Climate change, combined with the way we produce, distribute and consume food, has the potential to affect foodborne disease in the coming century. It is predicted that global warming, with its effect on temperature and rainfall (more storms in some areas and drought in others), will adversely affect food and water supplies, and that by 2100 an extra 80 to 90 million people will be hungry or malnourished.1 Climate change has the potential not only to decrease food supplies, but also to increase microbial and toxic contamination of foods.2
In addition, changing technology is creating new concerns about food safety. Medical practitioners may be consulted about the safety of take-away and pre-packaged foods, genetically modified foods, and toxins and allergens in food, as well as the risk of bovine spongiform encephalopathy.
We will discuss recent changes to the patterns of foodborne disease and the evidence that climate change may increase microbial and toxic contamination of food.
About four million cases of foodborne infectious disease are estimated to occur annually in Australia.3 The pattern of enteric diseases has changed considerably since the 19th century, with improved sanitation and water supplies. Nowadays, commonly reported pathogens include Salmonella spp. (causing 1%–2% of cases of community gastroenteritis), Campylobacter spp. (3%) and caliciviruses (10%).4
In Australia, as in many other developed countries, notification rates for potentially foodborne infections have increased over recent decades. While this is probably partly because of improved laboratory techniques for identifying pathogens and better reporting to surveillance systems, another possible reason is changing consumer behaviour — people are less likely to eat food cooked at home, favouring more takeaway and pre-packaged meals, which may carry higher risks if poorly prepared. More complex and globalised patterns of food production and distribution have resulted in outbreaks that are sometimes global in scale, such as the 2001 outbreak of Salmonella infection caused by peanuts imported into Australia and several other countries.5 On the other hand, large-scale commercial food processing may also decrease food contamination, as safety procedures are often stricter.
Outbreaks of infection are increasingly caused by novel foodborne organisms, such as Escherichia coli O111 and O157 (often caused by eating rare beef), Listeria spp. (generally a problem in immunocompromised people and pregnant women) and Cryptosporidium spp. (transmissible by food as well as water). Of concern is the development of antibiotic resistance among some pathogens, possibly because of antibiotic use in animal feeds,6 as well as overprescribing.
A link between climate and microbial foodborne disease remains speculative. Evidence for this link comes from the observed seasonality and latitudinal gradients in the amount of foodborne and diarrhoeal illnesses, changing disease patterns during El Niño warmings, and links between waterborne7 and foodborne8 illnesses and weather disturbances (Box 1). Some weather events affect water quality, which may lead to subsequent food contamination. A statistical association between disease and short-term temperature changes also suggests that foodborne disease will be affected by long-term climate changes.14,16
In developing countries, poor hygiene and sewage disposal, inadequate facilities for food preparation and storage and lack of potable water contribute to a high incidence of diarrhoea.18 The incidence generally rises in summer, but the reasons for this may vary in different environments. For example, seasonal lack of food may lead to seasonal malnutrition and hence susceptibility to infectious foodborne disease in some areas,19 while temperature and rainfall may have direct effects on growth and dissemination of pathogens in others.
In Australia, the most reliable data on foodborne disease are probably for Salmonella infections, although probably as few as 5%–10% of people with such infections in the community visit their doctor, and have a positive stool sample reported to surveillance (unpublished data, OzFoodNet, 2002). Australian surveillance data show that Salmonella infections increase in summer, while Campylobacter infections increase in spring20 (Box 2), similar to patterns seen overseas. The different timing of the peaks in Salmonella and Campylobacter notifications suggest that different mechanisms are responsible for their seasonality.
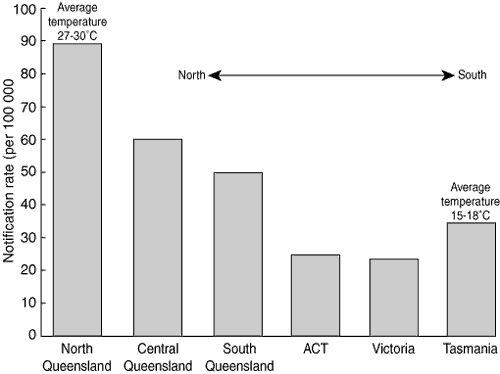
In eastern Australia, rates of Salmonella notifications increase with decreasing latitude and consequently with increasing average yearly temperature (Box 3). Even allowing for confounding factors, such as regional variation in environmental conditions, populations, serovars and routes of transmission, the pattern suggests that climate is a possible influence on the level of salmonellosis in eastern Australia. The higher rates in Tasmania could be due to Salmonella Mississippi, an endemic serogroup found predominantly in that State. This serovar may have a higher transmission rate directly from the environment than from food.
Some health effects related to El Niño are shown in Box 1. Notable effects include epidemics of cholera in Peru12 and Bangladesh,15 increased diarrhoeal illness in Peru13 and widespread faecal contamination of seafoods in Florida.8
Foodborne outbreaks may be linked to storms, as rainfall and runoff can help disseminate pathogens.8 Fresh fruit and vegetables may be contaminated by waterborne pathogens, such as the protozoa Cyclospora and Cryptosporidium spp.11 Seafoods may be contaminated by bacteria24 and enteric viruses that can survive sewage treatment and long periods in sea water.25
Food poisoning outbreaks may also be linked to unusually hot weather which can enhance bacterial replication. Reports of food poisoning outbreaks were higher during unusually hot summers in both the United Kingdom and Australia.17,23
Caution is required before inferring that climatic temperature is a direct cause of foodborne disease. Temperature may be a marker for other factors that change seasonally or with locality (eg, animal reproductive cycles), or seasonal variation in farming practices (eg, fertiliser application). There may also be confounding or biases in data collection methods. Nevertheless, the evidence suggests that a causal relationship between temperature variation and salmonellosis and some other foodborne illnesses is possible.
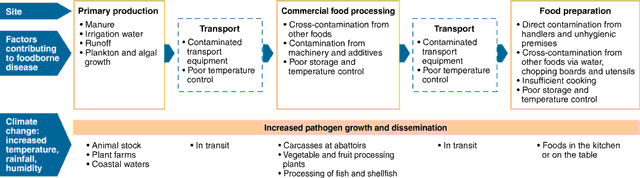
Poor hygiene and temperature control during food production, processing, transport, preparation or storage may interact with climate change, allowing pathogens to multiply (Box 4). The most commonly identified or suspected food vehicles reported in food-related outbreaks in Australia are poultry, red meat, fish, shellfish and salad.5 Some new pathogens have emerged due to changed food production conditions which favour proliferation of some pathogens rather than others (eg, Salmonella spp.), while others have become recognised with new identification techniques (eg, toxigenic E. coli).
Changing climate may also influence human exposure to natural and man-made toxins. For example, higher ocean temperatures may increase the incidence of ciguatera poisoning.26 This serious illness is associated with eating large fish that have accumulated toxins produced by dinoflagellates growing on bleached coral reefs.27 The illness is characterised by diarrhoea, vomiting and abdominal pain, then paraesthesiae and other neurological effects which may persist for weeks. In Australia, in 2001, five out of six reported outbreaks of ciguatera occurred in Queensland through amateur fishermen catching and eating contaminated fish.5 With higher surface ocean temperatures, the distribution of affected reefs may expand.
Higher global temperatures could increase human exposure to toxins produced by cyanobacteria (blue-green algae) in water supplies and recreational water bodies, which can cause gastrointestinal and dermatological symptoms.28 Similarly, production of mycotoxins in agricultural produce could increase. These include aflatoxins, which are produced by fungi growing in stored grains and nuts in hot, humid conditions and which are hepatotoxic and carcinogenic.29
Changing weather patterns may increase pests in crops and consequent use of agrochemicals, potentially exposing humans to greater concentrations of man-made chemicals. Genetically modified foods may become more common as the world attempts to feed a larger population and to control pests by developing strains resistant to infestation. The possible health effects of these foods are as yet unknown.30
In Australia, it is estimated that global warming will cause temperatures to rise 0.4o–2oC by 2030, and 1o–6oC by 2070.31 Assuming that a sustained temperature rise has a similar effect to monthly temperature variations, then the incidence of salmonellosis may rise, and, by extrapolation, the incidence of diseases caused by other foodborne pathogens and toxins could also rise (Box 5). Some communities might be more vulnerable to these effects than others, depending on the technology available to control food production and transport to provide "buffering" against the environmental change.
Regulatory authorities are currently attempting to implement food safety systems based on the international standard procedure HACCP (Hazard Analysis and Critical Control Point; Box 6). With modern complex processing and widespread distribution of foods, and the potential effects of climate change, HACCP will need to be applied even more stringently.
Needless to say, if it becomes clear in future that foodborne diseases are increasing in response to climate changes, then the primary preventive measure is to limit human-induced greenhouse gas emissions.
1: Some episodes of food and waterborne infection related to climate and weather
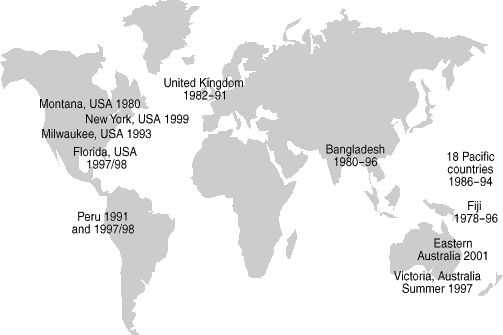
Montana, USA (1980): Waterborne outbreak of giardiasis associated with heavy rainfall (980 cases)9
New York State, USA (1999): Waterborne outbreak of E. coli O157: H7 related to heavy rainfall10
Milwaukee, USA (1993): Waterborne outbreak of cryptosporidiosis associated with heavy rainfall and run-off (403 000 cases, 54 deaths)7
Florida (1997–1998): Human enteroviruses; greater faecal contamination of waters and shellfish associated with heavy rainfall caused by El Niño11
Peru (1991): Waterborne cholera epidemic associated with El Niño (250 000 cases)12
Peru (1997–1998): Increase in hospital admissions for diarrhoea in Lima associated with El Niño13
United Kingdom (1982–1991): Food poisoning associated with monthly temperature (estimated potential extra 179 000 cases with 2.1°C temperature rise)14
Bangladesh (1980–1996): Rise in cholera cases during El Niño15
Pacific countries (1986–1996): Incidence of diarrhoea related positively to average annual temperature and negatively to water availability16
Fiji (1978–1998): Incidence of diarrhoea increased with temperature and extreme rainfall16
Eastern Australia (2001): Increased rates of Salmonella infection with decreasing latitude (corresponding to higher ambient temperatures)5
Victoria, Australia (1997): Increased outbreaks of foodborne disease during hottest summer on record17
2: Total monthly notifications of Salmonella and Campylobacter infections in Australia, 1991–200020
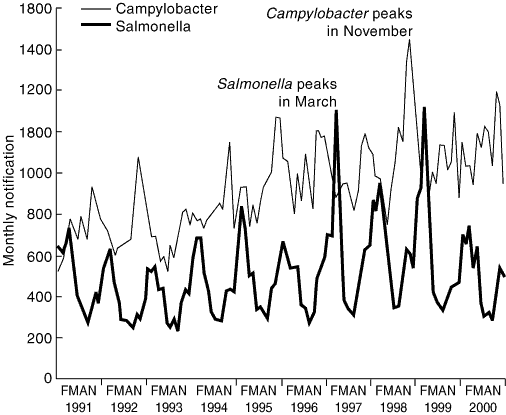
Salmonella notifications peak in summer, one to two months after summer temperature peaks, while Campylobacter notifications peak in spring, before temperature peaks. It is plausible that temperature has a direct effect on Salmonella numbers, as these organisms can replicate outside animal or human hosts.21 Higher environmental temperatures may increase their replication in manure and consequently enhance transmission between animals, especially in crowded conditions (pictured). Higher temperatures also promote replication in food. Hospital admissions for Salmonella infection show a similar seasonal pattern to notifications.22
In contrast, as Campylobacter spp. require specific conditions to replicate (including a temperature of 30°C), they are most unlikely to do so outside an animal or human host.21 The Campylobacter peak in spring is therefore more likely to be related to an intermediary event triggered by temperature. As the organism is carried by birds, one hypothesis is that this event may be some aspect of bird behaviour.23

Modern farming methods raise the possibility of mass infection of foodstuffs due to crowded conditions and enhanced transmission of pathogens among stock.
3: Age-standardised notification rates of Salmonella infections, by latitude, in eastern Australia, 20015
5: Reflections and predictions
Circa 1900
In Australia, foodborne outbreaks were localised, as foods were not distributed widely, and most meals were prepared at home.
Enteric fever, cholera and dysenteric illness predominated, caused by poor hygiene and sanitation, and contaminated milk and water.
Salmonellosis, shigellosis and paratyphoid fever were not recognised diseases.
Enteric diseases were seasonal, with higher rates in summer,32 and were a significant cause of mortality, especially in children aged under one year.
Circa 2100
New foodborne pathogens and larger-scale foodborne outbreaks continue to emerge owing to improved recognition, changed food production and processing techniques, and changed eating habits.
Climate change may interact with increasingly complex food production methods to potentiate foodborne disease and lead to global outbreaks.
A temperature rise of 1o–6oC in Australia may cause a rise in salmonellosis, and a rise in the overall incidence of foodborne infectious disease.
Toxic contamination of foods may increase through greater use of agrochemicals to control increased pests in a warmer climate.
Illness from natural toxins, such as ciguatera, may rise as the warmer climate leads to more marine algal blooms that affect fish in the human food chain.
Genetically modified foods are likely to be produced more widely to counteract diseases caused by global warming.
6: Principles of Hazard Analysis and Critical Control Point (HACCP) safety procedures33
Identify potential hazards associated with food, such as microbes and chemicals, and means to control them.
Identify critical points in food production where the potential hazard can be controlled (eg, on the farm, packaging).
Establish preventive measures with critical limits for each control point (eg, minimum cooking temperature and time).
Monitor critical points.
Take corrective actions when a critical limit has not been met (eg, disposing of food if the minimum temperature has not been achieved).
Verify that the system is working properly (eg, verify that time and temperature devices are working properly).
Maintain proper records of procedures.
- Gillian V Hall1
- Rennie M D'Souza2
- Martyn D Kirk3
- 1 National Centre for Epidemiology and Population Health, Australian National University, Acton, ACT.
- 2 Food Safety Australia, Food Standards Australia New Zealand, Melbourne, VIC.
We acknowledge the Communicable Diseases Network Australia, National Notifiable Diseases Surveillance System, for providing data for notifications of Salmonella and Campylobacter and the Queensland Department of Natural Resources and Mines
None identified.
- 1. McMichael AJ, Campbell-Lendrum D, Kovats S, et al. Comparative risk assessment: climate change. Draft report for the World Health Organization. London, UK: Centre on Global Change and Health, London School of Hygiene and Tropical Medicine; 2002.
- 2. Patz J, Engelberg E, Last J. The effects of changing weather on public health. Annu Rev Public Health 2000; 21: 271-307.
- 3. Australian and New Zealand Food Authority. Food safety standards costs and benefits. Canberra: ANZFA, 1999.
- 4. Sinclair M, Hellard M, Wolfe R, Fairley C. Pathogens causing community gastroenteritis in Australia. Abstracts of the Annual Scientific Meeting of the Australian Society for Infectious Diseases. Barossa, 2002.
- 5. Ashbolt R, Gregory J, Givney R, et al. Enhancing foodborne disease surveillance across Australia in 2001: the OzFoodNet Working Group. Comm Dis Intell 2002; 26: 375-406.
- 6. Barza M, Travers K. Excess infections due to antimicrobial resistance: the "attributable fraction". Clin Infect Dis 2002; 34 Suppl 3: S126-S130.
- 7. Curriero F, Patz J, Rose J, Lele S. The association between extreme precipitation and waterborne disease outbreaks in the United States, 1948-1994. Am J Public Health 2001; 91: 1194-1199.
- 8. Rose JB, Epstein PR, Lipp EK, et al. Climate variability and change in the United States: potential impacts on water and foodborne diseases caused by microbiologic agents. Environ Health Perspect 2001; 109 Suppl 2: 211-221.
- 9. Weniger B, Blaser M, Gedrose J, et al. An outbreak of waterborne giardiasis associated with heavy water runoff due to warm weather and volcanic ashfall. Am J Public Health 1983; 73: 868-872.
- 10. Centers for Disease Control. Outbreaks of Escherichia coli O157: H7 infection and Campylobacter among attendees of the Washington County Fair — New York. 1999. MMWR Morb Mortal Wkly Rep 1999; 48: 803-804.
- 11. Rose J, Slifko T. Giardia, Cryptosporidium, and Cyclospora and their impact on foods: a review. J Food Protection 1999; 62: 1059-1070.
- 12. Colwell R. Global climate and infectious disease: the cholera paradigm. Science 1996; 274: 2025-2031.
- 13. Checkley W, Epstein L, Gilman R, Figueroa D, et al. Effects of El Nino and ambient temperature on hospital admissions for diarrhoeal diseases in Peruvian children. Lancet 2000; 355: 442-450.
- 14. Bentham G, Langford I. Climate change and the incidence of food poisoning in England and Wales. J Biometeorol 1995; 39: 81-86.
- 15. Pascual M, Rodo X, Ellner S, et al. Cholera dynamics and El Nino southern oscillation. Science 2000; 289: 1766.
- 16. Singh R, Hales S, de Wet N, et al. The influence of climate variation and change on diarrheal disease in the Pacific Islands. Environ Health Perspect 2001; 109: 155-159.
- 17. Lester R, Carnie J, McLennan L, et al. Salmonella in Victoria, 1997: the story so far. Comm Dis Intell 1997; 21: 120-123.
- 18. Guerrant RL, Kirchhoff LV, Shields DS, et al. Prospective study of diarrheal illnesses in northeastern Brazil: patterns of disease, nutritional impact, etiologies, and risk factors. J Infect Dis 1983; 148: 986-997.
- 19. Samani E, Willett W, Ware J. Association of malnutrition and diarrhea in children aged under five years. Am J Epidemiology 1988; 128: 93-105.
- 20. National Notifiable Diseases Surveillance System. Communicable Diseases Network of Australia. Canberra. Available at <http://www.health.gov.au/pubhlth/cdi/cdihtml.htm> (originally accessed Nov 2002, now (Nov 2005) available at http://www.health.gov.au/internet/wcms/publishing.nsf/Content/Nationally+notifiable+diseases+(NNDSS)-2).
- 21. Hocking A, Arnold G, Jenson I, et al, editors. Foodborne microorganisms of public health significance. Sydney: Australian Institute of Food Science and Technology, Food Microbiology Group, NSW Branch, 1997.
- 22. Australian Institute for Health and Welfare national hospital morbidity database. Canberra: AIHW, 2002. Available from <http://www.aihw.gov.au/hospitaldata/datacubes/index.html> (accessed Nov 2002).
- 23. Gillespie I. The application of logistic regression to provide maximum likelihood estimates of factors affecting food borne general outbreaks of infectious intestinal disease [dissertation]. London: London School of Hygiene and Tropical Medicine, 2001, 114.
- 24. Tauxe R. Emerging foodborne diseases: an evolving public health challenge. Emerg Infect Dis 1997; 3: 425-434.
- 25. Birch C, Gust I. Sewage pollution of marine waters : the risks of viral infection. Med J Aust 1989; 151: 609-610.
- 26. Epstein P, Ford T, Colwell R. Marine ecosystems. Lancet 1993; 342: 1216-1219.
- 27. Lehane L. Ciguatera update. Med J Aust 2000; 172: 176-179.
- 28. El Saadi O, Esterman A, Cameron S, Roder D. Murray River water, raised cyanobacterial cell counts, and gastrointestinal and dermatological symptoms. Med J Aust 1995; 162: 122-125.
- 29. Peraica M, Radic B, Lucic A, Pavlovic M. Toxic effects of mycotoxins in humans. Bull World Health Organ 1999; 77: 754-766.
- 30. Leeder S. Genetically modified foods — food for thought. Med J Aust 2000; 172: 170-173. <eMJA full text>
- 31. Commonwealth Scientific and Industrial Research Organisation. Climate change projections for Australia. Melbourne Climate Impact Group, CSIRO Division of Atmospheric Research, 2001.
- 32. Cumpston J. Health and disease in Australia. A history. Canberra: AGPS, 1989.
- 33. United States Food and Drug Administration. HACCP: A state-of-the-art approach to food safety. FDA Backgrounder. Available at <http://www.cfsan.fda.gov/~lrd/bghaccp.html> (accessed Jul 2002).





Abstract
About four million cases of foodborne infectious disease occur annually in Australia; new foodborne pathogens, such as enterohaemorrhagic Escherichia coli, are emerging.
Climate change, combined with changes in how we produce and distribute food and how we behave as consumers, have the potential to affect foodborne disease in the coming century.
Foodborne disease outbreaks are now more far-reaching (and sometimes global) due to modern mass food production and widespread food distribution.
There are strong seasonal patterns for Salmonella and Campylobacter infection in Australia.
Global warming may increase the incidence of infections, such as salmonellosis, and diseases caused by toxins, such as ciguatera.