|
Research
Hospital in the home: a randomised controlled trial
Gideon A Caplan, John A Ward, Nicholas J Brennan, Janis Coconis,
Neville Board and Ann Brown
MJA 1999; 170: 156-160
For editorial comment, see Montalto
|
Abstract |
Objectives: To compare treatment of acute illness at
home and in hospital, assessing safety, effect on geriatric
complications, and patient/carer satisfaction.
Design: Randomised controlled trial.
Setting: A tertiary referral hospital affiliated with
the University of New South Wales.
Participants: 100 patients (69% older than 65 years) with
a variety of acute conditions, who were assessed in the emergency
department as requiring admission to hospital.
Interventions: Patients were allocated at random to be
treated by a hospital-in-the-home (HIH) service in their usual
residence or to be admitted to hospital.
Main outcome measures: Geriatric complications
(confusion, falls, urinary incontinence or retention, faecal
incontinence or constipation, phlebitis and pressure areas),
patient/carer satisfaction, adverse events, and death.
Results: There was a lower incidence of confusion (0 v.
20.4% [95% CI, 9.1%-31.7%]; P = 0.0005), urinary
complications (incontinence or retention) (2.0% [95% CI, -1.8%,
5.8%] v. 16.3% [95% CI, 6.0%, 26.6%]; P = 0.01), and bowel
complications (incontinence or constipation) (0 v. 22.5% [95% CI,
10.7%, 34.1%]; P =0.0003) among HIH-treated
patients. No significant difference in number of adverse events and
deaths (to 28 days after discharge) in the two groups was found
(although numbers were small). Patient and carer satisfaction was
significantly higher in the HIH group.
Conclusions: Home treatment appears to provide a safe
alternative to hospitalisation for selected patients, and may be
preferable for some older patients. We found high levels of both
patient and carer satisfaction with home treatment.
|
| | Introduction |
Acute care of patients at home is one of the fastest-growing
healthcare sectors in the United States1-3 and is gaining acceptance
in many countries.4 Although there have been
randomised controlled trials of patients receiving home versus
hospital treatment for deep venous thrombosis,5 there are few
data from trials involving other conditions, or assessing the safety
of acute care at home, especially for older patients. It is these
patients who occupy an increasing proportion of hospital beds and may
derive most benefit from home treatment.6,7 Recent studies characterising hospital-associated adverse
events8,9 make home treatment more
attractive,10 especially for elderly
patients who are known to suffer a higher incidence of complications
in hospital.11 When treated at home,
patients do not have to change their environment or routine, they are
not exposed to nosocomial infection, and they do not need to adapt to
the sociological culture of the hospital. On the other hand, the
incidence and severity of intrinsic complications in older patients
can be minimised by round-the-clock supervision by expert staff in
hospital. However, there is inadequate evidence to support the
popular belief that programs which transfer care to the home result in
a worse outcome for the patients.12,13
We have conducted a randomised controlled trial of a
hospital-in-the-home (HIH) program targeting older patients. We
selected conditions which were amenable to home treatment, but tried
to include a variety of diagnostic groups. To accentuate the
difference between the two groups, the HIH patients were taken home on
the day of presentation to the emergency department, or on the
following morning if they presented at night. We studied the safety,
efficacy and patient/carer satisfaction of home treatment compared
with hospital treatment.
|
| |
Methods |
Patients and randomisation
One hundred patients requiring admission to hospital and meeting
criteria for study inclusion were randomised to HIH treatment
(intervention group) or treatment in hospital (control group). We
targeted patients older than 65 years, including those living in
nursing homes, but also accepted younger patients. Patients were
accepted only if they had been assessed as requiring admission by the
relevant medical or surgical team. The medical, surgical and
emergency department staff were encouraged to refer patients with
acute (pneumonia, urinary tract infections and cellulitis) and
subacute (endocarditis and osteomyelitis) infections requiring
treatment with intravenous antibiotics, deep venous thrombosis
(DVT), minor cerebrovascular accidents (not affecting mobility or
swallowing), and cardiac failure.
Patients were excluded from the study
- if they had evidence of shock (systolic blood pressure <
100 mmHg);
- if they required oxygen (Pao2 < 60 mmHg);
- if they were judged too unwell by the study team;
- if they had no available carer;
- if they lived outside the local area; or
- if their home was unsuitable for home treatment (lack of running
water, electricity or an inside toilet, concerns about safety, or
dangerous pets).
If any doubts about home suitability arose during the emergency
department assessment, a study nurse visited the home before
randomisation.
After informed consent was obtained from the patient (written) and
the patient's carer (verbal), randomisation (stratified according
to whether the patient lived at home or in a nursing home, or had DVT) was
achieved by computer-generated random numbers coded into sealed
envelopes.
The study protocol required that patients in the HIH group be
discharged from hospital within 24 hours of diagnosis. HIH patients
receiving intravenous antibiotics were given the first dose in
hospital. The study protocol was approved by the hospital's Research
Ethics Committee.
Data collection
For all study patients, study nurses completed a Barthel Index of
Activities of Daily Living,14 a modified Instrumental
Activities of Daily Living Index15 and a Mental Status
Questionnaire16 on admission and
discharge. Baseline demographic data on current medical diagnoses,
a detailed social history, physical function, medications and
allergies were also recorded.
Hospital treatment
Hospital patients (control group) were admitted under the
appropriate physician or surgeon of the day and treated in accordance
with standard regimens without the intervention of the study team.
The hospital team treating the patient was notified that the patient
had been included in the trial.
HIH treatment
HIH patients (intervention group) were treated according to the
presenting diagnosis by the hospital community outreach team. The
range of treatments in the study protocol included administration of
parenteral antibiotics and other medications, and blood
transfusions. Infections were generally treated with once-daily
intravenous antibiotics such as ceftriaxone, gentamicin or
vancomycin, as appropriate, according to the result of
bacteriological tests (if positive) or by diagnosis. Intravenous
access was usually via cannulas inserted by study nurses. Owing to
safety concerns, some patients with dementia did not have cannulas
left in situ, and were cannulated daily with butterfly
cannulas. Patients requiring long term treatment or with difficult
venous access were treated via a peripherally inserted central
cannula. Patients with DVT were treated with daily subcutaneous
enoxaparin injections (1.5 mg/kg) and oral warfarin until
their international normalised ratio was 2.0 or above.
GP involvement
Before the study, we conducted an educational program consisting of
an evening lecture and a question-and-answer session for the local
division of general practice. Study nurses also visited general
practitioners (GPs) and nursing homes to explain the program. Our
preference was for the patient's own GP to be the primary medical
manager, and we therefore sought the agreement of the patient's GP
before entering the patient in the trial. If GPs declined to
participate, the hospital provided medical support.
Follow-up
After discharge, an unmarked satisfaction survey based on the
principles outlined by Draper and Hill,17 colour coded to
differentiate between responses from HIH and hospital treatment,
was sent to patients, carers and GPs. This was followed by a phone call
to encourage response. Patients were asked "How would you rate your
treatment overall?" and offered a four-point scale of answers:
excellent (1), good (2), fair (3), and poor (4). A similar question
about satisfaction with the patient's care was asked of the carer and
GP. Patients were recontacted by telephone at one and six months after
discharge to ascertain their health status.
Complications
Complications were assessed by two methods. Study personnel
performed a systematic medical record review, focusing on the more
common geriatric syndromes, as recorded in the patients' notes. The
geriatric syndromes18 include confusion,
falls, incontinence of bladder and bowel, constipation, urinary
retention, and pressure ulcers. These are not specific to older
patients, but occur more commonly in frail elderly patients
(geriatric patients).
The medical records were also assessed according to the validated
method of counting adverse events developed for the Harvard Medical
Practice Study8 and refined in the Quality in
Australian Health Care Study (QAHCS). This was done by independent
reviewers engaged from the team of the Australian study.9 This method
records an adverse event -- unintended injury or complication -- only
if it results in disability, death or prolonged hospital stay and is
caused by healthcare management. The reviewers were a doctor and a
nurse with extensive experience of QAHCS procedures. Reliability
assessments were undertaken by a senior member of the QAHCS study
team. The only difference from the standard technique was that the
reviewers were instructed only to seek adverse events arising after
randomisation, whereas the original study also sought those which
had caused the admission.
Statistical analyses
The study had a power of 80%, assuming  = 0.05, to find a
difference of about 20% in the occurrence of complications. All
analyses were performed on the basis of intention to treat, using the
SPSS for Windows and Epi Info statistical packages.19,20
Continuous data are expressed as means and 95% confidence intervals
(95% CI) and were compared by t tests. Satisfaction scores
were compared by the Mann-Whitney U test. Fisher's exact test
was used to compare proportions. All statistical tests were
two-tailed. = 0.05, to find a
difference of about 20% in the occurrence of complications. All
analyses were performed on the basis of intention to treat, using the
SPSS for Windows and Epi Info statistical packages.19,20
Continuous data are expressed as means and 95% confidence intervals
(95% CI) and were compared by t tests. Satisfaction scores
were compared by the Mann-Whitney U test. Fisher's exact test
was used to compare proportions. All statistical tests were
two-tailed.
|
| |
Results |
Between October 1995 and February 1997, 129 patients requiring
admission to hospital were assessed for participation in the study.
Reasons for exclusion before randomisation were: patient too unwell
for home treatment (12 patients), patient declined (6), carer
refused or no carer available (9), and patient lived too far from the
hospital (2). One hundred patients were enrolled; 51 were allocated
at random to HIH treatment and 49 to hospital treatment. The two groups
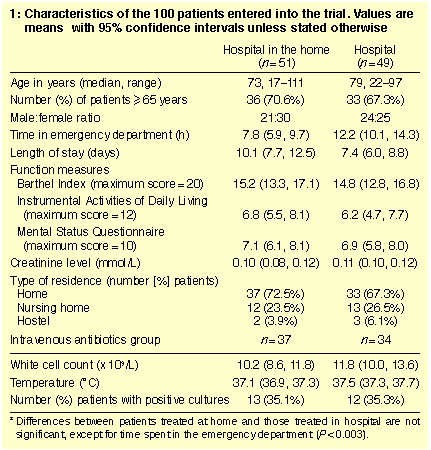
were comparable in characteristics and diagnoses (Tables 1 and 2). A
quarter of the patients lived in nursing homes and 69% were 65 years of
age or older. For 92 of the patients their GP agreed before
randomisation to assist in their care. Four patients had no GP, one GP
was not interested and three patients' GPs could not be contacted
before randomisation.
Adverse events and complications
The proportion of adverse events was similar in the HIH group and the
control (hospital) group (11.8% [95% CI, 3.0%, 20.6%] v. 16.3% [95%
CI, 6.0%, 26.6%]). However, there was a significantly lower
occurrence in the HIH group of confusion, urinary (either
incontinence or retention) complications, and bowel (either
constipation or faecal incontinence) complications (Table 3).
Home visits
On average, patients in the HIH group were seen, at home, on 9.0
occasions by the study nurse, 0.8 times by their GP, 0.9 times by a
doctor from the hospital, 0.2 times by a physiotherapist, and 0.1
times by an occupational therapist. This translates to one visit per
day by the nurse, given that each patient was also seen by a study nurse
in the emergency department.
Outcomes
Treatment failed in four of the 51 patients in the HIH group and they
were admitted to hospital. Three and five patients in the HIH group and
the hospital-treated group, respectively, were recorded as having
an unplanned readmision within 28 days of discharge.
There was one death in each of the HIH- and hospital-treated groups
during the admission. Total deaths up to 28 days after discharge were
three in the HIH group and four in the hospital-treated group, and at
six months after discharge six and seven deaths, respectively, had
occurred. There were no significant differences between the two
groups in these outcomes.
Patient, carer and GP satisfaction
The response rates for the satisfaction surveys were (HIH v.
control): patients 78% v. 40%, carers 55% v. 27%, and GPs 63% v. 37%.
There was significantly greater satisfaction with overall HIH
treatment among both patients (P < 0.0001) and
their carers (P = 0.0001). Despite the increased
workload and despite having to deal with more severely ill patients
than usual, GPs were equally satisfied by home and hospital treatment
(Table 4).
|
| |
Discussion |
In our study, treatment of a range of acute infections and other
diseases at home was as safe as treatment in hospital. Previous
studies which claimed to have demonstrated safety documented so few
complications that risk appeared to have been eliminated by patient
selection.1-3 Our study group's 7%
mortality up to 28 days after discharge (compared with zero mortality
in previous studies1-3) establishes our
patients' illness severity.
The most significant finding resulting from our inclusion of
geriatric complications was the higher incidence of confusion in
hospital-treated patients. The role of the hospital environment in
the aetiology of delirium has long been recognised,21 although this
is not universally accepted.22 For some of the patients in
our study recorded as having confusion, all of the features of
delirium according to the Diagnostic and statistical manual of
mental disorders (DSM-IV)23 were not present. Our aim
was to be as inclusive as possible of geriatric complications, so that
if a problem was noted by ward staff or carers it was included even if
study personnel had not observed it. These complications were not
always serious clinically and often did not have a great impact, but we
valued the perspective of patients, families and hospital staff.
Similarly, the occurrence of urinary and bowel complications
reflects the difficulty of caring for frail elderly
patients24 (especially those from
nursing homes) in an acute hospital ward. Patients with mobility or
communication problems require carers attuned to their routines and
signals to maintain continence.
Because of small numbers our study was limited in its power to draw
conclusions about the difference between HIH and hospital treatment
as far as adverse events and deaths were concerned. As there have been
no previous studies addressing this question, it was not possible to
estimate the size of the expected difference. Another limitation of
our study was that, although we did not directly inform the adverse
event reviewers about which patients were in each group, we were not
able to completely blind them to the status of each group because of
stylistic differences between the patient records of the hospital-
and the HIH-treated patients.
Few similar comparative studies have been published. As reports and
discussions entitled "home hospitalisation" or "hospital at home",
for example, may include few or no acute patients, the home treatment
of acute illness is obscured in the medical literature.25,26 Our study
included only patients who met the criterion of requiring admission
to hospital because of illness. By bringing the hospital care to the
patient's home, we substituted completely for hospital facilities.
There is a need for more studies of patients with illness of this
severity treated at home.
A number of factors may explain the greater satisfaction with
treatment at home. In their own homes, patients are in their familiar
environment, their privacy is protected, their sleep less
interrupted, and they can eat their usual food.27,28 As an
example, for an elderly patient with limited cognitive function
and/or decreased visual acuity, finding the bathroom at night in
hospital may be impossible. Moreover, elderly patients may be unable
to get out of bed because of rails on the sides of the bed. These
difficulties may have contributed to the higher incidence of
incontinence in our hospital-treated group. At home, patients are
more active participants, often partners, in their care. All these
factors invariably translate into greater satisfaction with home
treatment.29
Frail, older patients -- because of their atypical disease
presentations, more rapid deterioration when ill and greater
prevalence of disease -- need hospital-level services more
frequently than younger patients. However, admission to hospital,
like any medical intervention, has side effects as well as
benefits.8 Elderly patients have more
to gain from many treatments (eg, thrombolytic therapy) because of
their higher underlying mortality rates,30 but they also suffer from a
much greater occurrence of iatrogenic complications.10 Although many
of these complications may be explained by an interaction between
their underlying frailty and their disease process,8 we were able to
detect a measurable effect attributable to a change of environment.
The results of this study do not imply that older patients should never
be admitted to hospital. On the contrary, the elderly as a group have
more need for the technical expertise of the acute hospital than
younger people. However, if such technical expertise can be
delivered at home, this alternative should at least be evaluated. On
the other hand, our study does not imply that treatment which can be
delivered at home should always be delivered at home. Successful home
treatment depends on careful patient and home selection, as the
necessary minimum level of sanitation, facilities and support from
carers is not universally available.4 However, where it is
feasible, we have demonstrated that home treatment of acute illness,
even for frail elderly patients, can be effective, safe and more
satisfying for the patient and their families.
|
| |
Acknowledgements |
We would like to acknowledge the invaluable assistance of the staff of
Post Acute Care Services and the Emergency Department at Prince of
Wales Hospital and Ms Bernie Harrison and Dr Ross Wilson from QARNS at
Royal North Shore Hospital.
This study was supported by a grant from the Commonwealth Department
of Health and Family Services - Hospital Access (National Projects)
Program.
|
| |
References |
- Antoniskis A, Anderson BC, Von Volkinburg EJ, et al. Feasibility of
outpatient self-administration of parenteral antibiotics.
West J Med 1978; 128: 203-206.
-
Kind AC, Williams DN, Persons G, et al. Intravenous antibiotic
therapy at home. Arch Intern Med 1979; 139: 413-415.
-
Stiver HG, Telford GO, Mossey JM, et al. Intravenous antibiotic
therapy at home. Ann Intern Med 1978; 89: 690-693.
-
Tice AD. Outpatient parenteral antibiotic therapy in different
countries. Int J Infect Dis 1996; 1: 102-106.
-
Levine M, Gent M, Hirsh J, et al. A comparison of
low-molecular-weight heparin administered primarily at home with
unfractionated heparin administered in the hospital for proximal
deep-vein thrombosis. N Engl J Med 1996; 334: 677-681.
-
Balinsky W, Nesbitt S. Cost-effectiveness of outpatient
parenteral antibiotics: a review of the literature. Am J Med
1989; 87: 301-305.
-
Poretz DM, Eron LJ, Goldenberg RI, et al. Intravenous antibiotic
therapy in an outpatient setting. JAMA 1982; 248: 336-339.
-
Leape LL, Brennan TA, Laird N, et al. The nature of adverse events in
hospitalised patients: results of the Harvard Medical Practice
Study II. N Engl J Med 1991; 324: 377-384.
-
Wilson RM, Runciman WB, Gibberd RW, et al. The quality in Australian
health care study. Med J Aust 1995; 163: 458-471.
-
Caplan GA, Brown A. Post acute care: can hospitals do better with
less? Aust Health Rev 1997; 20: 43-54.
-
Fretwell MD. Acute hospital care for frail older patients. In:
Hazzard WR, Andres R, Bierman EL, Blass JP, editors. Principles of
geriatric medicine and gerontology, 2nd ed. New York: McGraw-Hill,
1990: 247-253.
-
Maxwell RJ. Why rationing is on the agenda. Br Med Bull
1995; 51: 761-768.
-
Larkins RG, Martin TJ, Johnston CI. The boundaryless hospital -- a
commentary. Aust N Z J Med 1995; 25: 169-170.
-
Mahoney FI, Barthel DW. Functional evaluation: the Barthel
index. Md Med J 1965; 14: 61-65.
-
Lawton MP, Brody EM. Assessment of older people:
self-maintaining and instrumental activities of daily living.
Gerontologist 1969; 9: 179-186.
-
Pfeiffer E. A short portable mental status questionnaire for the
assessment of organic brain deficit in elderly patients. J Am
Geriatr Soc 1975; 23: 433-441.
-
Draper M, Hill S. The role of patient satisfaction surveys in a
national approach to hospital quality management. Canberra: AGPS,
1996.
-
Hazzard WR, Andres R, Biermen EL, Blass JP, editors. Principles of
geriatric medicine and gerontology. 2nd ed. Section 4 -- geriatric
syndromes and special problems. New York: McGraw-Hill, 1990:
1055-1222.
-
SPSS for Windows [computer program], version 6.0. Chicago: SPSS
Inc, 1993.
-
Dean AG, Dean JA, Burton AH, Dicker RC. Epi-Info [computer
program], version 5. Stone Mountain, Ga: USD Inc, 1990.
-
Wahl CW, Golden JS, Liston EH, et al. Toxic and functional
psychoses: diagnosis and treatment in a medical setting. Ann
Intern Med 1967; 66: 989-1007.
-
Lipowski ZJ. Delirium and impaired consciousness. In: Evan JG,
Williams TF, editors. Oxford textbook of geriatric medicine.
Oxford: Oxford University Press, 1992: 490-495.
-
American Psychiatric Association. Diagnostic and statistical
manual of mental disorders (DSM-IV). Washington, DC: APA, 1994.
-
Caplan GA, Brown A, Croker WD, Doolan J. Risk of admission within
four weeks of discharge of elderly from the emergency department --
the DEED study. Age Ageing. In press.
-
Stressman J, Ginsberg G, Hammerman-Rozenberg R, et al. Decreased
hospital utilization by older adults attributable to a home
hospitalization program. J Am Geriatr Soc 1996; 44: 591-598.
-
Donald IP, Baldwin RN, Bannerjee M. Gloucester
hospital-at-home: a randomized controlled trial. Age Ageing
1995; 24: 434-439.
-
Consumer reports of hospital experiences. In: Draper M, Hill S,
editors. The role of patient satisfaction surveys in a national
approach to hospital quality management. Canberra: AGPS, 1996:
12-20.
-
Cruse PJE, Foord R. The epidemiology of wound infection: a 10-year
prospective study of 62,939 wounds. Surg Clin North Am 1980;
60: 27-40.
-
Brown RB. Selecting the patient. Hosp Pract 1993;
28(Suppl 1): 11-15.
-
Fibrinolytic Therapy Trialists' (FTT) Collaborative Group.
Indications for fibrinolytic therapy in suspected acute myocardial
infarction: collaborative overview of early mortality and major
morbidity results from all randomised trials of more than 1000
patients. Lancet 1994; 343: 311-322.
(Received 17 Jun, accepted 22 Oct, 1998)
|
| | Authors' details
|
Post Acute Care Services, Prince of Wales Hospital, Sydney, NSW.
Gideon A Caplan, MB BS, FRACP, Director; and Lecturer,
University of New South Wales, Sydney, NSW; Nicholas J
Brennan, MB BS, FRACP, Senior Registrar;
Janis Coconis,
RN, Clinical Nurse Specialist;
Neville Board, RN, BA,
Research Assistant;
Ann Brown, RN, Nurse Manager.
Community Health Services and Programs, South Eastern Sydney Area
Health Service, Sydney, NSW.
John A Ward, MB BS, MSc, FRACP, Community Geriatrician; and
Lecturer, University of New South Wales, Sydney, NSW.
Reprints: Dr G A Caplan, Post Acute Care Services, Prince of
Wales Hospital, Randwick, NSW 2031.
Email: g.caplanATunsw.edu.au
|
| |
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
|
| | 
Back to text | | 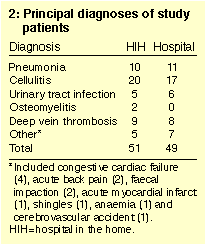
Back to text | | 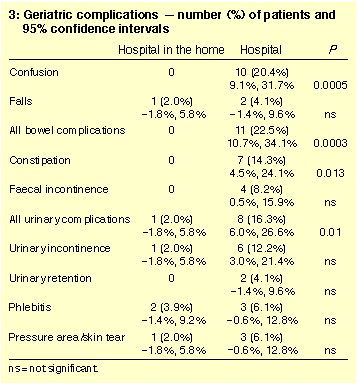
Back to text | | 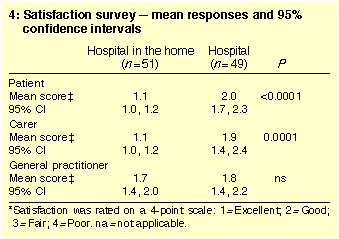
Back to text |
|








