|
Research
Outcomes after hip or knee replacement surgery for osteoarthritis
A prospective cohort study comparing patients' quality of life
before and after surgery with age-related population norms
Lyn M March, Marita J Cross, Helen Lapsley, Alan J M
Brnabic
Katherine L Tribe, Clarissa J M Bachmeier, Brett G Courtenay
and Peter M Brooks*
MJA 1999; 171: 235-238
For editorial comment, see Williamson
Abstract -
Introduction -
Methods -
Results -
Discussion -
Acknowledgements -
References -
Authors' details
-
-
More articles on Orthopaedic surgery
|
Abstract |
Objective: To compare the health-related quality of
life of people with osteoarthritis before and after primary total hip
and knee replacement surgery with that of the general Australian
population.
Design: A prospective cohort study.
Setting: Three Sydney hospitals, public
and private.
Participants: Patients with osteoarthritis
undergoing primary total hip (n = 59) and knee (n = 92)
joint replacement surgery.
Main outcome measure: Medical Outcomes Study Short
Form (SF-36) scores before and 12 months after joint replacement
surgery (compared with population norms).
Results: Patients in each age group showed a
significant improvement in health-related quality of life after
joint replacement surgery in most scales of the SF-36, particularly
physical function, role physical and bodily pain. SF-36 scores for
the 42 hip-replacement patients aged 55-74 years improved to equal or
exceed the population norm on all scales. SF-36 scores of the 52 knee
replacement patients aged 55-74 years improved, but physical
function and bodily pain scores remained significantly worse than
the population norm. SF-36 scores for both hip (n = 17) and knee
(n = 40) replacement patients aged 75 years and over improved
significantly, becoming similar to population norms for this age
group.
Conclusions: Total hip or knee replacement for
osteoarthritis significantly improves patient health and
well-being at 12 months after surgery. Age alone should not be a
barrier to surgery.
|
| | Introduction |
Osteoarthritis is one of the leading causes of pain and disability in
the Australian population.1,2 Total joint replacement
is the most common treatment for advanced osteoarthritis of the hip or
knee, with the primary goal of the procedure being to improve the
patient's quality of life.3 In Australia, in the financial year 1997/98, Medicare benefits of
$13 500 000 were paid for 17 000 hip
and knee replacements. This number represents only some of the total
surgery performed, as the number of operations on Veterans' Affairs
patients and on public patients in public hospitals are not
available. Despite joint replacement surgery being one of the most
common operations performed in this country, very limited
Australian outcomes data have been published.4
The Medical Outcomes Study Short-Form 36 (SF-36) has been used
extensively to assess the effect on quality of life of several
procedures, including total joint replacement,5,6 and it has been
suggested that it should be the focus of preoperative and
postoperative outcome evaluation for total hip
arthroplasty.7 As a generic measure of
health-related quality of life with standardised scoring, it
enables comparisons between diseases, treatments and published
population norms. It measures health on eight 100-point scales:
physical function, role physical (ie, role limitations due to
physical problems), bodily pain, general health, vitality, social
function, role emotional (ie, role limitations due to emotional
problems), and mental health. It is one of the most widely used
health-related quality-of-life instruments and has been shown to be
reliable and valid.
Studies in the US have shown that the SF-36 detects a
significant improvement in health-related quality of life in
patients undergoing total hip or knee replacement when preoperative
scores are compared with postoperative scores.8-11 The SF-36
also demonstrates a difference in outcome between total hip and total
knee replacement patients,8,10 with patients
undergoing total hip replacement achieving significantly better
outcomes than the knee replacement patients.
We aimed to compare the health-related quality of life (as measured by
the SF-36) of people with osteoarthritis undergoing primary total
hip and knee replacement surgery with that of the normal Australian
population.2 Putting changes in the
health-related quality of life of these patients in the context of
population norms for the same age group gives us a meaningful measure
of the effectiveness of this surgery. It also provides information in
a way that allows comparisons with other diseases and treatments,
assisting rational choices to be made about the use of the limited
healthcare dollar.
|
| |
Methods |
The information on the patients undergoing total joint replacement
collected for this analysis was part of a long-term follow-up of
patients in a cohort study aiming to assess the costs of arthritis and
the effectiveness of its treatment. The cohort includes patients
from both public and private hospitals and surgeons operating in both
sectors are involved.
Patients with osteoarthritis booked for primary total hip or knee
replacement surgery at three Sydney hospitals (St Vincent's public
and private hospitals and the Centre for Bone and Joint Diseases,
North Ryde) between March 1994 and December 1995 were approached to
participate in the study. Recruitment was through regular
contact with the orthopaedic surgeons and their practice staff.
Baseline information was collected from patients through a series of
questionnaires, including the SF-36. Questionnaires were
administered between one week and three months before surgery. After
surgery, patients completed the SF-36 questionnaire at the end of
each three months for their first postoperative year. Most
questionnaires were self-administered, with less than 10%
requiring face-to-face interview. This is consistent with the
Australian Bureau of Statistics methodology for collecting general
population data.2 Annual follow-up of these
patients by mail is continuing.
This article presents SF-36 information from patients at baseline
and 12 months after surgery.
Ethics committee and Medical Board approval was obtained from the St
Vincent's campus of the University of New South Wales Medical School,
the Centre for Bone and Joint Diseases and the Royal North Shore
Hospital. All patients in the study gave written informed consent.
| |
Analysis |
Mean scores for each of the SF-36 dimensions were calculated for
patients in the age groups 55-64, 65-74 and 75 years and over. Scores
for men and women were combined, as, apart from older males undergoing
joint replacement having lower preoperative scores for role
emotional, there was no significant difference in scores between the
sexes. Scores for each dimension were transformed according to the
SF-36 user's guide12 to a scale of 0-100 (100 =
best possible score).
We used one-sample t tests to compare the transformed scores
with general population norms derived by the Australian Bureau of
Statistics from the 1995 National Health Survey. The t test
was chosen on the assumption that the population value was the real
value (given that published standard errors were so low) and that we
were observing the variance of the study data from the population
value.
A P value of 0.05 was considered to be significant and no
adjustment was made for multiple comparisons.
| | | SF-36 on the web
More information about the SF-36 health survey can be found on the SF-36 website:
http://www.sf-36.com
An online demonstration of the SF-36 survey (score yourself and read an explanation of the result in comparison with US population norms) is available at:
http://www.qmetric.com/demo/sf-36v1.shtml
|
|
| |
Results |
Two-thirds of the eligible patients were recruited (226 of 343).
Reasons for exclusion included being unable to be contacted before
surgery (50% of those who did not participate in the study), being
non-English-speaking (10%) and refusal or inability to complete the
questionnaires (40%). Eligible patients who did not participate in
the study did not differ significantly from the cohort in terms of age,
sex or type of joint replacement (ie, hip or knee) (data not shown).
At the time of analysis, we had complete information for 151 patients
at 12 months' follow-up (59 with hip replacement and 92 knee
replacement; 52% female; median age, 72 years). An additional 75
patients (60% female; median age, 74 years) had incomplete follow-up
information. Their last recorded SF-36 scores showed no significant
differences from scores at the same stage of follow-up among those
with complete information (data not shown).
Patients' SF-36 scores before and 12 months after surgery are shown in
the Figure, in comparison with scores for the general population.
| |
Knee replacements | |
55-64 years age group: Eight patients undergoing
knee replacement were recruited. Six of these patients reported
having other illnesses, most commonly cardiovascular disease
(reported by five patients).
At 12 months' follow-up, these eight patients showed improvement
from baseline according to mean SF-36 scores for physical function,
role physical, bodily pain and vitality, but these scores remained
significantly lower than the population norms. The power to detect
the observed difference to be statistically significant at the 5%
level ranged from 83% to 100% for these four comparisons. Their scores
on the other four scales (general health, social function, role
emotional, mental health) remained lower than population norms, but
this difference was not statistically significant (power to detect a
significant difference ranged from 7% to 55%).
65-74 years age group: Twenty-eight of the 44
patients (64%) reported having a comorbid illness, with the most
commonly reported again being cardiovascular disease (61% of those
with comorbidity).
Mean SF-36 scores improved significantly on all scales except
general health. The mean general health score was significantly
higher than the population norm at 12 months' follow-up, but had been
higher to begin with at baseline. Mean physical function, role
physical and bodily pain scores remained significantly lower than
the population norms at 12 months' follow-up. The power to detect
these differences ranged from 85% to 99%. Mean vitality, social
function, role emotional and mental health scores improved from
baseline to be similar to population norms. The power to detect the
significance of these differences ranged from 8% to 36%.
75 years and over: Thirty-two of the 40 patients (80%)
reported suffering from another illness, most commonly
cardiovascular disease (60% of those with comorbidities).
Mean SF-36 scores improved significantly on most scales
(particularly role physical, physical function and bodily pain),
but not on general health and mental health, which were fairly high
before surgery. The mean general health score was significantly
higher than the population norm at 12 months' follow-up; the other
scores improved to population levels. Given the small difference
seen between patient and population scores, large numbers would be
required to show statistically significant differences (power
ranged from 7% to 33%).
| |
Hip replacements | |
55-64 years age group: Comorbidities were reported
by 5 of the 14 patients (36%). All five had cardiovascular disease
among other comorbidities.
Mean scores for vitality and social function improved to become
significantly higher than the population norms (power to detect
significant difference, 90% and 96%, respectively), while the other
scores improved to be similar to the population norms, with
particular improvement in physical function, role physical and
bodily pain.
65-74 years age group: Thirteen of the 28 patients
reported suffering from a comorbid illness, most commonly
cardiovascular disease (46% of patients with comorbidities).
Mean SF-36 scores improved on all scales except general health, which
had a baseline value above the population norm. Mean scores for
general health and mental health were significantly higher than the
population norms at 12 months' follow-up (power to detect
difference, 85% and 75%, respectively) and the other scores improved
to be similar to the population norms (power to detect difference
ranged from 7% to 58%). The improvement from baseline was
particularly evident in role physical, physical function and bodily
pain scores.
75 years and over: Comorbidities were reported by 12
of the 17 patients (71%), most commonly cardiovascular disease
(reported by 58% of those with comorbidities).
Mean SF-36 scores improved on all scales except general health and
mental health. At 12 months' follow-up, mean scores on none of the
scales were significantly different from the population norms,
possibly due to the small numbers in this group (power to detect a
difference less than 30% for most scales). Again, there was
improvement to population norms in role physical, physical function
and bodily pain.
|
| |
Discussion |
We found that knee or hip replacement surgery significantly improved
the health-related quality of life of patients with osteoarthritis.
Before surgery, the patients had poor SF-36 scores for bodily pain,
physical function and role physical, a clear reflection of the impact
of chronic osteoarthritis on health-related quality of life. After
surgery, the biggest improvements were in these scores. Improvement
in these physical dimensions of health is likely to lead to
improvements in social function, mental health and vitality.
We found no improvement in general health despite gains in the other
scales. This has been shown in other studies,11 and has been suggested to
be due to the patients' previous medical history and pre-existing and
general health-related conditions. In our study it was apparent that
the general health of patients was already higher at baseline than the
population norm, suggesting that relatively healthy patients are
being selected for total joint replacement.
A US study that compared patients undergoing total hip replacement
with age-matched and sex-matched population norms found that age and
sex made important differences in SF-36 scores.9 Men younger than
65 years had scores lower than the norms in the physical scales, but
were comparable in the mental scales, and women scored lower than the
norm in all scales. No sex differences were found in our study, but
similar age differences were observed, particularly for patients
undergoing total knee replacement, among whom the youngest age group
had the poorest outcome relative to the age-matched population. We
hypothesise that this may be related to the higher population norms
for this age group, unrealistic expectations for outcomes among
patients, and the presence of existing comorbidities in younger
patients requiring knee replacement. One implication of these
findings is that older age should not be a barrier to joint replacement
surgery, as the outcome is likely to be relatively successful for
older patients.
Potential limitations that need to be considered when interpreting
these results include the non-randomised cohort design, the power of
the analysis given the small sample size of the subgroups, and the
overall response rate. However, the inclusion of several groups of
surgeons operating at different sites and across the public and
private sectors contributed significantly to the generalisability
of the results.
This study showed the improvement of SF-36 scores of patients
undergoing total hip or knee replacement up to and in some cases beyond
population norms. Whether these statistically significant
differences are clinically important remains to be seen. Longer
follow-up is required to determine whether the dramatic improvement
from baseline is maintained. Nonetheless, at one year follow-up, it
would appear that total knee or hip joint replacements are successful
at restoring health and well-being, and that older age alone should
not be a barrier to surgery.
|
Acknowledgements | |
This study was funded by grants from the National Health and Medical
Research Council. We are grateful to the secretarial staff of the
orthopaedic surgeons for their assistance with recruitment to this
study and to the patients who have been so cooperative.
|
| |
References |
- Australian Bureau of Statistics. Disability and handicap,
Australia 1988. Canberra: ABS, 1996 (Catalogue No. 4120.0).
-
Australian Bureau of Statistics National Health Survey: SF-36
population norms, Australia, 1995. Canberra: ABS, 1997 (Catalogue
No. 4399.0).
-
Bombardier C, Melfi CA, Paul J, et al. Comparison of a generic and a
disease-specific measure of pain and physical function after knee
replacement surgery. Med Care 1995; 33 Suppl 4: AS131-AS144.
-
Van Essen GJ, Chipchase LS, O'Connor D, Krishnan J. Primary total
knee replacement: short-term outcomes in an Australian population.
J Quality Clin Practice 1998; 18: 135-142.
-
Bayley KB, London MR, Grunkemeier GL, Lansky DJ, Measuring the
success of treatment in patient terms. Med Care 1995; 33 Suppl
4: AS226-AS235.
-
Stucki G, Liang MH, Phillips C, Katz JN. The Short-Form 36 is
preferable to the SIP as a generic health status measure in patients
undergoing elective total hip arthroplasty. Arthritis Care
Res 1995; 8: 174-181.
-
Ritter MA, Albohm MJ, Overview: maintaining outcomes for total hip
arthroplasty. The past, present and future. Clin Orthop
1997; 344: 81-87.
-
Hozack J, Rothman RH, Albert TJ, et al. Relationship of total hip
arthroplasty outcomes to other orthopaedic procedures.
Clinical Orthop 1997; 344: 88-93.
-
Lieberman JR, Dorey F, Shekelle P, et al. Outcome after total hip
arthroplasty. Comparison of a traditional disease-specific and a
quality of life measurement of outcome. J Arthroplasty 1997;
12: 639-645.
-
Kiebzak GM, Vain PA, Gregory AM, et al. SF-36 general health status
survey to determine patient satisfaction at short-term follow-up
after total hip and knee arthroplasty. J Southern Orthop
Assoc 1997; 6: 169-172.
-
Ritter MA, Albohm MJ, Keating EM, et al. Comparative outcomes of
total joint arthroplasty. J Arthroplasty 1995; 10: 737-741.
-
Medical Outcomes Trust. How to score the SF-36 health survey.
Boston: The Trust, 1994.
(Received 16 Oct 1998, accepted 12 Jun 1999)
|
| | Authors' details |
University of Sydney, Department of Rheumatology, Royal North Shore
Hospital, Sydney, NSW.
Lyn M March, MB BS, PhD, FRACP, FAFPHM, Associate Professor.
Department of Medicine, University of New South Wales, Sydney, NSW.
Marita J Cross, BSc(Hons), Research Assistant;
Katherine L Tribe, BSc(Hons), Research Assistant;
Clarissa J M Bachmeier, MD, MMed(ClinEpidem), Research
Fellow.
School of Health Services Management, University of New South Wales.
Helen Lapsley, BA, MEc, Senior Lecturer.
Northern Sydney Public Health Unit, Hornsby Ku-ring-gai Hospital,
Sydney, NSW.
Alan J M Brnabic, MSc, Statistician.
Department of Orthopaedics, St Vincent's Hospital, Sydney, NSW.
Brett G Courtenay, MB BS, FRACS, Orthopaedic Surgeon.
Faculty of Health Sciences, University of Queensland, Brisbane,
Qld.
Peter M Brooks, MB BS, FRACP, FAFPHM, Executive Dean.
No reprints will be available from the authors.
Correspondence:
Associate Professor L M March, Department of Rheumatology, Royal
North Shore Hospital, St Leonards, NSW 2065.
Email: lmarcATdoh.health.nsw.gov.au
|
| | 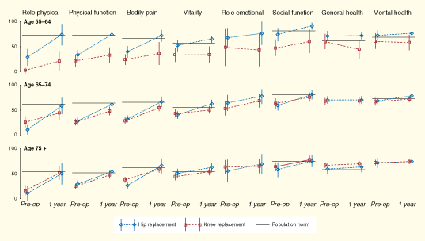 Click in figure for a larger version | | Back to text |
|





