Faecal incontinence is a significant cause of social embarrassment and imposes a high cost on the patient and the community. It can be physically and psychologically disabling, leading to progressive isolation and a devastating social impact. It is the second most common cause for institutionalisation of the elderly in the USA,2,3 and accounts for costs of over US$400 000 000 per year for adult diapers.4 Borrie et al estimated that the annual cost of incontinence for an institutionalised patient in Canada was C$9771.5 Patients suffering from faecal incontinence may be reluctant to seek medical advice,6,7 and doctors may be reluctant to ask about the condition.
Reports of the prevalence of faecal incontinence in the community have shown significant variability.1,8-13 An accurate estimation of the magnitude of the problem in the community would help in providing knowledge of who is at greatest risk so that preventive measures can be applied. For this reason, we undertook a population-based study of the epidemiology of faecal incontinence, using a self-administered questionnaire. We aimed to ascertain the prevalence of faecal incontinence in the community sample, evaluate the health-seeking behaviour in people afflicted by faecal incontinence, determine its associated risk factors, and assess the impact of the condition on quality of life.
This study was formally approved by the Wentworth Area Health Service's ethics committee. The samples were drawn randomly from the Lindsay electoral roll, an electoral region in western Sydney, Australia. Since voting is compulsory for all citizens 18 years and over in Australia, the Electoral Commission in each State routinely registers and updates the lists of citizens in each electorate. The population sampling frame is demographically similar to the Australian population, except that its inhabitants are slightly younger and have a slightly higher socioeconomic status.14 The survey consisted of a self-administered questionnaire sent out to 990 residents in two stages in 1997 and 1998 (stratified for equal numbers of men and women).
Most of the questionnaire items had been previously validated in Australian and US populations.14-16 Two forms of the questionnaire were used. A long form, consisting of 32 questions, assessed bowel habit, laxative use, presence and severity of faecal incontinence, previous suspected risk factors for faecal incontinence, health-seeking behaviour, degree of mobility, and social impact of faecal incontinence (n = 770 subjects). A short form, with seven questions on a single page, was a pruned version of the longer questionnaire, primarily aimed to assess the presence of faecal incontinence (n = 220 subjects). In the first stage, 440 questionnaires were sent out (220 short and 220 long). In the second stage, long questionnaires were mailed to a further 550 randomly selected residents. We used the two questionnaire formats to evaluate which would be optimal in achieving higher response rates (results reported elsewhere).17
We defined faecal incontinence as an involuntary loss of anal sphincteric control that led to unwanted release of liquid or solid faeces (not flatus) at an inappropriate time or in an inappropriate place. Symptoms were measured over the past 12 months, the standard time frame in our previously validated questionnaires.15 Faecal incontinence related to an acute illness (eg, acute diarrhoea) was excluded. Quality of life was measured by asking about interference with social activities or lifestyle.15 We also enquired about perceived level of health, mobility and independence.
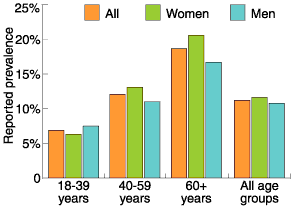
Faecal incontinence was reported by 72 of 642 responders (incomplete data for nine responders), yielding a prevalence of 11.2% (95% CI, 8.8%–13.7%). This was similar among men (31/286 [10.8%]; 95% CI, 7.2%–14.4%) and women (41/353 [11.6%]; 95% CI, 8.3%–15.0%). The prevalence of solid and liquid faecal incontinence was 2.0% (13/642; 95% CI, 0.9%–3.1%) and 9.0% (58/642; 95% CI, 6.8%–11.3%), respectively. Liquid faecal incontinence was reported by 8.8% of women (31/353; 95% CI, 5.8%–11.7%) and 9.4% of men (27/286; 95% CI, 6.1%–12.8%); solid faecal incontinence was reported by 1.1% of women (4/353; 95% CI, 0.03%–2.2%) and 3.1% of men (9/286; 95% CI, 1.1%–5.2%). The mean age of subjects with faecal incontinence was 53 years; 55% were women. Faecal incontinence was positively associated with age (χ2 = 11.75; P = 0.003) (Box 1).
After adjustment for age, the risk of faecal incontinence was significantly higher among those reporting injury or surgery in the perianal area (Box 2). Faecal incontinence was not associated with radiation treatment to the lower abdomen or pelvic area or with diabetes mellitus (Box 2).
Faecal incontinence was associated with a more than a threefold increase in the odds of reporting feelings of incomplete rectal evacuation, nearly a fivefold increase in the odds of reporting loose bowel movements, and over a fivefold increase in the odds of reporting stool urgency (Box 2). Faecal incontinence was not associated with straining on defecation or with hard or lumpy stool consistency (Box 2).
The odds of reporting fair or poor health (rather than good health) were significantly higher among people reporting faecal incontinence (Box 2). Twenty of the 72 people reporting faecal incontinence (28%; 95% CI, 17.4%–38.1%) reported some interference with their lifestyle. Nine of 48 (18.8%; 95% CI, 7.7%–29.8%) reported the need to change their underpants at least weekly because of faecal incontinence. Healthcare-seeking for faecal incontinence was reported by nine of 33 cases (27.3%; 95% CI, 12.1%–42.5%); doctor-initiated discussion of faecal incontinence was reported by just seven of 48 cases (14.6%; 95% CI, 4.6%–24.6%).
Daily or weekly episodes of faecal incontinence have previously been reported to occur in about 2% of the adult population and in about 7% of healthy independent adults over the age of 65.1,4,10 Community-based studies have shown prevalence rates of up to 16.9% in very old, independently living people.1,8,9,11,12,18,19 In this study, the prevalence was 11.2% — higher than in some previous community-based studies,1,8,11 but consistent with more recent studies12,13 (Box 3). The reason for this disparity may lie with the definition used as well as the study methodology. For example, Nelson et al used a telephone interview with a member of the household that asked about the health status of other household members.1 This method potentially underestimates the prevalence of faecal incontinence. Our random population sample should more realistically represent the community prevalence.
We found that the prevalence of faecal incontinence was similar in men and women (10.8% and 11.6%, respectively). Faecal incontinence has traditionally been thought to be more common in women,1,12,20 in part because obstetric trauma can result in unrecognised damage during childbirth. Obstetric injury to the pudendal nerve or sphincter muscle has been proposed as a primary risk factor for faecal incontinence.21,22 Irritable bowel syndrome, which is also more common in women, may be another risk factor.23 A few community-based studies show a higher prevalence of faecal incontinence in women,1,12,20 but others have shown a similar or even higher prevalence in men.8,11,13
Other causes of faecal incontinence are thought to include anal surgery, neurological disease and previously corrected congenital anorectal malformations.24,25 In our study, the prevalence of faecal incontinence was associated with advancing age as well as perianal surgery and injury. However, the prevalence of faecal incontinence was not significantly associated with diabetes or pelvic radiotherapy. Passage of loose or watery stool and urgency were all associated with faecal incontinence, suggesting that diarrhoea can overwhelm the mechanisms involved with maintaining continence. Feelings of incomplete rectal evacuation were also associated with incontinence, but straining was not. While feelings of incomplete defecation, possibly due to pelvic outlet obstruction, may seem to be a counterintuitive risk factor, faecal incontinence associated with faecal impaction and overflow incontinence is well described.26 An association between constipation and faecal incontinence has also been previously shown, which may be caused by pelvic nerve damage in this group of patients.27
Only nine of 33 individuals with faecal incontinence reported seeking medical attention (27.3%); only seven of 48 (14.6%) reported being asked about faecal incontinence by their medical practitioner. Johanson, on surveying patients during doctor visits, reported that 34% discussed their incontinence with the doctor.4 It is likely that patients visiting their doctors are a selected group. Enck et al have reported a systematic underestimation of faecal incontinence, finding that only 5% of patients with faecal incontinence, regardless of the underlying mechanism, had incontinence symptoms noted in the medical charts.6 It is not clear whether the lack of acknowledgement of faecal incontinence was mainly due to the patient's failure to volunteer the information or medical practitioners' reluctance to ask about it.
Many people with incontinence may not seek medical attention owing to the embarrassment associated with this condition, but medical practitioners may be even less likely to ask about this problem. This lack of interest may be because healthcare providers feel that little can be done for these patients other than antidiarrhoeal agents and diapers. With the advent of newer treatments, including surgical techniques and biofeedback,28 and professional awareness programs, doctors may usefully become more involved by asking directed questions about faecal incontinence.
2: Age-adjusted associations between faecal incontinence and bowel habit and potential risk factors (results from long questionnaire)*
Bowel habit |
||||
Potential risk factors |
||||
*Numbers vary because of incomplete responses to the questionnaire. †Odds ratios comparing people reporting faecal incontinence (cases) to non–cases. | ||||
3: Community-based studies of faecal incontinence (FI)
Received 9 February 2001, accepted 25 June 2001
- Jamshid S Kalantar1
- Stuart Howell2
- Nicholas J Talley3
- Department of Medicine, The University of Sydney, Nepean Hospital, Penrith, NSW.
We thank Dr Pauline Chiarelli, Newcastle University, for her assistance in preparing Box 3.
None declared.
- 1. Nelson R, Norton N, Cautley E, Furner S. Community-based prevalence of anal incontinence. JAMA 1995; 274: 559-561.
- 2. Cheskin L, Schuster M. Fecal incontinence. In: Hazzard W, Andres R, Bierman E, Blass J, editors. Principles of geriatric medicine and gerontology. New York: McGraw-Hill, 1990: 1143-1145.
- 3. Lahr C. Evaluation and treatment of incontinence. Practical Gastroenterol 1988; 12: 27-35.
- 4. Johanson JF, Lafferty J. Epidemiology of fecal incontinence: the silent affliction. Am J Gastroenterol 1996; 91: 33-36.
- 5. Borrie MJ, Davidson HA. Incontinence in institutions: costs and contributing factors. Can Med Assoc J 1992; 147: 322-328.
- 6. Enck P, Bielefeldt K, Rathmann W, et al. Epidemiology of faecal incontinence in selected patient groups. Int J Colorectal Dis 1991; 6: 143-146.
- 7. Leigh R, Turnberg L. Faecal incontinence: the unvoiced symptom. Lancet 1984; 12: 1349-1351.
- 8. Thomas TM, Egan M, Walgrove A, Meade TW. The prevalence of faecal and double incontinence. Community Med 1984; 6: 216-220.
- 9. Giebel GD, Lefering R, Troidl H, Blochl H. Prevalence of fecal incontinence: what can be expected? Int J Colorectal Dis 1998; 13: 73-77.
- 10. Talley NJ, O'Keefe EA, Zinsmeister AR, Melton LJ. Prevalence of gastrointestinal symptoms in the elderly: a population-based study. Gastroenterology 1992; 102: 895-901.
- 11. Drossman DA, Li Z, Andruzzi E, et al. US householder survey of functional gastrointestinal disorders. Prevalence, sociodemography, and health impact. Dig Dis Sci 1993; 38: 1569-1580.
- 12. Roberts RO, Jacobsen SJ, Reilly WT, et al. Prevalence of combined fecal and urinary incontinence: a community-based study. J Am Geriatr Soc 1999; 47: 837-841.
- 13. Lam L, Kennedy M, Chen F, et al. Prevalence of faecal incontinence: obstetric and constipation risk factors: a population based study. Colorectal Dis 1999; 1: 197-203.
- 14. Talley NJ, Boyce PM, Owen BK, et al. Initial validation of a bowel symptom questionnaire and measurement of chronic gastrointestinal symptoms in Australians. Aust N Z J Med 1995; 25: 302-308.
- 15. Talley NJ, Phillips SF, Melton J, et al. A patient questionnaire to identify bowel disease. Ann Intern Med 1989; 111: 671-674.
- 16. O'Keefe EA, Talley NJ, Tangalos EG, Zinsmeister AR. A bowel symptom questionnaire for the elderly. J Gerontol 1992; 47: M116-M121.
- 17. Kalantar JS, Talley NJ. The effects of lottery incentive and length of questionnaire on health survey response rates: a randomized study. J Clin Epidemiol 1999; 52: 1117-1122.
- 18. Kok AL, Voorhorst FJ, Burger CW, et al. Urinary and faecal incontinence in community-residing elderly women. Age Ageing 1992; 21: 211-215.
- 19. Nakanishi N, Tatara K, Nakajima K, et al. Urinary and fecal incontinence in a community-residing elderly population: prevalence, correlates and prognosis [in Japanese]. Nippon Koshu Eisei Zasshi — Jap J Public Health 1997; 44: 192-200.
- 20. Campbell AJ, Reinken J, McCosh L. Incontinence in the elderly: prevalence and prognosis. Age Ageing 1985; 14: 65-70.
- 21. Madoff RD, Williams J, Caushaj P. Fecal incontinence. N Engl J Med 1992; 326: 1002-1007.
- 22. Small K, Wynne J. Evaluating the pelvic floor in obstetric patients. Aust N Z J Obstet Gynaecol 1994; 1: 236-243.
- 23. Drossman DA. What can be done to control incontinence associated with the irritable bowel syndrome? Am J Gastroenterol 1989; 84: 355-357.
- 24. Jorge JM, Wexner SD. Etiology and management of fecal incontinence. Dis Colon Rectum 1993; 36: 77-97.
- 25. Kamm MA. Faecal incontinence. BMJ 1998; 316: 528-532.
- 26. Wald A. Fecal incontinence: three steps to successful management. Geriatrics 1997; 52: 49-52.
- 27. Read NW, Celik AF, Katsinelos P. Constipation and incontinence in the elderly. J Clin Gastroenterol 1995; 20: 61-70.
- 28. Bassotti G, Whitehead WE. Biofeedback as a treatment approach to gastrointestinal tract disorders. Am J Gastroenterol 1994; 89: 158-164.





Abstract
Objective: To determine the prevalence of faecal incontinence in the community and evaluate identifiable risk factors.
Design and setting: Cross-sectional survey using a validated questionnaire. A short version of the questionnaire was sent to 220 subjects and a long version to 770 subjects, randomly selected from western Sydney, Australia.
Main outcome measures: Self-reported faecal incontinence, defined as involuntary loss of anal sphincteric control leading to unwanted release of liquid or solid faeces (not flatus) at an inappropriate time or in an inappropriate place, within the past 12 months. The long questionnaire also sought information on bowel habit and potential risk factors for faecal incontinence.
Results: The response rate was 66%. The prevalence of solid or liquid faecal incontinence was 2% and 9%, respectively. The mean age of subjects with faecal incontinence was 53 years; 55% were women. After adjusting for age and sex, there was a significant association between faecal incontinence and perianal injury (P = 0.03), perianal surgery (P < 0.001), feelings of incomplete defecation (P < 0.0001), loose or watery motions (P < 0.0001) and urgency (P < 0.0001). Seven of 48 subjects with faecal incontinence reported being asked by their physician about faecal incontinence and nine of 33 reported seeking medical advice for their incontinence. Subjects with faecal incontinence perceived their health to be significantly poorer than did other subjects (P = 0.02).
Conclusion: There is a high burden of faecal incontinence in the community, and the prevalence in men may be greater than is usually appreciated. Despite significant associated morbidity, most cases of faecal incontinence were unrecognised by doctors.