Teaching hospital medical staff to handwash
Electronically published Tuesday April 30 1996
This article was published in the Medical Journal of Australia on 1 April 1996. Readers may print a single copy for personal use. No further reproduction or distribution of the article in whole or in part should proceed without the permission of the publisher. For copyright permission, contact the Australasian Medical Publishing Company
Abstract - Introduction - Methods - Results - Group performance - Cohort performance - Discussion - Author's Details - Figure - Table 1 - Table 2
- - ©MJA1996
Abstract
Objective: To increase the frequency of handwashing by medical staff.Design: A prospective study of handwashing before and after patient contact.
Setting: A paediatric intensive care unit in a tertiary hospital.
Participants: 61 intensive care unit medical staff and visiting medical staff.
Interventions: A five-phase behaviour modification program: (i) unobtrusive observation for four weeks to obtain a baseline handwashing rate; (ii) overt observation for five weeks (preceded by written advice); (iii) overt observation continued for four weeks with performance feedback; (iv) all observation and feedback discontinued for seven weeks; and (v) unobtrusive observation for five weeks to obtain a residual rate.
Results: 939 patient contacts were observed. The baseline handwashing rates before and after patient contact were 12.4% and 10.6%, respectively. During overt observation, the respective rates increased and plateaued at 32.7% and 33.3%, but increased further (to 68.3% and 64.8%) during the period of performance feedback. The residual handwashing rates, observed unobtrusively seven weeks after the cessation of performance feedback, were 54.6% before and 54.9% after patient contact.
Conclusions: Performance feedback is moderately effective in training hospital medical staff to handwash.
MJA 1996; 164: 395-398
Introduction
Handwashing is one of the most important measures for preventing and controlling nosocomial infection.1-4 Despite this, handwashing practices before and after patient contact by all hospital staff, and especially by physicians, are poor.5-9 Educational programs to improve handwashing by increasing awareness of nosocomial infection have had limited success,10-12 suggesting that an innovative approach is needed.13 A training program for nurses with observation and performance feedback as a behaviour modification technique was successful in the short term, but the relative effects of observation and performance feedback were inseparable.14 My study assessed the frequency of handwashing by medical officers in association with patient contact and determined the effects of observation and performance feedback.Methods
The study was conducted over a five-month period in the Intensive Care Unit (ICU), Royal Children's Hospital, Melbourne, and was approved by the hospital ethics committee. The ICU is an 18-bed multidisciplinary unit treating critically ill infants and children. During the study, 807 patients were admitted: 37% had undergone cardiac surgery, 27% had respiratory illnesses, 9% had general medical illnesses, 8% had newborn medical and surgical illnesses, 8% had trauma, and 8% had undergone neurosurgery and 3% general surgery. Mechanical ventilation was provided for 84% of patients. Most had invasive monitoring or therapeutic devices inserted into peripheral arteries, peripheral or central veins, the thoracic cavity, the urinary bladder or the extradural space. The mortality rate was 5.9%.The ICU is newly constructed and comprises four rooms adjacent to each other along a corridor. Windows enable vision between rooms and into each room from the corridor. Handwashing basins are located in each room within two to three metres of each bed and in the corridor. A choice of handwashing solutions are provided at each basin. During the study these were: (i) a mixture of 1% chlorhexidine gluconate, 70% ethyl alcohol and emollients; (ii) 2% aqueous chlorhexidine gluconate; (iii) 7.5% aqueous povidone-iodine; and (iv) domestic bar soap. Paper-towel dispensers are located at each basin.
I observed patient contact and handwashing practices of medical officers during ward rounds; at other times this observation was by instructed members of the nursing staff. Observations were made between the hours of 7 am and 6 pm on weekdays. Handwashing was regarded as any action to cleanse the hands with water and one of the available handwashing agents, or with a handwashing agent alone. No judgement was made about the duration or efficacy of the handwashing technique. Observations were recorded with the names of subjects and the patients involved. However, anonymity was preserved for data analysis and feedback purposes.
Patient contact was defined as any contact by the hands of a medical officer with a patient's skin or an indwelling invasive device during a procedure in which the hands could be contaminated with the patient's blood, secretions or excretions. Contact with bed linen, bed frames, medical records or monitoring equipment was not regarded as patient contact. Typical patient contact involved procedures such as examining wounds, inserting intravenous or arterial catheters, aspirating endotracheal tubes, performing echocardiographic examinations, auscultating the chest, palpating the chest or abdomen, manipulating chest drains or urinary catheters, inserting tracheal or gastric tubes, and withdrawing blood from intravascular catheters.
Handwashing was assessed before and after contact with a patient. Handwashing was not recorded if the subject was not observed immediately before patient contact, or could not be observed after contact until handwashing had been performed, or contact with another patient had occurred. Departure from the ICU area without handwashing was regarded as failure to handwash. Contact by the subject with his or her own skin, secretions or a mucous membrane (e.g., nasal mucosa) after handwashing but before patient contact was registered as failure to handwash. Medical officers were not requested to handwash, and the ICU did not have any information about handwashing displayed (other than the performance feedback when this part of the study was reached).
The behaviour modification program was divided into five phases1. Weeks 1-4: unobtrusive observation (only hospital personnel involved in the study knew this was happening). At the end of this phase, 19 medical officers who worked in the ICU or visited frequently were requested verbally to estimate their own handwashing rates before patient contact.
2. Weeks 5-9: overt observation; this was preceded by written advice to all medical staff of the intention to study handwashing in ICU. Subjects were not informed which aspect of handwashing was to be studied, although, if requested, information was not to be withheld (no medical staff requested clarification).
3. Weeks 10-13: overt observation with performance feedback; at the beginning of this phase all results collected thus far were displayed as brightly coloured histograms on 40 x 60 cm sheets of paper showing the group percentage handwashing rate before and after patient contact. These were placed in strategic locations used by the medical staff in ICU, but were out of sight of patients and visitors. Data were updated weekly for the four weeks. After two weeks of performance feedback, results of group data collected up to that time were mailed to the medical officers.
4. Weeks 14-20: observations and feedback were discontinued.
5. Weeks 21-25: unobtrusive observation, after which these data were added to the histograms displayed in the ICU.
Handwashing by members of the cohort who were requested to estimate their own handwashing rate and who participated in all phases of the program was analysed separately and is also reported here.
Results
Group performance
Sixty-one medical officers were observed making 939 patient contacts. Twelve were full-time senior or junior ICU staff, and the remainder full-time or part-time senior staff from other disciplines or junior full-time staff. Half the observations (470/939) were made by the investigator, and half by nursing staff.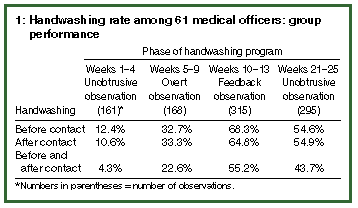
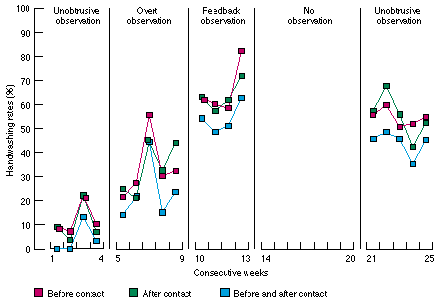
The aggregate handwashing rates before and after patient contact during phases of the program are presented in The aggregate handwashing rates before and after patient contact during phases of the program are presented in Table 1. The week-to-week variation within each phase and between each phase is shown in the Figure. During overt observation the handwashing rate rose from the baseline level (determined by unobtrusive observation), with the peak rate occurring in Week 3 of this five-week period. It rose again during performance feedback, peaking in the last week of this phase. During the second period of unobtrusive observation, seven weeks after performance feedback, the handwashing rate was lower but still showed a more than fourfold increase over baseline levels. There was a gradual decline from week to week during this last phase of unobtrusive observation.
Cohort performance
Nineteen medical officers estimated their own handwashing rate before patient contact after the first phase of covert observation. Their mean estimate was 66% (range, 30%-95%). Several commented that other medical officers washed their hands infrequently.The performance of the cohort during the other phases of the program is shown in Table 2. Significant improvement in handwashing before and after patient contact was observed during overt observation and performance feedback. The improved performance of these 14 subjects was maintained after the period without observation.

Discussion
Patients in intensive care units are at greater risk of nosocomial infection than those elsewhere in hospitals: they are already critically ill; are subject to multiple hand contacts from a wide variety of staff; have indwelling invasive therapeutic and monitoring devices; and often receive non-specific antimicrobial therapy. Reports of nosocomial infection in intensive care units show infection rates varying from 13% to 26%,15-19 whereas hospital-wide nosocomial infection rates are about 5%-10%.20-23Physicians freely acknowledge that handwashing is important in the control of nosocomial infection, and suggest pressure of work, a lack of patient contact, detrimental effects of handwashing agents on skin and the more important needs of the patient as reasons for not handwashing.4 Infection control is rarely taught in medical school,24 and poor handwashing practices may be learnt from peers at the bedside.25
In the first phase of this study, I found the handwashing rate among medical staff to be lower than rates reported previously (13%-28%,5 21%6 and 15%7). Physicians were observed unobtrusively as it is known that observation alone may alter behaviour, a phenomenon otherwise known as the "Hawthorne effect" (after the Hawthorne works of the Western Electric Company, where job performance was improved by the presence of observers).26 This effect was confirmed firstly by the abrupt increase in handwashing which accompanied notification of my intention to observe handwashing and again during the performance feedback phase.
Despite the relative lack of handwashing in relation to patient contact by hospital staff and its possible detrimental consequences, few reports of attempts to improve handwashing have been published. "Educational programs" which aim to increase medical staffs' awareness of nosocomial infection and the importance of handwashing have not been successful. In an intensive care unit the handwashing rate among physicians increased to only 17% after an educational program (in-service teaching rounds, poster displays, specific requests to handwash and unspecified performance feedback to all staff).10 Another study, in a paediatric ambulatory setting, found that physicians did not respond to written and verbal requests to handwash before patient contact.27 Moreover, my study showed that medical staff have an inflated impression of their own handwashing performance, which may possibly prejudice learning. Educational programs to teach nurses to handwash have also been unsuccessful. The failure of one consisting of poster displays and the distribution of booklets on isolation policy was attributed to a lack of motivation.11
Another strategy to improve handwashing is the installation of handwashing machines. This was associated with improvement over a short period in a small group of nurses and physicians, but it was abandoned when there was an outbreak of methicillin-resistant Staphylococcus aureus.28
Several "training programs" to increase handwashing have been more successful than educational awareness programs. A program for nurses consisted of observation and daily feedback of handwashing performance from the previous day; the handwashing rate after patient contact rose from 59% to 92% during a three-week period.14 However, the relative effects of observation and performance feedback could not be separated. Among food handlers in a university cafeteria, performance feedback alone was successful in training to handwash.29
Performance feedback is an intervention frequently used in organisational behaviour management to improve performance.30 In my study, it resulted in an increase in handwashing among medical officers which was sustained at a rate six times the baseline in about two-thirds of contacts with patients.
Regular programs are required to maintain an acceptable standard of performance among permanent staff10 and to compensate for departure and entry of staff members. In my study the difference in handwashing performance between the whole group of medical officers and a cohort within the group may be attributed to staff turnover outside the cohort or, alternatively, to greater exposure to the program, or may be a consequence of being asked to estimate their own handwashing rate. The cohort achieved and maintained a higher handwashing rate than the group as a whole. For reasons of economy and efficacy, behaviour intervention rather than educational awareness programs appears preferable in educating medical staff to handwash.
Acknowledgements
I thank Dr Gerald Elsworth, formerly of the Centre for the Study of Higher Education, University of Melbourne, for helpful suggestions concerning the design of the study. I thank the ICU nurses, particularly Sharon Kinney.
(©MJA 1996; 164: 14-17)
To beginning of this article
References
- Daschner F. Useful and useless hygienic techniques in intensive care units. Intensive Care Med 1985; 11: 280-283.
- Davies PA. Please wash your hands. Arch Dis Child 1982; 57: 647-648.
- Steere AC, Mallison GF. Handwashing practices for the prevention of nosocomial infections. Ann Intern Med 1975; 83: 683-690.
- Larson E, Killien M. Factors influencing handwashing behaviour of patient care personnel. Am J Infect Control 1982; 10: 93-99.
- Albert RK, Condie F. Hand-washing patterns in medical intensive care units. N Engl J Med 1981; 304: 1465-1466.
- Donowitz LG. Handwashing technique in a pediatric intensive care unit. Am J Dis Child 1987; 141: 683-685.
- De Carvalho M, Lopes JMA, Pellitteri M. Frequency and duration of handwashing in a neonatal intensive care unit. Pediatr Infect Dis J 1989; 8: 179-180.
- Larson E. Compliance with isolation technique. Am J Infect Control 1983; 11: 221-225.
- Meengs MR, Giles BK, Chisholm CD, et al. Hand washing frequency in an emergency department. Ann Emerg Med 1994; 23: 1307-1312.
- Conly JM, Hill S, Ross J, et al. Handwashing practices in an intensive care unit: the effects of an educational program and its relationship to infection rates. Am J Infect Control 1989; 17: 330-339.
- Williams E, Buckles A. A lack of motivation. Nursing Times 1988; 84: 60-64.
- Doebbeling BN, Stanley GL, Sheetz CT, et al. Comparative efficacy of alternative hand-washing agents in reducing nosocomial infections in intensive care units. N Engl J Med 1992; 327: 88-93.
- Goldmann D, Larson E. Hand-washing and nosocomial infections. N Engl J Med 1992; 327: 120-122.
- Mayer JA, Dubbert PM, Miller M, et al. Increasing handwashing in an intensive care unit. Infect Control 1986; 7: 259-262.
- Daschner FD, Frey P, Wolff G, et al. Nosocomial infections in intensive care wards: a multicenter prospective study. Intensive Care Med 1982; 8: 5-9.
- Donowitz LG, Wenzel RP, Hoyt JW. High risk of hospital-acquired infection in the ICU patient. Crit Care Med 1982; 10: 355-357.
- Potgieter PD, Linton DM, Oliver SO, Forder AA. Nosocomial infections in a respiratory intensive care unit. Crit Care Med 1987; 15: 495-498.
- Donowitz LG. High risk of nosocomial infection in the pediatric critical care patient. Crit Care Med 1986; 14: 26-28.
- Craig CB, Connelly S. Effect of intensive care unit nosocomial pneumonia on duration of stay and mortality. Am J Infect Control 1984; 12: 233-238.
- McLaws M-L, Gold J, King K, et al. The prevalence of nosocomial and community-acquired infections in Australian hospitals. Med J Aust 1988; 149: 582-590.
- Meers PD, Ayliffe GAJ, Emmerson AM, et al. Report on the national survey of infection in hospitals, 1980. J Hosp Infect 1981; 2(Suppl): 13-17.
- Haley RW, Culver DH, White JW, et al. The nationwide nosocomial infection rate. A new need for vital statistics. Am J Epidemiol 1985; 121: 159-167.
- Mayon-White RT, Ducel G, Kereselidze T, Tikomirov E. An international survey of the prevalence of hospital-acquired infection. J Hosp Infect 1988; 11(Suppl A): 43-48.
- Moss F, Cochrane JPS, Yudkin JS. Introducing medicine to tomorrow's doctors. Lancet 1987; 1: 203-205.
- Larson E, McGinley KJ, Grove GL, et al. Physiologic, microbiologic and seasonal effects on the skin of health care personnel. Am J Infect Control 1986; 14: 51-59.
- Roethlisberger FJ, Dickson WJ. Management and the worker. Cambridge, Mass: Harvard University Press, 1942.
- Lohr JA, Ingram DL, Dudley SM, et al. Handwashing in paediatric ambulatory settings. Am J Dis Child 1991; 145: 1198-1199.
- Wurtz R, Moye G, Jovanovic B. Handwashing machines, handwashing compliance and potential for cross-contamination. Am J Infect Control 1994; 22: 228-230.
- Geller ES, Eason SL, Phillips JA, Pierson MD. Interventions to improve sanitation during food preparation. J Organizational Behav Manage 1980; 2: 229-240.
- Prue DM, Fairbank JA. Performance feedback in organizational behavior management: a review. J Organizational Behav Manage 1981; 3: 1-16.
(Received 26 Jun, accepted 5 Dec 1995)
Author's details
Intensive Care Unit, Royal Children's Hospital, Melbourne, VIC.James Tibballs, MEd, FFICANZCA, Deputy Director.
Reprints: Dr J Tibballs, Intensive Care Unit, Royal Children's Hospital, Flemington Road, Parkville, VIC 3052. E-mail: tibballjATcryptic.rch.unimelb.edu.au
(©MJA 1996; 164: 14-17)
< URL: http://www.mja.com.au/>
© 1996 Medical Journal of Australia.
Received 20 May 2026, accepted 20 May 2026
- James Tibballs




