increasing age and coexisting illnesses,9 ethnicity10 and membership of a health maintenance organisation5 are associated with late referral.
Late-referral (LR) patients on dialysis experience greater early morbidity and higher early mortality. Late referral, associated with advanced uraemic symptoms, metabolic acidosis, hypertension, pulmonary oedema and pericarditis, frequently results in emergency haemodialysis using central venous catheters.6-8 It is also associated with longer6,7 and more costly6 initial hospitalisation. Early mortality, during the initial 6–12 months on dialysis, is higher for LR patients,4,11 but little is known about survival differences beyond the first year.
The aim of our study was to investigate whether or not late referral to a nephrologist influences the rates of transplantation and mortality among patients who have survived at least one year's dialysis.
The Australia and New Zealand Dialysis and Transplant Registry (ANZDATA) maintains a database of patients treated by maintenance dialysis or renal transplantation in Australia.12 All Australian renal units treating ESRD supply data to the Registry. Survey forms are completed six-monthly for all patients up to and including the date of death. The only patients not registered are the few who die before being established on a maintenance dialysis or transplant program. Data on the timing of referral (ie, whether "late" or "not late") have been collected for new patients entered onto the Registry since 1 April 1995.
Between 1 April 1995 and 31 March 2000, we followed up patients with ESRD to examine the long-term effects of late referral on both the likelihood of transplantation and on mortality.
Using the ANZDATA database, we recorded, for each patient, the timing of referral, age, sex, primary renal disease, the presence of selected comorbidities recorded at entry to the program, whether or not the patient was of Indigenous origin, and the treatment modality (haemodialysis, peritoneal dialysis or transplantation).
LR patients were defined as those needing to commence dialysis within three months of referral to a nephrologist. This definition, consistent with international nephrology research,7,8,13 reflects the minimum time required to educate patients regarding treatment options and to establish permanent vascular access for haemodialysis.
Comorbid illnesses noted were diabetes, ischaemic heart disease, cerebrovascular disease, peripheral vascular disease and chronic lung disease. Outcomes were patient survival and whether or not the patient received a transplant at any time between one year after starting dialysis and the completion of the study.
During the study period, 5590 patients with ESRD commenced renal replacement treatment (RRT). Excluded from the analysis were 36 patients (0.6%) who had started treatment outside Australia or who were overseas visitors, and 194 patients (3.5%) with ESRD due to rapidly progressive glomerulonephritis, Goodpasture's syndrome, cholesterol emboli, haemolytic–uraemic syndrome or cortical necrosis. (As these conditions generally have a very short course from inception to ESRD, contact with renal services earlier than three months before commencing RRT would not usually have been possible.)
In their first year on RRT, fewer LR patients received a transplant (5.5% [LR] v 10.6% [non-LR]; P < 0.001) and more died (15.9% [LR] v 9.4% [non-LR]; P < 0.001). In order to discount the short-term hazards of an unplanned commencement of dialysis, we focused on patients who survived their first year on dialysis. We therefore excluded 494 patients (8.8%) who received transplants, 600 patients (10.7%) who died and 23 patients (0.4%) who were lost to follow-up within the first year. Our analysis was based on data for the remaining 4243 patients.
Within the study period, patients were followed up to the time of transplantation, loss to follow-up, or death. Transplantation was chosen as an endpoint for follow-up, as it greatly reduces mortality14 and would therefore distort the effects of other factors, including late referral.
Statistical analysis was performed using STATA 7.0 software.15 Using the Cox proportional hazards model, we calculated a rate ratio for transplantation and a hazard ratio for death. Patient survival was estimated by the Kaplan–Meier method, with the log rank test used to compare survival curves. The first year on dialysis was not included in survival time, as patients had to survive at least that period to be included.
Of the 4243 patients included in the study, 1141 (26.9%) were LR patients (Box 1). Hypertensive renal disease, other types of primary renal disease and uncertain diagnoses were more common in the LR group. Primary glomerulonephritis, polycystic disease, analgesic nephropathy and reflux nephropathy were more common in the non-LR group. The LR group had a greater burden of comorbid illness.
There were no significant differences in age or sex between LR and non-LR patients, but a significantly higher proportion of the LR group was of Indigenous origin (13.4% v 7.7%; P < 0.001).
LR patients were also less likely to receive a transplant in their second and subsequent years on RRT (unadjusted rate ratio, 0.71; 95% CI, 0.58–0.86). This difference remained significant after adjustment for age, sex, number of comorbidities, primary cause of renal disease and Indigenous status (adjusted rate ratio, 0.78; 95% CI, 0.63–0.95).
Kaplan–Meier survival curves, according to timing of referral, showed a significant difference in survival after the first year on RRT (P value for log rank test, < 0.001) (Box 1). The mortality rate was 20 deaths (95% CI, 18–22 deaths) per 100 patient-years for the LR group and 15 deaths (95% CI, 14–16 deaths) for the non-LR group. The unadjusted hazard ratio for death in the LR group compared with the non-LR group was 1.30 (95% CI, 1.14–1.48). After adjusting for known predictors of mortality (age, sex, number of comorbidities, presence of primary renal disease and Indigenous status), the hazard ratio for death in the LR group was still significant (1.19; 95% CI, 1.04–1.35). The hazard ratio for death was significant even when Indigenous patients were excluded from the analysis. Inclusion of a variable that described the dialysis modality in the first year of treatment made no significant difference.
Our results show unequivocally that late referral is associated with increased mortality beyond the initial year of RRT. The association persists even after adjusting for known predictors of mortality, suggesting that additional factors may be involved. A plausible explanation is that late referral may be a reflection of suboptimal pre-ESRD care, affecting patient survival before commencement of dialysis and for years afterwards.
It is possible that the difference in survival rate between LR and non-LR patients is related to the level of renal function at the start of dialysis, which has been shown to be a determinant of patient survival.16 If non-LR patients start treatment earlier in the course of their chronic renal disease (at a stage when renal function is significantly less impaired), subsequent survival on dialysis may be longer. ANZDATA has, since 1998, collected data regarding the level of renal function at the start of dialysis. Of patients starting RRT during 1998, the LR patients (n = 358) had a mean creatinine clearance of 8.0 mL/min (SD, ± 7.1) and non-LR patients (n = 1133) had a mean clearance of 7.9 mL/min (SD, ± 3.6), a non-significant difference.14 Assuming that the results would have been similar for the other study years (1995–1997), the observed survival difference would not appear to be directly related to the level of renal function at the start of dialysis.
Incomplete adjustment for intervening and confounding variables may be part of the explanation for the survival difference attributed to late referral. Chandna et al11 have shown that a total comorbidity severity score is a better predictor of mortality on RRT than the number of comorbidities. We were unable to explore this possibility, as ANZDATA does not collect data on the severity of comorbid illnesses. However, if late referral is an indicator of suboptimal pre-ESRD care, it is plausible that worse outcomes might be due to inadequate management of comorbid illnesses, including vascular disease and heart failure.
Two previous studies7,8 of the effect of late referral on long-term survival (at least five years' follow-up) found no significant difference in long-term survival between LR and non-LR patients. Another study11 found that unplanned presentation (which is not the same as late referral) adversely affected survival. However, all three studies involved fewer than 300 patients and had limited power to detect a significant difference between LR and non-LR groups. By contrast, our study, based on a national cohort, has much greater power. Moreover, because our study (unlike previous studies) excluded all patients who died in their first year on dialysis, we were able to separate the short-term effects of unplanned commencement of RRT from the long-term disadvantage arising from suboptimally managed chronic renal insufficiency.
Our results suggest that improving the quality of pre-ESRD care, through timely referral, might improve long-term survival on RRT. Angiotensin-converting enzyme inhibitors,17,18 angiotensin-II-receptor antagonists,19 rigorous blood pressure control20 and rigorous glycaemic control21 have all been proven effective in slowing the progression of chronic renal insufficiency. However, there have been no definitive studies demonstrating methods to reduce mortality in people with chronic renal impairment.
The continuing high incidence of late referral seems to indicate that nephrologists are failing to communicate to physicians and general practitioners the importance of optimal pre-ESRD care. Primary care doctors may be unaware of the severity of renal insufficiency in some patients, particularly if serum creatinine level is the only measure used to monitor renal function.22 Late referral may stem from uncertainty about the appropriateness of RRT for a given patient,22 or the perception that treatment services are not easily accessible to the patient. In a US survey of GPs who referred new ESRD patients to a renal unit, Campbell et al23 found that key factors delaying referral were lack of knowledge of guidelines (relating to timing and indications for referral) and inadequate communication between nephrologists and GPs.
Levin13 contends that "many specialists (and general practitioners) perceive nephrologists only as providers of dialysis therapy . . . [and fail to appreciate] the utility of nephrological care during early stages of renal insufficiency". Although the Australian Kidney Foundation has issued guidelines for the care of people with renal impairment,24 to our knowledge no attempt has been made to assess the awareness of these guidelines among GPs and non-nephrologists.
The AusDiab study25 found that 2.5% of Australian adults aged 25 years or over had significant proteinuria and that 1.1% had a serum creatinine level of over 120 μmol/L. This suggests that several hundred thousand Australians have indicators of renal disease. Screening studies in Japan indicate that people with proteinuria are 15 times more likely than those without proteinuria to develop renal failure within 10 years.26 We believe that there is sufficient evidence that progression of chronic renal insufficiency to ESRD can be prevented to suggest that targeted screening for renal disease among people in high-risk groups should be undertaken in general practice. The most important potential benefit, despite the absence of strong evidence, could be reduced mortality among people with chronic renal insufficiency.
We suggest that GPs use dipstick urinalysis for proteinuria to screen patients who have any one of the following risk factors: age over 50, hypertension, diabetes, smoking, family history of renal disease, or being of Indigenous origin. Serum creatinine level should be measured to calculate the glomerular filtration rate using the Cockcroft–Gault equation.27 Where appropriate, patients should be treated aggressively for hypertension, proteinuria and other vascular risk factors, and, if the glomerular filtration rate falls below 30mL/min, referred promptly to a nephrologist.24
We must urgently address the lack of a strong evidence base in the management of patients with chronic renal insufficiency. These patients need a continuum of care from the time of diagnosis to the onset of ESRD. Achieving optimal treatment will require a true collaboration between GPs and specialist nephrologists.
1: Patient characteristics at start of renal replacement therapy (number [%] of patients, unless otherwise specified)
Not referred late (n = 3102) |
Referred late (n = 1141) |
||||||||||
Age (years) |
|||||||||||
Mean (± SD) |
56.8 |
(± 15.6) |
56.1 |
(± 16.1) |
|||||||
Range |
0.6–86.1 |
0.6–88.7 |
|||||||||
Female patients |
1362 |
(43.9%) |
478 |
(41.9%) |
|||||||
Comorbidities* |
|||||||||||
Ischaemic heart disease |
1183 |
(38.1%) |
454 |
(39.8%) |
|||||||
Cerebrovascular disease |
448 |
(14.4%) |
194 |
(17.0%) |
|||||||
Peripheral vascular disease |
765 |
(24.7%) |
337 |
(29.5%) |
|||||||
Chronic airways disease |
445 |
(14.4%) |
217 |
(19.0%) |
|||||||
Diabetes mellitus |
893 |
(28.8%) |
408 |
(35.8%) |
|||||||
Number of comorbidities |
|||||||||||
None |
1258 |
(40.6%) |
408 |
(35.8%) |
|||||||
One |
787 |
(25.4%) |
265 |
(23.2%) |
|||||||
Two |
487 |
(15.7%) |
201 |
(17.6%) |
|||||||
Three |
339 |
(10.9%) |
146 |
(12.8%) |
|||||||
Four |
195 |
(6.3%) |
100 |
(8.8%) |
|||||||
Five |
35 |
(1.1%) |
21 |
(1.8%) |
|||||||
Primary renal disease |
|||||||||||
Primary glomerulonephritis |
1065 |
(34.3%) |
348 |
(30.5%) |
|||||||
Diabetes mellitus |
640 |
(20.6%) |
290 |
(25.4%) |
|||||||
Hypertension |
311 |
(10.0%) |
151 |
(13.2%) |
|||||||
Polycystic disease |
282 |
(9.1%) |
38 |
(3.3%) |
|||||||
Analgesic nephropathy |
222 |
(7.2%) |
53 |
(4.7%) |
|||||||
Reflux nephropathy |
163 |
(5.3%) |
25 |
(2.2%) |
|||||||
Other diagnoses |
264 |
(8.5%) |
121 |
(10.6%) |
|||||||
Uncertain |
155 |
(5.0%) |
115 |
(10.1%) |
|||||||
Patients of Indigenous origin |
239 |
(7.7%) |
153 |
(13.4%) |
|||||||
*Comorbid illness categories are not mutually exclusive. |
|||||||||||
2: Kaplan–Meier curves of cumulative survival, by timing of referral
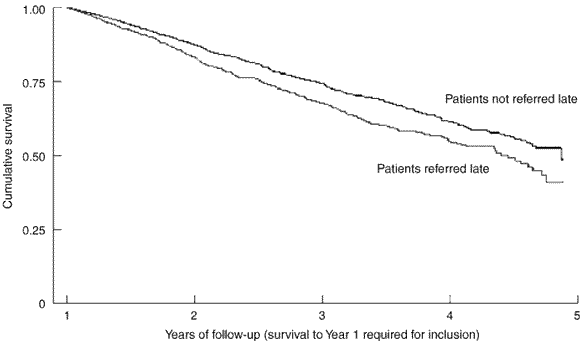
Number of patients at risk at beginning of each year of study
Year 1 |
Year 2 |
Year 3 |
Year 4 |
||||||||
LR patients |
1141 |
704 |
384 |
132 |
|||||||
Non-LR patients |
3102 |
1869 |
909 |
318 |
|||||||
LR = late referral. |
|||||||||||
Received 14 November 2001, accepted 11 April 2002
- Alan Cass1
- Joan Cunningham2
- Zhiqiang-Wang3
- Wendy Hoy4
- Peter C Arnold5
- Paul Snelling6
- 1 Menzies School of Health Research, Casuarina, NT.
- 2 PO Box 280, Edgecliff, NSW.
- 3 Cooperative Research Centre for Aboriginal and Tropical Health, Casuarina, NT.
The data reported here have been supplied by the Australia and New Zealand Dialysis and Transplant Registry (ANZDATA). The interpretation of these data is the responsibility of the authors and should in no way be seen as an official policy or interpretation of ANZDATA. The study is an approved research project of the Cooperative Research Centre for Aboriginal and Tropical Health. Alan Cass receives PhD scholarship funding from the Colonial Foundation, and Joan Cunningham is supported by a fellowship from the Menzies Foundation.
None identified.
- 1. Schena FP. Epidemiology of end-stage renal disease: international comparisons of renal replacement therapy. Kidney Int 2000; 57(Suppl 74): S39-S45.
- 2. Baigent C, Burbury K, Wheeler D. Premature cardiovascular disease in chronic renal failure. Lancet 2000; 356: 147-152.
- 3. Prichard SS. Comorbidities and their impact on outcome in patients with end-stage renal disease. Kidney Int 2000; 57(Suppl 74): S100-S104.
- 4. Sesso R, Belasco AG. Late diagnosis of chronic renal failure and mortality on maintenance dialysis. Nephrol Dial Transplant 1996; 11: 2417-2420.
- 5. Arora P, Obrador GT, Ruthazer R, et al. Prevalence, predictors, and consequences of late nephrology referral at a tertiary care center. J Am Soc Nephrol 1999; 10: 1281-1286.
- 6. Jungers P, Zingraff J, Albouze G, et al. Late referral to maintenance dialysis: detrimental consequences. Nephrol Dial Transplant 1993; 8: 1089-1093.
- 7. Roubicek C, Brunet P, Huiart L, et al. Timing of nephrology referral: influence on mortality and morbidity. Am J Kidney Dis 2000; 36: 35-41.
- 8. Schmidt RJ, Domico JR, Sorkin MI, Hobbs G. Early referral and its impact on emergent first dialyses, health care costs, and outcome. Am J Kidney Dis 1998; 32: 278-283.
- 9. Khan IH, Catto GR, Edward N, MacLeod AM. Chronic renal failure: factors influencing nephrology referral. QJM 1994; 87: 559-564.
- 10. Ifudu O, Dawood M, Iofel Y, et al. Delayed referral of black, Hispanic, and older patients with chronic renal failure. Am J Kidney Dis 1999; 33: 728-733.
- 11. Chandna SM, Schulz J, Lawrence C, et al. Is there a rationale for rationing chronic dialysis? A hospital based cohort study of factors affecting survival and morbidity. BMJ 1999; 318: 217-223.
- 12. Disney A, editor. ANZDATA registry report 2000. Adelaide: Australia and New Zealand Dialysis and Transplant Registry, 2000.
- 13. Levin A. Consequences of late referral on patient outcomes. Nephrol Dial Transplant 2000; 15(Suppl 3[6]): 8-13.
- 14. Disney A, Russ G, Walker R, et al, editors. ANZDATA registry report 1999. Adelaide: Australia and New Zealand Dialysis and Transplant Registry, 1999.
- 15. Stata statistical software. Release 7. College Station, TX: Stata Corporation, 2000.
- 16. Shemin D, Bostom A, Laliberty P, Dworkin L. Residual renal function and mortality risk in hemodialysis patients. Am J Kidney Dis 2001; 38: 85-90.
- 17. Ruggenenti P, Perna A, Gherardi G, et al. Renoprotective properties of ACE-inhibition in non-diabetic nephropathies with non-nephrotic proteinuria. Lancet 1999; 354: 359-364.
- 18. Lewis EJ, Hunsicker LG, Bain RP, Rohde RD. The effect of angiotensin-converting-enzyme inhibition on diabetic nephropathy. The Collaborative Study Group. N Engl J Med 1993; 329: 1456-1462.
- 19. Brenner BM, Cooper ME, de Zeeuw D, et al. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001; 345: 861-869.
- 20. Klahr S, Levey AS, Beck GJ, et al. The effects of dietary protein restriction and blood-pressure control on the progression of chronic renal disease. Modification of Diet in Renal Disease Study Group. N Engl J Med 1994; 330: 877-884.
- 21. The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 1993; 329: 977-986.
- 22. Eadington DW. Delayed referral for dialysis [editorial]. Nephrol Dial Transplant 1996; 11: 2124-2126.
- 23. Campbell JD, Ewigman B, Hosokawa M, Van Stone JC. The timing of referral of patients with end-stage renal disease. Dial Transplant 1989; 18: 660-686.
- 24. Knight J, Vimalachandra D, editors. The CARI guidelines — caring for Australians with renal impairment. Sydney: Excerpta Medica Communications, 2000. Available at: <http://www.ciap.health.nsw.gov.au/cari>. Accessed 24 June 2002, no longer available. Try <http://www.kidney.org.au/cari/guidelines.php>
- 25. Dunstan D, Zimmet P, Welborn T, et al, on behalf of the AusDiab Steering Committee. Diabesity and associated disorders in Australia — 2000: the accelerating epidemic. Australian diabetes, obesity and lifestyle report. Melbourne: International Diabetes Institute, 2001.
- 26. Iseki K, Iseki C, Ikemiya Y, Fukiyama K. Risk of developing end-stage renal disease in a cohort of mass screening. Kidney Int 1996; 49: 800-805.
- 27. Cockcroft DW, Gault MH. Prediction of creatinine clearance from serum creatinine. Nephron 1976; 16: 31-41.





Abstract
Objective: To investigate whether late referral to a nephrologist of patients with chronic renal insufficiency influences the likelihood of both transplantation and mortality among those who survive at least one year on dialysis.
Design: Retrospective national cohort study, using data from the Australia and New Zealand Dialysis and Transplant Registry database.
Participants: All patients with end-stage renal disease who started renal replacement treatment in Australia between 1 April 1995 and 31 December 1998, excluding those who received transplants or who died in their first year of dialysis. Patients referred "late" were defined as those who needed to commence dialysis within three months of referral to a nephrologist.
Main outcome measures: Length of patient survival, and whether patients received a transplant at any time between one year after starting dialysis and completion of the study on 31 March 2000.
Results: Of the 4243 patients included in the study, 1141 (26.9%) were referred late. Late-referral (LR) patients were significantly less likely to receive a transplant in their second and subsequent years on dialysis (adjusted rate ratio, 0.78; 95% CI, 0.64–0.95). LR patients were at significantly increased risk of death after their first year on dialysis (adjusted hazard ratio, 1.19; 95% CI, 1.04–1.35).
Conclusions: Late referral is associated with increased mortality, even among those who survive their first year on dialysis. Improving the quality of pre-dialysis care might improve access to transplantation and long-term survival. General practitioners could minimise late referrals through targeted screening of high-risk individuals.