The Hobart Salt Study 1995: few meet national sodium intake target
Trevor C Beard, David R Woodward, Peter J Ball, Helen Hornsby, Richard J von Witt and Terence Dwyer
MJA 1997; 166: 404
For editorial comment see Beilin
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au/>".
Abstract - Introduction - Methods - Statistical analysis - Results - Sodium and potassium excretion - Discretionary use of salt - Discussion - Public health implications - Conclusion - Acknowledgements - References - Authors' details
- - ©MJA1997
Abstract |
Objective: To estimate 24-hour sodium and potassium
excretion in an urban Australian population. Design and setting: Cross-sectional survey of an urban population in Hobart, Tasmania, in 1995. Participants: Systematic sample (87 men, 107 women) from the Commonwealth Electoral Roll of people aged 18-70 years on 30 June 1995 whose residential address was within 10 km of the Hobart General Post Office. Main outcome measure: Conformity with the national target for sodium intake for the year 2000 of ≤100 mmol/day. Results: The target was met by 6% of men and 36% of women. This difference between the sexes was significant ( P < 0.001), while differences between age groups and socioeconomic levels were not significant. Conclusion: Our findings confirm the low level of conformity with the national sodium target reported by the handful of Australian studies over the past decade. Given the major community costs associated with hypertension, our results highlight the need for effective and properly monitored action to reduce sodium intakes. |
Introduction |
Many health problems are associated with the current sodium intake of
people in Western societies.1
In 1988, an Australian target for a lower sodium intake was set
for the express purpose of reducing the prevalence of hypertension.2 Although other factors,
such as excess body weight, inadequate exercise, excess alcohol, low
dietary potassium and "psychological influences", may contribute
to hypertension,3
Australia's national target for sodium intake (≤100 mmol/day)2 is accepted internationally.4-6 Further, it is supported
by the discovery that the usual human salt intake in Western diets
induces hypertension in chimpanzees, and that this is reversed when
they return to their natural diet.7
The effect of low dietary potassium on health has received less attention, but there is good evidence that potassium intake should at least equal sodium intake in molar units.8,9 Potassium predominates in unsalted foods because it is the major intracellular cation in the living tissues of both plants and animals. Thus, virtually all the natural foods available to mammals have a molar sodium to potassium ratio of less than 1.0. The human body must have evolved on this dietary ratio; its inversion is recent in phylogenetic terms, unnecessary and probably unsafe.8,9 Published data on current intakes of sodium and potassium among Australians are very few, and usually based on small samples10-12 We report electrolyte excretion data obtained from 194 Hobart residents for a behavioural study in 1995. Our estimates are based on 24-hour excretion of these electrolytes in the urine (widely accepted as the preferred method of assessment of intake).13,14 |
Methods |
People aged 18-70 years on 30 June 1995 and residing within 10 km of the
Hobart General Post Office were selected from the Commonwealth
Electoral Roll (revised to February 1995) as follows. Every 500th
person on the roll was selected for contact or, if ineligible,
replaced by the next eligible person. A letter inviting
participation was mailed to each person, outlining the study
(including the need to attend for interview and to provide a 24-hour
urine sample) and enclosing a reply-paid envelope. Those failing to
reply were sent a second letter two weeks later, followed, if
necessary, by a telephone call within a further 10 days.
Unpredictable variability in sodium excretion (a confounder in the behavioural study) was reduced by excluding volunteers with serious intercurrent illness, pregnancy, breast-feeding or use of potassium supplements, diuretics or other drugs likely to affect sodium excretion. We estimated socioeconomic status by the postcode of the participant's address, using the Index of Relative Socioeconomic Disadvantage (IRSD);15 data for specific postcodes were supplied by the Australian Bureau of Statistics. Suburbs whose postcodes had an IRSD ≤ 1000 (the national mean score) were classified as "lower socio economic status", and those with an IRSD ≥ 1000 as "higher socioeconomic status". Two subjects listed a GPO box address and were not assigned a socio economic status rating. At interview, we collected demographic and anthropometric data and a short medical history. Participants completed a food-frequency questionnaire and answered behavioural and cognitive questions, which will be reported elsewhere. Each participant received detailed verbal and written instructions on how to make a complete 24-hour collection of urine; all were asked to collect urine on weekdays, and women of reproductive age were asked to avoid collection during the premenstrual week, when sodium retention may occur.16 Participants collected urine in 2 L plastic containers containing 20 mL of 6 molar hydrochloric acid and returned them promptly. Urine volume was estimated by weighing. For 82 of the 194 samples the estimated volume was adjusted to 24 hours because of longer or shorter actual collection times; the maximum adjustment was 175 minutes over the 24 hours (12.2%), and only five adjustments exceeded 5%. The samples, identified only by code numbers, were diluted with neutral pH buffer and analysed for sodium and potassium by ion-selective electrodes on a Kodak Ektachem 750 XRC analyser (Johnson & Johnson Clinical Diagnostics, Rochester, NY, USA) and, for creatinine, by the Ektachem method also. Laboratory results were sent to those participants who requested them. A duplicate of every tenth sample was sent for analysis under a different code number for quality assurance. We calculated imprecision of laboratory measurements from the differences between results for duplicate samples using the formula published for the Intersalt study.17 The coefficients of variation for laboratory imprecision were 0.6% for sodium, 1.1% for potassium and 5.4% for creatinine. The protocol was approved by the University of Tasmania Committee on Ethical Aspects of Human Experimentation, and all subjects gave written informed consent. |
Statistical analysis | We used SPSS18 to analyse the data; P< 0.05 was used as the criterion of statistical significance. Differences between sexes, age groups and socioeconomic status levels were assessed by t tests (for mean sodium and potassium excretion rates) and by chi-squared tests (for compliance with targets for sodium and sodium to potassium ratio). |
Results |
Of 619 individuals originally selected, 167 (27%) were
uncontactable despite active follow-up, 80 (13%) were ineligible
because they had moved out of the target area, 151 (24%) declined to
take part, 18 (3%) were eliminated by our exclusion criteria (nine for
medications, five for illness, and four for pregnancy or lactation),
and nine participated incompletely. The remaining 194 (31% of the
initial sample, or 52% of those known to be eligible) were interviewed
and provided a 24-hour urine collection.
Box 1 (below) compares sociodemographic characteristics for these 194 participants with those of the other 425 people originally selected. The two groups had a similar sex distribution, but participants were significantly older and had higher socioeconomic status. For participants, the sex ratio was similar in both age divisions (43% men in the 18-44 years group and 46% men in the 45-70 years group), and in both socioeconomic groups (47% and 44% men in the lower and higher socioeconomic status groups, respectively). While we do not have birthplace data for the non-participants, most participants were born in Australia (83%) or in the United Kingdom or Ireland (12%). |
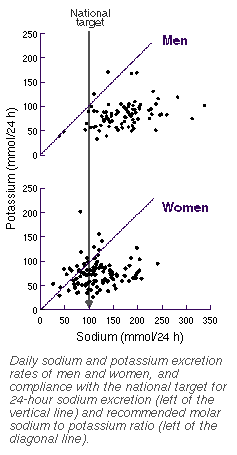
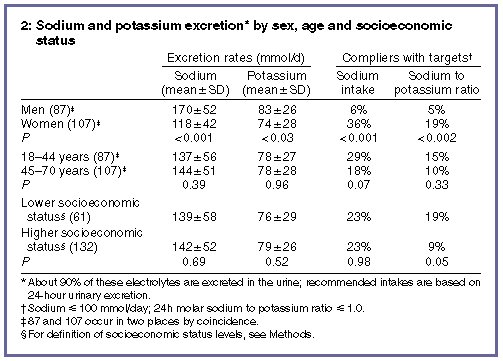
Sodium and potassium excretion | Twenty-four-hour sodium excretion was greater in men (range, 39-337 mmol) than in women (26-241 mmol), and the mean sodium intake (as reflected by this excretion rate) was 52 mmol higher in men than in women, a highly significant difference (P< 0.001). Only 6% of men, compared with 36% of women, met the Australian national target (≤ 100 mmol/day), represented by the vertical line in the Figure, and this difference was also significant at P< 0.001. Differences between age groups and socioeconomic status groups were not significant at the P< 0.05 level (Box 2, below). |
 | |
|
The mean potassium intake in men was 9 mmol higher than in women (P = 0.03), but differences between age groups and socioeconomic
status groups were not significant (Box 2, above). Only 5% of men and 19% of
women met the recommendation8,9
that the sodium to potassium ratio should not exceed 1.0
(diagonal line in the Figure); this sex difference was significant (P = 0.002). Differences were not statistically significant
between younger and older participants (P = 0.33), and were on
the margin of significance for socioeconomic status levels (P = 0.05). | |
Discretionary use | Most of our 194 participants claimed that they never or rarely added salt at the table (51% of men and 73% of women), and that they never or rarely cooked with salt (54% of men and 61% of women). Compliers and non-compliers with the sodium target gave similar answers about the use of salt: 66% of compliers and 62% of non-compliers rarely or never added salt at the table, and 57% of compliers and 58% of non-compliers rarely or never cooked with salt. |
Discussion |
Despite our relatively low response rate, Box 1 shows that our
participants had a similar sex ratio to that of a systematic sample
from the Hobart electoral roll, and we found that sex differences in
electrolyte excretion were significant. Although our sample was
biased in terms of age and socioeconomic status, the effect of age and
socioeconomic status on electrolyte excretion in the participants
barely reached significance (Box 2), and hence these biases are
unlikely to have influenced our findings. If the participants were
unrepresentative in some other way -- more health-conscious, for
example -- our data could underestimate sodium excretion and
overestimate compliance with the sodium target.
It is difficult to be certain of the completeness of 24-hour urine collections. Para-aminobenzoic acid has been used as a marker in overseas studies,19 but is not approved for use with healthy volunteers in Australia. Creatinine excretion is a customary indicator of completeness, but no standard cut-off points exist.19 As both undercollection and overcollection could have affected our results, we repeated the t-test analyses of Box 2 after excluding subjects whose creatinine outputs were in the lowest and highest 2.5% for men and women. For both sodium and potassium the changes in means and standard deviations were negligible, indicating no serious problem with outliers. Moreover, the range of excretion rates of each electrolyte in each sex remained unaltered. Accuracy and imprecision of assays are also important determinants of data quality. As reported in our Methods, duplicate assays indicated acceptable imprecision -- the laboratory is a participant in the Royal College of Pathologists of Australasia-Australian Association of Clinical Biochemists Quality Assurance Scheme and is accredited by the National Association of Testing Authorities. Few other Australian studies have been reported. In one, estimates based on food-frequency questionnaires were somewhat lower than ours,12 but urinary excretion is considered a more valid indicator of intakes.13,14 A Hobart study in 1989, with a similar protocol for sample selection and urine collection,10 found mean sodium and potassium excretion rates in men of 160 mmol/day and 77 mmol/day, respectively, compared with 124 mmol/day and 66 mmol/day in women. In Sydney, in 1992, Notowidjojo and Truswell11 found mean sodium and potassium excretion rates of 164 mmol/day and 74 mmol/day in men and 133 mmol/day and 66 mmol/day in women. These two studies support our conclusion that average intakes in Australia -- especially among men -- are substantially above the national target. |
Public health implications |
Meta-analysis by Law et al. indicates that a 50 mmol decrease in
community sodium intake could reduce mortality from heart disease by
16% and from stroke by 22%.20
The annual cost to Australia of heart disease, stroke and
hypertension was recently estimated at $1198 million, $666 million
and $546 million, respectively.21
If a lower salt intake reduced prevalence as much as it reduced
mortality, the saving from 16% less heart disease and 22% less stroke
and hypertension would be $458 million annually, with added savings
from reduced prevalence of other conditions.1 In the United Kingdom the complete elimination of table salt and cooking salt would reduce mean sodium intake by only about 15%.22 This figure might be even lower in Australia, as this and other studies show that most people already avoid adding salt to their food.23,24 The main source of dietary sodium -- at least 75% of the total -- is processed foods, and a major reduction depends on changing their composition.21 Government initiatives have been limited to recommending a lower salt content in processed foods,25 setting a national target for sodium intake of ≤100 mmol/day,2 and publishing the dietary guideline Choose low salt foods and use salt sparingly.26 Food manufacturers have made some commendable initiatives, but they depend on consumer demand, and little has been done to inform the public about the national target for sodium intake. Although some low-salt processed foods are available and labelled in accordance with the food regulations, shoppers receive little specific advice or encouragement to reduce their sodium intake by choosing them. |
Conclusion | By setting a national sodium-intake target, Australian health authorities have accepted that excessive dietary sodium is an important health issue, with significant morbidity, mortality and economic costs. Our results indicate the need for an active campaign to promote and monitor the nation's sodium target effectively. |
Acknowledgements | This study was carried out with an educational grant from the National Heart Foundation of Australia, and financial assistance towards the purchase of computer equipment was received from Sizzler Restaurants and from Salt Skip Incorporated. We are indebted to Leigh Blizzard, statistician at the Menzies Centre, for statistical advice. |
References |
(Received 24 Jun, accepted 4 Nov, 1996) |
Authors' details
Menzies Centre for Population Health Research, University of Tasmania, Hobart, TAS.Trevor C Beard, OBE, MB BChir, MPH, Senior Research Fellow; Helen Hornsby, BA(Hons), Research Assistant; Terence Dwyer, MD, MPH, Director.
Division of Biochemistry, University of Tasmania, Hobart, TAS.
David R Woodward, PhD, Senior Lecturer.
Department of Psychology, University of Tasmania, Hobart, TAS.
Peter J Ball, BSc, MA, Senior Lecturer.
Department of Clinical Chemistry, Royal Hobart Hospital, Hobart,
TAS.
Richard J von Witt, FRCPath, FRCPA, Director.
Reprints: Dr T C Beard, Menzies Centre for Population Health Research, 17 Liverpool Street, Hobart, TAS 7000.
©MJA 1997
<URL: http://www.mja.com.au/>
© 1997 Medical Journal of Australia.
Received 10 June 2026, accepted 10 June 2026
- Trevor C Beard
- David R Woodward
- Peter J Ball
- Helen Hornsby
- Terence Dwyer