Although modern treatment processes and stringent regulations mean that tap water is generally safe to drink in developed countries, microbial pathogens remain the major public health risk associated with drinking water. Major waterborne pathogens include bacteria (eg, pathogenic Escherichia coli strains, Campylobacter and Salmonella spp.), protozoa (eg, Cryptosporidium parvum and Giardia lamblia), and viruses (eg, adenoviruses, enteroviruses and rotaviruses).
These organisms may be transmitted by other routes, including food and person-to-person spread, and drinking water is thought to be a minor contributor to disease in most Australian communities. For example, a recent randomised controlled trial in Melbourne found no difference in gastroenteritis rates between people who drank regular tap water and those who drank filtered, ultraviolet-treated water, suggesting that drinking water does not contribute significantly to background rates of gastroenteritis in that city.1
However, the potential for large populations to be exposed to pathogens via the water supply mandates vigilance against contamination of source water and failure of water treatment procedures. In addition, for many smaller and remote communities, limited resources mean that reliable provision of microbiologically safe water remains a challenge.
Microbial contaminants in Australia's drinking water supplies are reduced or eliminated through protection of water catchment, disinfection, water treatment and filtration. Treated water is then monitored for bacterial indicator organisms to satisfy guidelines for use as drinking water. However, this type of monitoring inevitably involves a timelag between sampling and availability of test results, and water contamination will seldom be detected until after consumption. Moreover, while current indicator organisms (Escherichia coli or faecal coliforms) are good indicators of risks from bacterial pathogens, they correlate poorly with viral and protozoal pathogens.
Monitoring for viral or protozoal pathogens has been suggested to improve the microbial safety of water supplies, but is technically difficult and expensive, and results are hard to interpret. For example, in Sydney in 1998, high concentrations of Cryptosporidium oocysts and Giardia cysts were reported in treated drinking water, but subsequent investigations revealed no evidence of increased disease,2 and questions were raised about the validity of the test results.3
Cryptosporidium spp. and Bacillus anthracis are candidates for bioterrorist contamination of water supplies,4 because of their low infectious dose. Although the high level of dilution reduces the risk of health effects, the threat cannot be dismissed. Protecting the security of water supplies is now a major focus of the Australian and international water industry.
Use of alternative water sources, such as water reuse schemes and rainwater collection, may increase the risk of infection. New risk-management approaches or water treatment methods may be needed to protect public health. For example, increasing use of rainwater or "grey" water (laundry and shower waste) in urban areas raises the possibility of cross-connection with the tap water supply, and may require more stringent plumbing regulations.
Chemicals may enter drinking water through leaching from the environment, chemical spills and deliberate additions (eg, disinfectants), and contact with piping and plumbing materials. In addition, toxins produced by cyanobacteria (blue-green algae; Box 1) may be considered as chemical contaminants, as their health effects are mediated via intoxication rather than infection. Cyanobacterial blooms occur in warm, slow-moving rivers and lakes, and are promoted by nutrient runoff from the surrounding catchment.
Some chemicals relevant to drinking water quality and their potential health effects are summarised in Box 2. For many, there is clear evidence of adverse effects at high exposure levels, but the degree of risk at the lower levels found in drinking water is not well defined. Drinking water guideline levels for chemical contaminants incorporate safety factors, so that daily exposure at the guideline level over a lifetime poses no significant risk.
Debate continues about the health effects of exposure to disinfection byproducts, while more recent concerns include endocrine disrupters (chemicals which mimic or interfere with the actions of endocrine hormones) and pharmaceuticals.
Disinfectants such as chlorine and chloramines react with suspended organic material to produce a large range of byproducts. Some epidemiological studies have indicated a possible association between exposure to disinfection byproducts and adverse health effects (Box 2), although evidence in this area is conflicting and inconclusive.5 Attention has focused on chlorine-based disinfectants, with the byproducts of other chemical disinfectants less well studied. Overall, the immediate benefits of chlorination in terms of protection from microbial pathogens far outweigh theoretical long-term risks of disinfection byproducts. This was well illustrated in Peru, where inadequate or absent disinfection was a contributing factor in a major cholera outbreak.6
Manufactured chemicals, such as pesticides, insecticides, industrial waste products and pharmaceuticals (including antibiotics, steroids and reproductive hormones), may contaminate our water supplies. Use of recycled wastewater and biosolids from sewage increases the potential for exposure. Concern has arisen about the potential adverse effects of low-level exposures to these substances, particularly those with endocrine-disrupting activity. No impact on human health has been convincingly demonstrated so far, but research on this topic is a high priority.7
Many chemicals and toxins are odourless, colourless, tasteless and biologically active in microgram amounts and, as such, could serve as potential tools for bioterrorism. Possible candidates include botulinum toxin A, tetrodotoxin, ciguatoxins, arsenic, lead, mercury, pesticides and radionuclides.4
Potential health risks associated with exposure to swimming pools, spas, rivers, reservoirs or marine waters include gastrointestinal, skin and respiratory infections. Gastrointestinal infections transmitted by the faecal–oral route are most common. Public swimming pools have been linked with outbreaks of disease caused by E. coli, Shigella, Cryptosporidium and Giardia spp. Other illnesses related to recreational water exposure are shown in Box 3. In addition, cyanobacteria may cause contact dermatitis, gastroenteritis and allergic symptoms, possibly through endotoxins (Box 1).
Major problems facing water resources and urban supplies in Australia include:
In some areas of Australia, groundwater supplies contain high levels of dissolved salts, which make water unpalatable. As areas affected by salinity increase, additional drinking water sources or treatment methods will be needed (Box 4).
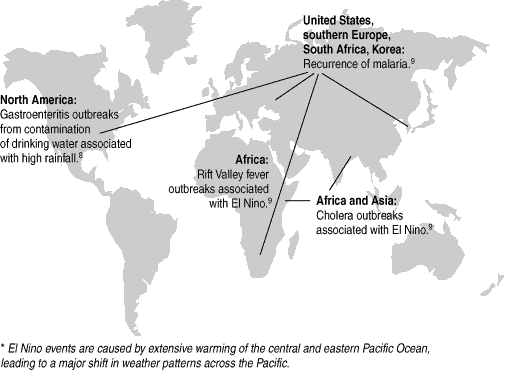
Climate change, particularly rising temperatures and changes in rainfall, will affect our water supplies (Box 5). Weather pattern changes, with more prolonged droughts alternating with high-intensity rainfall events, may alter disease transmission patterns. Waterborne outbreaks are significantly associated with high-rainfall events, which flush large quantities of contaminants into water sources and overwhelm water treatment systems.8 Falling water levels and reduced river flows during droughts increase the risk of cyanobacterial blooms, and also make water treatment more difficult as levels of sediment and organic material increase. Global warming is also predicted to extend the geographic range of many insect-borne diseases.9,10
Although drinking and recreational water supplies are unlikely to be major sources of illness in Australian communities, they pose a potential risk. Clinicians have a role in diagnosis of waterborne disease and prevention:
Physicians should be aware of local waterborne health problems in high-risk geographical areas (eg, nitrate in groundwater sources).
A disease cluster or outbreak suggested by a common history of exposure to drinking or recreational water should be immediately reported to the local health department. Faecal specimens should be collected to identify a pathogen, if warranted clinically. However, diagnosis of a specific pathogen does not identify the source, as multiple routes of transmission are possible. For example, although outbreaks of giardiasis and cryptosporidiosis have been related to contaminated drinking water overseas, no outbreaks have been associated with municipal water supplies in Australia, and most sporadic cases of diarrhoea caused by these pathogens are not caused by contaminated water supplies.
Preventive advice, particularly in the immunocompromised or other vulnerable groups, or during periods of suspected high health risk, may include the following:
- use an appropriate tap filter for drinking water;
- use alternative sources for drinking water;
- bring water to a rolling boil before use; and
- avoid recreational water exposures.
Water restrictions, increasing use of alternative water sources and more water-efficient appliances will be important elements in reducing our demand for drinking water, but may also present potential health risks. Solutions will include:
The Australian Drinking Water Guidelines are currently being revised to incorporate a preventive risk management approach.11 This emphasises the need for multiple barriers to microbial and chemical contamination throughout water supply systems and for real-time monitoring to detect and rectify problems before they affect water quality.
These have a long history of use for domestic drinking water in rural and remote areas of Australia and are being increasingly used in urban areas to conserve tap water supplies. While drinking water from these tanks is not believed to pose a major risk if systems are well designed and maintained,12 health authorities are generally not prepared to endorse the use of untreated rainwater for public consumption because of potential contamination and a lack of health outcome data.
Water is already recycled in agriculture and industry, which use most of our water supplies. Guidelines exist to control potential health risks from microbial and chemical contamination for different applications.13 It is technically feasible to raise the quality of recycled water to drinking water standard, but cost and public perception are obstacles.
Agriculture, industry and urban populations will continue to compete for land and water. Disease outbreaks and contamination events have often provided the impetus for upgrading drinking water technology, protecting watersheds, improving distribution and regulatory systems overseas,14 but water quality has not been seen as a major public health issue in Australia to date. We need new technologies and responses to ensure sustainability of our water supply, but new public health questions will undoubtedly arise. We should not expect limitless water supplies and should not take safe and clean water for granted (Box 6).
1: Recreational waterway closed because of a cyanobacterial bloom

Although cyanobacteria do not infect humans or animals, they may cause contact dermatitis, gastroenteritis and allergic symptoms (eg, rhinitis, conjunctivitis and asthma), probably through cellular endotoxins. Some blooms also produce hepatotoxins or neurotoxins.
2: Health outcomes possibly related to chemical exposures from drinking water
Chemical |
Possible health outcomes |
Comments |
|||||||||
Aluminium |
High levels possibly associated with Parkinsonian dementia, Alzheimer's disease and amyotrophic lateral sclerosis. |
No health guideline for aluminium in water supplies set by either the World Health Organization or National Health and Medical Research Council (NHMRC), because of insufficient data. Food and other beverages are the main sources of daily intake of aluminium, with < 2% from drinking water. |
|||||||||
Arsenic |
Chronic exposure associated with increased risks of cancer (particularly of the skin, lung, and genitourinary tract), skin changes, organomegaly, vascular changes (including hypertension) and neurotoxicity. |
Chronic arsenic toxicity is a current major health concern in Bangladesh and West Bengal. In Australia, arsenic contamination of groundwater may occur from past gold mining, sheep dipping or timber treatment practices, or natural geological sources. Levels recorded in Australia are 10–30 times lower than those associated with adverse effects documented from epidemiological studies. |
|||||||||
Copper |
High intake is associated with acute gastrointestinal symptoms (nausea, vomiting and abdominal pain) and chronic exposure can result in cirrhosis. |
Many cases of acute poisoning reported worldwide, but only two cases of liver failure in Australian children have been reported (associated with exposure to acidic bore water with high levels of copper from pipes).15 Food is the main source of copper intake, with < 10% contribution from drinking water. |
|||||||||
Disinfection byproducts (DBPs) |
Chronic exposure possibly associated with increased risk of cancer, particularly of the bladder and bowel. More recent attention focused on possible increased risks of miscarriage and birth defects. |
It is difficult to measure DBP exposure accurately and to account for potential confounding effects from other exposures. Evidence for adverse health effects from DBPs in drinking water is currently considered inconsistent and inconclusive,16-18 but this remains an area of active research. |
|||||||||
Lead |
Lead exposure can have central nervous system effects. Epidemiological evidence suggests cumulative exposure in children affects intellectual development. Carcinogenicity suggested by animal studies, but not documented in humans. |
Lead piping was used extensively for domestic plumbing in Europe and North America, but seldom in Australia. Most lead intake is from food and other sources, such as old paintwork. |
|||||||||
Nitrate |
Methaemoglobinaemia in infants aged under three months may occur if baby formula is made with water with raised nitrate concentrations (> 50 mg/L). |
Nitrate from natural and man-made sources (eg, agricultural fertilisers) may affect groundwater supplies. In several Western Australian towns, bottled water is supplied for making baby formula because of high nitrate levels in tap water. |
|||||||||
Fluoride |
Possible effects on bone (skeletal fluorosis, osteosarcomas, osteoporosis and fractures). High levels in children can lead to dental fluorosis. |
Levels of fluoride added to drinking water in Australia do not appear to have an adverse effect on bone mineral density or fracture incidence.19 NHMRC reviews have supported the dental health benefits and safety of water fluoridation.20 |
|||||||||
Cyano- bacterial toxins |
Some species produce endotoxins (causing allergic reactions, skin rashes, eye irritation, gastroenteritis), neurotoxins and hepatotoxins. |
High levels are very unlikely in drinking water supplies. The only significant human cyanobacterial poisoning recorded in Australia occurred on Palm Island in 1979, when use of copper sulfate to kill a cyanobacterial bloom in a reservoir released large amounts of hepatotoxin. About 140 children and 10 adults were hospitalised with hepatitis-like symptoms.21 |
|||||||||
3: Non-gastrointestinal illnesses associated with recreational water exposure, and their causes
Skin diseases
Pseudomonas aeruginosa
(eg, "spa" folliculitis)
Atypical mycobacteria, especially Mycobacterium marinum, Mycobacterium ulcerans (skin ulcers, common in southern Australia)
Respiratory diseases
Viruses, particularly adenovirus
Legionella spp. (may be associated with spas or whirlpools)
Environmental mycobacteria, especially Mycobacterium kansasii, Mycobacterium avium complex (lung disease, particularly in immunosuppressed people)
Ear infections
P. aeruginosa, Staphylococcus aureus (otitis externa and media)
Liver or renal disease
Leptospira spp. (via skin contact with water contaminated with animal or rodent urine, often in association with water sports and adventure travel;23 a recent large outbreak occurred among participants in a Malaysian triathlon24).
Central nervous system infections
Naegleria fowleri fulminant, usually fatal, amoebic meningoencephalitis, after swimming in contaminated ponds; cases recorded in several Australian states
Acanthamoeba spp. (universally fatal granulomatous encephalitis which can occur in immunosuppressed people after exposure to fresh or sea water or chlorinated swimming pools)
Keratitis
Acanthamoeba spp. (in people with corneal abrasions)
4: Bore water tanks with filter systems

These tanks are fitted with solar-powered reverse-osmosis filter systems to reduce levels of dissolved solids and render the water palatable.
6: Reflections and predictions
Circa 1900
Cholera known to be transmitted by drinking water.
Water supplies not yet routinely chlorinated, filtered or protected from sewage pollution.
No routine microbial monitoring of water.
Waterborne outbreaks, including cholera and typhoid, occurring in Australia.
Circa 2100
Water has re-emerged as a major public health concern.
Many natural water resources are depleted, and water restrictions are common.
Domestic water use has been greatly reduced by efficient conservation practices.
Water supplies are dual, with lower quality water for non-drinking purposes.
Rainwater tanks are compulsory for new developments.
More variable weather patterns have increased the risk of outbreaks of waterborne disease.
Global warming has increased rates of vector-borne disease.
- Karin Leder1
- Martha I Sinclair2
- John J McNeil3
- Department of Epidemiology and Preventive Medicine, Monash University Central and Eastern Clinical School, Alfred Hospital, Melbourne, VIC.
None identified.
- 1. Hellard ME, Sinclair MI, Forbes AB, Fairley CK. A randomized, blinded, controlled trial investigating the gastrointestinal health effects of drinking water quality. Environ Health Perspect 2001; 109: 773-778.
- 2. The Sydney water incident: July-September 1998. NSW Public Health Bull 1998; 9: 91-94.
- 3. Clancy JL. Sydney's 1998 water quality crisis. J Am Water Works Assoc 2000; 92: 55-66.
- 4. Khan AS, Swerdlow DL, Juranek DD. Precautions against biological and chemical terrorism directed at food and water supplies. Public Health Rep 2001; 116: 3-14.
- 5. Amy G, Bull R, Craun GF. Environmental health criteria 216: disinfectants and disinfectant by-products. Geneva: World Health Organization, 2000.
- 6. Swerdlow DL, Mintz ED, Rodriguez M, et al. Waterborne transmission of epidemic cholera in Trujillo, Peru: lessons for a continent at risk. Lancet 1992; 340: 28-33.
- 7. Safe SH. Endocrine disruptors and human health — is there a problem? An update. Environ Health Perspect 2000; 108: 487-493.
- 8. Curriero FC, Patz JA, Rose JB, Lele S. The association between extreme precipitation and waterborne disease outbreaks in the United States, 1948-1994. Am J Public Health 2001; 91: 1194-1199.
- 9. Epstein PR. Climate change and emerging infectious diseases. Microbes Infect 2001; 3: 747-754.
- 10. Patz JA, McGeehin MA, Bernard SM, et al. The potential health impacts of climate variability and change for the United States: executive summary of the report of the health sector of the US National Assessment. Environ Health Perspect 2000; 108: 367-376.
- 11. National Health and Medical Research Council/Agricultural and Resource Management Council of Australia and New Zealand. Australian Drinking Water Guidelines. Canberra: NHMRC/ARMCANZ: 1996. <http: //www.health.gov.au/nhmrc/publications/synopses/eh19syn.htm>
- 12. Cunliffe D. Guidance on the use of rainwater tanks. National Environmental Health Forum Monographs, 1998. Report No: Water Series No. 3.
- 13. National water quality management strategy: guidelines for sewerage systems — use of reclaimed water. Canberra: Agriculture and Resource Management Council of Australia and New Zealand, Australian and New Zealand Environment and Conservation Council, National Health and Medical Research Council, 2000.
- 14. Ford TE, MacKenzie WR. How safe is our drinking water? Despite technologic advances, waterborne disease is still a threat. Postgrad Med 2000; 108: 11-14.
- 15. Walker NI. Copper toxicosis in an Australian child. Eur J Med Res 1999; 4: 249-251.
- 16. Cantor KP. Drinking water and cancer. Cancer Causes Control 1997; 8: 292-308.
- 17. Hildesheim ME, Cantor KP, Lynch CF, et al. Drinking water source and chlorination byproducts. II. Risk of colon and rectal cancers. Epidemiology 1998; 9: 29-35.
- 18. Nieuwenhuijsen MJ, Toledano MB, Eaton NE, et al. Chlorination disinfection byproducts in water and their association with adverse reproductive outcomes: a review. Occup Environ Med 2000; 57: 73-85.
- 19. Demos LL, Kazda H, Cicuttini FM, et al. Water fluoridation, osteoporosis, fractures — recent developments. Aust Dent J 2001; 46: 80-87.
- 20. Review of water fluoridation and fluoride intake from discretionary fluoride supplements. Review for the National Health and Medical Research Council. Melbourne: RMIT University, Monash University, 1999.
- 21. Byth S. Palm Island mystery disease. Med J Aust 1980; 2: 40-42.
- 22. Veitch MGK, Johnson PDR, Flood PE, et al. A large localized outbreak of Mycobacterium ulcerans infection on a temperate southern Australian island. Epidemiol Infect 1997; 119: 313-318.
- 23. Cases of leptospirosis in hunters in the Top End — don't go barefoot. Commun Dis Intell 2000; 24: 384.
- 24. Centers for Disease Control and Prevention. Update: outbreak of acute febrile illness among athletes participating in Eco-Challenge-Sabah 2000–Borneo, Malaysia, 2000. JAMA 2001; 285: 728-730.





Abstract
The risk of contamination of drinking water supplies with microbial pathogens is minimised by modern approaches to water management, but continues to be the major public health concern.
Chemical contaminants usually pose little health risk except at very high levels, but debate continues over the potential adverse health effects of low-level, chronic exposure to compounds such as disinfection byproducts.
Recreational water contact can be associated with adverse health outcomes either from microbial infections or exposure to cyanobacterial toxins.
Environmental issues such as increasing salinity and global warming are likely to affect the sustainability of our current drinking water supplies and increase the threat of waterborne disease outbreaks.
New technologies, use of alternative water sources, such as rainwater tanks, water reuse and restrictions will undoubtedly be part of the solution to our diminishing water resources, but have the potential to introduce new health threats.