Bipolar disorder is a chronic mental illness that poses many treatment challenges. Although medication is a core treatment component (see Malhi et al),1 medications alone do not address many illness-related issues such as persistent subthreshold depression, adjustment to illness, medication adherence, and social and occupational functioning. Psychosocial interventions have an increasing evidence base as an adjunct to pharmacotherapy in the optimal management of this complex disorder.
Non-adherence to medication is a major cause of relapse in bipolar disorder.2,3 The factors involved in non-adherence are multifaceted and occur at the individual, service delivery, and illness levels.
Individual factors of illness acceptance, beliefs and level of understanding of the disorder, and fear of the role of medication all affect adherence.3-6 Treatment complexity and tolerability issues also contribute to non-adherence. This is further compounded by some patients “chasing” the elevated mood pole; those with a predominance of mania are more likely to be non-adherent.7 Lack of knowledge about the disorder and the reason for taking medication, and misinformation leading to inaccurate beliefs and fears about medication are risk factors for non-adherence in bipolar disorder.8 Psychoeducation combined with a collaborative alliance between the clinician and the patient can help to reduce these risks.9 Understanding the patient’s beliefs about the disorder and its treatment can facilitate targeted intervention to improve adherence.10 Interventions such as simplifying the treatment regimen and building in reminders (eg, a diary) or cues (eg, link to brushing teeth) can also be helpful: a recent study of 140 people with bipolar disorder found a strong factor in poor adherence was forgetting to take medication.8
Barriers to care can occur at a system and service delivery level, at which greater barriers are associated with more non-adherence.11 Issues of access, convenience and cost all affect engagement with treatment.12
At an illness level, psychiatric comorbidities are also associated with reduced medication adherence. Predictably, comorbid substance misuse predicts non-adherence, and is associated with a worse outcome13 and an increased risk of suicidality.2 A recent trial of a 12-session, group-based cognitive behaviour therapy (CBT) program for people with bipolar disorder and comorbid substance misuse showed promising trends in reducing substance misuse and bipolar relapse compared with group-based counselling for substance misuse alone.14
Although medications play a vital role in reducing relapse, relapse can occur even when medication adherence is optimal. Medications have been shown to have limited efficacy in addressing functional impairment between episodes and tend to have greater efficacy in depression than mania.13,15,16 As depression is the predominant burden, it is noteworthy that psychotherapy (eg, CBT) often shows more benefit in depression than mania.
Functional improvement following an illness episode takes considerably longer than symptomatic recovery.17 Even with effective pharmacotherapy, there is impairment in social and occupational domains for 60% of patients.18 Cognitive, relationship, living and work deficits can have a significant detrimental impact.17 While the primary outcome of most psychosocial interventions has been to reduce relapse, a number of adjunctive interventions show improvements in functionality;19,20 such interventions have also been shown to be more effective at enhancing social functioning than medication alone.21
Although there are distinct theoretical approaches to the psychosocial treatment of bipolar disorder, there is a blurring of boundaries between them, with a number of shared components. Overall, they differ more in their emphasis, rather than in their unique elements. A meta-analysis of psychosocial interventions for bipolar disorder showed no evidence to suggest superiority of any specific type of therapeutic approach, perhaps due to the extent to which their content overlapped.22 At the individual level, however, particular psychosocial needs should be identified, and treatment individualised as far as possible. As with medication, there is no single psychosocial tool that every patient will find useful.
The underlying principle of psychoeducation is information and education, which are typically given in a didactic manner.23 Points on providing psychoeducation are noted in Box 1.
Primary components of psychoeducation include information about: the illness and the role of medication; regulation of biological rhythms (eg, the sleep–wake cycle); identification of illness triggers; personal illness profiles (eg, identification of prodromes); and relapse prevention plans.24 Other elements encompass risk behaviour, including substance misuse, stress management and problem-solving strategies.24,25 The number of sessions involved in psychoeducation programs varies, from five sessions in the first phase of the Life Goals Program26 to 21 in another group-based psychoeducation program.27
Psychoeducation can significantly reduce relapse and improve functioning, over and beyond improving medication adherence.28 Recently published 5-year outcomes of group-based psychoeducation show enduring benefits, with fewer episodes of illness and higher levels of functioning, in comparison to non-structured group meetings.27
Based on the treatment of unipolar depression, CBT has been used as an adjunct to medication in bipolar disorder.29 CBT emphasises personal skill development using cognitive strategies to challenge distorted thoughts that may lead to changes in mood.30 Behavioural strategies focus on responding to triggers and mood changes; these include strategies to increase activity levels when the patient is lethargic and depressed, and strategies to assist the patient to set small manageable goals.
A study of individual cognitive therapy for bipolar disorder showed positive outcomes at 1-year follow-up, but the benefits were reduced over time, suggesting the need for booster sessions to sustain the gains.19 As with many forms of therapy, CBT has been found to be more successful in reducing relapse in the depressive pole compared with the manic pole.30 A large randomised trial of CBT showed no difference between CBT and treatment as usual, when all participants were included in the analyses.31 However, results of a post-hoc analysis suggested that CBT was effective for participants who reported fewer than 12 prior episodes of illness and were not acutely unwell when therapy began; numbers of episodes of mania rather than depression seemed to predict treatment response.32 Such data can help guide the clinical application of CBT for bipolar patients.
Few studies have assessed whether CBT alone is more or less effective than CBT plus psychoeducation, but no difference between CBT plus psychoeducation and psychoeducation alone has been reported.33 A 12-week group-based intervention (with three additional booster sessions) that encompasses psychoeducation and elements of CBT and social rhythm therapy has been developed.30,34,35 This program was found to be effective in reducing both depressive and manic relapses.35 An eclectic and comprehensive approach may be important for effectively dealing with both poles of the illness.
Based on the interpersonal psychotherapy model of depression and informed by the importance of regular social rhythms in bipolar disorder,36 interpersonal and social rhythm therapy explores pathways to relapse, including disruptions to social and circadian patterns, non-adherence to medication, and stressful life events.37 The model suggests that positive and negative life events can adversely affect circadian rhythms, posing a risk of recurrence.36 It tackles these issues by establishing regular routines, exploring interpersonal conflict and addressing issues around social roles,37 and it seems to have promise in managing bipolar disorder.
Interpersonal family stress contributes to relationship breakdown and lack of perceived social support, and high expressed emotion may contribute to relapse.21 Family-focused treatment has been shown to reduce recurrence when used as an adjunct to medication for bipolar disorder.38 It is initiated once stabilisation of mood has been effected after an acute episode, and includes the patient and at least one significant family member (eg, parent or spouse).39 The underlying focus of family-focused treatment is to provide education regarding the recent illness episode; this includes exploring possible causes and the patient’s personal triggers, discussing the importance of medication, differentiating between the person and the illness, and enhancing positive family relationships.40 Improved positive communication appears to be a key mechanism in this approach.38,41 Recent studies suggest greater benefits in reducing depressive rather than manic relapses.23,38,42
Family members of people with bipolar disorder suffer from high rates of carer burden.43 A group psychoeducation program for carers helped to reduce carer burden as well as manic and hypomanic relapse.44,45 This highlights the benefits of considering the patient’s social milieu and the way the illness affects meaningful relationships. Incorporating family members when possible in the routine management of bipolar disorder is valuable. Including the family in clinical care, basic psychoeducation, relapse planning and advance directives are strategies that can be adopted in routine clinical settings.
A rapidly growing area for the management of mental illnesses is that of online therapies. In general, online therapies are based on models of face-to-face therapy. Therapies for depression and panic disorder are established examples. For bipolar disorder, a number of models are in development, including MoodSwings (http://www.moodswings.net.au).46 It is expected that, if formal trials demonstrate efficacy, these programs will become widely used due to their cost-effectiveness, convenience and reach.
Studies of psychosocial interventions for bipolar disorder clearly indicate they have a role in adjunctive treatment of the illness. A meta-analysis has shown a significant reduction in relapse rates, of about 40%, in comparison to usual treatment.29 Approaches that have been flagged as most effective include CBT, group psychoeducation and family therapy.22
The success of these interventions may, to some extent, lie in their shared elements. The different psychosocial interventions all have some overlapping paradigms; for example, psychoeducation is part of CBT.47 It may also reflect a similar approach to delivery, in that material is presented in a sequential and structured manner, with an emphasis on patients gaining personalised skills in the management of their illness.34 Finally, the different psychological approaches each have their own emphasis, but share the strategies shown in Box 2 — that is, key content related to the therapeutic alliance, education, enhancement of adherence, early identification of prodromes, awareness of illness triggers, the importance of supportive relationships, and development of strategies such as relapse prevention plans and constructive coping skills.
Written materials that reinforce information are useful, and can also be passed on to friends and family. There are a number of books aimed at providing information and strategies to patients and their families. Books that highlight individual journeys can be particularly inspiring, such as those by clinical psychologist Kay Redfield Jamison and researcher Sarah Russell, who documents individual experiences with bipolar disorder. There are also several reputable, open-access websites that specifically provide information on bipolar disorder, including McMan’s Depression and Bipolar Web (http://www.mcmanweb.com), run by health journalist John McManamy, and PsychEducation.org (http://www.psycheducation.org), maintained by psychiatrist Jim Phelps.
Linking patients and their carers to local support groups can help reduce feelings of stigma and isolation. Some patients may also find online forums supportive, such as the bipolar forum on BlueBoard (http://blueboard.anu.edu.au), a discussion board monitored by researchers at the Australian National University. However, lack of monitoring can be an issue with some discussion boards and chat rooms, with patients sharing unpleasant experiences with other forum users.
Prospective mood monitoring: This form of monitoring is typically done on a daily basis, whereby patients record mood, anxiety and sleep, along with a journal note that can be used to identify possible triggers. Many mood monitors also record whether medication was taken as prescribed and phase of menstrual cycle. An example is shown in Box 3. This detailed approach allows for the identification of triggers, and can help develop insight into the illness and aid with adherence. It also provides a vehicle to identify symptoms of illness early and monitor response to treatment, and provides information on the course of an illness episode. It serves as a collaborative tool between patient and physician and can enhance the therapeutic alliance.48,49
1 Points on providing psychoeducation
No matter how long it is since a patient has been diagnosed with bipolar disorder, do not assume that he or she has a good knowledge of the illness.
As much as possible, relate education and information to the patient using examples.
Provide written material that can be referred to later and can be passed on to family and friends.
Linking with local support groups can help to reduce feelings of isolation and stigma through sharing of information and experiences.
It can be useful to include family members in basic information sessions — this requires prior consultation with the individual patient.
- Sue D Lauder1
- Michael Berk1,2,3,4
- David J Castle5,6
- Seetal Dodd1
- Lesley Berk4
- 1 Department of Clinical and Biomedical Sciences — Barwon Health, University of Melbourne, Geelong, VIC.
- 2 The Geelong Clinic, Healthscope, Geelong, VIC.
- 3 Mental Health Research Institute, Melbourne, VIC.
- 4 Orygen Youth Health Research Centre, University of Melbourne, Melbourne, VIC.
- 5 Department of Psychiatry, University of Melbourne, Melbourne, VIC.
- 6 St Vincent’s Hospital, Melbourne, VIC.
Lesley Berk is supported by a National Health and Medical Research Council (NHMRC) PhD Scholarship.
Seetal Dodd has received grants from the NHMRC, Stanley Medical Research Institute, Eli Lilly, GlaxoSmithKline, Servier, the Australian Rotary Health Research Fund and beyondblue, and has received speaker fees and funding for travel and accommodation expenses from Eli Lilly to present at symposia organised by Eli Lilly.
- 1. Malhi GS, Adams D, Berk M. The pharmacological treatment of bipolar disorder in primary care. Med J Aust 2010; 193 (4 Suppl): S24-S30. <MJA full text>
- 2. Perlick DA, Rosenheck RA, Kaczynski R, Kozma l. Medication non-adherence in bipolar disorder: a patient-centered review of research findings. Clin Approach Bipolar Disord 2004; 3: 56-64.
- 3. Baldessarini RJ, Perry R, Pike J. Factors associated with treatment nonadherence among US bipolar disorder patients. Hum Psychopharmacol 2008; 23: 95-105.
- 4. Clatworthy J, Bowskill R, Rank T, et al. Adherence to medication in bipolar disorder: a qualitative study exploring the role of patients’ beliefs about the condition and its treatment. Bipolar Disord 2007; 9: 656-664.
- 5. Scott J, Pope M. Nonadherence with mood stabilizers: prevalence and predictors. J Clin Psychiatry 2002; 63: 384-390.
- 6. Goodwin FK, Jamison K. Manic-depressive illness: bipolar disorders and recurrent depression. 2nd ed. New York: Oxford University Press, 2007.
- 7. Gutheil TG. The psychology of psychopharmacology. Bull Menninger Clin 1982; 46: 321-330.
- 8. Sajatovic M, Ignacio RV, West JA, et al. Predictors of nonadherence among individuals with bipolar disorder receiving treatment in a community mental health clinic. Compr Psychiatry 2009; 50: 100-107.
- 9. Berk M, Berk L, Castle D. A collaborative approach to the treatment alliance in bipolar disorder. Bipolar Disord 2004; 6: 504-518.
- 10. Colom F, Vieta E, Reinares M, et al. Psycho-education efficacy in bipolar disorders: beyond compliance enhancement. J Clin Psychiatry 2003; 64: 1101-1105.
- 11. Sajatovic M, Biswas K, Kilbourne AK, Fenn H. Factors associated with prospective long-term treatment adherence among individuals with bipolar disorder. Psychiatr Serv 2008; 59: 753-759.
- 12. Kessler RC, Berglund PA, Bruce ML, et al. The prevalence and correlates of untreated serious mental illness. Health Serv Res 2001; 36: 987-1007.
- 13. Keck PE, McElroy SL, Strakowski SM, et al. Compliance with maintenance treatment in bipolar disorder. Psychopharmacol Bull 1997; 33: 87-91.
- 14. Weiss RD, Griffin ML, Jaffee WB, et al. A “community-friendly” version of integrated group therapy for patients with bipolar disorder and substance dependence: a randomized controlled trial. Drug Alcohol Depend 2009; 104: 212-219.
- 15. Calabrese JR, Hirschfeld RM, Reed M, et al. Impact of bipolar disorder on a US community sample. J Clin Psychiatry 2003; 64: 425-432.
- 16. Mitchell P, Slade T, Andrews G. Twelve-month prevalence and disability of DSM-IV bipolar disorder in an Australian general population survey. Psychol Med 2004; 34: 777-785.
- 17. Tohen M, Zarate C, Hennen J, et al. The McLean-Harvard First-Episode Mania Study: prediction of recovery and first recurrence. Am J Psychiatry 2003; 160: 2099-2107.
- 18. MacQueen GM, Young LT, Joffe RT, et al. A review of psychosocial outcome in patients with bipolar disorder. Acta Psychiatr Scand 2001; 103: 163-170.
- 19. Lam D, Hayward P, Watkins ER, et al. Relapse prevention in patients with bipolar disorder: cognitive therapy outcome after 2 years. Am J Psychiatry 2005; 162: 324-329.
- 20. Miklowitz DJ. The role of the family in the course and treatment of bipolar disorder. Curr Dir Psychol Sci 2007; 16: 192-196.
- 21. Miklowitz DJ, Johnson SL. Social and familial factors in the course of bipolar disorder: basic processes and relevant interventions. Clin Psychol (New York) 2009; 16: 281-296.
- 22. Beynon S, Soares-Weiser K, Woolacott N, et al. Psychosocial interventions for the prevention of relapse in bipolar disorder: systematic review of controlled trials. Br J Psychiatry 2008; 192: 5-11.
- 23. Miklowitz DJ. Adjunctive psychotherapy for bipolar disorder: state of the evidence. Am J Psychiatry 2008; 165: 1408-1419.
- 24. Colom F, Vieta E. Psycho-education manual for bipolar disorder. Cambridge: Cambridge University Press, 2006.
- 25. Sajatovic M, Davies MA, Ganocy SJ, et al. A comparison of the life goals program and treatment as usual for individuals with bipolar disorder. Psychiatr Serv 2009; 60: 1182-1189.
- 26. Bauer M, McBride L. Structured group psychotherapy for bipolar disorder: the Life Goals Program. New York: Springer Publishing Company, 1996.
- 27. Colom F, Vieta E, Martinez-Aran A, et al. A randomized trial on the efficacy of group psycho-education in the prophylaxis of recurrences in bipolar patients whose disease is in remission. Arch Gen Psychiatry 2003; 60: 402-407.
- 28. Colom F, Vieta E, Tacchi MJ, et al. Identifying and improving non-adherence in bipolar disorders. Bipolar Disord 2005; 7 Suppl 5: 24-31.
- 29. Scott J, Colom F, Vieta E. A meta-analysis of relapse rates with adjunctive psychological therapies compared to usual psychiatric treatment for bipolar disorders. Int J Neuropsychopharmacol 2007; 10: 123-129.
- 30. Castle DJ, Berk L, Lauder S, et al. Psychosocial interventions for bipolar disorder. Acta Neuropsychiatrica 2009; 21: 275-284.
- 31. Scott J, Paykel E, Morriss R, et al. Cognitive-behavioural therapy for severe and recurrent bipolar disorders. Br J Psychiatry 2006; 188: 313-320.
- 32. Scott J. The MRC UK pragmatic effectiveness trial of CBT for severe and recurrent bipolar disorders: clouds and silver linings. Bipolar Disorders 2010; 12 Suppl 1: 64-65.
- 33. Zaretsky A, Lancee W, Miller C, et al. Is cognitive-behavioural therapy more effective than psycho-education in bipolar disorder? Can J Psychiatry 2008; 53: 441-448.
- 34. Castle D, Berk M, Berk L, et al. Pilot of group intervention for bipolar disorder. Int J Psychiatry Clin Pract 2007; 11: 279-284.
- 35. Castle D, White C, Chamberlain J, et al. Group-based psychosocial intervention for bipolar disorder: randomised controlled trial. Br J Psychiatry 2010; 196: 383-388.
- 36. Frank E, Swartz HA, Kupfer DJ. Interpersonal and social rhythm therapy: managing the chaos of bipolar disorder. Biol Psychiatry 2000; 48: 593-604.
- 37. Frank E. Interpersonal and social rhythm therapy: a means of improving depression and preventing relapse in bipolar disorder. J Clin Psychol 2007; 63: 463-473.
- 38. Miklowitz D, George E, Richards J, et al. A randomized study of family-focused psycho-education and pharmacotherapy in the outpatient management of bipolar disorder. Arch Gen Psychiatry 2003; 60: 904-912.
- 39. Miklowitz DJ, Scott J. Psychosocial treatments for bipolar disorder: cost-effectiveness, mediating mechanisms, and future directions. Bipolar Disord 2009; 11 Suppl 2: 110-122.
- 40. Miklowitz DJ, Otto MW. New psychosocial interventions for bipolar disorder: a review of literature and introduction of the systematic treatment enhancement program. J Cogn Psychother 2006; 20: 215-230.
- 41. Simoneau T, Miklowitz D, David J, et al. Bipolar disorder and family communications: effects of a psycho-educational treatment program. J Abnorm Psychol 1999; 108: 588-597.
- 42. Miller IW, Keitner GI, Ryan CE. Family treatment for bipolar disorder: family impairment by treatment interactions. J Clin Psychiatry 2008; 69: 732-740.
- 43. Perlick D, Clarkin JF, Sirey J, et al. Burden experienced by care-givers of persons with bipolar affective disorder. Br J Psychiatry 1999; 175: 56-62.
- 44. Reinares M, Vieta E, Colom F, et al. Impact of a psycho-educational family intervention on caregivers of stabilized bipolar patients. Psychother Psychosom 2004; 73: 312-319.
- 45. Reinares M, Colom F, Sanchez-Moreno J, et al. Impact of caregiver group psycho-education on the course and outcome of bipolar patients in remission: a randomized controlled trial. Bipolar Disord 2008; 10: 511-519.
- 46. Lauder S, Berk M, Castle D, et al. www.moodswings: the highs and lows of an online intervention for bipolar disorder, preliminary findings. Aust N Z J Psychiatry 2008; 42 Suppl 3: A83-A84.
- 47. Basco MR, Ladd G, Myers DS, Tyler D. Combining medication treatment and cognitive-behavior therapy for bipolar disorder. J Cogn Psychother 2007; 21: 7-15.
- 48. Baldassano CF. Assessment tools for screening and monitoring bipolar disorder. Bipolar Disord 2005; 7 Suppl 1: 8-15.
- 49. Denicoff K, Ali S, Sollinger A, et al. Utility of the daily prospective National Institute of Mental Health life-chart method (NIMH-LCM-p) ratings in clinical trials of bipolar disorder. Depress Anxiety 2002; 15: 1-9.






Abstract
Adjunctive psychosocial interventions for bipolar disorder target many of the issues that are not addressed by medication alone, including non-adherence, efficacy–effectiveness gap and functionality.
Psychosocial interventions have been found to reduce relapse, particularly for the depressive pole, and improve functionality.
Approaches such as psychoeducation, cognitive behaviour therapy, interpersonal and social rhythm therapy, and family therapy have shown benefits as adjunctive treatments.
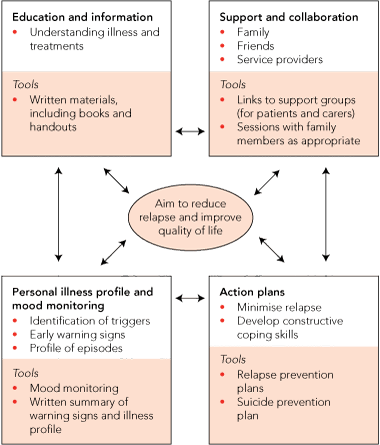
Each of the various psychosocial interventions has a unique emphasis, but they share common elements. These include: providing information and education; developing a personal understanding of the illness, such as triggers and early warning signs; having prepared strategies in place for early intervention, should symptoms of illness develop; and promoting a collaborative approach.
Evidence to date supports the use of adjunctive psychosocial interventions in the management of bipolar disorder.