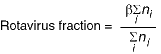Rotavirus infection and rates of hospitalisation for acute gastroenteritis in young children in Australia, 1993-1996
John B Carlin, Patty Chondros, Paul Masendycz, Helen Bugg, Ruth F Bishop and Graeme L Barnes
For editorial comment, see Ferson
MJA 1998; 169: 252-256
Abstract - Introduction - Methods - Results - Discussion - Acknowledgments - References - Authors' details - Figure 1 - Figure 2
-
-
-
©MJA1998
Abstract |
Objective: To determine rates of hospitalisation of
young children for acute gastroenteritis in Australia, and to
estimate the proportion of these admissions caused by rotavirus
infection. Design: Analysis of hospital admission records, and parallel, prospectively collected data on rotavirus-positive admissions. Setting: Hospitals admitting young children in all Australian States and Territories in 1993-1996. Patients: All children under five years admitted to hospital for acute gastroenteritis (International Classification of Diseases, ninth revision principal diagnosis codes 003.0, 004.0-009.3 and 558.9). Main outcome measures: Rate of hospital admission per 1000 children per year by State, and the proportion of admissions caused by rotavirus infection. Results: There were almost 20 000 hospital admissions annually in Australia for acute gastroenteritis in children under five years, at an average rate of 15/1000. An estimated 50% of these were attributable to rotavirus infection, implying a rate of hospitalisation for rotavirus-related gastroenteritis of 7.5/1000/year. Among children under two years this rate was 11.6/1000. Rotavirus incidence rates generally followed a typical seasonal pattern in temperate regions of the country, with sharp peaks in mid to late winter. Rates of hospitalisation varied markedly, even between States with apparently similar patterns of disease, while the incidence in the Northern Territory was 3-5 times higher than other States. Conclusions: Rotavirus-related gastroenteritis is a major cause of hospital admissions in young children, and large savings to the healthcare system are possible if it can be prevented at reasonable cost. Variation in treatment practices between States may be worth studying in greater detail as another source of potential savings. MJA 1998; 169: 252-256 | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Introduction |
Rotavirus is a major cause of severe gastroenteritis in young
children. Although discovered only 25 years ago,1 the role of this virus in the huge
burden of diarrhoeal disease in developing countries was recognised
quickly, and in 1985 it was estimated to be responsible for 870 000
deaths annually.2 In
developed countries, mortality from gastroenteritis is low, but
many studies have documented the large burden of morbidity caused by
rotavirus.3-7 Precise estimates of rotavirus-related morbidity are difficult to obtain from routine hospital data because stool samples for microbiological testing are not obtained from all children admitted to hospital with diarrhoea. Even when testing is performed, the findings may not be recorded or coded in the medical record. There was no specific category in the International Classification of Diseases, ninth revision (ICD-9-CM) for rotavirus diarrhoea until 1993, and since then the specified code (008.61) has not been used consistently. However, many studies have shown that at least 30% of hospital admissions for acute gastroenteritis in young children are the result of rotavirus infection and, further, that the incidence of rotavirus infection has a distinctive cyclical pattern with a peak in winter (this is unique to rotavirus among all major pathogens associated with gastroenteritis).3,4,6,8-10 While other Australian studies have examined aspects of rotavirus gastroenteritis,5,11 there are no national population-based estimates of the incidence of hospital admission for acute gastroenteritis in young children. Such estimates are important in assessing preventive measures, and in evaluating the cost-effectiveness of rotavirus vaccines currently under development.12,13 We aimed to provide the first national data on rates of hospitalisation of young children for acute gastroenteritis in Australia, and to estimate the proportion of these admissions that could be ascribed to rotavirus infection. Our results will be used in a later study to estimate the cost-effectiveness of rotavirus vaccination. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Methods |
State and Territory health departments provided computer files with
unidentified records for the years 1993 through 1996 of all hospital
admissions of children under the age of five with a principal
diagnosis in the medical record of acute gastroenteritis. In our
analysis, we combined data from the Australian Capital Territory
with those from New South Wales.
Acute gastroenteritis was identified as ICD-9-CM codes in the range 003-009 (covering infectious gastroenteritis of various known and unknown origins) or code 558.9 ("other and unspecified noninfectious gastroenteritis"). This last code was included for consistency with other studies in the expectation that it might comprise a substantial number of cases of infectious gastroenteritis. Similar files of admission records were obtained from participating paediatric hospitals in each of the States (see Box 1). Records from the Royal Children's Hospital (RCH), Melbourne, and Princess Margaret Hospital (PMH), Perth, also included an identifying hospital record number.
Microbiology departments at participating hospitals were asked to forward all rotavirus-positive faecal specimens obtained from children under five years who were admitted for acute gastroenteritis to laboratories at RCH, where rotavirus infection was confirmed by enzyme immunoassay.14 All participating hospitals provided specimens over the entire study period, except that Westmead Hospital participated in the study for the first two years only, and was replaced by Sydney Children's Hospital in 1995. Seasonal, temporal, and geographic variation in strains of rotaviruses will be reported elsewhere. We estimated the proportion of gastroenteritis admissions that were caused by rotavirus infection both by direct and indirect means. The direct method involved a linked analysis of admissions and rotavirus data. Admission and laboratory records from RCH (Melbourne) and PMH (Perth) were linked by means of hospital unit record number and date of admission/date of specimen, thus identifying the proportion of admissions that we could directly confirm as involving rotavirus infection. This analysis was supplemented with information from each hospital's pathology records, as it became clear that not every rotavirus-positive specimen was being sent on to our laboratory (usually owing to insufficient size of samples). Further, it was possible to omit patients for whom no faecal test was performed, to give a more appropriate denominator for estimating the fraction admitted because of rotavirus infection (calculated as rotavirus fraction = number of admissions with positive rotavirus test result/number of admissions with faecal specimen tested). The indirect statistical estimation of the rotavirus fraction and the rationale behind this method are described in Box 2. The study was approved by ethics committees in each of the participating hospitals.
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Results | Total numbers and estimated rates of acute gastroenteritis admissions are shown in Box 3. Of all admissions, 65.7% involved children under the age of two years, with approximately equal numbers in each of the first two years of life, and declining numbers in each of the subsequent three years to age five. The age breakdown was similar in all States except the Northern Territory, where a substantially larger proportion were aged under two (86.1%). Length of stay was also considerably longer in the Northern Territory. There were slightly more boys than girls (53.1% overall), consistent across all States. Of all admissions, 29.4% were coded 558.9, although this proportion declined sharply over the four years of the study as coding practices apparently changed. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
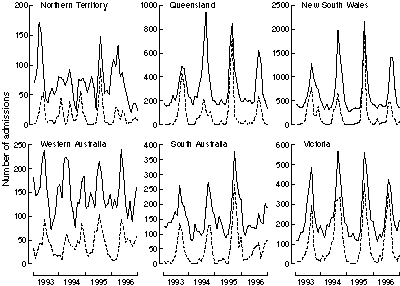
Box 4 shows the temporal pattern of all admissions and of rotavirus
admissions in index hospitals in the five largest States and the
Northern Territory. The seasonal peaks in the eastern States (New
South Wales, Victoria, Queensland, and South Australia)
For the data linkage method, among 1732 children admitted for whom a specimen was tested, we received 767 rotavirus-positive specimens from RCH (Melbourne) and found another 205 admissions with hospital records showing a positive rotavirus test, giving an estimated rotavirus fraction of 56%. The corresponding totals from PMH (Perth) were 1631, 626 and 161, respectively, giving a rotavirus fraction of 49%. Regression estimates of the rotavirus fraction ranged from a low of 22% for the Northern Territory (based on a total of 598 rotavirus-positive specimens) to a high of 41% for Victoria (984 specimens). When data from all States were combined, the correlation between rotavirus numbers and admissions increased, because a more accurate representation of the relationship between total admissions and rotavirus numbers in participating hospitals was obtained by pooling. The resulting estimated rotavirus fraction was 50% (based on 4634 specimens received). Separate estimates obtained for children aged under one year, one year to less than two years, and at least two years were 34%, 60% and 48%, respectively. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Discussion |
This national four-year study has shown that there are almost 20 000
hospital admissions annually in Australia for acute
gastroenteritis in children aged under five years -- an average rate
of 15 per 1000, 50% of which appear to be attributable to rotavirus
infection. The annual rate of hospitalisation for
rotavirus-related gastroenteritis in children under five is
therefore about 7.5 per 1000. Among children under two years,
combining estimates for the two one-year age brackets, the
corresponding rate is 11.6 per 1000, or just over one in every 100
children.
Of the two methods we used to estimate the proportion of admissions that were caused by rotavirus, the method involving direct linkage of hospital admission records and stool specimen tests is likely to be the more accurate. Estimates of 56% (Melbourne) and 49% (Perth) were obtained for the two centres where it was available. These estimates may be too low, as enzyme immunoassay can fail to detect up to 10% of rotavirus-positive specimens.15 Conversely, they might be too high on a population-wide basis, as they were based on tertiary referral centres where the severity of admitted cases -- and therefore the likelihood of rotavirus involvement -- might be higher (although this was only weakly supported by our data on mean length of stay [LOS], which showed a small difference between RCH [mean LOS 1995-1996, 2.15 days] and the whole of Victoria [1.87 days], and no difference between PMH and WA averages [2.80 v. 2.85]). Our second method, based on a regression model, was subject to statistical fluctuations and assumptions that imply it might produce an underestimate of the rotavirus fraction (see Box name="box2"2). In particular, the coverage of rotavirus specimen collection varied between States and also, at times, within States. For example, only a relatively small number of specimens (457) were ascertained from New South Wales, implying that the rotavirus fraction for that State might be considerably underestimated. In fact, when the regression method was applied to the pooled national data, we found reasonable convergence between the two methods, and believe they both support the conclusion that 50% of all gastroenteritis admissions in this age group are due to rotavirus. A reasonable range of possible alternative estimates around this value would be from 40% to 60%. In other studies, estimates of the proportion of hospital admissions in children under five years attributable to rotavirus have ranged from around 30% to as high as 66%.3,4,6,8,9,16 United States studies from the Centers for Disease Control have estimated this proportion both by a simple "residual" method based on assuming that all diarrhoea admissions in the winter seasonal peaks are rotavirus-related,17 and a more direct method based on an eight-year series of children admitted to a Washington DC hospital.6 Both methods indicated that rotavirus was responsible for about one-third of admissions, and the corresponding annual rate of hospitalisation for rotavirus-related gastroenteritis in children under five years was 2.8 per 1000. In the United Kingdom, estimates have been based on laboratory surveillance and hospital discharge data, with a similar statistically based estimation procedure to ours.4 It was found that 43% of admissions in children under five years could be attributed to rotavirus, corresponding to 5.3 per 1000 admissions per year. A New South Wales study by Ferson also used a regression method, based on a larger sample of rotavirus surveillance data than ours, and estimated an annual rate of hospital admission of 8.7 per 1000.5 Using the 1993-1996 NSW hospital admission rates (Box name="box3"3), this corresponds to a rotavirus fraction of 51%, very consistent with our national estimate. Ferson's study found over twice the rate of rotavirus gastroenteritis in the second year of life compared with the first, a slightly greater difference than suggested by our data. The findings of both studies are consistent with a detailed investigation of children with gastroenteritis over 13 years at RCH Melbourne, which found that no pathogen could be identified in a substantially greater proportion of infants under six months than in older children.18 There were substantial differences in hospital admission rates between the States, with NSW, Queensland and South Australia having almost twice the rate of hospitalisation of Victoria. It seems very unlikely that these differences are the result of different disease patterns, especially as the seasonal patterns in these States were very similar. Nor are they likely to be explained by differences in coding, as our incidence figures are based on an inclusive selection of principal diagnosis ICD-9-CM codes. In particular, the inclusion of code 558.9 ("non-infectious gastroenteritis") identified a substantial number of apparently miscoded cases of viral diarrhoea, consistent with findings in other reports.4,5 The differences may reflect variations in patterns of primary care influencing the numbers of children who present to hospital emergency departments, and/or differences in hospital admission policies. The relative importance of each of these factors warrants further study, as it appears likely that substantial savings could be made if hospitalisation rates nationally could be reduced. There were no major seasonal differences in gastroenteritis incidence between States, except in the Northern Territory and Western Australia, where the relative importance of rotavirus in the gastroenteritis disease burden may be somewhat reduced. There is little evidence in our data of a progressive spread of the rotavirus epidemic across the country each year, in the manner that has been described in North America,19 apart from the fact that the annual peak of rotavirus activity in Western Australia appears generally to precede that in the eastern States. The Northern Territory was the most clearly distinct of all the regions, not only in its substantially higher hospital admission rate and lack of seasonal pattern, but also in the dramatically longer length of stay of patients. Average length of stay in this study (2.2 days, excluding the Northern Territory) was substantially shorter than that reported in the United States (3.9 days20), but very similar to British findings.4 Given the higher admission rates in Australia, shorter length of stay may reflect a less severe spectrum of illness, or possibly better management involving more widespread use of oral rehydration solution. Our results imply that 10 000 hospital admissions occur annually in Australia for rotavirus gastroenteritis. The direct cost of this hospital care is at least $12 million, based on an (Australian national diagnosis-related group-based) estimate of $1244 per admission,21 and may be as high as $15-$18 million (preliminary analysis, RCH [Melbourne] costing data). A successful rotavirus vaccine -- depending on its cost -- could result in substantial savings to the healthcare system. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Acknowledgments | The study was funded by the Public Health Research and Development Committee of the National Health and Medical Research Council. It would not have been possible without the generous cooperation of numerous individuals in all State and Territory health authorities, and in medical records and hospital information units at the participating hospitals, or without the participation and skilled assistance of the following microbiologists and paediatricians: G Davidson, P Goldwater, T Kok, A Lawrence, L Micken, S Weir (Adelaide); G Clift, J Erlich, J Hagger, R Matters, F Morey (Alice Springs); J Faogali, J Farrah, R Shepherd, M Witt (Brisbane); G Lum, A Lowe, A Ruben, B Way, K Withnall (Darwin); A Carmichael, A Claridge, K Dahlenburg, R Fang, R Tucker (Hobart); B Crawford, G Hogg, B Ross, R Schnagl, P Ward (Melbourne); B Dwyer, R Hill, A May, G O Connor, B Wild (Perth); P Amin, T Borg, A Cunningham, J MacRae, P McIntyre, C McIvor, K McPhie, J Mitchell, J Montgomery, G Sandico (Sydney). | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
References |
(Received 30 Oct 1997, accepted 4 May 1998) | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Authors' details
Clinical Epidemiology and Biostatistics Unit, Royal Children's Hospital, Melbourne, VIC.John B Carlin, BSc(Hons), PhD, Deputy Head, and Associate Professor, Department of Paediatrics, University of Melbourne; Patty Chondros, BSc(Hons), Research Assistant.
Department of Gastroenterology and Clinical Nutrition, Royal Children's Hospital, Melbourne, VIC.
Paul Masendycz, BAppSc, Research Assistant; Helen Bugg, BSc, Research Assistant; Ruth F Bishop, AO, DSc, PhD, Senior Principal Research Fellow (NHMRC, and Professor, Department of Paediatrics, University of Melbourne; Graeme L Barnes, MD, FRACP, Senior Gastroenterologist, and Associate Professor, Department of Paediatrics, University of Melbourne.
Reprints: Associate Professor G L Barnes, Department of Gastroenterology and Clinical Nutrition, Royal Children's Hospital, Parkville, VIC 3052. E-mail: barnesgATcryptic.rch.unimelb.edu.au
-
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
Received 10 June 2026, accepted 10 June 2026
- John B Carlin
- Patty Chondros
- Paul Masendycz
- Helen Bugg
- Ruth F Bishop
- Graeme L Barnes





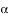 = monthly number of admissions statewide not caused by rotavirus; and
= monthly number of admissions statewide not caused by rotavirus; and
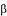 = scaling factor relating the number of "rotavirus-positive" admissions in the State to that in the index hospital(s).
= scaling factor relating the number of "rotavirus-positive" admissions in the State to that in the index hospital(s).
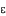 i = random error) is: Ni =
i = random error) is: Ni =