Raina K Plowright As a veterinarian working on an Adélie penguin research program, I was to spend six months on an island off the coast of Mawson Station in the
Australian Antarctic Territory. During a field training exercise on
my third day at Mawson, I fell into a crevasse with my four-wheel-drive
quad bike and was crushed between the bike and the crevasse wall six
metres below the rim. I had hypothermia and abdominal injuries, and
underwent two emergency surgical procedures at Mawson Station.
Sixteen days after the accident, I was evacuated by helicopter and
ship. Here, I describe my experiences.
At that moment death seemed violently and terrifyingly close. The
enormous weight of the bike was squeezing the life from me and I thought
that I had only minutes to live. I knew something was very wrong where
the bike was crushing my abdomen. Warm urine dribbled down my freezer
suit and I could no longer feel my legs. The possibilities that crossed
my mind included spinal injury and paraplegia, but I was unafraid, as a
chance of life as a paraplegic was preferable to dying.
I recall lying in a stretcher. Madeleine Wilcock, the station doctor,
was peering down at me and asking what day it was, an oxygen mask was
placed over my face and I was breathing rapidly, gulping for air, and I
remember thinking, "I'm breathing! I'm breathing!". The stretcher
was lifted onto the back of a utility, which started bumping over the
ice, while I stared at the blue sky thinking, "I'm still breathing, I'm
alive".
When Bryan Walpole walked in, with his cheerful hello, the relief of
his familiarity was so overwhelming that Madeleine noticed a drop in
my highly elevated pulse rate. Bryan had been the ship's doctor on my
voyage to Antarctica on the Aurora Australis. The ship was
still within helicopter range, and Bryan had been rushed 140 nautical
miles over the sea ice to Mawson. It was extremely important to me, and
for my morale, to see someone familiar taking control over a situation
in which I had none.
It was a lonely and daunting experience being wheeled into an empty,
sterile room under bright surgical lights. At least the lights
indicated that they had an operating theatre. My anaesthetist, his
beard covered in a mask, sat at the head of my bed. I had met him just two
days previously; he was an electronics engineer with only two weeks
training in anaesthetics at The Royal Hobart hospital 12 months
earlier. My nurses were a carpenter and a diesel mechanic. I recall
being terrified -- too sick and narcotised to interact or understand;
the situation was completely out of my control.
I remember someone explaining that the anaesthetic was being
injected and a mist washed over me and I couldn't see or breathe. I could
hear instruments being dropped onto metal trays and people talking
around me, but I felt unable to breathe. My neck had been cranked to one
side and the discomfort was excruciating. Then something was placed
down my throat, and the air that I was desperately craving flowed into
my lungs. I needed another breath and I strained to inhale, but my body
wouldn't respond. I realised that I was paralysed and experiencing
anaesthetic awareness and the doctors were about to operate while I
was still conscious. I started screaming and screaming but I couldn't
open my mouth to make a sound. With the most enormous effort I tried to
move my arms and open my eyes to show them that I was fully conscious, but
nothing I did made me move.
However, I must have lost consciousness, as I felt no pain during the
surgery, and my next memory was of regaining consciousness on a wave of
nausea. Someone was holding a bowl to my mouth, and as I vomited I felt a
sensation like sutures ripping through the tissues in my abdomen. The
surgery was over and I was wheeled back into my hospital room.
During exploratory laparotomy, they found a mesenteric tear with
some bleeding vessels, which were ligated, and a large
retroperitoneal haematoma, about which they could do nothing. There
were also crushing injuries to my small intestine.
During long sleepless nights in the care of the nurses my veterinary
skills were often useful, in ways such as guiding them in fixing
blocked intravenous lines or giving injections. At first I was
nervous about a diesel mechanic or a carpenter trying to give me
intramuscular injections, but then I noticed that they were even more
terrified than I. I learned how stressful it is having to endure and
anticipate multiple painful procedures each day, and would have
preferred all dressing changes, catheter changes, injections and
other painful events to be finished in one go. I appreciated
Madeleine's efforts to relieve my pain, such as administering local
anaesthetic before inserting a cannula. I decided that I would take
great care to avoid inflicting pain on my patients in the future.
On returning to Australia, I spent two weeks at a rehabilitation
hospital in Melbourne undergoing intensive physiotherapy for right
lumbar plexopathy. Two months after the accident I underwent an
incisional hernia repair and bowel resection because of adhesions. I
have been fortunate and grateful to make a complete recovery.
Madeleine Wilcock and my nurses, Garry Watson, Jason Reinke and Nick
Mortimer, were awarded the Australian Antarctic Medal for their
extraordinary efforts while I was under their care. I would like, once
again, to express my deep gratitude for their dedicated, skilful and
untiring efforts to nurse and restore me. I will always remember my
journey to Antarctica by the aura of love and compassion and care that
contained me during those critical days of recovery from the crevasse
fall.
Reprints will not be available from the author.
The Antarctic plateau is a crevasse-riven mass of ice rising steeply
behind Mawson Station. While riding across sastrugi (ridges in the
ice formed by frozen accumulations of blown snow) on the plateau, I
slowed to avoid skidding on a snowdrift that was barely visible in the
glare. The front wheels of my quad bike reached the other side of the
drift, but spun on blue ice. There was a deafening sound, like
shattering glass, then ice and metal rushed past me as I plummeted down
the walls of the crevasse and was crushed into the ice by the oppressive
weight of metal. When everything stopped, I opened my eyes and found I
couldn't breathe. I was wedged vertically in a narrow part of the
crevasse, pinned between the bike and the ice wall 30 metres from the
bottom. The 250 kg bike was crushing my abdomen and thorax against the
ice, my chest flattened by the seat, the petrol tank against my lower
body.

Four-wheel-drive quad bikes being driven across sea ice. (Photograph courtesy of Kym Newbery)

Westbay and the area where I fell into the crevasse: a view from Mawson Station. (Photograph courtesy of Kym Newbery)
Rescue
By the time rescuers descended into the crevasse 90 minutes after my
fall, I thought that I couldn't manage the extraordinary effort of
moving air into my lungs any longer. As the bike was lifted off me I was
crushed back into the ice and a white curtain of unconsciousness
descended. It took six people over 15 minutes to haul me out of the
crevasse using a "Z"-pulley rigged with ropes secured to an oversnow
vehicle.
Triage
I have vague memories of painful needles being pushed into my arms and
abdomen, uncontrollable shaking from the ice at my core and nausea
that suddenly swept over me causing me to vomit a liquid like coffee
grounds. I knew this was altered blood, but my mind refused to make the
next logical step and question why I would be vomiting digested blood.
There was a frantic effort to find Jason the electrician, as he was the
only one of the 44 expeditioners on station who shared my Rh negative
blood type.
"We have to operate"
The next morning Bryan announced that they had to operate. The thought
of postoperative pain on top of discomfort and nausea I could already
barely tolerate was devastating. I didn't even know if the station had
surgical facilities, or if Madeleine or Bryan had surgical
experience. It did not occur to me to ask them why I needed surgery.
However, my haemoglobin level had fallen from 140 g/L to 100 g/L
overnight, my pulse rate was rising, and I had developed abdominal
pain. The only diagnostic tools available were haematological and
biochemical tests, and x-rays. Thus, it was necessary to open me up to
see if there was continued bleeding. There was also concern that I may
have had a perforated gut, as I had been vomiting altered blood.
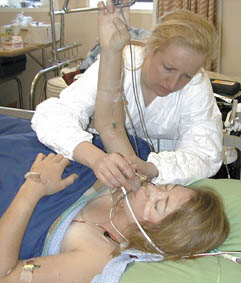
Dr Madeleine Wilcock putting an oxygen mask on me immediately after the first operation. (Photograph courtesy of Jason Reinke)
My care team
The next seven days were a blur of unbearable suffering, surrounded by
the extraordinary compassion and dedication of Madeleine Wilcock,
my doctor (Bryan was required to return to the ship), who understood my
suffering as if she were going through it too. This was complemented by
the diligence and kindness of my three dedicated (bearded) nurses,
who were there 24 hours a day and would do anything for me. Their
combined love and concern enveloped and helped me during those awful
days.
No visitors
Madeleine understood that I was unable to cope with visitors and
allowed only Lyn (my biologist colleague, and one of only two other
women on the station) to visit every day to read emails, which were
important for maintaining my morale. I appreciated Madeleine's
sensitivity, as I found interaction with people almost unbearable.
Moving, and especially speaking, caused the nasogastric tube to
irritate my pharynx and induced gagging and vomiting. I was anxious
for people to leave. If they remained for any length of time, I needed
their reassurance that they didn't expect me to answer or to look at
them. I needed them to acknowledge and empathise with my suffering,
the awful nausea, and the pain that vomiting caused me, as well as the
exhaustion from lack of sleep, and the demoralising affliction of the
nasogastric tube.
No medical details, please
Uncharacteristically, despite my usual curiosity and medical
background, I had no interest in my medical details. I was unable to
process any information. My entire focus was on existing. Until I was
well again I didn't ask what the outcomes of the surgery were. I could
not think about the accident, full stop. Flashbacks were immediately
pushed out of my mind, and it wasn't until the nausea had subsided and
the nasogastric tube had been removed that I was ready to face the full
psychological trauma of the accident.
My past veterinary patients
As I lay in the white hospital room, watching the opaque grey world of a
passing blizzard through my tiny porthole, I remember thinking, "My
God, this is what sick people feel like". This new insight into
suffering was particularly harrowing when I related it to all of those
animals which had sat in the back of their cages, unmoving and
unresponsive: I now understood what they may have been experiencing.
I was certain that I would never work as a veterinarian again; I never
wanted to face anything -- human or animal -- that felt as sick and
uncomfortable as I did then.
A slow recovery
Traumatic pancreatitis -- diagnosed during further surgery after my
return to Melbourne -- and recurrent forceful vomiting contributed
to delayed wound healing. Eleven days after my operation my wound
completely dehisced, and the next day I underwent further surgery for
abdominal wall repair at Mawson Station. The Aurora
Australis was turned around from its position in the Southern
Ocean to bring me home. This was a major disappointment, as I was so much
looking forward to recovering among the people who had cared for me and
to continuing working on the island with the penguins. However, as
well as the risk of further complications, supplies of drugs,
cannulas, and fluid administration kits were running very low.
Moreover, there was no total parenteral nutrition and my body had
wasted away. Six days after the second operation I was 12-13 kg lighter
than before my accident.

The Aurora Australis, which turned back to bring me home (Adélie penguins in the foreground). (Photograph courtesy of Kym Newbery)
Authors' details
Wentworth Falls, NSW.
Raina K Plowright, BVSc(Hons), Veterinary Surgeon.
Correspondence: Ms R K
Plowright, PO Box 241, Wentworth Falls, NSW 2782.
rainapATozemail.com.au
Connect
Advertisement
Crevasse fall in the Antarctic: a patient's perspective
Med J Aust 2000; 173 (11)
Published online: 4 December 2000
Published online: 4 December 2000
The full article is accessible to AMA
Correspondence:
Online responses are no longer available. Please refer to our instructions for authors page for more information.
Advertisement




