Treatment decision-making at the end of life: a survey of Australian doctors' attitudes towards patients' wishes and euthanasia
Charles Waddell, Roger M Clarnette, Michael Smith, Lynn Oldham and Allan Kellehear
MJA 1996; 165: 540
For editorial comment, see Hassan
Readers may print a single copy for personal use. No further reproduction or distribution of the articles in whole or in part should proceed without the permission of the publisher. For copyright permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au/>".
Abstract - Introduction - Methods - Survey participants - Questionnaire - Statistical analysis - Results - Case scenarios 1 and 2 - Case scenario 3 - Case scenario 4 - Responses to request for assisted death - Factors influencing choice of treatment - Factors influencing doctors' responses to patient's request for assisted death - Discussion - Acknowledgements - References - Authors' details
- - ©MJA1996
Abstract Objective: To examine factors that influence medical practitioners' treatment decisions for patients with life-threatening or terminal illnesses.
Design: Postal survey, conducted between September and November 1995, of a self-administered questionnaire, describing four clinical case scenarios, to a random sample of 2172 Australian doctors in all States and Territories. Respondents were asked to prescribe treatment for the patients described in the scenarios. Patients' characteristics varied in terms of mental competence, illness severity, prognosis, the presence of advance directives, request for assisted death, and sociodemographic factors. The respondents' sociodemographic and medical training characteristics were also obtained.
Setting: Random national sample of all active medical practitioners.
Participants: Hospital trainees, general practitioners, physicians, palliative care practitioners and surgeons were surveyed. A response rate of 73% was achieved.
Main outcome measures: Frequency of prescription of supportive, acute or intensive treatment for patients in the four clinical scenarios based on respondents' sex, religion, medical training and country of medical degree.
Results: Three main findings were: (i) doctors did not make consistent decisions, but their decisions varied systematically by sociodemographic and medical training factors; (ii) doctors generally adhered to patient and family wishes when these were known; (iii) doctors did not generally adhere to a patient's request for assisted death.
Conclusion: Treatment provided is significantly determined by the individual characteristics of the doctor and not solely by the nature of the medical problem. Participation in the informed-consent process and in the preparation of advance health care directives would enable practitioners to be familiar with patient and family wishes and could reduce variations of treatment related to sociodemographic and medical training factors. Stronger empirical data on the way that treatment decisions are made could provide the basis for an informed euthanasia policy.
MJA 1996; 165: 540-544
Introduction
Advances in medical technology have allowed the medical profession to maintain life to an extent that is beyond the limits of what many would consider reasonable quality. 1-5 The use of advanced technology, particularly for terminal illnesses, has created a complex array of ethical, moral and legal issues, 6-8 and has been accompanied by opportunities for greater patient participation in treatment decision-making and individual involvement in choosing care. 1,3,4,8 The most contentious aspect of these developments seems to be the promotion of requests for physician-assisted death -- euthanasia. 1,6,9 However, the emphasis on euthanasia has been tempered by a greater focus on palliative-care principles in the management of patients with terminal and life-threatening illnesses. 10-12A major impediment to the consideration of these issues is the lack of strong empirical data to indicate the way in which treatment decisions are reached. The process that leads to decision-making and action in clinical practice is unclear, and the factors that determine who ultimately makes a treatment decision, what influences treatment choice, and how the treatment is carried out have yet to be established. Although the idea of informed consent implies significant patient participation in decision-making, there is no evidence that such participation actually occurs. Indeed, many patients are incapable of giving informed consent. Doctors and family members usually make decisions in such circumstances, but the path for this process is unknown. Some authors have advocated the use of advance health care directives that can advise doctors of a patient's wishes regarding care should he or she become incompetent. 2
Several studies, surveying both the general public and health professionals, have examined areas relevant to these issues, including reactions of family members to the death of loved ones; 8,10,13 attitudes of doctors to death, dying 1-5 and palliative care; 12,14 doctors' experience with requests for euthanasia; 1,9,15 and factors that influence doctors' choice of treatment. 1-5,7 However, while many of these reports discuss the legal, ethical, medical and philosophical problems confronting health professionals, they do not address the factors that influence the health professionals to act as they do.
To examine the factors that influence doctors' decisions on treatment for patients with life-threatening or terminal illnesses, we presented doctors with actual comprehensive clinical scenarios described in a questionnaire and asked them to state what they would do.
Methods
Survey participants
A postal survey was conducted between September and November 1995. An
initial mailing of the questionnaire was sent to a national sample of
2016 doctors with a workload of 50 or more services (i.e., items billed
to Medicare) per quarter, randomly selected by the Health Benefits
Division of the then Commonwealth Department of Human Services and
Health. The questionnaire was also posted to all Australian
palliative care practitioners registered with the Australian and
New Zealand Society of Palliative Medicine ( n = 156).
Each practitioner was asked to complete and return the questionnaire anonymously. After two weeks, a reminder card was sent to all in the sample. Of the 2172 posted, 1588 usable questionnaires were returned (3% trainees [interns, residents, registrars]; 41% general practitioners; 10% palliative care practitioners; 46% specialists). The response rate, 73.1%, compared favourably with that of Baume and O'Malley (76.1%). 9 Eighty-seven questionnaires were returned because they were incorrectly addressed.
Questionnaire The questionnaire was based upon that used by Molloy and colleagues 2 in Canada. We adapted their case scenarios to the 1995 Australian context, particularly including the issue of physician-assisted death. The questionnaire presented scenarios based on clinical cases (see Box 1). The doctors were asked to choose one of three treatment options in each scenario:
1. Supportive care -- keep warm, dry and pain-free; use only those measures that enhance comfort or minimise pain; start intravenous line only if it improves comfort; perform no x-rays or blood tests and give no antibiotics unless such measures are intended only to improve comfort;
2. Acute care -- may involve transfer to acute-care facility; perform emergency surgery if necessary; do not ventilate (except during and after surgery); carry out all acute-care interventions, except for admission to the intensive care unit or the coronary care unit and performing organ transplantation;
3. Intensive care -- all possible interventions necessary to maintain life.
The doctors were also asked how they would respond to a patient's request for assisted death (scenario 4). Three possible responses were listed:
1. Refuse request for assisted death, and explain and provide palliative (supportive) care only;
2. Agree to assist death by providing the means (e.g., by prescribing lethal medication); and
3. Agree to assist death by active intervention (e.g., by administering a fatal dose of narcotic analgesic).
To assess the degree to which six independent variables -- legal, ethical, religious and economic factors and patient's and family's wishes -- influenced the choice of treatment, the doctors were asked to complete a five-point Likert-type scale following each scenario.
Finally, the questionnaire addressed the sociodemographic characteristics (sex; religious background) and the training of the participating doctors (country of basic medical degree; number of years qualified; level of medical training). The study was approved by the Human Rights Committee, the University of Western Australia.
Statistical analysis
Our analysis cross-tabulated the aggregated responses to the treatment options of the four clinical scenarios with the sociodemographic and medical training factors to examine whether medical decision-making varied significantly depending on these factors. Statistical significance was tested by chi-squared tests, with exact probability levels being reported. 16 We examined the strength and direction of the relationships among treatment options for the four clinical scenarios and the six independent variables. Somers' d correlation matrix is presented with chi-squared levels of statistical significance of 0.01 and 0.001. 16 Stepwise regression analysis was used to assess the degree of variance explained by the six independent variables in the doctors' responses to the request for physician-assisted death.
Results
Case scenarios 1 and 2
In the 80-year-old incompetent woman with life-threatening and
acute illnesses without the medical directive (Box 2, scenario 1),
there were significant differences among doctors' choices by all
sociodemographic and medical training factors, except for
religion. In the 80-year-old incompetent woman with
life-threatening and acute illnesses with a medical directive for
acute treatment (Box 2, scenario 2), there were significant
differences by religion and medical training factors, but no
significant difference between male and female doctors. This woman
was twice as likely to receive acute care than was the woman without a
medical directive.
Case scenario 3
In their treatment choices for the 33-year-old competent woman with
terminal and acute illnesses insisting on intensive care, there were
significant differences among the doctors by medical training
factors but not by sociodemographic factors (see Box 2). Doctors from
non-Western countries were more likely to honour the patient's
request for intensive care than were Western-trained
practitioners; however, most doctors chose acute care for this
patient. Older doctors and those not trained in palliative care were
also more likely to honour the patient's request for intensive care.
Case scenario 4
Nearly all doctors (more than 93%) chose supportive care for the
treatment of the 56-year-old competent man with motor neurone
disease who requested physician-assisted death. The only
significant difference was between doctors trained in Western and
non-Western countries, with a greater percentage of the latter
choosing more interventionist medical treatment.
Responses to request for assisted death
Box 2 shows three notable findings on the doctors' responses to the
request for assisted death:
1. Most doctors reported that they would provide palliative care only to this patient (explaining the grounds for the decision);
2. The percentage of doctors who were willing to provide only the means to assist death was larger than the percentage who were willing to intervene actively to assist death (frequently referred to as active euthanasia);
3. Female, Catholic, Western-trained and older doctors, as well as palliative care practitioners, were the least willing to engage in any form of euthanasia; agnostic/atheist doctors were the most willing to engage in some form of euthanasia; and doctors trained in non-Western countries were more likely than Western-trained doctors to be willing to provide the means to assist death, but were less likely than Western-trained doctors to actively intervene to assist death. Factors influencing choice of treatment Box 3 presents the Somers' d correlation matrix for scenario treatments with factors influencing treatment choice. For the incompetent 80-year-old woman without the medical directive (scenario 1), legal and ethical factors showed a significant positive correlation with the treatment choice, whereas the patient's and the family's wishes had a significant negative correlation with treatment choice. For the incompetent 80-year-old woman with a medical directive (scenario 2), cost and the patient's and family's wishes were significantly related to the treatment choice, the latter two of these three independent variables being positively associated with treatment choice.
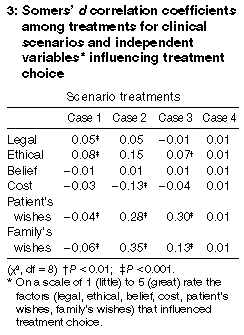
For the 33-year-old competent woman insisting on intensive treatment (scenario 3), ethics and the patient's and family's wishes had a significant relation to treatment choice. For the 56-year-old man with motor neurone disease who requested assisted death (scenario 4), none of the factors examined were significantly related to treatment choice.
Across the matrix, patient's wishes seemed to have a significant positive relationship with doctors' treatment choice in scenarios 2 and 3, but not in scenario 1 (patient's wishes not known) or in scenario 4 (the patient who requested assisted death). This pattern of correlation suggests face validity for this set of questions. It should be noted that, while some coefficients are statistically significant, they do not suggest strong relationships between the variables.
Factors influencing doctors' responses to patient's request for assisted death Stepwise regression analysis of the six independent variables that influenced the doctors' responses to the patient's request for assisted death showed three of these variables to be significant: patient's wishes (F = 67.0; P < 0.001), ethical factors (F = 38.8; P < 0.001) and religious beliefs (F = 27.2; P < 0.001). However, together, these three variables still explained only seven per cent of the variance in doctors' responses to the patient's request for assisted death. Legal (F = 0.028; P = 0.87) and cost factors (F = 2.618; P = 0.11) and family wishes (F = 0.017; P = 0.90) were not significant in predicting doctors' responses to the patient's request for assisted death in this analysis. Discussion A major finding of this study was that doctors did not make consistent decisions on the treatment of severely ill and terminally ill patients at the end of life. The data suggest that there are no uniform criteria to guide doctors in managing such clinical situations. If these decisions are left solely to doctors then the outcome will vary systematically according to medical training and sociodemographic factors.
The data also show that doctors generally adhered to patients' wishes, both those expressed contemporaneously and those expressed via advance directives. The doctors also considered the wishes of family members to be important in making their treatment choices.
Doctors' capacity to treat patients according to their wishes (and, if necessary, according to the wishes of their families) could be enhanced in two ways:
1. By engaging competent patients (and their families, if required) in comprehensive discussions of treatment options and likely outcomes -- in short, by participating in the informed-consent process.
2. By developing and implementing methods for advanced care planning (advance directives) so that patients can inform doctors of the care they would want if they were to suffer severe and terminal illness and become incompetent.
The first practice, informed consent, may be required by law. However, the concept of informed consent presents problems in a multicultural society, not only because of potential communication problems, but also because of cultural differences in such matters as "truth telling" about the seriousness of an illness. 17
The second practice, the use of advance care planning, is accepted in principle (although its manner of implementation is debated) in North America and the United Kingdom. The practice is rarely even discussed in Australia. In multicultural Australia, research that could inform policy on the acceptability and the implementation of these two practices is lacking. Such research would seem to be imperative.
With respect to euthanasia, this study showed that few doctors would have complied with the wish of the patient who requested assisted death. Baume and O'Malley 9 speculated that such reluctance was a function of the illegality of the action. Our data do not support this speculation. While patients' wishes, and ethical and religious factors for doctors (as with Baume et al. 18 ), seem to be more efficient predictors than legal factors, even the three former variables explain little of the variance in doctors' response to this request for assisted death (only seven per cent for the three variables together).
As an alternative to the speculation of Baume and O'Malley, 9 it may be that, in Australia today, doctors believe that assisting a patient to die is an act that negates what they perceive to be the very essence of their profession. The different ways that doctors perceive this indefinable essential quality (that is, what it means to each of them to be a doctor) may explain the variations in their decision-making.
As Lickiss 19 writes:
There will always be differences of opinion on profound matters in a free society, but being put to death with one's consent is not a private matter, for it strikes at the foundations of what we are, and affects not only the one put to death but the one who carries it out. Our acts shape us, and the act of putting another person to death must change us. If we are doctors, it strikes at the core of what we should be in society: bringers of life, of hope, of healing, of comfort, sometimes bringers of bad news, companions on the way. But not bringers of death.
Hunt, 20 an apparent proponent of some forms of euthanasia, notes that palliative-care practitioners are firmly opposed to physician-assisted death. Other medical practitioners are also opposed. 6,15 Nevertheless, despite the finest symptom management, some terminally ill patients make serious requests for assisted death. 21,22 Perhaps, if some form of euthanasia is to be available to these patients, medical practitioners may not be the most appropriate group to carry out the request. Certainly, it would be prudent to investigate doctors' perceptions of what it means to them to be a doctor in Australia today.
Furthermore, as stated at the beginning of the paper, a major impediment to informed consideration of the issue of euthanasia in Australia is the lack of strong empirical data. While we have added to and improved the data by this study, in which we questioned a national sample of doctors about their end-of-life treatment decisions in the specific clinical scenarios described, we did not attempt the difficult task of obtaining empirical data related to clinical decision-making at the bedside.
Data drawn from strong research into this decision-making process could provide important information before policy on euthanasia is drafted and implemented.
Acknowledgements
This research was funded by the Commonwealth Department of Health and
Family Services, Canberra.
References
- Stevens CA, Hassan R. Management of death, dying and euthanasia:
attitudes and practices of medical practitioners in South
Australia. J Med Ethics 1994; 20: 41-46.
-
Molloy W, Guyatt GH, Alemayehu E, et al. Factors affecting
physicians' decisions on caring for an incompetent elderly patient:
an international study. Can Med Assoc J 1991; 145: 947-952.
-
Kelner MJ, Bourgealt IL. Patient control over dying: responses of
health care professionals. Soc Sci Med 1993; 36: 757-765.
-
Solomon MZ, O'Donnell L, Jennings B, et al. Decisions near the end of
life: Professional views on life- sustaining treatments. Am J
Public Health ; 1993; 83: 14-22.
-
Christakis NA. Physician characteristics associated with
decisions to withdraw life support. Am J Public Health 1995;
85: 367-372.
-
Komesaroff PA, Lickiss JN, Parker M, Ashby MA. The euthanasia
controversy: decision-making in extreme cases. Med J Aust
1995; 162: 594-597.
-
Kaufman SR. Decision making, responsibility, and advocacy in
geriatric medicine: physician dilemmas with elderly in the
community. Gerontologist 1995; 35: 481-488.
-
Ashby M, Wakefield M. Attitudes to some aspects of death and dying,
living wills and substituted health care decision-making in South
Australia: public opinion survey for a parliamentary select
committee. Palliat Med 1993; 7: 273-282.
-
Baume P, O'Malley E. Euthanasia: attitudes and practices of
medical practitioners. Med J Aust 1994; 161: 137-145.
-
Maddocks I. Good palliative care orders. Palliat Med
1993; 7: 35-37.
-
Baume P. Living and dying: a paradox of medical progress. Med J
Aust 1993; 59: 792-794.
-
Wakefield MA, Beilby J, Ashby MA. General practitioners and
palliative care. Palliat Med 1993; 7: 117-126.
-
Seale C, Addington-Hall J. Euthanasia: the role of good care.
Soc Sci Med 1995; 40: 581-587.
-
Allbrook D. Palliative care in the 1990s? Med J Aust 1991;
155: 286-287.
-
Anderson JG, Caddell DP. Attitudes of medical professionals
toward euthanasia. Soc Sci Med 1993; 37: 105-114.
-
Siegel S. Nonparametric statistics for the behavioural
scientist . London: McGraw-Hill 1956.
-
Waddell C, McNamara B. The stereotypical fallacy: a comparison of
Chinese- and Anglo-Australians' thoughts about death-related
matters. Presented at the Annual Australian Sociology Association
Meeting, Newcastle, NSW. December 1995.
-
Baume P, O'Malley E, Bauman A. Professed religious affiliation
and the practice of euthanasia. J Med Ethics 1995; 21: 49-54.
-
Lickiss, N. Chapter in: Chapman S, Leeder S, editors The
last right? Australians take sides on the right to die. Melbourne:
Mandarin, 1995: 98.
-
Hunt RW. The hospice movement matures. Med J Aust 1996;
164: 452-453.
-
Stephany TM. Assisted suicide: how hospice fails. Am J Hospice
Palliat Care 1994; 11: 4-5.
-
Peteet JR. Treating patients who request suicide: a closer look at
the physician's role. Arch Fam Med 1994; 3: 723-727.
(Received 15 May, accepted 29 Jul 1996)
Authors' details
The University of Western Australia, Nedlands, WA.
Charles Waddell, PhD, Senior Lecturer in Anthropology.
Department of Geriatric Medicine, Osborne Park Hospital, Perth, WA.
Roger M Clarnette, MB BS, FRACP, Consultant Physician.
Silver Chain Hospice Care Services, Perth, WA.
Michael Smith, MB BS, MRACMA, Director of Clinical Services.
The Cancer Foundation Cottage Hospice, Perth, WA.
Lynn Oldham , BN(Hons), Clinical Nurse Specialist.
Turning Point Alcohol and Drug Centre, Fitzroy, VIC.
Allan Kellehear, PhD, Professor, and Head of Research
Development.
No reprints will be available. Correspondence: Dr Charles Waddell,
Department of Anthropology, The University of Western Australia,
Nedlands, WA 6907.
E-mail: cwaddell AT uniwa.uwa.edu.au
- - To top of article - ©MJA 1996
<URL: http://www.mja.com.au/> © 1996 Medical Journal of Australia.
Received 25 May 2026, accepted 25 May 2026
- Charles Waddell
- Rodger M Clarnette
- Michael Smith
- Lynn Oldham
- Allan Kellehear




