Abstract
Objective: To ascertain the effectiveness of
clinical pathways for improving patient outcomes and decreasing
lengths of stay after hip and knee arthroplasty.
Design and setting: Twelve-month randomised
prospective trial comparing patients treated through a clinical
pathway with those treated by an established standard of care at a
single tertiary referral university hospital.
Participants: 163 patients (56 men and 107 women;
mean age, 66 years) undergoing primary hip or knee arthroplasty, and
randomly allocated to the clinical pathway (92 patients) and the
control group (71 patients).
Main outcome measures: Time to sitting out of bed and
walking; rates of complications and readmissions; match to planned
discharge destination; and length of hospital stay.
Results: Clinical pathway patients had a shorter
mean length of stay (P = 0.011), earlier ambulation(P
= 0.001), a lower readmission rate (P = 0.06) and closer
matching of discharge destination. There were beneficial effects of
attending patient seminars and preadmission clinics for both
pathway and control patients.
Conclusion: Clinical pathway is an effective method
of improving patient outcomes and decreasing length of stay
following hip and knee arthroplasty.
Introduction
The past two decades have seen an 85% rise in Australian health costs to 36.6 billion dollars, with the largest proportion of this expended in acute hospital care.1 Newer health policies now incorporate measures to rationalise and improve the efficiency of many services. Such policies, however, are economically driven and frequently fail to consider the optimum level of service required by the community.2
Treatment protocols, variously known as clinical pathways, critical pathways and care paths, that aim to streamline and standardise management through a systematic approach so that high quality care may be provided in a timely and cost effective manner3,4 have been developed. Clinical pathways describe the course of hospitalisation for patients with a specified illness and encompass a predetermined plan of treatment.
The use of clinical pathways is now well established and their successes are widely reported.5-7 Joint arthroplasty is a common and costly procedure associated with high resource use that is frequently performed in the elderly who may have many coexisting morbidities. These characteristics suggest that joint arthroplasty may be a suitable procedure to incorporate into a clinical pathway.8
As part of a "best practice" initiative in line with quality assurance activities at St Vincent's Hospital, the hospital's Orthopaedic Service has developed clinical pathways for hip and knee joint arthroplasty for treating osteoarthritis which aim to maximise the use of all available resources and minimise negative patient outcomes, thereby improving patient care.
To this end, we report the effects of introducing clinical pathways at our hospital on quality indicators such as mobilisation, complication rates, discharge planning and readmission rates while also exploring the impact on length of stay.
Methods
We used a prospective randomised control group design to compare the outcomes of patients who underwent hip or knee joint arthroplasty at St Vincent's Hospital, Melbourne (a tertiary referral hospital affiliated with the University of Melbourne), between 1 January 1996 and 30 December 1997. All such patients were randomly allocated to either the control or clinical pathway group by a clerical assistant who was blinded to their demographic and clinical profiles. Diagnostic category and comorbidities had no bearing on the allocation of patients to either the pathway or control groups, but patients were excluded from the study after randomisation if they were having revision arthroplasty, simultaneous bilateral joint arthroplasty, arthroplasty for acute trauma or complex tumour surgery. The management of patients undergoing joint arthroplasty at St Vincent's Hospital, Melbourne, is outlined in Box 1.Outcome measures
- Length of stay (calculated from the time of the patient's admission
to the time of discharge and expressed in days);
- Time to sitting out of bed and ambulation (time between surgery and
the patient's first day of sitting out of bed or walking with
assistance);
- Complications (wound infections, including all wound erythema
lasting more than 24 hours, chest infections, deep vein thrombosis
[DVT] as diagnosed by clinical features and confirmed by
ultrasonography, joint dislocation, decubitus pressure areas,
failure to cope at home and a decreased range of motion after
discharge);
- Readmission (for complications during a follow-up period of three
months from discharge); and
- Discharge matching (between the presumptive discharge destination given at the preadmission clinic and the patient's postdischarge destination).
Clinical pathway and control patients
Patients randomly allocated to the clinical pathway received proactive treatment whereby specific goals were set each day for the patient and treating team. Their hospital records included a special written protocol which listed milestones to be achieved, identified tests that should be ordered, set daily tasks for patients and members of the treating team, and provided space for documenting any variation in treatment or patient response. Each intervention was signed by the treating health professional and the discharge plan was re-evaluated daily to ensure it remained realistic and appropriate to the patient's needs. The clinical pathway formalised in writing the participation of the various members of the treating team.Patients not allocated to the pathway received "reactive" treatment whereby the treating team responded to the will and condition of the patient in providing postoperative care.
Statistical analysis
Results were analysed with SigmaStat V2 software.9 Data were compared using t tests for independent groups and multiple linear regression where appropriate. We used the z test for comparisons of proportions between groups. As the data for length of stay (LOS), time to sitting out of bed and time to ambulation were not normally distributed, these data were transformed using a logarithmic transformation before analysis with t tests.We calculated the sample size for this study after reviewing all hip and knee arthroplasty patient data for 1995, which showed a mean LOS of 13 days (range, 5.8-43.3; SD, 5.3). We believed that a 20% reduction in LOS (2.6 days) would represent a clinically significant outcome. Therefore, we calculated that to detect a reduction of 2.6 days in LOS at a significance level of 0.05 with a power of 0.8 would require two groups with a minimum of 65 subjects in each group.
Results
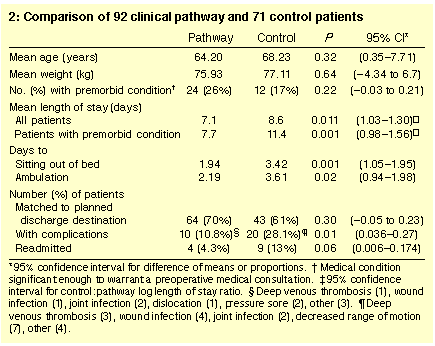
During the study period 175 patients underwent hip or knee joint arthroplasty and were randomly allocated to the pathway (94 patients) and control (81 patients) groups. Twelve patients were then excluded by the crtiteria listed in the methods, leaving 163 patients -- 92 in the clinical pathway group and 71 in the control group. The sample comprised 56 men and 107 women, with a mean age of 66 years (range, 67-93 years). All patients were followed for a minimum of three months and none were lost to follow-up.Our findings are summarised in Box 2. There was no significant difference between control and pathway patients in terms of age or weight. Although the clinical pathway group included more patients with premorbid conditions than the control group, this difference was not statistically significant (95% CI, - 0.03 to 0.21). Length of stay (LOS) was significantly shorter for the pathway group than for the control group (t = 2.585; P = 0.011). When LOS was analysed for the subgroups of patients in each group with premorbid conditions, this was still significantly shorter for the pathway group than the control group (t = 3.152; P = 0.001) despite the larger number of patients with premorbid conditions in the pathway group.
Patients in the clinical pathway group sat out of bed and walked earlier after surgery than control patients. Multiple linear regression for each group showed that time to ambulation was the only significant contributor to reduction in log LOS in the clinical pathway group (time to ambulation -- coeff = 19.6, standard error [SE] = 9.6, P = 0.04; time to sitting out of bed -- coeff = - 4.35, SE = 9.3, P = 0.64, R2 = 0.127). Neither time to ambulation nor time to sit out of bed was significantly associated with reduced log LOS in the control group (time to ambulation -- coeff = 21.05; SE = 26.28, P = 0.42; time to sit out of bed -- coeff = - 4.13, SE = 28.54, P = 0.88, R2 = 0.0251).
Patients from both the clinical pathway and control groups who attended either the preadmission clinic (n = 122) or the patient information seminar (n = 61) had a shorter LOS (7.22 days and 6.84 days, respectively) than patients who attended neither (n = 36; LOS, 8.55 days). The 54 patients who attended both the clinic and seminar had the shortest LOS at 6.6 days, and t tests showed that the shorter LOS for these patients relative to those who attended neither the clinic nor seminar was significant (t = 2.66; P = 0.009). Post-hoc t tests showed that the shorter LOS for patients who had attended both preadmission clinics and information seminars relative to those who had attended neither was significant (t = 2.66; P = 0.009).
Box 2 shows that a greater proportion of clinical pathway patients were discharged to their planned discharge destination than control patients (95% CI, - 0.05 to 0.23), and that there were fewer readmissions in clinical pathway patients (95% CI, 0.006-0.174), although neither result was statistically significant. However, there were significantly fewer complications in clinical pathway patients (95% CI, 0.036-0.27).
Discussion
We found that a clinical pathway for hip and knee joint arthroplasty had a beneficial impact on the duration of admission, with patients on the pathway having a 1.5-day shorter stay than control patients. The seven-day LOS for our pathway patients compared favourably with that of Gregor et al,10 who showed a reduction in LOS from 12 to nine days for pathway patients.Length of stay was significantly shorter for the pathway group than the control group despite the larger proportion of pathway patients with premorbid conditions. This result should be interpreted cautiously, as the small overall number of patients with premorbid conditions meant that the test had less than optimal power (0.45). However, we conclude that comorbidities per se should not exclude patients from clinical pathways. Patients with comorbid conditions may actually be better served because of the greater fastidiousness and vigilance imposed by the daily protocol.
While our findings that there were fewer complications and readmissions in clinical pathway patients were not significant, we believe that given the appropriate number of subjects in future studies both of these areas may approach significance.
We noted that reducing the length of stay did not increase the complication rate, a finding corroborated by others.11 In addition, the readmission rate for complications for pathway patients was one-third that of controls. This contrasts with some studies which have reported an inverse relationship between length of stay and readmission rates.11 We, like other authors,12 believe that it is a lower quality of care and not length of stay per se that increases the risk of unplanned readmission.
Discharge planning is an important part of the clinical pathway which appears to be closely linked with the length of stay. Appropriate matching of predetermined discharge destinations is a correlate of shorter admissions. If we are able to improve on our destination matching rate of 70%, we may be able to further reduce our length of stay, thereby making more resources available for other patients.
Education of patients and their relatives appeared to have a positive influence on the patients' recovery after joint arthroplasty, with earlier mobilisation and discharge from hospital. Attending information seminars and preadmission clinics assisted in reducing the length of stay by almost two days. Patients and their relatives who understand the disease and the necessary treatment may be in a better position to assist with care and rehabilitation. Attendances for our information seminar and preadmission clinic were 38% and 74%, respectively, and we are endeavouring to increase these.
First introduced by the New England Medical Center, clinical pathways are now incorporated into the management philosophy of many hospitals worldwide.13,14 Pathways involve input from medical, nursing, paramedical and administrative staff, and reflect the expertise of all members of the healthcare team while highlighting the interdependent nature of these roles in achieving positive outcomes for patients.15
A valuable subsidiary purpose of pathways is in providing information from which the financial cost of care may also be derived.16 Accurate costing of treatment is fundamental to the operation of institutions where prospective payments are made in accordance with diagnosis-related groups (DRGs), standardised lengths of stay and fixed reimbursement for care. Clinical pathways thus provide an important tool for coordinating and managing clinical resources. However, the driving force behind clinical pathways must remain the need to improve the quality of care and patient outcomes, and not their utility as a tool to ensure that budgetary demands are met.
We are encouraged by our findings, which indicate substantial improvements for patients on a clinical pathway. To our knowledge, no other study has investigated the effect of clinical pathways on joint arthroplasty using a contemporaneous control group.
1 Management of joint arthroplasty patients at St Vincent's Hospital, Melbourne
Preadmission clinics
Preoperative review for patients undergoing elective joint replacement involves a multidisciplinary approach and includes medical, nursing, physiotherapy and occupational therapy consultation and anaesthetic and social work screening. Preexisting conditions are identified and testing and treatment are undertaken to achieve an optimum level of preoperative health. A discharge destination is determined based on medical and projected rehabilitation needs. Appropriate referrals are initiated.
Patient information seminars
Groups of patients and their families are invited to attend an information seminar about the surgery. The surgeon explains the aetiology of the disease, principles of management, nature of potential risks and their prevention. The nursing staff discuss acute postoperative care, including pain relief, pressure and wound care, intravenous therapy, and prophylaxis for deep venous thrombosis. The physiotherapist discusses the regimen of postoperative exercises, cautions and mobilisation. The occupational therapist describes the availability and use of various personal aids which assist the patient in preventing complications such as falls, injury or dislocation. Patients are able to raise any questions related to their surgery. Patients and their families
are encouraged to take an active role in the postoperative management, and are acquainted with their very important role in the postdischarge phase. All members of the team stress the philosophy that the primary intention is to return patients home in preference to a rehabilitation hospital after the surgery.
Discharge
Patients are discharged home or to a rehabilitation unit. For those discharged home, community nursing care is provided at regular intervals for the first three weeks after discharge. Community nurses pay special attention to the nature of the patient's wounds, their exercise regimen and general medical condition. Any concerns are immediately related to the medical staff for further attention. Patients are followed up on a regular basis in the outpatient department.
References
- MacIntyre CR, Brook CW, Chandraraj E, Plant AJ. Changes in bed resources and admission patterns in acute public hospitals in Victoria, 1987-95. Med J Aust 1997; 167: 186-189.
- Parry TG. Health expenditure in Australia -- the current dilemma. Med J Aust 1992; 156: 592-594.
- Wigfield A, Boon E. Critical care pathway development: the way forward. Br J Nursing 1996; 5: 732-735.
- Grudich G. The critical path system. AORN J 1991; 53: 705-714.
- Gouveia WA, Massaro FJ. Critical pathway experience at New England Medical Center. Am J Health-Syst Pharm 1995; 52: 1068-1070.
- Saltiel E. Critical pathway experience at Cedars-Sinai Medical Center. Am J Health-Syst Pharm 1995; 52: 1063-1068.
- Stevenson LL. Critical pathway experience at Saratosa Memorial Hospital. Am J Health-Syst Pharm 1995; 52: 1071-1073.
- Leininger SM. Tools for building a successful orthopaedic pathway. Orthop Nurs 1996; 15: 11-19.
- SigmaStat [computer program]. Version 2. San Rafael, CA: Jandel Scientific Software, 1995.
- Gregor C, Pope S, Werry D, Dodek P. Reduced length of stay and improved appropriateness of care with a clinical path for total knee or hip arthroplasty. Joint Commiss J Qual Improv 1996; 22: 617-628.
- Rushworth RL, Rob MI. Readmissions to hospital: the contribution of morbidity data to the evaluation of asthma management. Aust J Public Health 1995; 19: 363-367.
- Ashton CM, Kuykendall DH, Johnson ML, et al. The association between the quality of inpatient care and early readmission. Ann Intern Med 1995; 122: 415-421.
- Zander K. Managed care within acute care settings: design and implementation via nursing case management. Health Care Supervisor 1988; 6: 27-43.
- Bower KA. Managed care: controlling costs, guaranteeing outcomes. Definition 1988; 3: 14.
- Heacock D, Brobst RA. A multidisciplinary approach to critical path development: a valuable CQI tool. J Nurs Care Qual 1994; 8: 38-41.
- Weilitz PB, Potter PA. A managed care system. Financial and clinical evaluation. J Nurs Admin 1993; 23: 51-7.
(Received 27 Jan, accepted 20 Aug, 1998)
Authors' details
Department of Orthopaedics, St Vincent's Hospital, Melbourne, VIC.Michelle M Dowsey, BN, GradCertOrth, Clinical Nurse Specialist;
Meredith L Kilgour, BN, GradDipAdvClinPrac, Nurse Unit Manager;
Nick M Santamaria, BAppSc, PhD, Director of Nursing Research;
Peter F M Choong, MD, FRACS, Professor, and Director of Orthopaedics.
Reprints: Professor P F M Choong, Department of
Orthopaedics, St Vincent's Hospital, 41 Victoria Parade, Fitzroy,
VIC 3065.
Email: PeterChoongATc031.aone.net.au
Received 26 May 2026, accepted 26 May 2026
- Michelle M Dowsey
- Meredith L Kilgour
- Nick M Santamaria