Men's estimates of prostate cancer risk and self-reported rates of screening
Jeanette E Ward, Ann-Maree Hughes, Geoffrey H L Hirst and Lorraine Winchester
For editorial comment, see Stricker & Eisinger
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au/>".
Abstract - Introduction - Methods - Results - Discussion - Acknowledgements - References - Authors' details
- ©MJA1997
Abstract |
Objective: To determine rates of prostate cancer
screening and predictors of men's participation in this screening in
the light of national recommendations against prostate cancer
screening. Design: Community-based study (computer-assisted telephone survey). Setting: Central Sydney Area Health Service. Participants: Randomly selected men aged 40-80 years. Results: 340 men participated (65% response rate). While the true lifetime (0-74 years) risk of developing or dying from prostate cancer is reported to be one in 18 (6%) and one in 65 (1.5%), respectively, 37% of respondents thought that at least one in five men (20%) would develop prostate cancer before the age of 75 years and 11% that one in five (20%) would die from it. Twenty-two per cent of men aged 50 years or over had been screened for prostate cancer within the previous 12 months. Ever worrying about prostate cancer and bothersome urinary symptoms independently predicted the probability of screening within the previous year. Sociodemographic characteristics such as age, occupation and country of birth were not associated with screening. Conclusions: Public health initiatives to discourage prostate cancer screening should focus particularly on men with bothersome urinary symptoms and those who worry about prostate cancer. Accurate information about the low risks of dying from prostate cancer needs to be communicated, and the speculative nature of current evidence in support of screening as a means of reducing this risk should be emphasised. |
Introduction |
Despite repeated advice to the contrary, screening for prostate
cancer is being requested by patients and conducted by doctors.
Advice against screening has come from a policy statement for health
professionals released in 1995 by the Australian Cancer Society,1 and a 1996 report of a
multidisciplinary committee convened by the Australian Health
Technology Advisory Committee on the basis that the evidence did not
meet accepted criteria for benefits, risks and costs.2 In addition, the National
Health and Medical Research Council (NHMRC) evidence-based
guidelines for the management of men with uncomplicated lower
urinary tract symptoms (LUTS)3
state that there is no evidence that prostate specific antigen
(PSA) tests are required for men with uncomplicated LUTS as men with
these symptoms are at no greater risk of prostate cancer than
asymptomatic men.4 Data indicating that screening is occurring come from the Department of Veterans' Affairs,5 as well as surveys of urologists6 and general practitioners (unpublished data). In describing this "conundrum", Horner identified a pressing need for research to support educational programs for men, focusing on "strategies to combat uninformed patient demand".7 While the Australian Health Technology Advisory Committee guidelines advocate national action involving the NHMRC,2 the need for health services to intervene actively at a local level to discourage prostate cancer screening has also been recognised in New South Wales.8 In the absence of more recent data, we used the opportunity of a large population-based study about men's health to determine the prevalence and predictors of participation in screening for prostate cancer in the area defined by the Central Sydney Area Health Service. |
Methods | The study was approved by the Royal Prince Alfred Hospital Ethics Review Committee. |
Community sampling | Two thousand names, addresses and telephone numbers within the 35 postcodes constituting the Central Sydney area were randomly selected from the Electronic White Pages.9 To maximise participation rates, each household received a one-page letter outlining the Men's Health Study and anticipating telephone contact, supported by a media release to further publicise the study. The initial sample size of 2000 was estimated to be sufficient to provide between 250-350 completed surveys given an estimated prevalence of 38%10 of eligible male respondents in contacted households and a conservative consent rate. |
Computer-assisted telephone interview survey |
A market research company with computer-assisted telephone
interview facilities contacted all 2000 households between 26
November and 12 December 1996 on weekdays between 1500 and 2100. Where
the first contact was unsuccessful, a further five attempts were made
at different times and on different days. Men aged between 40 and 80
years residing in the household and fluent in English were eligible to
participate. If there was more than one man in the household meeting
these criteria, the one with the most recent birthday was asked to
participate.
Due to the sensitive nature of the survey, all telephone interviewers were mature females with previous experience in conducting health-related surveys. A briefing session for interviewers was conducted to address potential difficulties with medical jargon, to ensure sensitivity towards the issues and to standardise the interviews. |
Survey instrument |
At the beginning of the interview, respondents were asked standard
sociodemographic questions, as well as whether they had ever been
diagnosed with a urological condition and questions modified from
the International Prostate Symptom Score11 to assess the presence of and
degree of "bother" attributable to urinary symptoms.
We then asked respondents five questions about prostate cancer. 1. "Have you ever worried that you might have prostate cancer?" Those answering "yes" were asked "For what reasons?". 2. "Have you had any test to detect prostate cancer in the last 12 months?" Those answering "yes" were asked to name the test(s). 3. "Have you heard of any tests for prostate cancer?" 4. "Out of 100 Australian men, how many or what percentage do you think will get prostate cancer before the age of 75?" If the respondent was unable to quantify his response, the interviewer was instructed to establish a range by saying "Would it be more or less than 1%? Less than 5%? Between 5% and 9%? More than 10% or more than 20%?" until an answer was given. 5. "Out of 100 Australian men, how many or what percentage do you think will die from prostate cancer before the age of 75?" If necessary, an answer to this question was prompted in the same way as Question 4. For Questions 4 and 5, interviewers were unaware of the correct answers. Questions 4 and 5 were modelled on previous research. 12 |
Data analysis | Data were analysed using SAS13 and Epi Info.14 We used chi-squared tests to examine associations between knowledge of prostate cancer screening tests and eight respondent characteristics: age (40-49, 50-59, 60-69, 70-80 years); country of birth (Australia v. other); socioeconomic status based on occupation (manager/ administrator and professional/para-professional combined v. all other categories [tradesperson/clerk/salesperson and personal service worker/plant and machine operator/driver and labourer]);15 education (up to and including Intermediate or School Certificate [Year 10] v. Leaving or Higher School Certificate [Year 11 or 12] and beyond); moderate or severe "bother" from urinary symptoms (a score equal to or greater than six from a possible range of 0-18); ever worrying about prostate cancer (yes v. no); estimate of risk of developing prostate cancer (correct or lower estimate v. overestimate); and estimate of risk of death from prostate cancer (correct or lower estimate v. overestimate). Jelfs et al. report a lifetime risk of developing prostate cancer of one in 18 (6%).16 We considered an estimate of 10% or greater to be an overestimate of incidence risk. Using the Jelfs data,16 we calculated the lifetime risk of dying of prostate cancer as one in 65 (1.5%). We considered an estimate of 5% or greater as an overestimate of mortality risk. For the sample of men 50 years and over, we used chi-squared tests to determine associations between the outcome variable -- having had either a prostate specific antigen test, a digital rectal examination, or both, within the previous 12 months -- and these eight variables as well as knowledge of prostate cancer tests. Logistic regression analysis was performed, using significant univariate variables and any plausible non-significant variable. |
Results | |
Response rate and characteristics of the sample | Of 2000 randomly selected households, 1481 (74%) were ineligible. Of the remaining 519 households with an eligible male resident, 340 agreed (65% response rate). Men who refused were significantly older than those who participated (t27.49 = 4.19; P < 0.01). Compared with 1991 Census data12 (Box 1), the sample under-represented older men. No respondent indicated a past history of prostate cancer. |
Respondents' worry about prostate cancer, estimates of risk and knowledge of tests |
Ninety-nine men (29%) indicated they had ever worried about prostate
cancer. The three most frequently cited reasons were: presence of
urinary symptoms (36 men [11%]), age (26 men [8%]), and media
publicity (24 men [7%]).
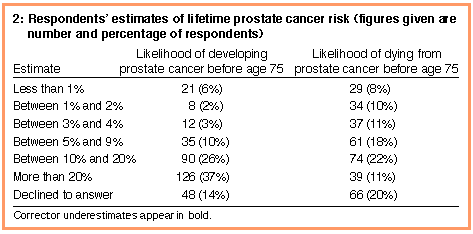
Of the sample, 216 men (63%) overestimated lifetime risk of developing prostate cancer (Box 2). Respondents were significantly more likely to overestimate the risk of death from prostate cancer than the risk of developing it (McNemar's test, 10.800; df = 1; P = 0.001). Ever having worried about prostate cancer was not associated with correctly estimating the risk of developing it or the risk of dying from it. Of the total sample, 237 (70%) and 228 (67%) required no prompting to estimate lifetime risk of developing or dying from prostate cancer, respectively. |
| |
| One hundred and seventy-two men (51%) reported they had heard of one or more tests for prostate cancer. Respondents who had heard of any test were more likely to be managers or professionals than to have other occupations (chi-squared = 4.04; df = 1; P = 0.044) or were educated to Year 12 or beyond (chi-squared = 5.49; df = 1; P = 0.019). Knowledge of tests was unrelated to age, country of birth, perception of risk, "bother" from urinary symptoms or anxiety. | |
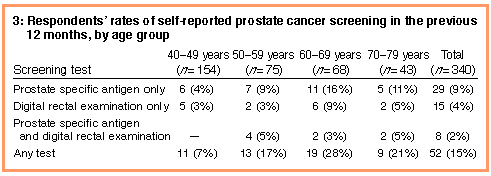
Rates and predictors of prostate cancer screening within the previous 12 months | Of the total sample, 52 men (15%) had had at least one prostate cancer screening test within the previous 12 months (Box 3). Almost all tests (97%) were reported by men 50 years or older, yielding an annual screening rate of 22% for this older group. For the subsample of 186 men aged 50 years or over, univariate analyses revealed only two variables to be significantly associated with having had a prostate cancer screening test within the past year: moderate or severe "bother" from urinary symptoms (chi-squared = 13.41; df = 1; P < 0.001), and "ever worrying" about prostate cancer (chi-squared = 18.38; df = 1; P < 0.001). |
 | |
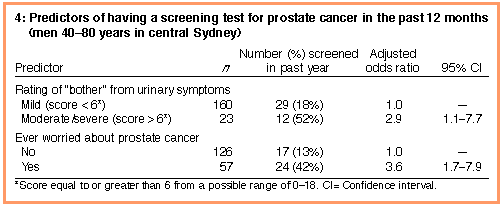
| Knowledge of available tests and other sociodemographic variables were not associated with having had a test within the past year. However, as age was a potential confounder, it was included with the two significant univariate associations in the logistic regression analysis. After adjustment, "bother" and "anxiety" remained independent predictors (Box 4). | |
 | |
Discussion |
Just over one in five of the men in our study 50 years or over had had a
prostate cancer screening test within the previous 12 months, a rate
almost double that given in an earlier report of national claims data.5 Screening was
significantly more likely among those who had ever worried about
prostate cancer or were bothered by urinary symptoms. In contrast to
research in other countries demonstrating that economic and ethnic
factors influence participation in prostate cancer screening,17,18 our study showed no
association between screening and men's occupation, education or
country of birth.
As a priority for public campaigns, men who experience uncomplicated LUTS -- nocturia, frequency, dribbling, urgency, hesitancy or reduced stream -- in the absence of haematuria need to be reassured that there is no empirical evidence of a relationship between such symptoms and early prostate cancer.3 Men's anxiety about prostate cancer may also be explained, in part, by their overestimation of the actual risks of prostate cancer. More than a third of respondents thought that at least one in five men would develop prostate cancer before the age of 74 years, and 11% thought that one in five would actually die from this disease before that age. Reasons for consistent overestimation of risk remain speculative but might reflect extensive media coverage of prostate cancer, possibly fuelled by commercial interests, which increases men's anxiety, and, in turn, raises their perception of risk.19 In contrast, McCormick20 has argued that informed public participation in screening should be founded on clear messages about absolute risk, the evidence from rigorous randomised trials for reduction in risk, the costs and adverse outcomes. Our study is the first to quantify a considerable gap between men's perceptions of risk and the actual risk. When provided with impartial information on an individual basis about the risks and unknown benefits of prostate cancer screening, men are less inclined to have a screening test.21 Given our collective failure to convey accurate health risk information to the public about risks for other cancers,9 risk reduction22 or screening,23 a systematic approach to the development, implementation and evaluation of a public health initiative to discourage prostate cancer screening is required. The recent release of the guidelines for the management of uncomplicated LUTS in men3 provides a focus for such an initiative. Our study suggests that men who are anxious about prostate cancer or have bothersome urinary symptoms represent priority target groups for educational messages via general practice, men's service and recreation clubs, mass media and peak groups such as the Council of the Ageing and the Consumers' Health Forum. Because of the limitations of our study, we also recommend that a dedicated survey about prostate cancer be conducted which examines in depth men's knowledge of indolent and aggressive cancer types, their health beliefs and attitudes towards early detection, their awareness of the speculative and controversial nature of screening, and their knowledge of treatment options and their effectiveness. Men's recall of the recommendations of their GP in either promoting or discouraging prostate cancer screening could also be ascertained. As female partners represent a key source of health information for men,24 a concurrent survey of partners of men in these age groups is also recommended. |
Acknowledgements | The Men's Health Study was conducted for the NHMRC Working Party developing guidelines for the management of lower urinary tract symptoms in men with funds from the Commonwealth Department of Health and Family Services. We thank members of the Working Party for comments on survey protocols; the men who participated in the computer-assisted telephone interview and the Hunter Valley Research Foundation for diligent administration of the survey; Jo Williams and the Central Sydney Area Health Service Public Relations Unit for assisting with the media release; and Neil Donnelly for statistical advice. |
References |
Subsequently cited in Prostate-specific antigen testing in Australia and association with prostate cancer incidence in New South Wales by David P Smith and Bruce K Armstrong, Med J Aust 1998; 169: 17-20 |
Authors' details
Central Sydney Area Health Service, Needs Assessment & Health Outcomes Unit, Sydney, NSW.Jeanette E Ward, PhD, FAFPHM, Director;
Ann-Maree Hughes, BEd, GradDipAppSci(Nursing), Research Assistant;
Lorraine Winchester, BSocSc(Hons), Data Manager.
Taylor Medical Centre, Brisbane, QLD.
Geoffrey H L Hirst, MB BS, FRACS, Urologist.
Reprints: Associate Professor J E Ward, Central Sydney Area
Health Service, Needs Assessment & Health Outcomes Unit, PO Box 374,
Camperdown, NSW 2050.
E-mail: jward AT nah.rpa.cs.nsw.gov.au
©MJA 1997
<URL: http://www.mja.com.au/> © 1997 Medical Journal of Australia.
Received 25 May 2026, accepted 25 May 2026
- Jeanette E Ward
- Anne-Maree Hughes
- Lorraine Winchester




