Several studies quantifying the impact of poor communication on clinical work suggest that communication is a likely cause of systematic error in the health system. In Australia, inadequate communication has been associated with 17% of system problems, and, of these, 84% were deemed potentially preventable.1 About 50% of all adverse events detected by general practitioners were associated with communication difficulties.2 Within intensive care units, 2% of the activity consists of verbal communication between nurses and doctors, but accounts for 37% of error reports.3 Thus, the evidence strongly suggests that poor communication wastes time, threatens patient care and may be one of the chief culprits behind preventable adverse events in clinical practice.4
The research reported here extends work begun in the United Kingdom in the mid-1990s,5,6 in which it was found that physician teams in hospital were subject to high levels of interruption. Clinical staff also appeared to bear a higher communication load than necessary, considering the many tasks that could be accomplished by accessing information sources rather than asking questions of people. It has since been hypothesised that such interruptions impose cognitive loads on clinical staff and have a negative impact on memory, leading to clinical error.7
As a continuation of this research, we measured communication load more precisely and studied communication patterns in a high-workload clinical setting.
The communication load on clinical staff was measured by the proportion of observed time spent in communication, the proportion of communication events involving concurrent communication tasks, and the proportion of interruptions experienced by subjects. We calculated the rates of communication events and interruptions and 95% CIs for counted variables.
Patterns of communication were examined by classifying communication events into informal (face-to-face conversation, telephone, pager, letter, whiteboard and email) or formal (patients' medical records, computer information system, test results, forms, medical literature, drug manuals); the purpose of communication (eg, test ordering, results gathering or exchange of information); and by the channel of communication (synchronous or asynchronous; see Glossary, Box 1).
The six nurses and six doctors were observed in June and July 1999. During the 35 hours and 13 minutes of observation time, 1286 distinct communication events were identified, representing an average of 36.5 events per person per hour (95% CI, 34.5–38.5). The medical staff experienced 33.6 events per hour (n = 625; 95% CI, 31.0–36.2) and nursing staff 39.8 per hour (n = 661; 95% CI, 36.7–42.8) (Box 2).
Almost 89% (n = 1141) of all events involved the use of a synchronous channel (Box 2). Of the possible synchronous channels, face-to-face conversation clearly was dominant, accounting for 82% (n = 1055) of all conversation events (87.1% for nurses, 76.6% for doctors). Informal communication sources accounted for 89.6% (n = 1152) of events (92.4% for nurses and 86.6% for doctors).
Fewer communications, 12.3% (n = 158) (10.4% for nurses and 14.2% for doctors), involved formal information sources (Box 2).
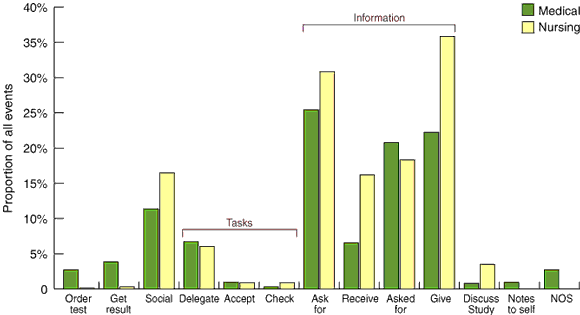
Events were analysed by the purpose of the task being carried out. Test-ordering (1.5% of events) and results-gathering (2.2% of events) accounted for only a few events, and the bulk (94.8%) were related to the exchange of information between clinical staff (Box 3).
This information exchange was sub-categorised as "asking" or "being asked for" information, and "giving" or "receiving" information. While medical staff asked for information slightly less than nursing staff (25.4% [n = 159] v 30.9% [n = 204]), they received information much less frequently (6.6% [n = 41] v 16.2% [n = 107]). Medical staff seemed to be asked for information as often as nurses (20.8% [n = 130] v 18.3% [n = 121]) but seemed to give information less frequently (22.2% [n = 139] v 35.8% [n = 237]).
Our study involved a relatively small sample of subjects and this must be taken into consideration in any discussion of results. The level of interruption, with about 90% of information transactions involving informal communication rather than interaction with formal information sources, was also highlighted in the original study.6 Further, since our study was completed a very similar result of 10.3 interruptions per hour has been reported for US emergency departments.8 Interruptions are an important measure of communication load, as an interruption can disrupt memory and generate errors.7 The level of multitasking we found is also of concern, as it too may affect memory. The number of items that can be held in memory is very small and several concurrent tasks may overload memory.9 The combination of multitasking and interruption may be a potent cocktail and a potential source of error.
Our results support those advocating specific communication training in emergency departments, operating rooms, and other high-interaction workplaces.10 Specific strategies to reduce interruptions have been suggested elsewhere5,6 and include:
Education to increase awareness of the costs of interruption;
Increased use of asynchronous communication tools like email and voicemail;
Communal communication tools such as message boards, which are well suited to the emergency department setting, as staff are mostly physically collocated.
We found that there were nine times as many informal interactions as there were formal. When considered from an information flow perspective, this is staggering; it suggests that there is a low upper limit on the potential for electronic medical records (EMRs) to improve information processes within healthcare organisations, since the EMR is essentially a formal medium. These findings are consistent with study results from another hospital with EMRs in which 50% of information transactions were still face to face.11 More positively, it suggests that small improvements in communication may substantially benefit information processes within our organisations, potentially providing greater benefits than EMRs.
Medical staff had fewer information-seeking and -receiving interactions than nursing staff. This may be because they either have a lower information need, or are less likely to seek information than nursing staff. They also seemed to get less information than they asked for. This suggests that medical staff may not be satisfying all the information requests that they receive, nor satisfying all the information requests they themselves make. It fits with the higher communication load they seem to carry as measured by the multitasking measure. Medical staff may need to have a reduced communication load, or a reduction in peak loading. It is also interesting to find out whether the questions asked by doctors are less easily answered, less well articulated, or perhaps less well delivered.
The picture of communication within the emergency department suggests that communication processes dominate information exchanges, and that communication may be strained because of the communication loads on individual clinical staff. It suggests that active training to improve team communication, as well as optimisation of communication processes, have the potential to substantially improve clinical work, and may have a positive impact on clinical outcomes.
While it was not the purpose of this study to correlate communication loads with errors or poor outcomes, such studies need to be done. Further research is needed to replicate these findings in other clinical settings, with a view to ensuring that communication processes are considered in any program to reduce error and improve the quality and safety of healthcare delivery.
1: Glossary
Formal communication: When a message conforms to a predetermined structure (ie, is in a predefined form).
Informal communication: When the message structure is determined solely by the conversing parties.
Synchronous communication: When two parties exchange messages across a communication channel at the same time (eg, telephone).
Asynchronous communication: When communication exchange does not require both parties to be active in the conversation at the same time (eg, email). The recipient can deal with communication at a time of his or her choosing.
Interruption: A communication event in which the subject did not initiate the conversation, and which used a synchronous communication channel.
Multitasking: A period when two or more concurrent communication events occur.
2: Summary of communication data for the 12 clinical staff in the study
Medical staff |
Nursing staff |
Total |
|||||||||
Communication events |
|||||||||||
Number of events |
625 |
661 |
1286 |
||||||||
Observation time (hours) |
18:36 |
16:37 |
35:13 |
||||||||
Total event time (hours) |
14:38 |
13:33 |
28:12 |
||||||||
Overlap time (hours) |
2:42 |
1:04 |
3:48 |
||||||||
Number of communication events initiated by subject |
421 |
472 |
893 |
||||||||
Number of interruptions |
208 |
185 |
393 |
||||||||
Communication channels (number of events) |
|||||||||||
Face to face |
479 |
576 |
1055 |
||||||||
Telephone |
41 |
25 |
66 |
||||||||
Pager |
17 |
3 |
20 |
||||||||
Computer |
29 |
21 |
50 |
||||||||
Patient's medical record |
34 |
31 |
65 |
||||||||
Forms |
20 |
16 |
36 |
||||||||
Medical literature |
3 |
1 |
4 |
||||||||
Test results |
3 |
0 |
3 |
||||||||
Drug manual |
0 |
0 |
0 |
||||||||
Letter |
4 |
1 |
5 |
||||||||
Whiteboard |
0 |
6 |
6 |
||||||||
0 |
0 |
0 |
|||||||||
As each communication event could involve more than two people or more than one purpose, some had multiple classifications. |
|||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
Received 25 July 2001, accepted 20 December 2001
- Enrico W Coiera1
- Rohan A Jayasuriya2
- Jennifer Hardy3
- Aiveen Bannan
- Max E C Thorpe5
- 1
- 2 Faculty of Medicine, University of New South Wales, NSW.
- 3 School of Public Health, University of Wollongong, Wollongong, NSW.
- 4 Faculty of Health Sciences, Australian Catholic University, North Sydney, NSW.
- 5 Prince of Wales Hospital Clinical School, Randwick, NSW.
Associate Professor Johanna Westbrook kindly assisted in the statistical analysis of the data. This work was funded by a grant from the New South Wales Department of Health.
None declared.
- 1. Australian Health Ministers' Advisory Council. The final report of the Taskforce on Quality in Australian Health Care. Canberra: Australian Health Ministers' Advisory Council, 1996.
- 2. Bhasale AL, Miller GC, Reid SE. Analysing potential harm in Australian general practice: an incident-monitoring study. Med J Aust 1998; 169: 73-76.
- 3. Donchin Y, Gopher D, Olin M, et al A look into the nature and causes of human errors in the intensive care unit. Crit Care Med 1995; 23: 294-300.
- 4. Gosbee J. Communication among health professionals. BMJ 1998; 316: 642.
- 5. Coiera E. Clinical communication: A new informatics paradigm. Proceedings of the American Medical Informatics Association, Washington DC, Autumn Symposium 1996; J Am Med Informatics Assoc Symposium Supplement 1996; 17-21.
- 6. Coiera E, Tombs V. Communication behaviours in a hospital setting: an observational study. BMJ 1998; 316: 673-676.
- 7. Parker J, Coiera E. Improving clinical communication: A view from psychology. J Am Med Informatics Assoc 2000; 7: 453-461.
- 8. Chisholm C, Collison K, Nelson D, Cordell W. Emergency department workplace interruptions. Acad Emerg Med 2000; 7: 1239-1243.
- 9. Reason J. Human error. New York: Cambridge University Press, 1990.
- 10. Williams KA, Rose WD, Simon R. Teamwork in Emergency Medical Services. Air Med J 1999; 18: 149-153.
- 11. Safran C, Sands DZ, Rind DM. Online medical records: a decade of experience. In: Moorman PW, van der Lei J, Musen MA, editors. Proceedings of EPRiMP: The International Working Conference on Electronic Patient Records in Medical Practice. Rotterdam, The Netherlands: IMIA, 1998: 128-132.





Abstract
Objective: To measure communication loads on clinical staff in an acute clinical setting, and to describe the pattern of informal and formal communication events.
Design: Observational study.
Setting: Two emergency departments, one rural and one urban, in New South Wales hospitals, between June and July 1999.
Participants: Twelve clinical staff members, comprising six nurses and six doctors.
Main outcome measures: Time involved in communication; number of communication events, interruptions, and overlapping communications; choice of communication channel; purpose of communication.
Results: 35 hours and 13 minutes were observed, and 1286 distinct communication events were identified, representing 36.5 events per person per hour (95% CI, 34.5–38.5). A third of communication events (30.6%) were classified as interruptions, giving a rate of 11.15 interruptions per hour for all subjects; 10% of communication time involved two or more concurrent conversations; and 12.7% of all events involved formal information sources such as patients' medical records. Face-to-face conversation accounted for 82%. While medical staff asked for information slightly less frequently than nursing staff (25.4% v 30.9%), they received information much less frequently (6.6% v 16.2%).
Conclusion: Our results support the need for communication training in emergency departments and other similar workplaces. The combination of interruptions and multiple concurrent tasks may produce clinical errors by disrupting memory processes. About 90% of the information transactions observed involved interpersonal exchanges rather than interaction with formal information sources. This may put a low upper limit on the potential for improving information processes by introducing electronic medical records.