|
Medical Research Perspectives
The Menzies School of Health Research offers a new paradigm of
cooperative research
John D Mathews
The Menzies School has addressed problems in Aboriginal and tropical
health through research that requires cooperation between
disciplines as well as improved communication and trust between
researchers, Aboriginal people and the wider community.
MJA 1998; 169: 625-629
Introduction -
The politics of Aboriginal health -
Success in interdisciplinary and crosscultural collaboration -
Some research highlights of medical importance -
The Menzies School's work in central Australia -
Research highlights in tropical and international health -
Resources and links -
Cooperation is the secret of success -
Looking ahead -
Acknowledgements -
References -
Author's details
-
-
More articles on Aboriginal health
|
| |
Introduction
| |
The Menzies School of Health Research, in the Northern Territory, has
been a surprisingly successful research investment. The dividends
since 1985 include increased understanding of Aboriginal and
tropical health problems, the transfer of knowledge and skills into
training and improved health services, and some 70 research
publications each year.
The Menzies School is a brave and cooperative venture of the Northern
Territory Government, the Menzies Foundation (commemorating the
name of our longest-serving prime minister), and the University of
Sydney. I was appointed as Foundation Director and we moved to Darwin
in January 1985, in quixotic mood, and not knowing what to expect. My
wife had found a Thomas Keneally quote:
. . . the north is
littered with the detritus of great hopes, and Darwin is still an
outpost . . . but with a sense of destiny that would have done Athens
credit.1
We were naive enough to ignore the implicit warning, and to dream of
Athens in the north.
To Darwin I brought a research background in medicine and
epidemiology; experience from New Guinea, the Walter and Eliza Hall
Institute and Oxford; and 10 years as an NHMRC Fellow at the University
of Melbourne. My first dream for the Menzies School was to establish a
centre of research excellence. The second dream was to somehow make a
difference in Aboriginal health. The potential nightmare was to work
out how to realise each dream without jeopardising the other.
|
The politics of Aboriginal health
| |
Countries with the least education and income tend to have the poorest
health, and within any one country persons with the least education
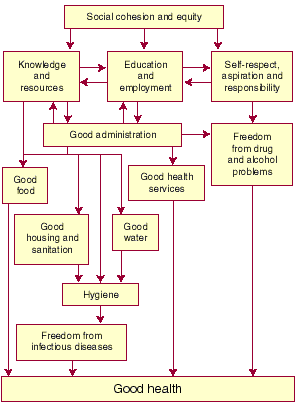
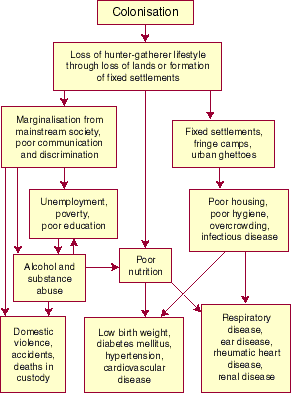
and income tend to have the worst health. Box 1 shows the causal
linkages between education, income and health in any society, and Box
2 shows how the social dislocation suffered by Aboriginal
Australians since colonisation has specifically contributed to
their poor health.2
The poor health of Aboriginal Australians is primarily due to social
and environmental disadvantage. It is not due to any absolute lack of
knowledge about the causes of their ill-health (Box 3), but to the fact
that Aboriginal people have had limited access to health resources
and knowledge because of their own poverty and educational
disadvantage. There has also been limited understanding of
Aboriginal health issues by those responsible for funding
decisions, compounded by inadequate knowledge and training of
health advisers and providers.
Unfortunately, the poor state of Aboriginal health has also been
perpetuated by disagreements about what should be done and how, who
should do it, and who should pay for it. This lack of consensus,
amounting to a modern Babel (Box 4), is only now beginning to be
resolved.
The Menzies School has contributed to the debate on Aboriginal health
by helping to fill gaps in understanding, communication and
implementation. It has attracted expert staff to the Northern
Territory, driven research to identify areas of unmet health need,
tested innovative health interventions, and been an evaluator,
critic and advocate for Aboriginal health policy.
|
Success in interdisciplinary and crosscultural collaboration
| |
The success of the Menzies School has been driven by the quality of our
staff, the challenges faced, and by the added value that comes from
collaboration and communication between diverse disciplines.
Above all, success would have been impossible without the expertise
and commitment of Aboriginal staff and colleagues. Major
contributions have been made by Lorna Fejo, Jessica Bujevich, the
late Sally Ross, Louisa Collins, Daisy Yarmirr, Josie Crawshaw,
Annie Bonson, Geoffrey Angeles, Mai Katona and many others. Their
achievements have been to communicate the health priorities and
values of Aboriginal people to non-Aboriginal researchers, to
facilitate research projects in a culturally appropriate manner,
and to work with other Aboriginal people to show how knowledge and
research findings can be fed back to communities and applied to
achieve practical health benefits. Recently, the Tiwi Health Board
has played a key role in codifying the many sensitive issues that arise
in crosscultural research and providing a framework for future
research in a Legal Agreement signed with the School (Box 5).
|
Some research highlights of medical importance
(See also Box 6) | |
Understanding streptococcal infection and rheumatic fever |
At any one time, up to 60% of Aboriginal children in bush schools have
skin sores infected with group A streptococci, and there are
occasional epidemics of acute poststreptococcal
glomerulonephritis. Bart Currie, Jonathan Carapetis and
colleagues have shown that the same communities suffer from the
highest rates of rheumatic fever in the world. To overcome the limited
awareness of rheumatic fever and the low rates of compliance with
penicillin prophylaxis, Geoffrey Angeles, Norma Benger and other
members of our Aboriginal Unit have developed The Rheumatic Fever
Story, a successful education program (booklets, songs and
videos) for patients, relatives, health workers and the wider
community.
K S Sriprakash, a talented molecular geneticist, has led molecular
studies of group A streptococci, detecting as many as 13
immunologically distinct types present at the same time in a single
bush community of a few hundred children, with a total of about 100
different types circulating through Aboriginal communities in
northern Australia, many that have never been identified elsewhere.
Candidate nephritogenic strains have recently been identified.
This work is linked to studies of the epidemiology and population
biology of group A streptococci in Aboriginal communities, to
studies of treatment efficacy, and to studies directed towards
vaccine development with Michael Good and the Cooperative Research
Centre for Vaccine Technology in Brisbane.
| |
Understanding endemicity of respiratory bacteria |
For Aboriginal children, persistent otitis media is a major cause of
illness, hearing loss and educational disadvantage. Amanda Leach,
Judith Boswell, Terry Nienhuys and others have shown that otitis
media develops in all Aboriginal infants within a few weeks of birth
immediately after nasopharyngeal colonisation with
Streptococcus pneumoniae and Haemophilus
influenzae. Although each infection seems to be eventually
cleared by the host response, there are some 30 different serotypes of
pneumococcus and at least 50 types of haemophilus which can queue up to
infect every child in every community. The persistence of nasal
infection and respiratory disease is associated with the persistent
colonisation by such multiple bacterial strains into adult life.
Cross-infection is driven by overcrowding, poor hygiene and the
large numbers of bacterial strains circulating. Detailed modelling
suggests that each strain is maintained indefinitely, even in
relatively small populations, because there are always a few
carriers of each strain left to infect susceptible newborn infants.
Furthermore, with the carriage of multiple serotypes or strains at
the same time by the same host individual, some of the strains are
"hidden" from the immune system, giving them an extra survival
advantage. Likewise, antibiotic-resistant strains "hide" behind
sensitive strains, only to be revealed by antibiotic treatment.
| |
Understanding scabies in dogs and people |
Skin infections associated with scabies infestation are frequent in
Aboriginal communities, particularly among children. Because dog
scabies was thought to be a source of infection for people, scabies
control programs have sometimes treated dogs rather than people.
Now, using molecular genotyping, Shelley Walton and colleagues have
shown that populations of scabies mites from dogs in Australia and
America do not overlap with scabies from people in those same areas.
This strongly suggests that scabies from dogs are not driving human
scabies in remote communities and that control programs for human
scabies must focus on people. Jonathan Carapetis and Daisy Yarmirr,
in cooperation with Aboriginal and health service colleagues, have
shown that community-based treatment with pyrethrin can reduce both
scabies and streptococcal impetigo.
| |
Understanding renal disease and cardiovascular disease |
Mortality from renal failure for Aboriginal Australians is very high
and rising. Up to 50% of Aboriginal adults have proteinuria
and in some communities 2% are receiving renal dialysis to stay alive.
Paul van Buynder and colleagues identified obesity, hypertension
and non-insulin-dependent diabetes mellitus (NIDDM) as risk
factors for proteinuria in Aboriginal communities. Modelling
studies with Alison Goodfellow and others suggest that proteinuria
develops from very early in life in those with evidence of past
infection with group A streptococci. Wendy Hoy and colleagues have
shown that low birth weight is predictive of NIDDM, proteinuria, and
presumably renal disease, and have suggested that the risk factors
for renal disease can also help to explain the high rates of
cardiovascular disease in Aboriginal adults.
| |
Causes of disease acting from early in life |
The role of low birth weight as a predictor of poor health in later life
has attracted much recent attention, and is of particular importance
for Aboriginal Australians. Wendy Hoy and others have shown that the
combination of low birth weight with adult obesity appears to confer
the highest risk of NIDDM, proteinuria and other disorders. Sue
Sayers has shown that high rates of Aboriginal low birth weight are due
to intrauterine growth retardation, possibly resulting from
maternal malnutrition, infection and substance abuse. Thus, low
birth weight may be best regarded as a marker of those adverse
influences in pregnancy that are the actual mediators of adverse
health effects in later life. This hypothesis would explain how poor
health can pass from generation to generation, and may provide
another reason why health has been slow to improve for many Aboriginal
Australians.
| |
Early treatment of renal disease |
The epidemic of Aboriginal renal disease should eventually be
controllable through public health measures such as improved
nutrition and infection control, particularly in pregnancy. In the
meantime, there is a strong rationale to provide "best-practice"
clinical treatment, not previously available for Aboriginal
people. Accordingly, Wendy Hoy, as an adjunct to the NHMRC-funded
research program, has introduced treatment with ACE inhibitors for
Tiwi people with early renal disease. Compliance is good, and
treatment markedly reduces the rate of deterioration of kidney
function, which will in turn prolong life and reduce the escalating
social and financial costs of dialysis services.
|
The Menzies School's work in central Australia
| |
We have a small research unit in Alice Springs to complement our major
operation in Darwin. Major contributions include those of Tim Rowse
(historical, social and nutritional studies), David Scrimgeour,
Robyn McDermott, Ilan Warchivker and John Wakerman (evaluation
studies), and Komla Tsey (health and education).
|
Research highlights in tropical and international health
| |
David Kemp, FAA, joined the School as Deputy Director in 1992, with
support from the Wellcome Trust and from the Howard Hughes Institute
to continue his fundamental work with falciparum malaria, and to
commence new molecular studies of haemophilus, donovanosis, and
scabies. This year saw the culmination of his 10-year search, begun at
the Walter and Eliza Hall Institute, to find the cytoadherence gene in
Plasmodium falciparum that is believed to explain the
stickiness of red blood cells in cerebral malaria. The new gene,
designated CLAG, was identified and sequenced, and a CLAG knock-out
was shown to have lost the stickiness phenotype. The team has
subsequently identified additional genes, similar to CLAG,
elsewhere in the malaria genome, opening up exciting new
possibilities for treatment or prevention of cerebral malaria.
Other malaria projects in Indonesia are funded by a grant from the
Northern Territory Government to mark the 50th anniversary of
Indonesian independence and a US National Institutes of Health grant
to Nick Anstey, and are being carried out in cooperation with Emiliana
Tjitra and Indonesian colleagues.
|
Resources and links
(See also Box 7) | |
The achievements of the Menzies School have depended on the generous
financial support of the Northern Territory Government and the
Menzies Foundation, competitive grants from the National Health and
Medical Research Council and other agencies in Australia and
overseas, and private and corporate donations. In 1998, the annual
budget was $6 million to support about 100 employees and postgraduate
research students.
The School has also enjoyed the goodwill and cooperation of Territory
Health Services and other arms of government, Aboriginal
communities, medical services and organisations, the National
Heart Foundation and other non-government organisations, the
University of Sydney, the Northern Territory University, and
Flinders University Clinical School at the Royal Darwin Hospital.
The Menzies School became the lead agency in a successful bid to
establish the Cooperative Research Centre for Aboriginal and
Tropical Health in 1997. Through its Board, chaired by Dr Lowitja
O'Donoghue, and with a majority of Aboriginal members, the
Cooperative Research Centre has an agenda to discover and
disseminate knowledge about Aboriginal health problems, to provide
more research and training positions for Aboriginal people and to
facilitate Aboriginal control of the planning and implementation of
health research and health services.
From 1994, the School has taught postgraduate coursework in public
health to help develop skills in the local health workforce. Now, in
partnership with the Northern Territory University, the School is
promoting a broader vision of public health education through a
Faculty of Public Health. This Faculty will continue postgraduate
teaching and promote access to accredited courses at multiple levels
and to short courses to meet the needs of teachers and educators,
administrators, Aboriginal people and others in need of public
health knowledge and expertise.
|
Cooperation is the secret of success
| |
The Menzies School has become a leader in tropical and Aboriginal
health research, not only through the talent and commitment of
individuals, but also because of its capacity to encourage
cooperation between disciplines, and to build and sustain
cooperative partnerships with Aboriginal stakeholders, health
services and governments in northern and central Australia.
This cooperative research paradigm, linking the laboratory with the
clinic and the community, has delivered important understandings
and contributed to more effective strategies for training of health
staff, and to improved health promotion, prevention and treatment
strategies. Despite its short-term opportunity costs, cooperation
in health research pays off in the longer term by helping to translate
modern scientific knowledge into direct community benefit, just as
natural selection has discovered that cooperative processes
provide pay-offs in the longer term in most otherwise competitive
biological and social systems. Indeed, interactions that balance
competition with cooperation turn up in all evolving systems to
achieve a balance between short term returns (efficiency) and longer
term strategic outcomes.
|
Looking ahead
| |
The multidisciplinary focus of the Menzies School of Health Research
has more than justified the vision of its founders by delivering value
for money to its stakeholders and the wider community. However, as the
School faces the new millennium, it needs
- to serve the community with a broad public health perspective while
maintaining the deep biomedical expertise that underpins strategic
research
- to be an academic critic of health policy, while working in
partnership with health services to promote necessary improvements
- to persuade funding agencies to recognise the value of, and to pay the
full opportunity costs of, cooperation and collaboration between
different disciplines and organisations
- to maintain its cohesion, corporate identity, shared values and
vision for the future.
Talent and enthusiasm are always welcome!
|
Acknowledgements
| |
This summary is based on the work of many colleagues to whom I am deeply
indebted. Special thanks to Coralie Mathews, Bart Currie, Dave Kemp
and Lindy Warrell for reviewing the manuscript, and Debra Davis for
its preparation.
|
References
| |
- Keneally T. Outback. Sydney: Coronel Books, 1983.
-
Mathews JD. Historical, social and biological understanding is
needed to improve Aboriginal health. Recent Adv Microbiol
1997; 5: 257-334.
|
Author's details
| |
Menzies School of Health Research, Darwin, NT.
John D Mathews, AM, MD, Professor and Director.
Reprints will not be available from the author. Correspondence:
Professor J D Mathews, Menzies School of Health Research, PO Box
41096, Casuarina, NT 0811
Email: johnATmenzies.su.edu.au
| |
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
|
|