A number of recent studies have reviewed aspects of the complex questions associated with alcohol consumption, particularly with the misuse of alcohol.1-4 The impact of alcohol on emergency services has also been examined.5-10 It was found that drinking a single glass of wine doubled the risk of presentation to an emergency department; after three glasses, there was a 5-fold increase.11 The same study found that, after 10 standard drinks, the risk of needing to attend an emergency department was increased 10-fold for men and 14-fold for women.
There have been few well designed studies of alcohol-related injuries, and they often rely on emergency department data. Although of some value, such data have significant limitations if not collected prospectively and their acquisition appropriately resourced.12
On 24 February 2014, the New South Wales Government introduced changes to liquor regulations in the central district of the City of Sydney, the so-called “party precinct”. These legislative changes were enacted in response to community outrage after a series of adverse events reported in the media, particularly the deaths of two young men associated with alcohol-fuelled violence.
Many of the changes were based on successful strategies in the nearby Australian city of Newcastle, which had experienced similar alcohol-related serious injury problems.7,8 Some of the core changes are listed in Box 1. Several other, possibly key, initiatives were introduced in Sydney during the first year of the changed regulations. These included:
visibly increased police presence and monitoring;
introduction of identity document scanning on entry into some venues; and
sharing of information by venues to prevent intoxicated persons who have been refused entry at one site from gaining access to another.
In addition to the legislative changes, volunteer nocturnal patrols, usually under the auspices of non-government organisations, also commenced activities in the precinct.
Some of the initiatives were controversial in both the medical literature and the broader media.7-9,13 Our study was undertaken to assess the impact of these measures on alcohol-related serious injury, and also to determine the possible impact on emergency services in the relevant catchment area. Our study is timely in view of the review process currently being undertaken by the Australian Government on the impact of the lockout laws.14
Methods
To determine whether the strategy adopted to reduce alcohol-related injury in central Sydney has been successful, we undertook a 2-year retrospective analysis of alcohol-associated serious presentations to the emergency department of St Vincent’s Hospital, a major teaching hospital in the heart of the area where the changes were instituted. We analysed patient data stored on the hospital’s emergency department patient information computer system (EDIS).
Patient records for two periods were analysed: the 12 months preceding the introduction of the new alcohol laws (24 February 2013 – 23 February 2014; period 1) and the 12 months after their introduction (24 February 2014 – 23 February 2015; period 2). To avoid any bias, the researchers were blinded to which year was being analysed. One of the authors (G F) was assigned as the sole assessor who identified cases of alcohol-related serious injury.
Our search was restricted to persons with injuries classified under Australasian triage categories 1 and 2, as our attention was focused on the seriously or critically injured (Box 2). De-identified, routinely obtained demographic data included time and day of the week of the relevant injury. Other key data fields that were extracted and analysed were presenting symptoms and triage assessment.
In order to identify patients injured by serious assault, but also those suffering other serious injuries and major traumas associated with alcohol (such as vehicular and pedestrian injuries, or falls from a height), the presenting symptoms, triage assessment and diagnosis of all patients who presented as a result of serious trauma during the periods of analysis were examined for any reference to alcohol. All patients identified in this manner were included in this study.
The Fisher exact test was used to compare categorical outcome data, with statistical significance defined as P < 0.05. Confidence intervals (95%) for proportions were calculated with the standard assumption of normally distributed logarithms of the relative risk. There were no missing data for the analysed variables. Data analysis was performed with Stata 13 (StataCorp).
Ethics
Ethics approval was obtained for the study from the St Vincent’s Hospital Human Research Ethics Committee (ref. HREC/LNR/15/SVHA/62).
Results
During the 2-year study period, there were 13 110 Australasian triage category 1 and 2 presentations to the St Vincent’s Hospital emergency department: 6467 patients during period 1 and 6643 during period 2.
Of these presentations, 564 (4.3%) were identified as alcohol-related serious injuries: 318 during period 1 (4.9% of presentations during this period) and 246 during period 2 (3.7%). This decrease was statistically significant (P < 0.05), and occurred gradually during period 2 (Box 3).
Given the nature of the problem, we examined the high alcohol time (HAT) separately; ie, the weekend, from 6 pm Friday to 6 am Sunday. The proportion of alcohol-related serious injury presentations in triage categories 1 and 2 was much higher during HAT (9.1%) than the rest of the week (3.1%; P < 0.05). There was a significant decrease in the total number of seriously injured patients during HAT after the introduction of the various control measures in 2014: from 140 presentations (10.4%) in the 12 months before the changes to 106 (7.8%) in period 2 (P < 0.05). This was a relative risk reduction of 24.8% (95% CI, 4.3%–40.9%).
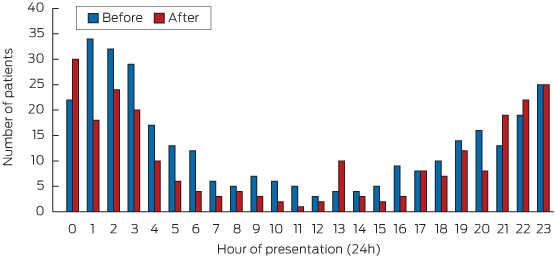
Analysis of the numbers of alcohol-related injuries by time of day found a consistent decrease in the number of presentations of seriously injured patients with alcohol-related injuries between 1 am and noon after the introduction of the new regulations. There was, however, a small increase in the number of patients presenting with alcohol-related injuries between 9 pm and midnight, as well as a small spike around 1 pm (Box 4).
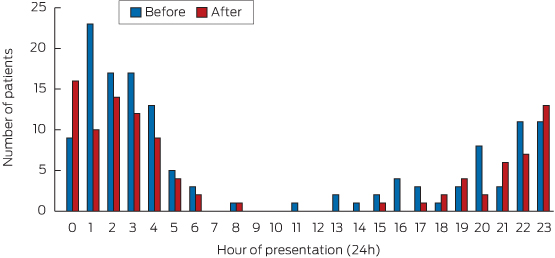
These trends were even clearer when analysis was restricted to HAT (Box 5). During this time period, large reductions in serious injuries associated with alcohol-related violence were seen after 1 am.
Discussion
Our analysis has identified some significant positive results that followed the 2014 changes to the liquor laws and associated measures.
The clear decrease in serious injuries related to alcohol took some time to occur (Box 3); the gradual implementation of the policies may have led to a delayed decline in alcohol-related serious injuries. The small increase in alcohol-related injuries between 9 pm and midnight after the changes were introduced may have been related to increased alcohol intake earlier in the evening (“preloading”), before the times when the various bans take effect; the 1 pm spike may reflect lunchtime alcohol consumption.
The new measures were focused on curbing excessive drinking and violent behaviour after midnight, which could also explain some of our findings. Other indicators outside the scope of this study also support the success of the combined measures during their first 12 months of operation. Neurosurgeons at St Vincent’s Hospital reported a decrease in the numbers of patients presenting between 8 pm and 8 am with serious head injuries, which often require immediate surgery, from 26 patients during period 1 to 11 in the 12 months after the changes. Intensive care use also decreased; notably, there was not a single admission associated with alcohol-related violence during the first New Year’s Eve after the changes.16 The NSW Bureau of Crime Statistics reported a 32%–40% drop in assaults across the CBD Entertainment Precinct, and there was no increase in the number of assaults in neighbouring police command areas during the 12 months after the changes.17
There is significant controversy and discussion about which elements of the interventions may have been effective. Because of the non-specific nature of the data recorded, our study could not examine the effects of individual measures. The cost–benefit relationship of changes introduced to reduce alcohol-related serious harm has also been debated, as income, jobs and businesses have been lost as a result of the changes.4,10 This is especially relevant because the NSW Government is reported to be considering widening the regulations to include other geographical areas.
The precise costing of any reduction in the need for hospital care can be difficult,18 but the resources needed to treat critically ill, seriously injured patients, often after regular operating hours, and other associated costs are significant. The burden to both the patient and the community must be considered alongside the morbidity and mortality data.1,19
There are many limitations inherent to this and similar studies.8-10,13 Our methods cannot accurately capture complete data on the intake of alcohol. They rely on voluntary information provided by the patient and enquiries by health care workers; the information is recorded as free text in the EDIS system, without specific details about a number of relevant factors, such as the precise details of the reported injury or accident. The involvement of alcohol in trauma cases is almost certainly underestimated to a considerable extent, as blood alcohol testing may not be routinely undertaken in all unconscious or severely injured patients. Further, it was beyond the scope of our study to correct for potentially relevant demographic or ecological variables during the period of the study, such as population volumes.
Published research on acute alcohol harm relies heavily on information from emergency departments.5,11,20 This approach to data collection is not methodologically designed, and, being retrospective, is especially limited when trying to establish any causal relationships. In response to this, an Australia-wide research and data collection initiative has been established, and this collaboration between researchers, health organisations and the Australasian College of Emergency Medicine should facilitate a formal, more robust approach to data collection (personal communication, Associate Professor Peter G. Miller, School of Psychology, Deakin University, June 2015).
This study found a significant decrease in the number of patients presenting to a major trauma and teaching hospital with critical or seriously injuries related to alcohol use following the 2014 changes to regulations in the inner-city precinct of Sydney, Australia. The reduction was most marked in the period after midnight, which corresponds with the main thrust of the changed regulations.
Box 1 – Key changes to alcohol laws for the Sydney CBD Entertainment Precinct, 2014
- All takeaway alcohol sales stop at 10 pm.
- No service of “shots” (alcoholic spirits) after midnight.
- 1.30 am–3.30 am “lockouts” at hotels, registered clubs, nightclubs and licensed karaoke bars. No entry for patrons, or re-entry for those who exit during the lockout period.
- 3.00 am “last drinks”. All alcohol service ceases.
Box 2 – Australasian triage categories relevant to serious or critical injuries15
Category 1 |
Immediately life-threatening: conditions that are threats to life (or imminent risk of deterioration) and require immediate aggressive intervention. |
||||||||||||||
Category 2 |
Imminently life-threatening: condition is serious enough or deteriorating so rapidly that there is the potential of threat to life, or organ system failure, if not treated within 10 minutes of arrival in the emergency department; orImportant time-critical treatment: the potential for time-critical treatment (eg, thrombolysis, antidote) to make a significant effect on clinical outcome depends on treatment commencing within a few minutes of the patient’s arrival in the emergency department; orVery severe pain: humane practice mandates the relief of very severe pain or distress within 10 minutes. |
||||||||||||||
Box 3 – Alcohol-related serious injury presentations to the emergency department of St Vincent’s Hospital, Sydney, by calendar month, before and after changes to alcohol regulations.
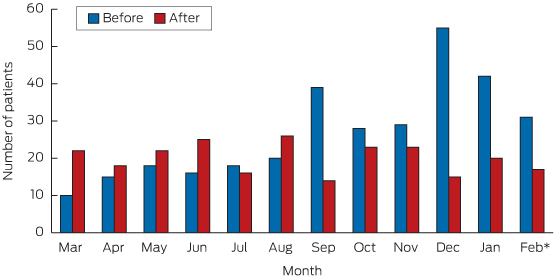
*February 2014: 26 cases to 23 February, 5 for 24–28 February; February 2015: cases until 23 February (study end).
Received 1 June 2015, accepted 9 September 2015
- Gordian WO Fulde
- Myles Smith
- S Lesley Forster
- 1 St Vincent’s Hospital, Sydney, NSW
- 2 Rural Clinical School, University of New South Wales, Wagga Wagga, NSW
: No relevant disclosures.
- 1. Janusic T. Graduating to better health: “Schoolies” without a hangover. Med J Aust 2014; 201: 559. <MJA full text>
- 2. Lindo J, Siminski P. Should the legal age for buying alcohol be raised to 21 years? Med J Aust 2014; 201: 571. <MJA full text>
- 3. Toumbourou J, Kypri K, Jones S. Should the legal age for buying alcohol be raised to 21 years? Med J Aust 2014; 201: 571. <MJA full text>
- 4. Cowie G, Bolam B. Anomalous warning labels on alcohol energy drink cans. Med J Aust 2014; 201: 572. <MJA full text>
- 5. Egerton-Warburton D, Gosbell A, Wadsworth A, et al. Survey of alcohol-related presentations to Australasian emergency departments. Med J Aust 2014; 201: 584-587. <MJA full text>
- 6. Cherpitel C, Ye Y, Bond J, et al. Relative risk of injury from acute alcohol consumption: modelling the dose—response relationship in emergency department data from 18 countries. Addiction 2015; 110: 279-288.
- 7. Kypri K, McElduff P, Miller P. Restrictions in pub closing times and lockouts in Newcastle, Australia five years on. Drug Alcohol Rev 2014; 33: 323-326.
- 8. Miller P, Coomber K, Sonderlund A, et al. The long term effect of lockouts on alcohol-related emergency department attendances within Ballarat, Australia. Drug Alcohol Rev 2012; 31: 370-376.
- 9. Miller P, Curtis A, Palmer D, et al. Changes in injury related emergency department presentations associated with the imposition of regulatory versus voluntary licensing conditions on licensed venues in two cities. Drug Alcohol Rev 2014; 33: 314-322.
- 10. Miller P, Droste N, Baker T, et al. Last drinks: A study of rural emergency department data collection to identify and target community alcohol-related violence. Emerg Med Australas 2015; 27: 225-231.
- 11. Cherpitel C, Ye Y, Bond J, et al. The effect of alcohol consumption on emergency department services use among injured patients: a cross-national emergency room study. J Stud Alcohol 2006; 67: 890-897.
- 12. Indig D, Copeland J, Conigrave K, et al. Why are alcohol-related emergency department presentations under-detected? An exploratory study using nursing triage text. Drug Alcohol Rev 2008; 27: 584-590.
- 13. Peirce B, Boyle A. How has the Licensing Act (2003) changed the epidemiology of assaults presenting to a Cambridgeshire emergency department? Before and after study. Eur J Emerg Med 2011; 18: 351-356.
- 14. Senate Standing Committee on Economics. Personal choice and community impacts inquiry. http://www.aph.gov.au/Parliamentary_Business/Committees/Senate/Economics/Personal_choice (accessed Aug 2015).
- 15. Australian Government, Department of Health and Ageing. Emergency triage education kit. Triage workbook. Canberra: Commonwealth of Australia, 2009. https://www.health.gov.au/internet/main/publishing.nsf/Content/387970CE723E2BD8CA257BF0001DC49F/$File/Triage%20Workbook.pdf (accessed Aug 2015).
- 16. Hall T. Lockout Laws have reduced numbers hospitalised due to alcohol- related violence. Sydney Morning Herald 2015; 16 Apr. http://www.smh.com.au/comment/lockout-laws-have-reduced-numbers-hospitalised-due-to-alcoholrelated-violence-20150415-1mlliy.html (accessed Aug 2015).
- 17. Menéndez P, Weatherburn D, Kypri K, Fitzgerald J. Lockouts and last drinks. The impact of the January 2014 liquor licence reforms on assaults in NSW. Crime and Justice Bulletin [internet] 2015; no. 183 (Apr). http://www.bocsar.nsw.gov.au/Documents/CJB/CJB183.pdf (accessed Aug 2015).
- 18. Poynton S, Donnelly N, Weatherburn D, et al. The role of alcohol in injuries presenting to St Vincent’s Hospital Emergency Department and the associated short term costs. Alcohol Stud Bull 2005; 6: 1-6.
- 19. Kang M. The health of emerging adults in Australia: Freedom, risk and rites of passage. Med J Aust 2014; 562-563. <MJA full text>
- 20. Warburton A, Shepherd J. Tackling alcohol related violence in city centres: effect of emergency medicine and police intervention. Emerg Med J 2006; 23: 12-17.





Abstract
Objective: To determine any impact associated with changes to liquor licensing regulations on emergency department attendances for alcohol-related serious injuries in an inner-city entertainment precinct.
Design, setting and participants: A blinded retrospective analysis of data from the Emergency Department Information System (EDIS) of the major trauma and teaching hospital (St Vincent’s Hospital, Darlinghurst) in the Sydney CBD Entertainment Precinct. Data for trauma cases classified as Australasian triage categories 1 (immediately life-threatening) and 2 (imminently life-threatening, important time-critical treatment, very severe pain) in the 12 months before (24 February 2013 – 23 February 2014; period 1) and the 12 months after (24 February 2014 – 23 February 2015; period 2) the 2014 changes to liquor licensing regulations applied to the precinct.
Main outcome measures: Critically or seriously injured emergency presentations that were identified as related to alcohol use.
Results: In the 2-year study period, there were 13 110 triage category 1 and 2 presentations to the St Vincent’s Hospital emergency department: 6467 during period 1 and 6643 during period 2. Of these, 1564 (4.3%) were patients who presented with alcohol-related serious injuries: 318 (4.9%) during period 1 and 246 (3.7%) during period 2 (P < 0.05). The proportion of alcohol-related serious injury presentations (triage categories 1 and 2) was much higher (9.1% of presentations) during the high alcohol time (HAT; 6 pm Friday to 6 am Sunday) than during the rest of the week (3.1%). After the introduction of the regulatory changes, there was a significant decrease in the number of seriously injured patients during HAT, from 140 presentations (10.4% of presentations) before the change to 106 (7.8%) after their introduction, a relative reduction of 24.8% (P < 0.05). There was a small increase in the number of patients presenting with alcohol-related injuries between 9 pm and midnight.
Conclusions: There was a significant reduction in the number of alcohol-related serious injury and trauma presentations to the emergency department in the 12 months after the introduction of the new liquor regulations. This change was seen throughout the week, but was especially marked at weekends.